You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Since the beginning of time, facial esthetics have played a prominent role in communication among individuals. A person's smile is an integral part of facial esthetics and frequently reflects a distinctive impression of the individual's personality; therefore, this human characteristic has always received considerable attention. Today, facial attractiveness plays an important role in affecting not only an individual's self-esteem but also social opportunities, professional presentation, and employment options. An attractive smile revealing a healthy-looking and appealing dentition has become a major demand by patients and professionals. The American Academy of Cosmetic Dentistry reported in 2018 that 86% to 89% of dental patients sought treatment to improve physical attractiveness and self-esteem for various reasons.1
Losing a tooth or teeth in the esthetic zone can be traumatic for a patient. Treatment is professionally demanding and time-consuming. Moreover, patients can become emotionally dissatisfied and frustrated with esthetically poor prostheses, whether tooth- or implant-supported. Traditionally, providing a tooth-supported esthetic prosthesis demanded dental professionals to focus on achieving a high level of excellence. Then, when implants were incorporated into everyday dental therapy, even greater professional skills were required to achieve optimal surgical as well as prosthetic outcomes.
Naturally, numerous "pros and cons" can be attributed to both treatment choices-implant- or tooth-supported restorations-in the esthetic zone. Both options are achievable when provided by skilled clinicians, but many variables dictate a clinician's decision. The scientific literature of long-term success of teeth- and implant-supported restorations fails to demonstrate a superiority between the two modalities.2
Almost all studies have examined the survival rate of restorations in posterior sites. Yet, no long-term controlled data has been published regarding the success of teeth- and implant-supported restorations in the esthetic zone. Additionally, unlike restorations in the posterior segments, the evaluation of success/failure in the esthetic zone cannot be based exclusively on whether or not osseointegration is achieved, nor can it be limited to the evaluation of survival rates of teeth/implants or lack of pathologies around the restoration. Rather, the assessment of success or failure of anterior restorations must equally refer to additional factors such as hard- and soft-tissue appearance and skeletal facial changes that may occur over time and affect esthetics. Adverse changes, particularly around implants, can be problematic for clinicians, especially those who are less experienced and may lack the skills and training to properly manage such complications. In a review article, Fuentealba and Jofre summarized in detail common esthetic failures of implant-supported restorations and concluded that all aspects of treatment should be borne in each clinician's mind before attempting esthetic therapy.3
The purpose of this article is to discuss specifically long-term changes that can be anticipated following placement of implant-supported restorations in the esthetic zone and the critical risk factors that clinicians should consider during treatment planning to help prevent such harmful consequences.
Soft-Tissue Dehiscence
Implant therapy in the maxillary anterior region of the dentition is technique sensitive. Proper diagnosis, treatment planning, and execution can minimize unfavorable outcomes. Even so, long-term complications can occur. One of the most critical determinants of soft-tissue esthetics is the apicocoronal level of the buccal mucosal margins. An apical shift of the mucosal margins and changes in the soft-tissue contour may cause an esthetic failure,4 and approximately 26% of cases may experience buccal soft-tissue dehiscence (STD) (Figure 1).5
Treatments of STD around implants are far more complex than around teeth. Peri-implant soft tissues have a reduced blood supply, and the structure of their fibers differs from that of gingival tissues. Various soft-tissue grafting techniques have been proposed to treat STD in the esthetic zone but have displayed inconsistent results. At present, no predictable procedure is recognized as one that attains complete dehiscence coverage of exposed implants. Often, implant removal followed by ridge reconstruction and a new, properly positioned implant placement provides a more predictable outcome and better prognosis than soft-tissue management for implant coverage.6
Risk and Protective Factors for Soft-Tissue Dehiscence
It has been proposed that up to 2 mm of bone thickness should be maintained to support soft-tissue levels and prevent soft-tissue recession.7,8 Achieving soft-tissue thickness of at least 2 mm has also been shown to preserve crestal bone levels around bone-level implants.9,10 Soft-tissue thickness also aids in concealing "shine through" of prosthetic components and producing noticeable color variations compared to adjacent natural teeth.11,12 Increasing the supracrestal soft-tissue dimensions at the time of immediate placement also improves the opportunity for stable esthetics over time.13
Tissue augmentation can play a dramatic role in minimizing some of these negative physiologic changes after extraction, regardless of whether implants are placed immediately or in a delayed fashion.14 Unfortunately, even with augmentation, bone loss, soft-tissue recession, and esthetic complications can occur.15 The fact that some degree of negative changes will transpire around implants placed in the anterior dentition has led researchers and clinicians to develop novel techniques, such as partial extraction therapy and socket shield techniques, to avoid these changes.16,17 Such techniques are effective; however, complications are not uncommon, and not all teeth requiring extraction are suitable for these types of treatment.
Other aspects of implant therapy can be taken into consideration to mitigate the aforementioned complications, such as implant platform diameter, position within an extraction socket or edentulous site, and prosthetic contours. Ideally, an implant placed in the anterior sextant should not approximate the facial bone plate or adjacent teeth, so as to accommodate the biologic width around the implant without causing bone remodeling at the natural tooth. Recently, a new implant design with a hybrid macrogeometry has been introduced featuring a narrower coronal portion to maintain greater implant-tooth and implant-facial plate distances.18 The opportunity this affords to augment the peri-implant socket gaps proximally and facially can support the soft tissues and improve esthetic outcomes.19 Maintaining a larger horizontal distance between the implant platform and the facial tissues of an extraction socket has been shown to result in significantly less facial recession.20 Short-term studies have demonstrated that narrow-neck implants improved esthetic results over a 1- to 2-year period.21-23
Skeletal Changes Adjacent to Single Implant-Supported Restorations
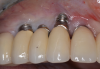
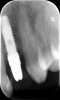
Numerous clinical studies of skeletal changes and alveolar bone growth modifications around single implant-supported restorations in the esthetic zone in growing pigs and human case reports have been published.24-27 This issue has attracted particular attention in young individuals, most of whom required implant therapy due to congenital agenesis or trauma. A topic of thorough discussion among clinicians has been whether to use dental implants in young patients at all to replace missing teeth and, if so, what is the optimal age to place them with regard to possible skeletal changes that might follow. Implants become ankylosed to the bone in an identical way that an avulsed tooth behaves following late re-implantation.28 Such ankylosed teeth as well as dental implants do not adapt to eruptive processes of the surrounding skeletal growth and thus develop infraocclusion, which can severely affect esthetic appearance by the tooth or restoration being shorter than the neighboring teeth, which continue their growth (Figure 2 and Figure 3). Additionally, interproximal contact opening has been observed between the ankylosed crown and nearby natural crowns. Several in vivo experiments that examined osseointegrated implants in young populations concluded that dental implants should not be placed in young patients until their permanent dentition is fully erupted and their skeletal growth completed.29 Such recommendation was even more accentuated when the esthetic zone was involved.
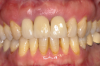
Further investigations of a crown's submersion risk among adults showed that significant skeletal dimensional changes as well as continuous eruption of teeth can occur later in life also (Figure 4).30 Such findings prompted researchers to follow-up single implant-supported prosthesis cases of different age populations for various time periods. Over an 8-year period, Thilander et al followed 15 adolescents who had single implant-supported crowns placed in the anterior maxilla.29 They reported no implant loss as well as an acceptable esthetic appearance in most subjects at the end of the observation period; however, eruption of the adjacent natural teeth continued and resulted in infraocclusion of the implant-supported crowns in some patients, as well as reduction of marginal bone level around some teeth adjacent to the implants. The authors specified that the infraocclusion was mainly found where incisor contact was absent meaning that good incisor stability is of utmost importance before an implant is placed in the esthetic area. Additionally, the authors tracked a single implant-supported crown placement in the upper incisor area of three adults and observed infraocclusion years after installation. They concluded that infraocclusion might occur in adulthood also and no chronological age is considered safe from such skeletal changes. In the adolescent group, the main vertical marginal difference occurred during the first 3 years of follow-up, which corresponded to the overall body growth of the individual. Still, infraocclusion further continued in 10 individuals during the subsequent years, despite body growth cessation. In a case report by Rossi and Andreasen, unfavorable clinical and radiographic findings were demonstrated over a 15-year period after a single tooth replacement by dental implants.25 In addition to the 9 mm discrepancy between the implant collar and the cementoenamel junction of the adjacent central incisor, the authors found that the maxilla significantly resorbed on the labial aspect during the skeletal facial vertical growth.
Based on clinical findings among young populations, it has been suggested that the most appropriate time for implant placement is the age when skeletal growth is finalized,31,32 which corresponds with the termination of general skeletal growth. However, the orthodontic literature has disclosed that facial growth actually continues throughout life (Figure 4),33 and therefore, at present, it is recognized that no decision as to the right time to place implants in the esthetic area is definite, and each case should be discussed with the patient and/or, in the case of adolescents, the parents as well.
Most case reports discussed infraocclusion following single implant-supported crown placement in adolescents and young patients. Cocchetto et al demonstrated that facial skeletal growth does not stop after adolescence but continues into adulthood.27 Therefore, the timing of esthetic treatment that includes single implant placement next to natural teeth should be carefully considered and discussed with the patient. In a retrospective evaluation of implant-retained crowns in the anterior maxillae of adult patients during a 20-year span, 73% of recalled patients displayed infraocclusion. There was no statistical difference between the younger (<30) and older (>30) groups. When evaluating their awareness and perception of the problem, most of the patients were unaware of the change, or if they were aware, they showed no interest in changing the situation. No predisposition risk factors have been identified for this potentially frustrating situation.34
Mijiritsky et al reviewed the literature on this topic among adolescent and adult patients and attempted to evaluate the effect of age, gender, facial shape, occlusal contact, and implant location in the maxilla on continuous tooth eruption next to implant-supported crowns.35 No definite conclusions were drawn from their search other than confirming that facial skeletal growth might continue even into the fifth decade of life; thus, it should be the clinician's decision whether to treat such cases and consider possible future consequences.
Treatment of tooth infraocclusion is challenging, prolonged, and expensive. Such treatment is even more difficult and professionally stimulating when a high smile line is present and/or in cases of a thin-scalloped gingival phenotype. Therefore, prevention of such situations is recommended. Prevention primarily includes verification of skeletal growth termination, a thorough evaluation of the patient's lip line during smiling, and examination of the patient's periodontal condition of teeth adjacent to the future implant installation in order to estimate future tooth stability.29
Peri-implantitis
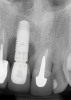
Peri-implantitis is an inflammatory disease affecting the tissues around dental implants. It is characterized by inflammation in the peri-implant mucosa and progressive loss of the implant-supporting bone (Figure 5 and Figure 6).36 A meta-analysis estimated the prevalence of peri-implantitis to be 22%, and it increases as a function of time.37 A recent study indicated that implants in the maxillary anterior and mandibular anterior regions had a higher prevalence of peri-implantitis than the maxillary posterior region,38 making the esthetic zone a risk area for the long-term success of dental implants.
The clinical appearance of peri-implantitis defects may vary and is dependent on the nature of the implant's surrounding hard and soft tissues (eg, thin or thick phenotype), severity of bone resorption, and level of inflammation. In the absence of treatment, peri-implantitis progresses in a nonlinear and accelerating pattern.36
Presently, there is no consensus regarding the treatment of peri-implantitis. Nonsurgical treatment of peri-implantitis was found to be ineffective in preventing disease progression, and surgical intervention is recommended to prevent further bone loss.39 Adjunctive implantoplasty, the addition of a bone graft, or both, were shown to be effective in the long term; however, their potential benefit over conventional surgical therapy is yet to be determined.40,41 Nevertheless, the treatment success of this condition was at best favorable in the short term, with 75% of the cases unresolved or recurred after 5 years.42 Moreover, a systematic review and meta-analysis evaluating the efficacy of bone augmentation at peri-implantitis sites revealed that significant mucosal recessions occurred over a 12-month follow-up period after treatment.43
The effect of surgical therapy on the postoperative soft-tissue response and marginal recession is crucial for the final esthetic outcome, particularly for patients with a high smile line that exposes interdental papillae and gingival margins. Presently, no study has specifically investigated the effect of surgical intervention treatment of peri-implantitis in the esthetic zone on esthetic outcomes using patient-centered and subjective markers. Only a few case reports have described successful resolution of inflammation and partial bone fill events but with highly compromised esthetic outcome.44
Severe peri-implantitis occasionally dictates implant removal and retreatment. In most cases, it leads to a severe residual bone defect that requires sophisticated methods to create proper bone for implant placement. To date, the treatment of complex alveolar bone defects, especially within the esthetic zone, remains challenging.
Because of the aforementioned issues, clinicians should consider alternatives to implant-supported restorations in the esthetic zone. Such alternatives include tooth-supported restorations or conventional or adhesive bridges. Medium- to long-term resin-bonded bridges showed survival rates of 91.4% and 82.9% after 5 and 10 years, respectively.45 These results support the use of resin-bonded restorations as a predictable alternative to implant-supported restorations in the esthetic zone. Anterior bridges had a higher survival rate, with zirconia frameworks performing better than those comprised of metal alloys. Undoubtedly, dental implants provide an excellent solution for long-term function and esthetics; however, such a restoration involves extremely accurate and complex planning and treatment and carries copious risks that might evolve over the long term. Particular care should be taken when placing implants in young patients since this treatment option can have negative repercussions for a lifetime. If implant placement is considered in these situations, adherence to biologic principles is essential to minimize risk for future peri-implantitis.
Minimizing Risk for Peri-implantitis
Currently, the most recognized etiological agent of peri-implantitis is bacterial plaque.36 To reduce the risk for inflammation, patients should perform effective plaque control measures and comply with a personalized maintenance program.46 Smoking and uncontrolled diabetes are also suggested risk factors that promote peri-implantitis, but the evidence is still inconclusive.36
Some clinical considerations prior to implant therapy can also minimize the risk of future peri-implantitis. Thick and wide keratinized peri-implant tissue was shown to be less susceptible to inflammation and bone loss.47 In the absence of such favorable conditions, soft-tissue grafting should be indicated to protect the underlying crestal bone.
The prosthetic design is also important. Prosthetically driven implant position and adequate spacing may facilitate a cleansable restoration. Screw-retained restorations prevent submucosal cement retention, which may trigger inflammation and damage.48 Periodontally susceptible patients were found to be two to three times more prone to peri-implantitis than healthy individuals.36 In such cases, an alternative to implant-supported restoration should be considered. If implant treatment is utilized, evidence has shown that a machined collar or minimally rough surface exhibits a lower prevalence of peri-implantitis.49
Conclusion
A "picture-perfect" smile has become highly desired among much of the western population. People seek esthetic dental treatment for a variety of reasons, including correction of previously failed cosmetic treatments, repair of trauma-related incidents, preparation for upcoming social or professional events, and a desire to look and feel younger. However, long-term esthetic complications can lead to a patient's disappointment. When devising a treatment plan for patients with compromised dentitions, the clinician's choice often is either to build on the existing teeth or perform tooth extraction followed by restoration with implant-supported reconstruction. Where esthetic tooth replacement is involved, the choice is even more challenging.
Both tooth- and implant-supported restorations are acceptable in the hands of a capable clinician, but many variables dictate clinicians' decisions. Some of these variables are patient dependent, and many are operator dependent; hence, the dental team must thoroughly discuss all factors before coming to a final treatment decision.
A crucial point of emphasis is that when extractions in the esthetic zone are planned, a careful provision of possible treatment alternatives and expectations should be discussed with the patient and all members of the dental team beforehand. Potential adverse long-term changes should be considered and communicated with the patient. This is essential when proposing implant therapy, as is the ability of the clinician to prevent or treat esthetic complications, which must factor into the decision-making process. The individual risk for peri-implantitis, the patient's gingival phenotype, the height of lip line during smiling and at rest, and the patient's chronological as well as skeletal age should be included in the equation prior to constructing a definitive treatment plan. Furthermore, behavioral traits, including parafunctional habits and various psychological disorders, should be considered beforehand. A detailed informed consent must be completed by the patient that mentions all possible side effects that might occur. If an implant treatment is selected, soft- and hard-tissue enhancement and patient education will be beneficial for the long-term esthetic results.
About the Authors
Lior Shapira, DMD, PhD
Betty and D. Walter Cohen Professor for Clinical Periodontal Research, Chair - Department of Periodontology, Hadassah Medical Center, Faculty of Dental Medicine, Hebrew University of Jerusalem, Jerusalem, Israel
Barry P. Levin, DMD
Clinical Associate Professor in Periodontology, University of Pennsylvania, Philadelphia Pennsylvania; Private Practice in Periodontology and Dental Implant Therapy, Jenkintown, Pennsylvania
Ayala Stabholz, DMD
Clinical Professor in Periodontology, Department of Periodontology, Hadassah Medical Center, Faculty of Dental Medicine, Hebrew University of Jerusalem, Jerusalem, Israel
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Zucchelli G, Sharma P, Mounssif I. Esthetics in periodontics and implant-ology. Periodontol 2000. 2018;77(1):7-18.
2. Pjetursson BE, Heimisdottir K. Dental implants - are they better than natural teeth? Eur J Oral Sci. 2018;126(suppl 1):81-87.
3. Fuentealba R, Jofre J. Esthetic failure in implant dentistry. Dent Clin North Am. 2015;59(1):227-246.
4. Fickl S, Zuhr O, Wachtel H, et al. Hard tissue alterations after socket preservation: an experimental study in the beagle dog. Clin Oral Implants Res. 2008;19(11):1111-1118.
5. Romandini M, Lima C, Pedrinaci I, et al. Prevalence and risk/protective indicators of peri-implant diseases: a university-representative cross-sectional study. Clin Oral Implants Res. 2021;32(1):112-122.
6. Frizzera F, Oliveira G, Shibli JA, et al. Treatment of peri-implant soft tissue defects: a narrative review. Braz Oral Res. 2019;33(suppl 1):e073.
7. Chappuis V, Rahman L, Buser R, et al. Effectiveness of contour augmentation with guided bone regeneration: 10-year results. J Dent Res. 2018;97(3):266-274.
8. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005;25(2):113-119.
9. Hermann JS, Buser D, Schenk RK, et al. Biologic width around titanium implants. A physiologically formed and stable dimension over time. Clin Oral Implants Res. 2000;11(1):1-11.
10. Linkevicius T, Apse P, Grybauskas S, Puisys A. Influence of thin mucosal tissues on crestal bone stability around implants with platform switching: a 1-year pilot study. J Oral Maxillofac Surg. 2010;68(9):2272-2277.
11. Benic GI, Scherrer D, Sancho-Puchades M, et al. Spectrophotometric and visual evaluation of peri-implant soft tissue color. Clin Oral Implants Res. 2017;28(2):192-200.
12. Ferrari M, Carrabba M, Vichi A, et al. Influence of abutment color and mucosal thickness on soft tissue color. Int J Oral Maxillofac Implants. 2017;32(2):393-399.
13. Levin BP, Saito H, Reynolds MA, Chu SJ. Changes in peri-implant soft tissue thickness with bone grafting and dermis allograft. Part II: A comparative retrospective case series using a subcrestal angle correction implant design. Int J Periodontics Restorative Dent. 2020;40(4):539-547.
14. Chu SJ, Salama MA, Garber DA, et al. Flapless postextraction socket implant placement, Part 2: The effects of bone grafting and provisional restoration on peri-implant soft tissue height and thickness - a retrospective study. Int J Periodontics Restorative Dent. 2015;35(6):803-809.
15. Kan JY, Rungcharassaeng K, Lozada JL, Zimmerman G. Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. Int J Oral Maxillofac Implants. 2011;26(1):179-187.
16. Hurzeler MB, Zuhr O, Schupbach P, et al. The socket-shield technique: a proof-of-principle report. J Clin Periodontol. 2010;37(9):855-862.
17. Gluckman H, Salama M, Du Toit J. Partial extraction therapies (PET) Part 1: Maintaining alveolar ridge contour at pontic and immediate implant sites. Int J Periodontics Restorative Dent. 2016;36(5):681-687.
18. Chu SJ, Tan-Chu JHP, Saito H, et al. Tapered versus inverted body-shift implants placed into anterior post-extraction sockets: a retrospective comparative study. Compend Contin Educ Dent. 2020;41(5):e1-e10.
19. Nevins M, Benfenati SP, Galletti P, et al. Human histologic evaluations of implants with a unique triangular neck design. Int J Periodontics Restorative Dent. 2020;40(5):657-664.
20. Pluemsakunthai W, Le B, Kasugai S. Effect of buccal gap distance on alveolar ridge alteration after immediate implant placement: a microcomputed tomographic and morphometric analysis in dogs. Implant Dent. 2015;24(1):70-76.
21. Ostman PO, Chu SJ, Drago C, et al. Clinical outcomes of maxillary anterior postextraction socket implants with immediate provisional restorations using a novel macro-hybrid implant design: an 18- to 24-month single-cohort prospective study. Int J Periodontics Restorative Dent. 2020;40(3):355-363.
22. D'Avenia F, Del Fabbro M, Karanxha L, et al. Hard and soft tissue changes in the rehabilitation of the anterior maxilla with triangular shape neck implants: a retrospective clinical study with a one-year follow up. J Biol Regul Homeost Agents. 2019;33(6 suppl):13-21.
23. Li Manni L, Lecloux G, Rompen E, et al. Clinical and radiographic assessment of circular versus triangular cross-section neck implants in the posterior maxilla: a 1-year randomized controlled trial. Clin Oral Implants Res. 2020;31(9):814-824.
24. Odman J, Grondahl K, Lekholm U, Thilander B. The effect of osseointegrated implants on the dento-alveolar development. A clinical and radiographic study in growing pigs. Eur J Orthod. 1991;13(4):279-286.
25. Rossi E, Andreasen JO. Maxillary bone growth and implant positioning in a young patient: a case report. Int J Periodontics Restorative Dent. 2003;23(2):113-119.
26. Westwood RM, Duncan JM. Implants in adolescents: a literature review and case reports. Int J Oral Maxillofac Implants. 1996;11(6):750-755.
27. Cocchetto R, Canullo L, Celletti R. Infraposition of implant-retained maxillary incisor crown placed in an adult patient: case report. Int J Oral Maxillofac Implants. 2018;33(4):e107-e111.
28. Andreasen JO, Borum MK, Jacobsen HL, Andreasen FM. Replantation of 400 avulsed permanent incisors. 4. Factors related to periodontal ligament healing. Endod Dent Traumatol. 1995;11(2):76-89.
29. Thilander B, Odman J, Jemt T. Single implants in the upper incisor region and their relationship to the adjacent teeth. An 8-year follow-up study. Clin Oral Implants Res. 1999;10(5):346-355.
30. Forsberg CM, Eliasson S, Westergren H. Face height and tooth eruption in adults-a 20-year follow-up investigation. Eur J Orthod. 1991;13(4):249-254.
31. Carmichael RP, Sandor GK. Dental implants, growth of the jaws, and determination of skeletal maturity. Atlas Oral Maxillofac Surg Clin North Am. 2008;16(1):1-9.
32. Oesterle LJ, Cronin RJ Jr. Adult growth, aging, and the single-tooth implant. Int J Oral Maxillofac Implants. 2000;15(2):252-260.
33. Bishara SE, Treder JE, Damon P, Olsen M. Changes in the dental arches and dentition between 25 and 45 years of age. Angle Orthod. 1996;66(6):417-422.
34. Cocchetto R, Pradies G, Celletti R, Canullo L. Continuous craniofacial growth in adult patients treated with dental implants in the anterior maxilla. Clin Implant Dent Relat Res. 2019;21(4):627-634.
35. Mijiritsky E, Badran M, Kleinman S, et al. Continuous tooth eruption adjacent to single-implant restorations in the anterior maxilla: aetiology, mechanism and outcomes - a review of the literature. Int Dent J.2020;70(3):155-160.
36. Schwarz F, Derks J, Monje A, Wang HL. Peri-implantitis. J Clin Periodontol. 2018;45(suppl 20):S246-S266.
37. Derks J, Tomasi C. Peri-implant health and disease. A systematic review of current epidemiology. J Clin Periodontol. 2015;42(suppl 16):S158-S171.
38. Song X, Li L, Gou H, Xu Y. Impact of implant location on the prevalence of peri-implantitis: a systematic review and meta-analysis. J Dent. 2020;103:103490.
39. Karlsson K, Derks J, Hakansson J, et al. Interventions for peri-implantitis and their effects on further bone loss: a retrospective analysis of a registry-based cohort. J Clin Periodontol. 2019;46(8):872-879.
40. Bianchini MA, Galarraga-Vinueza ME, Apaza-Bedoya K, et al. Two to six-year disease resolution and marginal bone stability rates of a modified resective-implantoplasty therapy in 32 peri-implantitis cases. Clin Implant Dent Relat Res. 2019;21(4):758-765.
41. Schwarz F, John G, Schmucker A, et al. Combined surgical therapy of advanced peri-implantitis evaluating two methods of surface decontamination: a 7-year follow-up observation. J Clin Periodontol. 2017;44(3):337-342.
42. Heitz-Mayfield LJ, Aaboe M, Araujo M, et al. Group 4 ITI consensus report: risks and biologic complications associated with implant dentistry. Clin Oral Implants Res. 2018;29(suppl 16):351-358.
43. Tomasi C, Regidor E, Ortiz-Vigon A, Derks J. Efficacy of reconstructive surgical therapy at peri-implantitis-related bone defects. A systematic review and meta-analysis. J Clin Periodontol. 2019;46(suppl 21):340-356.
44. Fu PS, Wu YM, Wang JC, et al. Surgical management of severe peri-implantitis in the esthetic zone: a case report with a 6-year follow-up. J Oral Implantol. 2016;42(1):86-92.
45. Thoma DS, Sailer I, Ioannidis A, et al. A systematic review of the survival and complication rates of resin-bonded fixed dental prostheses after a mean observation period of at least 5 years. Clin Oral Implants Res. 2017;28(11):1421-1432.
46. Monje A, Aranda L, Diaz KT, et al. Impact of maintenance therapy for the prevention of peri-implant diseases: a systematic review and meta-analysis. J Dent Res. 2016;95(4):372-379.
47. Thoma DS, Naenni N, Figuero E, et al. Effects of soft tissue augmentation procedures on peri-implant health or disease: a systematic review and meta-analysis. Clin Oral Implants Res. 2018;29(suppl 15):32-49.
48. Staubli N, Walter C, Schmidt JC, et al. Excess cement and the risk of peri-implant disease - a systematic review. Clin Oral Implants Res. 2017;28(10):1278-1290.
49. Raes M, D'Hondt R, Teughels W, et al. A 5-year randomized clinical trial comparing minimally with moderately rough implants in patients with severe periodontitis. J Clin Periodontol. 2018;45(6):711-720.