You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Today, many adult patients' expectations for orthodontic treatment far exceed just straightening of teeth, as most desire to attain favorable function and oral health along with improved facial and dental esthetics.1,2 To that end, so-called "short-face" patients have been considered one of the more challenging groups of patients with regard to achieving their desired goals because they often present with complex facial, smile, and dental problems.3
The "short-face" designation primarily refers to a clinical impression of reduced lower anterior facial height (LAFH). This is an esthetic disharmony in vertical facial proportions rather than a flaw defined by absolute dimension measurements. Usually, the face of a short-face patient appears broad and square in the frontal view. The profile often displays a distinct chin button with a deep labiomental fold and well-developed masseter muscles. Intraorally, though the dentoalveolar relations vary, they usually include crowding, multiple worn/short teeth, and apparent super-eruption of the mandibular incisors with an excessive mandibular curve of Spee. In the past, short-face patients have been described with such characterizations as short-face syndrome, skeletal deep bite, hypodivergent face, and vertical maxillary deficiency. In actuality, short-face patients may be associated with a variety of facial, smile, and dental characteristics depending on the structural etiologies and individual variations.3
Traditional Treatment Options
Currently, dental treatments for short-face patients require consideration of increased LAFH to satisfy patients' expectations of improved facial beauty as part of the final result. Treatment for short-face patients can become complicated when clinicians attempt to deal with all of the contributing problems simultaneously. According to the literature, three different methods traditionally have been employed in these endeavors, each with its own drawbacks.
The first method is the use of orthodontic therapy alone, typically with fixed orthodontic braces, in an attempt to extrude posterior teeth in order to increase vertical dimension, lengthen the face, and correct the associated malocclusion. This approach often has been ineffective in changing the inherent short facial proportions.4,5
The second method has been to combine orthodontics with orthognathic surgery.6-10 While this strategy may solve both facial and smile esthetic problems, dental esthetic concerns might remain. Obviously, inherent surgical risk and complications are associated with this approach.
Third, esthetic contouring procedures in the lower face may include masseteric injections of botulinum toxin, autologous chin fat grafting, mandibular reduction angleplasty contouring, and/or possibly genioplasty.11 These approaches deal only with some facial esthetic issues but do not necessarily address smile and dental esthetic issues, which could still remain after treatment.
Each of the aforementioned methods is incapable of completely correcting all facial, smile, and dental esthetic problems at the same time. Instead, an interdisciplinary treatment (IDT) approach with global esthetic considerations may serve as an effective alternative.
Traditional IDT has involved mainly prosthetically driven treatment planning based on mostly dental diagnosis (eg, periodontal/endodontic status, restorative spaces, occlusal relationships, etc) without consideration for the correct correspondence of teeth position to the patient's jaws so as to enhance overall esthetics (ie, face, smile, and dental esthetics, with dental esthetics equaling pink/white esthetics). Therefore, traditional IDT may not be suitable for short-face patients with high facial esthetic demands when they have complex facial, smile, and dental situations.
Modern esthetic interdisciplinary treatment (E-IDT) is basically an overall esthetics-driven treatment planning approach based on a global diagnosis rather than primarily a dental diagnosis, while still taking into consideration the achievement of good health and function. Factors comprising a global diagnosis include but are not limited to facial proportions, smile, dental problems, occlusion, skeletal relationship, nose/lip/chin patterns, airways, and the teeth position correctly and esthetically corresponding to the patient's jawbones, mouth, and face. Thus, the E-IDT approach may be an effective way to meet a short-face patient's esthetic desire, especially when facial beauty improvement is a priority of the patient.
To illustrate this approach, a clinical case of a female patient with complex facial, smile, and dental esthetic problems is presented. The patient not only wanted her dental problems resolved but also desired facial esthetic improvements, which traditionally would have been done through cosmetic surgery. In this case, a nonsurgical E-IDT approach that included a combination of orthodontic, prosthodontic, periodontal, and implant therapy was utilized to achieve an optimal esthetic treatment outcome and maintain a long-term stable result.
Sequence and Goals of E-IDT Approach
Step 1: Facial esthetics—The first step of E-IDT is to increase the patient's LAFH to achieve a harmonic facial proportion (ie, soft-tissue ratio of upper anterior facial height [UAFH] to LAFH of 50% to 50%). The lower one-third of the facial height is strongly related to the vertical dimension of occlusion (VDO); therefore, increasing VDO could immediately increase LAFH for short-face patients to dramatically improve their facial and perioral esthetics.12-14 Increasing VDO may be accomplished by using orthodontic therapy combined with prosthodontic treatment and/or dental implants.
In some cases, to achieve an ideal harmonic facial proportion, orthognathic surgery and/or cosmetic procedures (eg, genioplasty, chin fat grafting, chin implant, or mandibular reduction angleplasty) might be needed to attain optimal LAFH and jaw line. Some examples of such short-face cases might include a skeletal class I case with retruded chin projection/chin deviation/prominent mandibular angle; skeletal class II case with protrusive maxilla and retrusive mandible/chin deviation; skeletal class III case with retrusive maxilla and protrusive mandible/chin deviation/prominent mandible angle; or skeletal class I/II/III case with facial asymmetry due to maxilla/mandible horizontal bony discrepancies.
Step 2: Smile esthetics—Addressing smile esthetics is the next step of E-IDT, as smile design is a critical element in the process. Tooth size, shape, and proportion (width/length), incisal edge position, gingival margin, and smile lines in the anterior all must be taken into consideration in relation to the patient's facial profile, shape and length of lips, and posed smile movement. An interdisciplinary approach involving various dental specialists and/or cosmetic procedures will be needed to achieve optimal smile esthetics.
Step 3: Dental esthetics—The final step is to obtain a pleasing esthetic appearance of the patient's teeth, including shade, morphology, and other general features, in conjunction with an ideal functional occlusion.
All of these considerations are taken into account to generate a thorough treatment plan and establish a facial and smile esthetic framework to achieve the best possible result. The following case report demonstrates these E-IDT steps.
Case Report
Clinical Examination
A 50-year-old female patient presented desiring to simultaneously correct her short, square face; unesthetic smile; upper front teeth, particularly the color and shape; and large overjet. She specifically inquired about orthodontic treatment as a resolution to her problems.
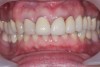
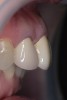
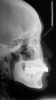
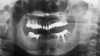
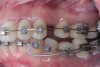
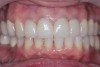
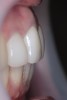
Clinical examination revealed an acute nasolabial angle, a protrusive lateral profile, and a marked short, square face (Figure 1 through Figure 3). Facial esthetics were dominated by a short LAFH with a UAFH/LAFH ratio of 54%/46% (Figure 3). Intraoral examination demonstrated bilateral class II canine and molar relationships, a 10 mm overjet and 3 mm overbite, and a deep curve of Spee of the lower dentition (Figure 4 through Figure 6). Most of her upper teeth and lower posterior teeth were crowned, with the exceptions being the upper right canine (No. 6) and upper left second molar (No. 15). Her lower right second premolar to second molar (Nos. 29 through 31) were restored with a prosthetic bridge, and her lower left second premolar (No. 20) and second molar (No. 18) were restored with crowns. Additionally, she had a dental implant in the lower left first molar (No. 19) position (Figure 7). Her upper anterior crowns had unpleasant tooth proportion, morphology, and shade.
The periodontal status and oral hygiene were acceptable except for the lower left second molar (No. 18), whose status was poor. Adequate width of keratinized tissue was present throughout the patient's dentition. A buccal bony defect was noted over the edentulous ridge at tooth No. 30 due to long-term tooth missing.
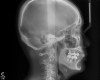
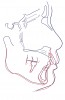
From radiographic examination, tooth No. 18 was found to have a poor prognosis due to furcation bone loss. The cephalometric x-ray showed a skeletal class II relationship, a reduced mandibular plane angle, flared upper incisors, a deep bite, and significant overjet (Figure 6). The panoramic radiograph confirmed many restorations and that No. 19 was a dental implant (Figure 7). There were no symptoms of temporomandibular joint disorder.
E-IDT Treatment Plan
Although a lower-face esthetic contouring procedure was first recommended by a plastic surgeon and would have addressed the patient's facial esthetic concerns, it was deemed not suitable because of the many other dental issues, as outlined above. Moreover, the patient refused to undergo cosmetic surgery due to the risks and possible complications, such as hematoma, infection, condyle fracture, and facial nerve palsy. Consequently, a nonsurgical E-IDT treatment plan was formulated as follows:
To address and enhance facial esthetics, the initial stage would involve increasing the LAFH by opening the VDO using a temporary crown on the No. 19 dental implant. This would be followed by orthodontic extrusion of bilateral lower posterior teeth, specifically the lower first and second premolars and second molars (Nos. 18, 20, 21, 28, 29, and 31). The final stage of the facial esthetic portion of the treatment plan involved prosthetic crown fabrication for the posterior teeth. To correct the protrusive lateral profile, orthodontic treatment was performed and teeth Nos. 5 and 12 were extracted to provide space for upper anterior teeth retraction.
To improve smile esthetics, orthodontic and prosthetic treatment as well as an esthetic crown lengthening procedure were performed to modify the alignment, size, proportion, and shape of teeth, the gingival margin, and the smile line of the upper front teeth.
Dental esthetics was addressed using orthodontic treatment to align all teeth to be in class I occlusion with ideal overjet and overbite. Implant treatment was used to restore missing teeth Nos. 18 and 19 and to augment the buccal bony defect over No. 30. The dental esthetic portion of the plan also included a teeth whitening procedure and prosthetic treatment to brighten the teeth shade and fabricate crowns for all implants to support the newly established VDO and LAFH.
Progression of Treatment
Prior to orthodontic treatment, all existing crowns were replaced by temporary crowns with proper size and shape. Disease control, including treatments for caries, periodontal disease, and pathological periapical lesions, was completed. Two months into orthodontic treatment, the No. 19 implant temporary crown was intentionally fabricated in a higher occlusal stop to increase the patient's VDO and allow orthodontic extrusion of bilateral lower posterior teeth. The No. 19 implant could serve as not only a bite opening anchor but also an excellent anchor for subsequent orthodontic intrusion-proclination of lower anterior teeth (Figure 8). Tooth No. 18 was extracted during the orthodontic treatment due to its poor prognosis.
Six months after orthodontic treatment, the original large overjet and deep bite were almost corrected. However, thick protuberance of alveolar bone, uneven gingival margins, and an unpleasant tooth proportion of the upper front teeth were noticed. To correct these problems, esthetic crown lengthening on the upper anterior teeth, Nos. 6 through 11, was recommended and performed. After the crown lengthening procedure, temporary crowns were refabricated to mimic ideal size and width/length ratio. Upon completion of orthodontic treatment, dental implant fixtures for Nos. 18 and 30 were inserted; No. 30 also underwent a guided bone regeneration procedure to augment the buccal bony defect. Eventually, new definitive prostheses for all crowns and implants were fabricated and delivered after teeth whitening treatment.
Treatment Results
Post-treatment records showed a dramatic improvement in the patient's profile, smile, and dental esthetics and occlusion. The modified VDO had significantly increased the LAFH to achieve better facial proportion (UAFH/LAFH ratio of 50%/50%) and caused the depression of her chin to become shallower (Figure 9 and Figure 10). Intraorally, class I occlusion with well-aligned arch form and ideal overjet and overbite, esthetic upper anterior teeth size and proportion, good gingival margins, and proper prosthetic restorations were all achieved (Figure 11 and Figure 12).
Cephalometric superimposition showed almost complete bodily retraction of the upper anterior teeth and intrusion-proclination of the lower anterior teeth. The upper and lower molars demonstrated extrusion of the coronal portions as a result of prosthetic crown fabrication, resulting in a clockwise rotation of the mandible (Figure 13 and Figure 14). The vertical dimension was successfully increased by 3 mm, and LAFH was improved.
After 5 years' follow-up, the patient's profile and occlusion were still well maintained. The patient was extremely pleased and satisfied with the treatment outcome and also appreciative of not needing to have cosmetic surgery (Figure 15).
Discussion
Patients today often have high demands for not only dental and smile esthetic outcomes but also for facial esthetics through their dental treatment. In the case presented, the patient had great expectations for improving her short, square face. A nonsurgical E-IDT plan was carefully scrutinized and implemented and led to a successful final result.
Altering VDO is a debatable controversy in the dental profession.15-18 Spear and colleagues stated that VDO is a highly adaptable position and that many VDOs may be successful; they added that it is sensible to choose the VDO that satisfies both the patient's esthetic goals and the clinician's functional goals.19 Abduo suggested that permanent increase of VDO up to 5 mm is a safe and predictable procedure without detrimental consequences. Associated signs and symptoms that coincide with the increase in VDO in short-face cases are self-limiting and tend to resolve within 2 weeks.20 Therefore, increasing VDO is considered an effective and safe strategy when implementing E-IDT cases to meet both esthetic and functional needs.
To achieve optimal esthetic results, the authors recommend all-ceramic restorations in most E-IDT cases. Full-contoured zirconia and monolithic lithium disilicate have the favorable features of high compression strength and wear resistance, which are typically advantageous for occlusal support and long-term stability of final occlusion, especially for posterior teeth. The selection of restoration material can play an important role in long-term success.
Conclusion
This clinical report has described the esthetic interdisciplinary management of a short-face female patient who had numerous complex clinical issues and high esthetic expectations. The E-IDT treatment comprised a combination of therapies, including orthodontics, implant placement, periodontics, and prosthodontics, to achieve restorative correction. The E-IDT approach offers a novel alternative option for treating short-face adult patients who desire a slim lower face yet refuse cosmetic surgery.
About the Authors
James Cheng-Yi Lin, DDS
Clinical Assistant Professor, Department of Orthodontics and Pediatric Dentistry, School of Dentistry, National Defense Medical University, Taipei, Taiwan; Private Practice specializing in Orthodontics and Implantology, Taipei, Taiwan
Ching-Ling Chang, DDS, MS
Private Practice specializing in Prosthodontics, Taipei, Taiwan
Stacy Chen, DDS
Private Practice specializing in Orthodontics, Taipei, Taiwan
Eric Jein-Wein Liou, DDS, MS
Chairman, Faculty of Dentistry, Chang-Gung Memorial Hospital, Taipei, Taiwan; Associate Professor, Institute of Craniofacial Medicine, Chang-Gung University, Taipei, Taiwan
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Burrow SJ. Biomechanics and the paradigm shift in orthodontic treatment planning. J Clin Orthod. 2009;43(10):635-644.
2. Kois JC. Diagnostically driven interdisciplinary treatment planning. In: Cohen M, ed. Interdisciplinary Treatment Planning: Principles, Design, Implementation. Chicago, IL: Quintessence Publishing; 2008:190-212.
3. Opdebeeck H, Bell WH. The short face syndrome. Am J Orthod. 1978;73(5):499-511.
4. Turley PK. Orthodontic management of the short face patient. Semin Orthod. 1996;2(2):138-153.
5. Vaden JL. Alternative nonsurgical strategies to treat complex orthodontic problems. Semin Orthod. 1996;2(2):90-113.
6. Bell WH. Correction of the short-face syndrome-vertical maxillary deficiency: a preliminary report. J Oral Surg. 1977;35(2):110-120.
7. Freihofer HP. Surgical treatment of the short face syndrome. J Oral Surg. 1981;39(11):907-911.
8. Wessberg GA, Fish LC, Epker BN. The short face patient: surgical-orthodontic treatment options. J Clin Orthod. 1982;16(10):668-685.
9. Arnett GW, Kreashko RG, Jelic JS. Correcting vertically altered faces: orthodontics and orthognathic surgery. Int J Adult Orthodon Orthognath Surg. 1998;13(4):267-276.
10. Watted N, Bartsch A. Esthetic aspects of orthodontic-surgical treatment of sagittal-vertical anomalies: the example of the short face syndrome. J Orofac Orthop. 2002;63(2):129-142.
11. Chang CS, Kang GC. Achieving ideal lower face aesthetic contours: combination of tridimensional fat grafting to the chin with masseter botulinum toxin injection. Aesthet Surg J. 2016;36(10):1093-1100.
12. Mack MR. Perspective of facial esthetics in dental treatment planning. J Prosthet Dent. 1996;75(2):169-176.
13. Mack MR. Vertical dimension: a dynamic concept based on facial form and oropharyngeal function. J Prosthet Dent. 1991;66(4):478-485.
14. Mack MR. Facially generated occlusal vertical dimension. Compend Contin Educ Dent. 1997;18(12):1183-1190.
15. Kokich VG. Altering vertical dimension in the perio-restorative patient: the orthodontic possibilities. In: Cohen M, ed. Interdisciplinary Treatment Planning: Principles, Design, Implementation. Chicago, IL: Quintessence Publishing; 2008;50-80.
16. Bloom DR, Padayachy JN. Increasing occlusal vertical dimension-why, when and how. Br Dent J. 2006;200(5):251-256.
17. Kois JC, Phillips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1177.
18. Moreno-Hay I, Okeson JP. Does altering the occlusal vertical dimension produce temporomandibular disorders? A literature review. J Oral Rehabil. 2015;42(11):875-882.
19. Spear F, Kinzer G. Approaches to vertical dimension. In: Cohen M, ed. Interdisciplinary Treatment Planning: Principles, Design, Implementation. Chicago, IL: Quintessence Publishing; 2008:249-281.
20. Abduo J, Lyons K. Clinical considerations for increasing occlusal vertical dimension: a review. Aust Dent J. 2012;57(1):2-10.