You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
For more than 250 years, clinicians have utilized the placement of posts in the roots of teeth to retain restorations.1,2 As early as 1728, Pierre Fauchard described the use of "tenons" or metal posts screwed into the roots of teeth to retain bridges.1,3 In the mid-1800s, wood replaced metal as the post material, and the "pivot crown" became popular among dentists; this was a wooden post fitted to an artificial crown and the root canal.1,2,4 Often, these wooden posts would absorb fluids and expand, frequently causing root fractures.4 In the late 19th century, the "Richmond crown," a single-piece post-retained crown with a porcelain facing, was engineered to function as a bridge retainer.2,4 During the 1930s, the custom cast post and core was developed to replace the one-piece post crowns. This procedure required casting a post and core as a separate component from the crown.4 This two-step technique improved marginal adaptation, allowed variation in the path of insertion of the crown,1 and provided a better alignment of the core when the tooth being restored was flared or overlapped the adjacent tooth. In the 1990s, tooth-colored fiber posts debuted as an alternative to these conventional metal post systems.5
The Post and Core Landscape
From the past to the present, the rationale for the utilization of a post system has metamorphosed. The concepts of the past were designed with the belief that endodontically treated teeth were brittle from a loss of moisture6 and required a post to strengthen the weakened tooth.7 Although there is a reduction in moisture content after endodontic treatment, current concepts refute this postulate.6,8,9 Current concepts supported by evidence-based research indicate that the primary objective of any post and core system is to replace missing coronal tooth structure, retain the core,10-12 and provide sufficient retention13,14 and resistance form to the final restoration to restore original form and function.10,11,15 Today, clinicians can choose from a variety of user-friendly post and core systems for different endodontic, restorative, and esthetic requirements.8,16,17 These systems and methods are well documented in the literature.8,11,12,18,19 However, no single post system meets the demands for favorable biomechanical compatibility20,21 or provides the perfect restorative solution for every clinical circumstance, and each situation requires an individual evaluation.22
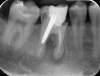
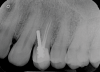
Furthermore, the reconstruction of endodontically treated teeth can present restorative and esthetic challenges for the technician and clinician.23 The failure of these post-retained systems has been documented in numerous clinical studies.10,13,21,24-29 Many of these studies indicate that the failure rate of restorations on pulpless teeth with posts and cores is higher than that for restorations of vital teeth because of their structural differences and the significant loss of tissue.30-35 Several main causes of failure of post-retained restorations have been identified, including recurrent caries, endodontic failure, periodontal disease, post dislodgment, cement failure, post-core separation, crown-core separation, loss of post retention, core fracture, loss of crown retention, post distortion, post fracture, tooth fracture, root perforation (Figure 1), improper post placement (Figure 2), and root fracture.11,36,37Also, corrosion of metal posts has been proposed as a cause of root fracture.38 A post and core system fabricated with dissimilar metals can cause galvanic corrosion that occurs between the two dissimilar materials.39 This gradual destructive process involves the electrical interaction of at least two different metals or nonmetallic conductors in an environment (ie, microleakage) that accelerates the corrosion of at least one of them, while the least noble metal corrodes the most.
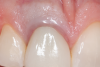
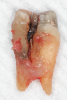
The traditional custom cast dowel core provides a better geometric adaptation to excessively flared or elliptical canals and almost always requires minimal removal of tooth structure.1 Custom cast posts and cores adapt well to extremely tapered canals or those with a noncircular cross section and/or irregular shape and roots with minimal remaining coronal tooth structure.22 Patterns for custom cast posts can be formed either directly in the mouth or indirectly in the laboratory. Regardless, this method requires two appointment visits and a laboratory fee. Also, because it is cast in an alloy with a modulus of elasticity that can be as high as 10 times greater than that of natural dentin,40 this possible incompatibility and rigidity can create stress concentrations in the less rigid root, resulting in post separation or failure.41,42 Additionally, the transmission of occlusal forces through the metal core can focus stresses at specific regions of the root, causing root fracture (Figure 3).40 Furthermore, upon esthetic consideration, the cast-metal post can result in discoloration and shadowing of the gingiva and the cervical aspect of the tooth (Figure 4).43
An alternative and currently more popular method for developing the intraradicular space is the prefabricated post and core system. These systems are classified according to their geometry (ie, shape and surface configuration) and method of retention. The methods of retention are designated as active or passive. Active posts engage the dentin walls of the post space preparation during cementation, whereas passive posts do not engage the dentin but rely on the use of cement for retention.1,44 The basic post shapes and surface configurations are tapered serrated, tapered smooth-sided, tapered threaded, parallel serrated, parallel smooth-sided, and parallel threaded. While active or threaded posts are more retentive than passive posts,45,46 active posts create high stress concentrations in root dentin at each thread during placement.46-48 These stresses have the potential to create cracks that can increase the susceptibility of root fracture when occlusal forces are applied.49-52 Thus, a significant cause of failure with an active post system is root fracture.53-55 More-recent modern designs provide a collar that limits insertion, flexible tips (eg, Flexipost), and stress-reducing thread design. Metal screws have a survival rate of 78% after 1 year and 50% after 5 years.51,56 Parallel-sided serrated posts are the most retentive of the passive prefabricated posts, and the tapered smooth-sided posts are the least retentive of all designs.4
Traditional prefabricated metal posts are made of platinum-gold-palladium, brass, nickel-chromium (stainless steel), pure titanium, titanium alloys, and chromium alloys.4,10,36 Although stainless steel is stronger, the potential for adverse tissue responses to nickel has resulted in the use of a biocompatible titanium alloy.57,58 Also, contributing factors to root fracture such as excessive stiffness (modulus of elasticity)59 and post corrosion4,25 (Figure 5) from many of these metal posts have generated concerns about their use. In addition, prefabricated metal posts can negatively affect the esthetic result.
Nonmetallic prefabricated posts have been developed as alternatives, including ceramic (white zirconia) posts, carbon-fiber posts, and fiber-reinforced resin posts. Zirconia posts have a high flexural strength and are biocompatible and corrosion-resistant.60 This material, however, is difficult to section with a diamond bur intraorally and remove from the canal for retreatment.36 Carbon-fiber posts are made from unidirectional carbon fibers held together with an epoxy resin and ceramic. They exhibit strength and relatively high flexibility and can be retrieved from the canal preparation with ease for retreatment. However, their black color has a negative effect on the final esthetic result of all-ceramic crowns.57 New advances with next-generation tooth-colored posts, which are identical in design to conventional carbon-fiber posts, reduce this esthetic challenge.
Currently, an increased demand for clinically convenient post and core systems to replace lost tooth structure has provided clinicians with a plethora of simplified "one-visit" post and core restorative options.61 Thus, clinicians may be unsure about which restorative materials and techniques to use to achieve optimal results for post and core buildup procedures. As modern dental research continues its quest for the ideal material to restore lost tooth structure, many post and core techniques are available to clinicians for a variety of clinical procedures, and each clinical situation should be evaluated individually.22,61 Clinical and laboratory studies have demonstrated that fiber-reinforced resin posts provide an excellent alternative option for restoring endodontically treated teeth versus metal posts.12,49,62 Studies found fiber-reinforced post systems to be superior to metal prefabricated posts.63 In recent years, there has been a major shift away from metal custom cast posts and cores toward prefabricated metal posts and resin-based composite cores, including a significant movement toward the use of fiber-reinforced resin-based composite posts used with bonded composite buildups.49,64-66 Prefabricated composite post systems are replacing metal post systems because an adhesive procedure with the fiber-reinforced composite post system adds strength to the tooth-restorative interface after bonding.67 Therefore, the fiber-reinforced post has an advantage after assembly by creating a monoblock system.
Direct Fiber-Reinforced Post and Core System
This composite post and core system offers several advantages: a one-appointment technique; no laboratory fees; resistance to corrosion, solubility, and biochemical degradation; reduced root fracture; atraumatic retrievability; and increased retention resulting from microretentive bonding surfaces.5,61,68 It also conserves tooth structure and yields biomechanical properties similar to those of the host dental tissue and has no negative effect on esthetics.5,61,67,69,70 Disadvantages of the technique include technique sensitivity and the need for a careful adhesive protocol and larger inventory of reinforcement materials.5
Several methods are used for the fabrication of the direct fiber-reinforced resin post system, including a custom-made glass fiber post system, which uses a polyethylene woven reinforcement fiber; a prefabricated fiber-reinforced composite post; a direct anatomical formed fiber-reinforced post; and a direct/indirect anatomical formed fiber-reinforced post. Prefabricated fiber-reinforced resin posts flex with the tooth structure, are easy to remove if retreatment is required, and have no negative effects on esthetics. However, the adaptation of the prefabricated post to the canal wall is important for retention, and in some cases the canal must be enlarged to fit the configuration of the selected post, requiring removal of more tooth structure to achieve optimal adaptation. Therefore, these prefabricated posts have optimal adaptation and function in teeth with small circular canals.71 Many roots, however, have irregularly shaped canals, and the prefabricated system is not ideal because of the improper adaptation and the required thickness of the resin cement. This increased cement layer thickness can influence the stress distribution on the restorative assembly and increase the potential risk for the loss of post retention.72 Prospective and retrospective clinical studies have indicated that fiber post dislodgment occurs with greater frequency with thicker cement layers.25,73,74 The thinner the joint, the greater the strength. Also, there is indication that a thin layer of resin cement provides frictional retention of the post.42,75
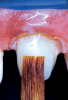
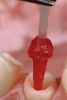
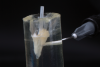
Various methods can be utilized for the treatment of irregular configurations (eg, oval shape, flared roots), including a custom-made glass fiber post system that uses a bondable reinforcement fiber (eg, Ribbond®-THM, Ribbond; Construct™, Kerr Endodontics; everStick®, GC America), a direct anatomical formed fiber-reinforced post system that uses a resin composite to modify the shape of the prefabricated post (Figure 6 and Figure 7),49,76 and a direct/indirect anatomical formed fiber-reinforced post system that entails use of a pattern resin to replicate the anatomical configuration of the post channel that can be translated with flowable resin composite in the laboratory or chairside (Figure 8 through Figure 10). Other methods suggested in the literature for reducing the thickness of the cement layer include root reinforcement with a composite material, the use of accessory fiber posts, or the use of an ovoid-shaped post system (eg, Macro-Lock™ Oval Post, RTD; Polygon Post, Overfibers; Ellipson Post, Acteon/Salitec).77,78
Empirical Data
Most clinical failures involving fiber-reinforced post systems occur through debonding.8,20,24,26,79,80 Clinicians must avoid performing outdated procedures with modern restorative materials when restoring intraradicular post space. It has been reported that bond strengths in different areas of the post channel can be influenced by technique and dentin microanatomy.81 Challenges related to this issue include insufficient light energy being transmitted to the cement at the apical third of the channel,82 the concentration of the dentin tubules that greatly decreases toward the apical region,83 the fact that radicular dentin is irregular and may be void of dentin tubules,83 and the operator applying different conditioners, bonding agents, and cements to these areas in unfavorable conditions.
Evidence suggests that light transmission of translucent fiber post systems may be inadequate; as such, the light intensity of curing units decreases from the coronal to the apical of the post channel for these fiber post systems, and the amount of light reaching the apical third of the post spaces may be insufficient to effectively cure the resin cement.12,68,84 Therefore, light-cured resin cements are not adequate for luting posts.68,85 While one study has reported a fiber-optic post system that had significantly greater light transmission with a light-polymerized resin cement,86 other studies have documented inferior bonding performance of the post channel in apical regions with the use of light-cured adhesives.87,88 Additionally, research has demonstrated that the autopolymerizing potential of dual-cured cements alone is not sufficient to achieve maximum hardness of the cement.89,90 Also, it has been reported that in the presence of translucent posts, the amount of light reaching the apical third of the post channel may be insufficient to effectively cure the resin cement.84 Some specific translucent fiber posts diminish light transmission more than other posts,84,86 and with these translucent posts, the transmission of applied light can be reduced to less than 40%, which can decrease the polymerization of the resin cement.86,91 These differences in light transmission among post systems can be correlated to the variations that exist in their fiber diameter, orientation pattern, and matrix. Furthermore, when light is transmitted through the channel post space, its intensity is significantly diminished as it passes through the resin cement because of attenuation and the shadowing caused by the tooth structure and the post.86,92 However, light intensity reaching the cement may be sufficient to initiate the polymerization process, while the self-curing catalyst is required to ensure maximum degree of cure.89 Nonetheless, dual-cured and self-cured resin cements are recommended because of the light attenuation at the increased depths of the post channel.86,93
No differences have been demonstrated in bonding effectiveness of translucent posts and light-cured or dual-cured composites.86,94 Some clinicians purport the use of dual-cured resin cements with etch-and-rinse adhesives as an excellent restorative choice,20,68 whereas current evidence suggests that for fiber post cementation the most reliable results are achieved with etch-and-rinse adhesives in combination with dual-cured resin cements.12,20,95 Furthermore, studies indicate etch-and-rinse adhesive systems combined with self- or dual-cured resin cements are used more often than self-etching systems to cement fiber posts.26,96 Another systematic review and meta-analysis of in vitro literature reported superior retention of fiber posts to dentin with the use of self-adhesive resin cement.97 This same review indicated that the use of self-adhesive resin cements may improve bond strength of fiber posts to the post channel dentin,97 and this same cement demonstrated less nanoleakage compared to multi-step resin cements when fiber posts were luted to the post channel dentin.98 Another study indicated that the performance of a self-adhesive resin cement along the post channel was similar to that of self-cured resin cements and demonstrated that these materials appear to be less dependent on light irradiation to achieve high bond strength.99 Also, there is evidence that suggests that fiber post bonding is more reliable when utilizing self-adhesive cements due to the multiple steps and difficulty in reaching the apex of the post space.100 Furthermore, several studies reported that use of resin cement or self-adhesive resin cement resulted in increased bond strength between the fiber post and post channel dentin and improved the fracture resistance of the endodontically treated tooth.101,102 Thus, it is well established that the luting procedure plays a significant role in the clinical performance of the restoration of an endodontically treated tooth, and the use of a resin luting cement to line and strengthen the canal walls actually reinforces the root and supports the tooth-restorative complex.37,103
Click here for Part 2 of this article, which describes a novel concept for developing a precise, predictable post and core complex using the injectable resin method and a newly developed fiber-optic post system.
About the Authors
Douglas A. Terry, DDS
Adjunct Professor, Department of Restorative Sciences, University of Alabama at Birmingham, Birmingham, Alabama; Professor Emeritus, Department of Restorative and Esthetic Dentistry, V.S. Dental College and Hospital, Rajiv Gandhi University of Health Sciences, Bengaluru, India; Founder and CEO, Institute of Esthetic and Restorative Dentistry; Private Practice, Houston, Texas
John O. Burgess, DDS, MS
Director of Clinical Research, Clinical Research Professor, School of Dentistry, Louisiana State University, New Orleans, Louisiana; Diplomate, Federal Services Board of General Dentistry
John M. Powers, PhD
Professor Emeritus, UTHealth School of Dentistry, Houston, Texas
Markus B. Blatz, DMD, PhD
Professor of Restorative Dentistry, Chair, Department of Preventive and Restorative Sciences, and Assistant Dean, Digital Innovation and Professional Development, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com.
References
1. Smith CT, Schuman NJ, Wasson W. Biomechanical criteria for evaluating prefabricated post-and-core systems: a guide for the restorative dentist. Quintessence Int. 1998;29(5):305-312.
2. Tylman SD. Theory and Practice of Crown and Bridge Prosthesis. 2nd ed. St. Louis, MO: C.V. Mosby; 1947:1-13.
3. Lynch CD, O'Sullivan VR, McGillycuddy CT. Pierre Fauchard: the ‘father of modern dentistry.' Br Dent J. 2006;201(12):779-781.
4. Smith CT, Shuman N. Prefabricated post-and-core systems: an overview. Compend Contin Educ Dent. 1998;19(10):1013-1020.
5. Terry DA. Restoring the Intraradicular Space: Esthetic Post Systems. Chicago, IL: Quintessence Publishing; 2021.
6. Helfer AR, Melnick S, Schilder H. Determination of the moisture content of vital and pulpless teeth. Oral Surg Oral Med Oral Pathol. 1972;34(4):661-670.
7. Assif D, Gorfil C. Biomechanical considerations in restoring endodontically treated teeth. J Prosthet Dent. 1994;71(6):565-567.
8. Dietschi D, Duc O, Krejci I, Sadan A. Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review of the literature-Part 1. Composition and micro- and macrostructure alterations. Quintessence Int. 2007;38(9):733-743.
9. Papa J, Cain C, Messer HH. Moisture content of vital vs endodontically treated teeth. Endod Dent Traumatol. 1994;10(2):91-93.
10. Upadhyaya V, Bhargava A, Parkash H, et al. A finite element study of teeth restored with post and core: effect of design, material, and ferrule. Dent Res J (Isfahan). 2016;13(3):233-238.
11. Baba NZ, Goodacre CJ. Restoration of endodontically treated teeth: contemporary concepts and future perspectives. Endod Topics. 2014;31(1):68-83.
12. Goracci C, Ferrari M. Current perspective on post systems: a literature review. Aust Dent J. 2011;56(suppl 1):77-83.
13. Sorensen JA, Martinoff JT. Intracoronal reinforcement and coronal coverage: a study of endodontically treated teeth. J Prosthet Dent. 1984;51(6):780-784.
14. Goodacre CJ, Spolnik KJ. The prosthodontic management endodontically treated teeth: a literature review. Part I. Success and failure data, treatment concepts. J Prosthodont. 1994;3(4):234-250.
15. Trushkowsky RD. Restoration of endodontically treated teeth: criteria and technique considerations. Quintessence Int. 2014;45(7):557-567.
16. Paul SJ, Scharer P. Post and core reconstruction for fixed prosthodontic restoration. Pract Periodont Aesthet Dent. 1997;9(5):513-520.
17. Meyenberg KH, Luthy H, Scharer P. Zirconia posts: a new all-ceramic concept for nonvital abutment teeth. J Esthet Dent. 1995;7(2):73-80.
18. Hudis SI, Goldstein GR. Restoration of endodontically treated teeth: a review of the literature. J Prosthet Dent. 1986;55(1):33-38.
19. Lee JH, Sohn DS, Lee CH. Fabricating a fiber-reinforced post and zirconia core with CAD/CAM technology. J Prosthet Dent. 2014;112(3);683-685.
20. Dietschi D, Duc O, Krejci I, Sadan A. Biomedical considerations for the restoration of endodontically treated teeth: a systematic review of the literature, Part II (Evaluation of fatigue behavior, interfaces, and in vivo studies). Quintessence Int. 2008;39(2):117-129.
21. Asmussen E, Peutzfeldt A, Sahafi A. Finite element analysis of stresses in endodontically treated, dowel-restored teeth. J Prosthet Dent. 2005;94(4):321-329.
22. Coleman AJ, Urquiola J. An injection technique for generating direct resin post and core patterns. Quintessence Int. 1996;27(11):749-752.
23. Terry DA, Triolo PT Jr, Swift EJ Jr. Fabrication of direct fiber-reinforced posts: a structural design concept. J Esthet Restor Dent. 2001;13(4):228-240.
24. Cagidiaco MC, Goracci C, Garcia-Godoy F, Ferrari M. Clinical studies of fiber posts: a literature review. Int J Prosthodont. 2008;21(4):328-336.
25. Ferrari M, Vichi A, Garcia-Godoy F. Clinical evaluation of fiber-reinforced epoxy resin posts and cast post and cores. Am J Dent. 2000;13
(spec no):15B-18B.
26. Cagidiaco MC, Radovic I, Simonetti M, et al. Clinical performance of fiber post restorations in endodontically treated teeth: 2-year results. Int J Prosthodont. 2007;20(3):293-298.
27. Balkenhol M, Wostmann B, Rein C, Ferger P. Survival time of cast post and cores: a 10-year restrospective study. J Dent. 2007;35(1):50-58.
28. Wegner PK, Freitag S, Kern M. Survival rate of endodontically treated teeth with posts after prosthetic restoration. J Endod. 2006;32(10):928-931.
29. Gomez-Polo M, Llido B, Rivero A, et al. A 10-year retrospective study of the survival rate of teeth restored with metal prefabricated posts versus cast metal posts and cores. J Dent. 2010;38(11):916-920.
30. Turner CH. Post-retained crown failure: a survey. Dent Update. 1982;9(4):221-229.
31. Tan K, Pjetursson BE, Lang NP, Chan ES. A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clin Oral Implant Res. 2004;15(6):654-666.
32. Heydecke G, Peters MC. The restoration of endodontically treated, single-rooted teeth with cast of direct posts and cores: a systematic review. J Prosthet Dent. 2002;87(4):380-386.
33. Karlsson S. A clinical evaluation of fixed bridges, 10 years following insertion. J Oral Rehabil. 1986;13(5):423-432.
34. Sundh B, Odman P. A study of fixed prosthodontics performed at a university clinic 18 years after insertion. Int J Prosthodont. 1997;10(6):513-519.
35. Basaran ET, Gokce Y. Evaluation of the influence of various restoration techniques on fracture resistance of endodontically treated teeth with different cavity wall thicknesses. Niger J Clin Pract. 2019;22(3):328-334.
36. Asmussen E, Peutzfeldt A, Heitmann T. Stiffness, elastic limit, and strength of newer types of endodontic posts. J Dent. 1999;27(4):275-278.
37. Sirimai S, Riis DN, Morgano SM. An in vitro study of the fracture resistance and the incidence of vertical root fracture of pulpless teeth restored with six post-and-core systems. J Prosthet Dent. 1999;81(3):262-269.
38. Purton DG, Payne JA. Comparison of carbon fiber and stainless steel root canal posts. Quintessence Int. 1996;27(2):93-97.
39. Pameijer CH, Glatz PO, Mobasherat MA. On clinical corrosion of pins. Swed Dent J. 1983;7(4):161-167.
40. Freedman G. The carbon fibre post: metal-free, post-endodontic rehabilitation. Oral Health. 1996;86(2):23-30.
41. Bacchi A, Caldas RA, Schmidt D, et al. Fracture strength and stress distribution in premolars restored with cast post-and-cores or glass-fiber posts considering the influence of ferrule. BioMed Res Int. 2019;2019:2196519.
42. Barcellos RR, Correia DPD, Farina AP, et al. Fracture resistance of endodontically treated teeth restored with intra-radicular post: the effects of post system and dentine thickness. J Biomech. 2013;46(15):2572-2577.
43. Vichi A, Ferrari M, Davidson CL. Influence of ceramic and cement thickness on the masking of various types of opaque posts. J Prosthet Dent. 2000;83(4):412-417.
44. Shillingburg HT Jr, Sather DA, Wilson EL Jr, et al. Fundamentals of Fixed Prosthodontics. 4th ed. Chicago, IL: Quintessence Publishing; 2012.
45. Burgess JO, Summitt JB, Robbins JW. The resistance to tensile, compression, and torsional forces provided by four post systems. J Prosthet Dent. 1992;68(6):899-903.
46. Standlee JP, Caputo AA, Hanson EC. Retention of endodontic dowels: effects of cement, dowel length, diameter, and design. J Prosthet Dent. 1978;39(4):400-405.
47. Standlee JP, Caputo AA, Collard EW, Pollack MH. Analysis of stress distribution by endodontic posts. Oral Surg Oral Med Oral Pathol. 1972;
33(6):952-960.
48. Standlee JP, Caputo AA, Holcomb J, Trabert KC. The retentive and stress-distributing properties of a threaded endodontic dowel. J Prosthet Dent. 1980;44(4):398-404.
49. Soares CJ, Versluis A, Tantbirojin D, et al. Biomechanical principle of root canal-treated-teeth restored with fiber-reinforced resin posts. In: Perdigão J, ed. Restoration of Root Canal-Treated Teeth: An Adhesive Dentistry Perspective. New York, NY: Springer; 2015:87-100.
50. Santos-Filho PC, Soares PV, Reis BR, et al. Effects of threaded post placement on strain and stress distribution of endodontically treated teeth. Braz Oral Res. 2013;27(4):305-310.
51. Schmitter M, Rammelsberg P, Gabbert O, Ohlmann B. Influence of clinical baseline findings on the survival of 2 post systems: a randomized clinical trial. Int J Prosthodont. 2007;20(2):173-178.
52. King PA, Setchell DJ. An in vitro evaluation of a prototype CFRC prefabricated post developed for the restoration of pulpless teeth. J Oral Rehabil. 1990;17(6):599-609.
53. Peroz I, Blankenstein F, Lange KP, Naumann M. Restoring endodontically treated teeth with posts and cores-a review. Quintessence Int. 2005;36(9):737-746.
54. Ekerbom M, Magnusson T, Martinsson T. Prevalence of apical periodontitis, crowned teeth and teeth with posts in a Swedish population. Endod Dent Traumtol. 1991;7(5):214-220.
55. Creugers NH, Mentink AG, Kayser AF. An analysis of durability data on post and core restorations. J Dent. 1993;21(5):281-284.
56. Ahmed SN, Donovan TE, Ghuman T. Survey of dentists to determine contemporary use of endodontic posts. J Prosthet Dent. 2017;117(5):642-645.
57. Christensen GJ. Post and cores: state of the art. J Am Dent Assoc. 1998;129(1):96-97.
58. Sivers JE, Johnson WT. Restoration of endodontically treated teeth. Dent Clin North Am. 1992;36(3):631-650.
59. Assif D, Bitenski A, Pilo R, Oren E. Effect of post design on resistance to fracture of endodontically treated teeth with complete crowns. J Prosthet Dent. 1993;69(1):36-40.
60. Terry DA. Design principles for fibre-reinforced composite resin post and core system. Private Dent. December 2003;60-70.
61. Terry DA, Geller W. Esthetic post systems. In: Esthetic and Restorative Dentistry: Material Selection and Technique. 3rd ed. Chicago, IL: Quintessence Publishing; 2018:458-493.
62. Soares CJ, Valdivia AD, da Silva GR, et al. Longitudinal clinical evaluation of post systems: a literature review. Braz Dent J. 2012;23(2):135-140.
63. Clinical Research Associates. Posts: a shift away from metal? CRA Newsletter. 2004;28(5):1-3.
64. Christensen GJ. When to use fillers, build-ups or post and cores. J Am Dent Assoc. 1996;127(9):1397-1398.
65. Christensen GJ. Building up tooth preparations for full crowns-2000. J Am Dent Assoc. 2000;131(4):505-506.
66. Christensen GJ. Post concepts are changing. J Am Dent Assoc. 2004;
135(9):1308-1310.
67. Perdigão J. Fiber-reinforced resin posts (fiber posts). In: Restoration of Root Canal-Treated Teeth: An Adhesive Dentistry Perspective. New York, NY: Springer; 2015:101-136.
68. Keul C, Kohler P, Hampe R, et al. Glass fiber post/composite core systems bonded to human dentin: analysis of tensile load vs calculated tensile strength of various systems using pull-out tests. J Adhes Dent. 2016;18(3):247-256.
69. Akkayan B, Gulmez T. Resistance to fracture of endodontically treated teeth restored with different post systems. J Prosthet Dent. 2002;87(4):431-437.
70. Gonclaves LA, Vansan LP, Paulino SM, Sousa Neto MD. Fracture resistance of weakened roots restored with a transilluminating post and adhesive restorative materials. J Prosthet Dent. 2006;96(5):339-344.
71. Rosenstiel SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. St Louis: Mosby; 1988.
72. de Andrade GS, Tribst JPM, Dal Piva AMO, et al. A study on stress distribution to cement layer and root dentin for post and cores made of CAD/CAM materials with different elasticity modulus in the absence of ferrule. J Clin Exp Dent. 2019;11(1):e1-e8.
73. Fredriksson M, Astback J, Pamenius M, Arvidson K. A retrospective study of 236 patients with teeth restored by carbon fiber-reinforced epoxy resin posts. J Prosthet Dent. 1998;80(2):151-157.
74. Zarow M, Ramirez-Sebastia A, Paolone G, et al. A new classification system for the restoration of root filled teeth. Int Endod J. 2018;51(3):318-334.
75. Goracci C, Fabianelli A, Sadek FT, et al. The contribution of friction to the dislocation resistance of bonded fiber posts. J Endod. 2005;31(8):608-612.
76. Grandini S, Sapio S, Simonetti M. Use of anatomic post and core for reconstructing an endodontically treated tooth: a case report. J Adhes Dent. 2003;5(3):243-247.
77. Bakaus TE, Gruber YL, Reis A, et al. Bond strength values of fiberglass post to flared root canals reinforced with different materials. Braz Oral Res. 2018;32:e13.
78. Clavijo VG, Reis JM, Kabbach W, et al. Fracture strength of flared bovine roots restored with different intraradicular posts. J Appl Oral Sci. 2009;17(6):574-578.
79. Ferrari M, Cagidiaco MC, Goracci C, et al. Long-term retrospective study of the clinical performance of fiber posts. Am J Dent. 2007;20(5):287-291.
80. Bitter K, Noetzel J, Stamm O, et al. Randomized clinical trial comparing the effects of post placement on failure rate of postendodontic restorations: preliminary results of a mean period of 32 months. J Endod. 2009;35(11):1477-1482.
81. Daleprane B, Pereira CNB, Bueno AC, et al. Bond strength of fiber posts to the root canal: effects of anatomic root levels and resin cements. J Prosthet Dent. 2016;116(3):416-424.
82. Myers ML, Caughman WF, Rueggenberg FA. Effect of restoration composition, shade, and thickness on the cure of a photoactivated resin cement. J Prosthodont. 1994;3(3):149-157.
83. Mjor IA, Smith MR, Ferrari M, Mannocci F. The structure of dentine in the apical region of human teeth. Int Endod J. 2001;34(5):346-353.
84. Goracci C, Corciolani G, Vichi A, Ferrari M. Light-transmitting ability of marketed fiber posts. J Dent Res. 2008;87(12):1122-1126.
85. Meyenberg K. The ideal restoration of endodontically treated teeth - structural and esthetic considerations: a review of the literature and clinical guidelines for the restorative clinician. Part II esthetic consideration. Eur J Esthet Dent. 2013;8(2):238-268.
86. Stylianou A, Burgess JO, Liu PR, et al. Light-transmitting fiber optic posts: an in vitro evaluation. J Prosthet Dent. 2017;117(1):116-123.
87. Bouillaguet S, Troesch S, Wataha JC, et al. Microtensile bond strength between adhesive cements and root canal dentin. Dent Mater. 2003;19(3):199-205.
88. Aksornmuang J, Nakajima M, Foxton RM, Tagami J. Mechanical properties and bond strength of dual-cure resin composites to root canal dentin. Dent Mater. 2007;23(2):226-234.
89. Caughman WF, Chan DC, Rueggenberg FA. Curing potential of dual-polymerizable resin cements in simulated clinical situations. J Prosthet Dent. 2001;86(1):101-106.
90. Hasegawa EA, Boyer DB, Chan DC. Hardening of dual-cured cements under composite resin inlays. J Prosthet Dent. 1991;66(2):187-192.
91. Teixeira EC, Teixeira FB, Piasick JR, Thompson JY. An in vitro assessment of prefabricated fiber post systems. J Am Dent Assoc. 2006;137(7):1006-1012.
92. Musanje L, Darvell BW. Curing-light attenuation in filled-resin restorative materials. Dent Mater. 2006;22(9):804-817.
93. Ferrari M, Vichi A, Grandini S, Goracci C. Efficacy of a self-curing adhesive-resin cement system on luting glass-fiber posts into root canals: an SEM investigation. Int J Prosthodont. 2001;14(6):543-549.
94. Giachetti L, Scaminaci Russo D, Baldini M, et al. Push-out strength of translucent fibre posts cemented using a dual-curing technique or a light-curing self-adhering material. Int Endod J. 2012;45(3):249-256.
95. Breschi L, Mazzoni A, Ferrari M. Adhesion to intra-radicular dentin. In: Ferrari M, Breschi L, Grandini S, eds. Fiber Posts and Endodontically Treated Teeth: A Compendium of Scientific and Clinical Perspectives. Wendywood, South Africa: Modern Dentistry Media; 2008:39-49.
96. Goracci C, Sadek FT, Fabianelli A, et al. Evaluation of the adhesion of fiber posts to intraradicular dentin. Oper Dent. 2005;30(5):627-635.
97. Sarkis-Onofre R, Skupien JA, Cenci MS, et al. The role of resin cement on bond strength of glass-fiber posts luted into root canals: a systematic review and meta-analysis of vitro studies. Oper Dent. 2014;39(1):E31-E44.
98. Bitter K, Perdigão J, Hartwig C, et al. Nanoleakage of luting agents for bonding fiber posts after thermomechanical fatigue. J Adhes Dent. 2011;13(1):61-69.
99. Calixto LR, Bandeca MC, Clavijo V, et al. Effect of resin cement system and root region on the push-out bond strength of a translucent fiber post. Oper Dent. 2012;37(1):80-86.
100. Bitter K. Selection of luting materials for bonding fiber posts. In: Perdigão J, ed. Restoration of Root Canal-Treated Teeth: An Adhesive Dentistry Perspective. New York, NY: Springer; 2015:181-203.
101. Buttel L, Krasti G, Lorch H, et al. Influence of post fit and post length on fracture resistance. Int Endod J. 2009;42(1):47-53.
102. Yaman BC, Ozer F, Takeichi T, et al. Effect of thermomechanical aging on bond strength and interface morphology of glass fiber and zirconia posts bonded with a self-etch adhesive and a self-adhesive resin cement to natural teeth. J Prosthet Dent. 2014;112(3):455-464.
103. Lui JL. A technique to reinforce weakened roots with post canals. Endod Dent Traumatol. 1987;3(6):310-314.