You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Conventional implants require sufficient bone volume and quality for correct placement and successful osseointegration. However, conditions such as prolonged edentulism, unmanaged infections, and expansion of the maxillary sinuses can lead to severe atrophy of the maxillary alveolar bone.1 The severely atrophied maxilla presents serious limitations for conventional implant placement. Patients with such conditions often present with insufficiently retained dentures that give them little to no function. This population of patients is constantly growing with the increase in average life expectancy and edentulism.1
Extensive bone grafting procedures are usually employed to compensate for the bone loss before placement of implants in these orally amputated patients. Sinus and nasal lifts create space for
bone grafting material and eventual implant placement after the elevation of the inferior portion of the sinus and nasal membranes.2,3 Autologous bone is usually required and harvested from other parts of the body to increase the bone volume in both vertical and horizontal dimensions. Autologous bone can be used in both block and particulated forms to be shaped into the defect sites.4,5 Hard tissue can also be intentionally separated through techniques such as vertical distraction osteogenesis and Le Fort 1 osteotomies to place bone grafts in between hard tissues after relocating bone segments to ideal positions.6,7
These various "grafted" approaches often come with long treatment times and high costs. Potential complications such as infections, unpredictable graft resorption, morbidity at the donor sites, and even failure to integrate can occur.1 Therefore, a trend in implant dentistry has been toward less invasive treatment options. This strategy attempts to avoid complicated procedures involving bone augmentation for conventional implant therapy.
"Graftless" approaches, such as the use of alternative implant designs that maximally utilize these patients' residual bone structure and volume, can be employed with no or only minimal bone grafting. Alternative implant macro designs and individualized implants that utilize the patient's residual bone structure and volume are increasingly being applied as alternate solutions for these severely atrophic cases.8-15 Paranasal, pterygoid, and zygomatic implants utilize the patient's extraoral facial bone outside the alveolar process and can provide predictable and optimal results without the need for bone grafting, or using only a small amount of grafting, thus requiring less treatment time. The modern development of diagnostic imaging and 3D printing technology allows clinicians to provide individualized subperiosteal implants that can adapt precisely to the patient's remaining alveolar and surrounding facial bone.
Thus, the objective of this article is to research and evaluate the current state of the art of graftless implantology as an alternative to extensive bone grafting procedures to rehabilitate severely atrophic maxillary arches.
Materials and Methods
Electronic PubMed and Google Scholar searches were conducted in May 2022. The literature search was carried out on articles published up to and including April 2022. The keywords used in this search were: bone graft, sinus lift, distraction osteogenesis, Le Fort 1, graftless, short, narrow, tilted, interantral, paranasal, pterygoid, zygomatic, zygoma, individualized, subperiosteal, and implants. Titles and abstracts from these results were read to find studies eligible for the review.
The studies were selected upon the following criteria: (1) The study should provide clear and adequate descriptions and photographic documentations of the various bone grafting procedures. (2) The study should provide clear descriptions of the implant designs with the associated anatomical landmarks. (3) The study should provide adequate visualization of the implant designs with photographs and graphics.
Systematic reviews, prospective and retrospective cohort studies, case series/reports, and literature review articles that fit the criteria were selected for final review.
Modification of Implant Dimensions: Short and Narrow-Diameter Implants
Review Results
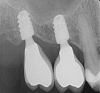
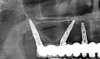
In edentulous areas with compromised bone availability in the vertical or horizontal dimensions, short and/or narrow-diameter implants are alternative treatment modalities to bone grafting procedures for conventional implant placement (Figure 1 and Figure 2). Short implants (<10 mm length) can be placed without vertical bone grafting.9,16 In general, implant width can be considered to be more crucial than implant length for the dissipation of stresses. The crestal bone area receives the maximum pressure, and very little stress is transferred to the apical portion of the implant.17 This is further reinforced through finite element analysis, which shows that implant length is not the principal factor influencing the transfer of occlusal loads to the bone-implant interface. Horizontal and vertical occlusal forces were shown to be directed primarily along the crestal bone surrounding the implant head instead of along the entire bone-implant interface.18 With short implants, there is less risk of damaging vital adjacent structures, such as the maxillary sinus, facial nerves, and roots of adjacent teeth. The relatively shallow osteotomies that accompany short implants and easier access for water irrigation also minimize the risk of bone damage from overheating.9 However, unfavorable crown-implant ratios associated with short implants can lead to complications such as marginal bone loss and even the potential loss of the implant.9 Initial implant stability can also be difficult to achieve in the posterior maxilla where very porous type 4 bone is often present.16
Narrow-diameter implants (NDIs) can be placed in edentulous areas with very thin residual ridges but sufficient bone height.10,19 Also known as small-diameter implants (SDIs) or mini-implants, NDIs have diameters less than 3.5 mm (typically 1.8 mm to 2.9 mm), with various lengths.20 The surfaces of NDIs are blasted and acid-etched to increase roughness and surface area. These implants also often have microthreaded transgingival collars to facilitate soft-tissue adherence.21 The tips of NDIs are often sharp or slightly blunted to provide self-tapping and bone compression capabilities when inserted through the medullary bone. Variable thread thickness and spacings allow for the delivery and use of the implants in the different bone densities present throughout the mouth.20 Square, rectangular, or o-ball implant head designs are utilized to retain both fixed and removable restorations.21
NDIs require a less traumatic process for placement than standard-sized implants, which can be beneficial for medically compromised and elderly patients.19 The inherent lack of microgaps minimizes the risk of peri-implantitis and subsequent crestal bone loss due to less exposure to pathogenic microorganisms.21 The small diameter facilitates osteogenesis and angiogenesis and reduces the chances of osseocompression necrosis occurring in the peri-implant environment.19,21 The inherent self-tapping of these implants and their bone-compressing designs allow for immediate loading.20 However, sufficient control of occlusal loading is necessary since NDIs can be more prone to fatigue fracture.10,19 Also, lack of parallelism between these implants is less forgiving because of their one-piece design. The quality and density of bone is critical for the long-term survival of NDIs.21
Notably, multiple short and narrow-diameter implants can be placed and splinted together to restore both partially and completely edentulous maxillary arches.9,10,16,19
Discussion
Considerable debate has taken place over the use of these unconventionally sized implants with reduced dimensions in width and length. Their capabilities of withstanding occlusal forces have been questioned due to their smaller dimensions and functional surface area. However, numerous studies have shown that short implants with modified and oxidized surfaces and adequate insertion techniques might be as effective as standard-length implants.22Implants with rough surfaces promote better osteoconduction, contact osteogenesis, and osseointegration to enable better bone-to-implant contact. Other modifications such as the use of hydroxyapatite and calcium coating on their surfaces enhance adhesion of proteins and osteoprogenitor cells. Such qualities further contribute to the usage and high survival rates of short implants. Prosthetic restorations utilizing multiple short implants further contribute to high survival rates.17 The use of short implants placed in the posterior atrophic maxilla with sinus autografting has reached success comparable to conventional implants.16 The splinting of multiple short implants can offer improved distribution of occlusal forces to reduce the stress imparted on the implants.
Narrow-diameter implants are typically inserted via minimally invasive or even flapless surgeries.21 Use of a flapless approach maintains the periosteum and reduces postoperative edema, pain, bleeding, morbidity, and bone and soft-tissue loss.21 However, the literature is not clear regarding the terminology associated with reduced-diameter implants. The terms "mini-implants," "narrow-diameter implants," and "small-diameter implants" have been used interchangeably. Additionally, the use of terms such as "provisional implants" and "transitional implants" has further contributed to the confusion. Despite these multiple terminologies, no consensus on the definition of reduced-diameter implants exists in the literature. Although mini-implants were first introduced more than 15 years ago, no studies have compared them with standard dental implants for rehabilitation of complete edentulism. The evidence for short-term survival of NDIs used in partial edentulous situations, however, is encouraging as they have reached success rates ranging from 88.9% to 100%,10 with a first-year interval survival rate of 94.7%. However, the follow-up period of several implants was reported to be less than 12 months. Limited evidence for medium-term survival and no evidence for long-term survival of NDIs in highly atrophic maxillary arches for definitive prosthodontic treatment is available in the literature.
Still, the survival of both short and reduced-diameter implants requires the clinician to sufficiently consider biomechanical and prosthodontic principles before placing and restoring them. The prostheses should be designed to reduce excess lateral occlusal forces to minimize the risk of complications occurring in reduced-dimension implants. Although the use of short and reduced-diameter implants still demands surgical expertise and careful treatment planning, they offer an opportunity for less-experienced clinicians to avoid complex augmentation procedures and successfully treat edentulous patients with less surgical risk and morbidity.
Modification of Implant Orientation and Bone Engagement: Nonalveolar Anatomical and Tilted Implants
Review Results
Tilting of dental implants in the posterior region of the jaw has been demonstrated as an alternative to bone grafting for atrophied jaws. A tilted distal implant can allow a longer dental implant to be used and a more posterior implant position to be achieved. The theory here is that greater distances between the anterior and posterior implants would better distribute occlusal forces; thus, the transverse force placed on the tilted implants would not be detrimental to them. In the maxilla, the distal implants also could benefit from the cortical bony walls of the sinuses and nasal fossae. Therefore, implants can be placed in tilted instead of axial orientations to engage the residual cortical bone in all directions, such as in the palate, anterior and posterior walls of the maxillary sinus, and maxillary tuberosity.23,24 Tilted implants with various macro designs can also adapt to nonalveolar anatomical bone in the paranasal/interantral and pterygomaxillary regions and the zygomatic bone (Figure 3).11,13,25
This approach has become more prevalent especially over the past 15 to 20 years, and its use has been extended beyond the treatment of the severely resorbed maxilla. Clinicians have adopted the use of tilted implants to avoid grafting procedures and maximize the utilization of existing alveolar bone, and often only four implants distributed in the anterior-posterior direction are used. The tilting of distal implants to avoid sinus grafting can also be applied to unilateral fixed dental prostheses.
Anatomical nonalveolar bony regions do not undergo resorption like alveolar bone, as they do not depend on masticatory stimulation for maintenance.12 They are relatively less affected by disuse atrophy. They also provide strong initial stability, enabling immediate loading with provisional prostheses.12 The presence of multiple anatomical bony regions in the perifacial area affords the surgeon the flexibility of not having to depend entirely on alveolar bone availability for complete maxillary rehabilitations.
Paranasal implants engage the residual cortical bone of the interantral region such as the lateral pyriform rim, vomer bone, and nasal crest.11 Tilted paranasal implants are commonly used when there is insufficient native bone volume in the posterior region of the edentulous maxilla. They are most frequently used in full-arch restoration treatment plans utilizing multiple implants, such as the "all-on-4" method. Both the anterior and posterior implants in "all-on-X" treatment plans are placed strategically to obtain an anterior-posterior spread of at least 15 mm for maximal cross-arch stability. The anterior-posterior spread, a biomechanical concept that is crucial for full-arch restorations, can be better achieved with the use of paranasal implants. Ideally, a 12 mm to 15 mm spread between the anterior and posterior implants is necessary to restore maxillary full-arch restorations safely and adequately.11
In cases of extreme alveolar atrophy when such conditions cannot be met, implants can be placed into the residual cortical bone of the paranasal region for rehabilitation.11 The paranasal bone available in the lateral pyriform rim area and midline nasal crest allows for flexible insertion orientations of both the posterior and anterior implants. Such versatility enables the implants to emerge in positions that attain the 12 mm to 15 mm anterior-posterior spread, further maximizing biomechanical stability while minimizing unfavorable distal cantilevers.
The inherent cortical quality of paranasal bone can also help the maxillary implants achieve a combined torque value of 120 Ncm. Such a value is often necessary to be able to deliver immediately loaded provisional prostheses for all-on-X treatments. The cortical bone is most importantly found in the lateral nasal wall, subnasal bone, and height of the midline suture that includes the vomer and nasal crestal bone.
Discussion
The use of paranasal, pterygoid, and zygomatic implants can be combined with conventional implants or with each other to restore completely edentulous atrophic maxillary arches. In certain cases, such as when there is only minimal bone available in the posterior region but adequate anterior maxillary bone, conventional implants in the anterior region can be combined with posterior pterygoid or zygomatic implants to completely rehabilitate the maxillary arch. In cases of generalized extreme alveolar atrophy, paranasal implants engaged in the anterior can also be combined with posterior zygomatic and/or pterygoid implants for full-arch rehabilitation. Such versatility in treatment options allows clinicians to adequately restore any edentulous arch.
Paranasal and tilted implants are considered to be relatively less invasive with a more favorable complication pattern compared to implants engaging in the pterygoid and zygomatic regions.11 In cases of extreme alveolar atrophy in fully edentulous patients, the presence of bone mass in the interantral region that encompasses the pyriform rim and midline nasal crest area should be evaluated first. The amount of bone mass in these areas can often be sufficient to fully restore the completely edentulous arches before resorting to zygomatic implants, a treatment option that is often considered to be more invasive and riskier. Furthermore, the cortical nature of this region allows for increased composite torque value, which allows for the number of implants needed for full-arch restorations to be reduced to as few as four. Fewer implants delivered renders the entire treatment process less traumatic for patients. In cases where only the vomer bone is present, the use of paranasal implants combined with bilateral posterior zygomatic implants can circumvent the need to utilize four zygomatic implants, or "quad zygoma" treatment, for full-arch rehabilitation.
Bellini et al investigated the stress patterns at the bone-implant interface of tilted implants using 3-dimensional finite element analysis and found that the numerical values of compressive stress were lower in the tilted implant configurations.26 They also found that tilting the implants reduces cantilever length by increasing the inter-implant distance. This may have produced a better load distribution, thereby reducing the stress level of the splinted implants. As a result, a biomechanical advantage is gained by using the tilted implants. Within the limitations of the study, the Bellini analysis supports the use of tilted implants to treat the edentulous maxilla. Menini et al systematically reviewed 1,623 implants placed in the maxillae of 324 patients.27 Of these implants, 778 were tilted. The overall weighted cumulative success rate was reported as 98.62%. They suggested the use of tilted implants for full-arch immediate loading rehabilitations of the maxilla with a favorable short-term prognosis.
Pterygoid Implants
Review Results
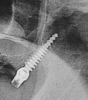
Pterygoid implants have been defined as "[an] implant placed through the maxillary tuberosity into the pterygoid plate"28 (Figure 4). Pterygoid implants cross the maxillary tuberosity from the edentulous second or third molar regions to engage the dense cortical bone formed by the posterior wall of the maxillary tuberosity, horizontal process of the palatine bone, and pterygoid process of the sphenoid bone.12,25,28
These implants are typically 3.5 mm to 4.3 mm in diameter and 18 mm to 25 mm long with multi-unit abutment angulations up to 60 degrees. Such lengths are necessary to ensure that the implant's apex engages the cortical bone of the pterygopalatine suture after crossing the thick tissue often present in the maxillary tuberosity. The angulation is also dependent on the angle of the posterior wall of the maxillary sinus and its proximity to the posterior wall of the maxillary tuberosity. Pterygoid implants often have aggressive V-shaped, pointed, self-tapping apices to ensure stable anchorage upon delivery and widely threaded necks to compress the low-density bone in the maxillary tuberosity region.29
Discussion
The posterior maxilla represents a challenging intraoral area for rehabilitation with osseointegrated implants for many reasons, such as anatomy and presence of the maxillary sinus, insufficient bone volume, poor bone quality, and difficult access. Other anatomical factors, such as large fatty marrow spaces and the rare presence of cortical bone covering the alveolus, have also made the posterior maxilla area less than ideally suited for implant placement. Biomechanical factors, including intense chewing forces generated during mastication, add to the challenges in this area, as occlusal forces are higher in the premolar and molar regions than in the anterior maxilla.
Introduced more than 30 years ago, the placement of implants in the pterygomaxillary region provides bone anchorage in the atrophic posterior maxilla without the need for sinus augmentation or supplemental grafting procedures. Pterygoid implants also can eliminate the detrimental effects of cantilever-induced loading forces when only anterior implants are used to support a complete fixed prosthesis.12 The excellent primary stability provided by the engagement into dense cortical bone allows for immediate loading; additionally, very thick and keratinized soft tissue commonly found in the tuberosity area can aid in the maintenance of peri-implant health.12 Overall, the procedure is associated with lower costs, shorter healing times, and less overall morbidity when compared with grafting approaches for treatment of the resorbed posterior maxilla.12
The proximity of the pterygoid bone to vital structures, however, such as the internal maxillary and greater palatine arteries, posterior superior alveolar nerve, pterygoid muscles, contents of the infratemporal and pterygopalatine fossae, nasopharynx, and sphenoid sinus, is a major risk factor.25 The technique sensitivity, presence of impacted third molars, and difficult access to visualization of the entire surgical site can be obstacles for placement. There is also difficulty in radiographically assessing marginal bone loss around pterygoid implants over time.12,25 Limited oral hygiene access associated with the distal portion of the prosthesis is also a drawback of this therapy. Finally, placement of pterygoid implants involves a significant learning curve for the surgeon.
Despite being a somewhat infrequently used surgical approach, the use of pterygoid implants to enable the avoidance of grafting of the edentulous posterior maxilla offers clinicians an additional treatment method that is supported by modest clinical evidence of success rates of up to 94.87%.12 Candel et al reviewed 1,053 pterygoid implants placed in the maxillae of 676 patients.30 The weighted average success rate was reported as 90.7%. The authors concluded that pterygoid implants have a high success rate with bone loss levels similar to conventional implants and are, therefore, a viable alternative to rehabilitate the posterior atrophic maxilla. Curi et al investigated 66 pterygoid implants placed in 56 patients.31 The 3-year overall pterygoid implant survival rate was 99%, the 3-year overall prosthesis survival rate was 97.7%, and the mean bone loss around pterygoid implants 3 years after loading averaged 1.21 mm.
(Click here to access Part 2 of this article.)
About the Authors
Sung Hoon Choo, DDS
General Practice Residency, Kings County Hospital Center, Brooklyn, New York
Robert S. Glickman, DMD
Associate Dean for Clinical Affairs and Hospital Relations, Professor and Chair, Department of Oral and Maxillofacial Surgery, New York University College of Dentistry, New York, New York
Thomas G. Wiedemann, MD, PhD, DDS
Clinical Associate Professor, New York University College of Dentistry, New York, York
Queries to the author regarding this course may be submitted to authorqueries@broadcastmed.com.
References
1. Davó R, David L. Quad zygoma: technique and realities. Oral Maxillofac Surg Clin North Am. 2019;31(2):285-297.
2. Mohan N, Wolf J, Dym H. Maxillary sinus augmentation. Dent Clin North Am. 2015;59(2):375-388.
3. Raja SV. Management of the posterior maxilla with sinus lift: review of techniques. J Oral Maxillofac Surg. 2009;67(8):1730-1734.
4. Schwartz-Arad D, Levin L. Intraoral autogenous block onlay bone grafting for extensive reconstruction of atrophic maxillary alveolar ridges. J Periodontol. 2005;76(4):636-641.
5. Louis PJ, Gutta R, Said-Al-Naief N, Bartolucci AA. Reconstruction of the maxilla and mandible with particulate bone graft and titanium mesh for implant placement. J Oral Maxillofac Surg. 2008;66(2):235-245.
6. Block MS, Baughman DG. Reconstruction of severe anterior maxillary defects using distraction osteogenesis, bone grafts, and implants. J Oral Maxillofac Surg. 2005;63(3):291-297.
7. Marchetti C, Felice P, Lizio G, Rossi F. Le Fort I osteotomy with interpositional graft and immediate loading of delayed modified SLActive surface dental implants for rehabilitation of extremely atrophied maxilla: a case report. J Oral Maxillofac Surg. 2009;67(7):1486-1494.
8. Pommer B, Busenlechner D, Fürhauser R, et al. Trends in techniques to avoid bone augmentation surgery: application of short implants, narrow-diameter implants and guided surgery. J Craniomaxillofac Surg. 2016;44(10):1630-1634.
9. Torres-Alemany A, Fernández-Estevan L, Agustín-Panadero R, et al. Clinical behavior of short dental implants: systematic review and meta-analysis. J Clin Med. 2020;9(10):3271.
10. Klein MO, Schiegnitz E, Al-Nawas B. Systematic review on success of narrow-diameter dental implants. Int J Oral Maxillofac Implants. 2014;29 suppl:43-54.
11. Jensen OT, Adams MW, Smith E. Paranasal bone: the prime factor affecting the decision to use transsinus vs zygomatic implants for biomechanical support for immediate function in maxillary dental implant reconstruction. Int J Oral Maxillofac Implants. 2014;29(1):e130-e138.
12. Araujo RZ, Santiago Júnior JF, Cardoso CL, et al. Clinical outcomes of pterygoid implants: systematic review and meta-analysis. J Craniomaxillofac Surg. 2019;47(4):651-660.
13. Sharma A, Rahul GR. Zygomatic implants/fixture: a systematic review. J Oral Implantol. 2013;39(2):215-224.
14. Gellrich NC, Rahlf B, Zimmerer R, et al. A new concept for implant-borne dental rehabilitation; how to overcome the biological weak-spot of conventional dental implants? Head Face Med. 2017;13(1):17.
15. Mian M, Delpachitra S, Ackland D, et al. Three-dimensional printing in oral and maxillofacial surgery: current landscape and future directions. Oral Surgery. 2022;15(3):431-442.
16. Chaware SH, Thakare V, Chaudhary R, et al. The rehabilitation of posterior atrophic maxilla by using the graftless option of short implant versus conventional long implant with sinus graft: a systematic review and meta-analysis of randomized controlled clinical trial. J Indian Prosthodont Soc. 2021;21(1):28-44.
17. Romeo E, Bivio A, Mosca D, et al. The use of short dental implants in clinical practice: literature review. Minerva Stomatol. 2010;59(1-2):23-31.
18. Fugazzotto PA, Beagle JR, Ganeles J, et al. Success and failure rates of 9 mm or shorter implants in the replacement of missing maxillary molars when restored with individual crowns: preliminary results 0 to 84 months in function. A retrospective study. J Periodontol. 2004;75(2):327-332.
19. Flanagan D. Fixed partial dentures and crowns supported by very small diameter dental implants in compromised sites. Implant Dent. 2008;17(2):182-191.
20. Sharma S, Dhruvakumar D. Recent trends in implant dentistry: a mini-review. Tanta Dental Journal. 2018;15(3):127-131.
21. Jackson BJ. Small-diameter implants: a 7-year retrospective study. J Oral Implantol. 2017;43(2):125-129.
22. Maló P, de Araújo Nobre M, Rangert B. Short implants placed one-stage in maxillae and mandibles: a retrospective clinical study with 1 to 9 years of follow-up. Clin Implant Dent Relat Res. 2007;9(1):15-21.
23. Chrcanovic BR, Albrektsson T, Wennerberg A. Tilted versus axially placed dental implants: a meta-analysis. J Dent. 2015;43(2):149-170.
24. Peñarrocha-Oltra D, Candel-Martí E, Ata-Ali J, Peñarrocha-Diago M. Rehabilitation of the atrophic maxilla with tilted implants: review of the literature. J Oral Implantol. 2013;39(5):625-632.
25. Bidra AS, Huynh-Ba G. Implants in the pterygoid region: a systematic review of the literature. Int J Oral Maxillofac Surg. 2011;40(8):773-781.
26. Bellini CM, Romeo D, Galbusera F, et al. A finite element analysis of tilted versus nontilted implant configurations in the edentulous maxilla. Int J Prosthodont. 2009;22(2):155-157.
27. Menini M, Signori A, Tealdo T, et al. Tilted implants in the immediate loading rehabilitation of the maxilla: a systematic review. J Dent Res. 2012;
91(9):821-827.
28. Nag PVR, Sarika P, Bhagwatkar T, Dhara V. Pterygoid implant: option for rehabilitation of the atrophic posterior maxilla. Int J Contemp Dent Med Rev. 2019. doi: 10.15713/ins.ijcdmr.135.
29. Agbaje JO, Meeus J, Vrielinck L, Diederich H. Rehabilitation of atrophic maxilla using pterygoid implants: case reports. Modern Approaches in Dentistry and Oral Health Care. 2018;1(1). doi: 10.32474/MADOHC.2018.01.000103.
30. Candel E, Peñarrocha D, Peñarrocha M. Rehabilitation of the atrophic posterior maxilla with pterygoid implants: a review. J Oral Implantol. 2012;38(spec no):461-466.
31. Curi MM, Cardoso CL, Ribeiro Kde C. Retrospective study of pterygoid implants in the atrophic posterior maxilla: implant and prosthesis survival rates up to 3 years. Int J Oral Maxillofac Implants. 2015;30(2):378-383.