You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Regular biofilm removal is critical for good oral health.1 This also applies to interproximal surfaces. Most dental patients, however, do not floss on a regular basis. While almost 32% of adults reported daily flossing, a higher number reported not flossing and the remaining 36.6% reported flossing between 1 and 6 days each week.2 Of those that at least try to floss, many are not flossing correctly. In another study conducted by Shaheen et al examining the technique of dental students, only 39% of the students were able to accomplish thorough biofilm removal when flossing.3
With the low prevalence of string flossing paired with the high prevalence of less-than-ideal flossing technique, it is unsurprising that the American Dental Association (ADA) now lists options besides string floss for interdental biofilm removal, such as water flossers, brushes, or picks designed for cleaning between teeth.4 Maintaining periodontal health is closely related to having both an effective interdental cleaning tool and the ability to perform oral hygiene procedures.5 The latter is dependent on individual factors, including interest, motivation, dexterity, and ability.6
Addressing Patient Noncompliance
Interdental cleaning is an essential part of maintaining good oral hygiene, however many individuals find it difficult to incorporate it into their daily routine. There are several reasons why patients may not comply with flossing recommendations.
Lack of awareness and education. Inconsistent education is a concern for patient care. Some patients may not be aware of the potential consequences of not flossing regularly or may not have received proper instruction on how to floss effectively, leading to frustration and ineffectiveness.
Inability to integrate flossing into an at-home routine. Time constraints are a common reason for noncompliance. Many people may perceive flossing as an optional, time-consuming, and inconvenient task in their daily routine. Additionally, effective flossing is extremely technique dependent and can be challenging for patients, especially if dexterity issues exist7 or there are tight spaces between teeth. Flossing can also be uncomfortable or painful if done incorrectly or if there are underlying dental issues.
Dissatisfaction with an interproximal routine. Patients may understand the benefits of interproximal cleaning and know how to clean effectively, yet may dislike the flossing method they're using.
Good oral health involves more than just receiving treatment from an oral healthcare provider; it also requires consistent at-home care, and this may necessitate behavior change. Techniques such as motivational interviewing (MI)/brief MI have been noted in the literature as effective communication approaches to improve oral hygiene.8-15
Patient compliance may require ongoing support and encouragement from their dental provider. Taking a holistic and patient-centered approach to oral healthcare may increase the likelihood of patients successfully incorporating new habits into their routines and achieving better oral health outcomes. Noncompliance can present in numerous ways. While some reasons for refusal have a simple solution, others require more attention to resolve. Generally, noncompliance can be resolved through communication and by taking the time to discuss the patient's concerns, questions, and details.
The more dental providers can customize their recommendations to fit a patient's lifestyle and capabilities, the more likely the patient will be at successfully adhering to the recommendations. Most people do not floss on a regular basis. Knowing this, there are other options that providers can recommend that are at least equally effective and may appeal to patients more than floss.
Modalities for Interdental Cleaning
There are a variety of options to remove or disrupt biofilm from interproximal spaces, including dental floss, interdental brushes, rubber tips, toothpicks, and oral irrigators (ie, water jets, water flossers).16-18 Each has its pros and cons, and they are all somewhat effective.6 Oral irrigation devices have been found to be as efficient as string floss in removing interdental biofilm.19 Barnes et al found that when combined with toothbrushing, oral irrigation is an effective alternative to manual toothbrushing and dental flossing to reduce bleeding and gingival inflammation and for biofilm removal.20 Research supports the use of oral irrigation devices, with studies suggesting that dental professionals can feel comfortable recommending them to their patients for improved oral health.21
Candidates for Oral Irrigation
With an adequate dental flossing technique, contact-to-contact direct mechanical removal of plaque can be achieved. Patients who struggle with dental flossing should be encouraged to consider alternative methods of interdental cleaning. Sufficient evidence shows that oral irrigation/power interdental devices are as effective, if not more effective, than string floss.17,19-21 Unlike string floss, water flossers are relatively easy to use and may improve compliance. Oral irrigators may be an appropriate option for patients undergoing orthodontic and/or periodontal treatment, utilizing fixed prosthodontics, experiencing dexterity issues, or who simply won't use string floss.
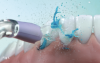
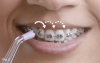
An advantage of using fluid forces to remove or disrupt biofilm is that mechanical forces can be projected beyond the device itself by generating currents in the fluid surrounding the teeth, either by powered brushing or through the creation of water jets by oral irrigation (Figure 1).22 Recently added features to oral irrigators have evolved beyond standard nozzles and simple units. Newer nozzles have a wider coverage area than standard nozzles. Additionally, pacers keep users on track, providing guidance to make it easy for them to clean their whole mouth uniformly, whether moving from one half of the mouth to the other or from one tooth to the next (Figure 2).
Three-Step Framework for At-home Care Recommendations
Time with patients in the dental chair is relatively short, and dental professionals should strive to make the most of it. While most of this time is spent providing care, it is also important to align with patients on effective oral health treatment plans to maintain or improve oral health status. A simple framework, described in the following three steps, can be employed to deliver impactful chairside recommendations for at-home care.
Step 1. Understand the Patient's Mindset
While dental professionals are experts in oral healthcare and assessment, the patient's actions that led to their oral health status and their oral health goals are often unclear. To better understand a patient's willingness to accept recommended treatment, assess the following:
What is the patient's top goal for their oral health? This question helps the clinician determine if patients have a goal they are working toward. Once this is understood, the clinician can use the patient's own goals as a frame of reference when communicating the treatment plan.
Does the patient like their current routine? If patients do not like their current oral hygiene routine, this is an opportunity for the clinician to discuss alternatives. For example, if the patient finds flossing difficult to perform regularly, the clinician might recommend another interdental cleaning option.
Does the patient feel empowered to change their routine if necessary? If patients need to change their routine based on their goals and the clinician's assessment of their oral health, understanding the barriers that may be keeping them from feeling empowered to change can lead to different conversational pathways. Clinicians may find that patients:
like their routine and do not feel motivated to change it
do not like their routine but may not understand how to change it
like their routine and could be motivated to change it if they hear their technique isn't working, or
like their routine and don't want to or don't understand why they need to change it.
Step 2. Communicate Oral Health Status to the Patient and Demonstrate Treatment Solutions
Effective communication is key. Clinicians should use plain language to describe the problem, its causes, and the treatment options available to the patient. Encouraging patients to ask questions and voice concerns helps enhance understanding. Dental providers should use clear and patient-friendly language for a variety of reasons. Using understandable language empowers patients to make informed decisions about their oral health. When patients understand their treatment options, risks, and benefits, they can actively participate in their own care. Also, dental visits can be stressful for many patients, and clear and simple language can help alleviate anxiety by making the information more approachable and less intimidating. Finally, patients are more likely to follow through with recommended treatments and homecare instructions if they understand why they are necessary and how to perform them correctly. Informed consent is a fundamental ethical principle in healthcare.23 Patients must fully understand the risks, benefits, and alternatives of any proposed treatment before giving their consent.
Effective communication builds trust between dental providers and their patients. Patients are more likely to trust providers who can explain things in a way they can grasp. Using medical jargon or overly technical terms can lead to misunderstandings or misinterpretations. Healthcare organizations are increasingly recognizing the importance of health literacy, which involves ensuring that health information is understandable to patients with varying levels of education and literacy.24 Various communication strategies are listed in Table 1.
Step 3: Make Oral Irrigation Recommendations That Are Compelling
Any recommendation for an oral irrigation tool to be part of a patient's homecare routine should be tailored to match their needs and lifestyle. Providers should first assess the patient's oral health needs. They should understand the patient's current oral hygiene practices and any specific issues they are dealing with, such as periodontal disease, orthodontic work, or sensitive teeth. Then they should educate the patient about the benefits of oral irrigation in addressing their unique concerns. Based on the assessment, a specific oral irrigation tool that suits their needs should be recommended. The provider should explain why this tool is recommended and how it can improve the patient's oral health. Factors to consider when making the recommendation include water pressure settings, reservoir capacity, nozzle design, and ease of use. Providing a demonstration of how to use the oral irrigation tool utilizing visual aids and/or videos and offering hands-on demonstrations can be very helpful. The provider needs to ensure that the patient understands the correct technique and might suggest any specific settings or nozzles that would be beneficial for them to use. The provider should confirm that the patient feels comfortable trying oral irrigation and that this change to their routine feels realistic and sustainable.
Written instructions should be given to the patient that outline the steps for using the oral irrigation tool. Information should include how often to use it, any maintenance requirements, and safety precautions. The patient should be made aware of where the recommended tool may be purchased, whether locally or online, or the dental professional might consider dispensing them from their practice. If applicable, the provider should help the patient navigate any insurance or billing concerns related to the purchase and provide necessary documentation or codes for reimbursement, if available.
Check-ins should be scheduled to monitor the patient's progress and address any questions or concerns they may have. The patient may need to be encouraged to integrate the use of the oral irrigation tool into their existing oral hygiene routine. Clinicians should emphasize the importance of consistency in using the tool for maximum benefits. Positive feedback can motivate patients to continue their oral care efforts.
Following these steps will help dental healthcare providers ensure that their patients receive clear, actionable recommendations for incorporating an oral irrigation tool into their homecare routine, ultimately improving their oral health.25 Oral irrigation is a versatile option that can benefit individuals of various age groups, from children to seniors. It can be particularly useful for people with specific oral health needs, such as braces or dental implants, or oral health issues like periodontal disease, or for those simply looking to improve their oral hygiene. Dental professionals should take time to understand each patient's specific oral health goals and motivations.
Conclusion
Recommending oral irrigation as a hygiene solution for patients requires a comprehensive, collaborative approach that considers each patient's individual needs, abilities, and motivations. By tailoring recommendations and offering support throughout the patient's oral health journey, dental professionals can help patients achieve better oral health outcomes and ensure long-term compliance with their treatment plans. By combining patient education, behavior-change techniques, and personalized care plans, dental providers can significantly improve patient compliance with recommended interdental care, ultimately leading to better oral health outcomes.
About the Author
Jennifer Carrie Howard, RDH, BS, MCM
Hygienist, Consultant, Educator/Past National Dental Hygiene Director for Pure Dental Brands
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com.
References
1. Gurenlian JR. The role of dental plaque biofilm in oral health. J Dent Hyg. 2007;81(5):1-11.
2. Fleming EB, Nguyen D, Afful J, et al. Prevalence of daily flossing among adults by selected risk factors for periodontal disease-United States, 2011-2014. J Periodontol. 2018;89(8):933-939.
3. Shaheen RS, Aldosari MM, Altuwaijri HA, et al. Efficiency of flossing technique application among dental students at Riyadh Elm University, Riyadh, Kingdom of Saudi Arabia. J Oral Health Comm Dent. 2019;13(3):63-68.
4. Mark AM. Keeping your gums healthy. J Am Dent Assoc. 2022;153(7):730.
5. Axelsson P, Lindhe J. Effect of oral hygiene instruction and professional toothcleaning on caries and gingivitis in schoolchildren. Community Dent Oral Epidemiol. 1981;9(6):251-255.
6. Zanatta FB, de Mattos WD, Moreira CH, et al. Efficacy of plaque removal by two types of toothpick. Oral Health Prev Dent. 2008;6(4):309-314.
7. Milleman K, Milleman J, Bosma ML, et al. Role of manual dexterity on mechanical and chemotherapeutic oral hygiene regimens. J Dent Hyg. 2022;96(3):35-45.
8. Arnett M, Paulson DR, Evans MD, et al. Health topics emerged from brief motivational interviewing: a randomized clinical trial. J Dent Hyg. 2023;97(5):116-127.
9. Brand VS, Bray KK, MacNeill S, et al. Impact of single-session motivational interviewing on clinical outcomes following periodontal maintenance therapy. Int J Dent Hyg. 2013;11(2):134-141.
10. Arnett MC, Blue CM, Ahmann L, et al. Impact of brief motivational interviewing on periodontal clinical outcomes: a randomized clinical trial. J Dent Hyg. 2022;96(5):13-22.
11. Gao X, Lo EC, Kot SC, Chan KC. Motivational interviewing in improving oral health: a systematic review of randomized controlled trials. J Periodontol. 2014;85(3):426-437.
12. Carra MC, Detzen L, Kitzmann J, et al. Promoting behavioural changes to improve oral hygiene in patients with periodontal diseases: a systematic review. J Clin Periodontol. 2020;47 suppl 22:72-89.
13. Almomani F, Williams K, Catley D, Brown C. Effects of an oral health promotion program in people with mental illness. J Dent Res. 2009;88 (7):648-652.
14. Jönsson B, Ohrn K, Oscarson N, Lindberg P. An individually tailored treatment programme for improved oral hygiene; introduction of a new course of action in health education for patients with periodontitis. Int J Dent Hyg. 2009;7(3):166-175.
15. Renz A, Ide M, Newton T, et al. Psychological interventions to improve adherence to oral hygiene instructions in adults with periodontal diseases. Cochrane Database Syst Rev. 2007;18(2):CD005097.
16. Mani A, Sachdeva S, Gholap S, et al. Interdental aids - a review. IP International J Periodontol and Implantol. 2021;6(4):201-203.
17. Ciancio SG. The dental water jet: a product ahead of its time. Compend Contin Educ Dent. 2009;30(spec no 1):7-13.
18. Lyle DM. Use of a water flosser for interdental cleaning. Inside Dental Assisting. 2012;10(6). https://www.aegisdentalnetwork.com/ida/2012/12/use-of-a-water-flosser-for-interdental-cleaning. Accessed January 25, 2024.
19. Abdellatif H, Alnaeimi N, Alruwais H, et al. Comparison between water flosser and regular floss in the efficacy of plaque removal in patients after single use. Saudi Dent J. 2021;33(5):256-259.
20. Barnes CM, Russell CM, Reinhardt RA, et al. Comparison of irrigation to floss as an adjunct to tooth brushing: effect on bleeding, gingivitis, and supragingival plaque. J Clin Dent. 2005;16(3):71-77.
21. Lyle DM. Relevance of the water flosser: 50 years of data. Compend Contin Educ Dent. 2012;33(4):278-282.
22. Rmaile A, Carugo D, Capretto L, et al. Removal of interproximal dental biofilms by high-velocity water microdrops. J Dent Res. 2014;93(1):68-73.
23. Varkey B. Principles of clinical ethics and their application to practice. Med Princ Pract. 2021;30(1):17-28.
24. Batterham RW, Hawkins M, Collins PA, et al. Health literacy: applying current concepts to improve health services and reduce health inequalities. Public Health. 2016;132:3-12.
25. Misra S, Daly B, Dunne S, et al. Dentist-patient communication: what do patients and dentists remember following a consultation? Implications for patient compliance. Patient Prefer Adherence. 2013;7:543-549.