You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
As reviewed in part 1 of this article (Compendium, April 2019),1 while standard osteotomy drilling using traditional "cutting" drills removes bone from a dental implant site, osseodensification (OD) utilizes a significantly different approach. OD is essentially a burnishing process whereby burs with specially designed flutes rotating counterclockwise redistribute autogenous bone contained within the osteotomy back onto the bony surface through plastic deformation. The counterclockwise rotation of the OD bur causes the lands of the bur to slide across the surface of the bone by means of low plastic deformation; the burs are purposefully designed with a compressive force less than the ultimate strength of bone. OD burs offer the clinician many reported advantages as highlighted in part 1, including the ability to achieve primary implant stability in cases where previously it may not have been obtainable.1
The focus of this second article is on the clinical uses and indications for OD. While OD is generally accepted as a safe method, it is important for clinicians to understand that with this technique it is possible to over-compress bone, which can potentially lead to necrosis. Therefore, the densification of dense cortical bone is prone to mechanical sensivity and, as a result, apoptosis of osteocytes.2-5 Consequently, clinicians should become familiar with this technology before employing it and must utilize the burs in the correct manner depending on bone density.
Three cases are presented that highlight the clinical indications supporting the use of OD and discuss relevant protocols. These include a lateral sinus augmentation procedure, a crestal sinus augmentation procedure in combination with the use of a synthetic bone putty, and a socket-shield technique in the esthetic zone. This article is intended to provide clinicians a better understanding of OD and how to optimize the technique and underscore its clinical advantages in cases where initial bone density has been compromised. In such cases, enhanced primary stability may be obtained when it would otherwise not be possible with conventional burs.
Case 1: Use of Osseodensification for a Lateral Sinus Augmentation Procedure
In this first case, OD burs were used at a site requiring maxillary sinus augmentation, an area that is frequently associated with low-density bone. A 60-year-old female patient presented with missing posterior teeth in the right maxillary quadrant. Clinical and cone-beam computed tomography (CBCT) evaluation revealed a partially pneumatized maxillary right sinus with residual bone height of 5 mm (Figure 1 and Figure 2). A lateral sinus augmentation procedure was planned as a result of the minimal residual bone height present and would include simultaneous placement of two implants (one-stage).
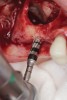
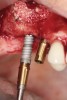
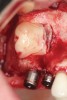
A lateral sinus window was created using a combination of a round fissure bur and piezosurgery device tip (Figure 3). The elevation of the Schneiderian membrane was also performed with a piezosurgery device along with hand instruments (Figure 4). A type 1 bovine cross-linked collagen membrane (Mem-Lok®, BioHorizons, biohorizons.com) soaked in liquid platelet-rich fibrin (PRF) was placed over the Schneiderian membrane along with two PRF membranes prior to the use of OD burs (Figure 5). The OD burs were then utilized to densify bone on the osteotomy walls (Figure 6). The bone graft, composed of a 50/50 mixture of cortico-cancellous allograft and xenograft mixed with PRF fragments, was used to fill the bone defect in the sinus, followed by implant placement (Figure 7). Primary implant stability was measured at 60 Ncm. Lastly, a collagen membrane was placed over the lateral window with fixation and covered by two PRF membranes to enhance soft-tissue healing (Figure 8). Primary closure was obtained using 3.0 polytetrafluoroethylene (PTFE) sutures (Figure 9).
In summary, this case demonstrates a typical indication for OD burs. The posterior maxilla is routinely associated with low-density bone, and therefore its densification optimized primary implant stability by favoring the accumulation of autogenous cancellous bone from the osteotomy site, redistributing this bone along the implant osteotomy walls as opposed to it being removed, as would be the case if standard drilling was used.
Case 2: Use of Osseodensification During Crestal Sinus Augmentation in Combination With Bone Putty
The second case using OD burs involved a right maxillary sinus with partial pneumatization and a residual bone height of 5 mm. The treatment plan included utilizing a crestal approach for sinus grafting with alloplast bone putty and simultaneous (one-stage) implant placement using OD burs.
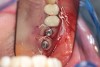
Figure 10 shows a missing maxillary left first bicuspid tooth. An envelope incision with full flap reflection was used to reveal division A ridge width.6 OD burs were then used to create an implant osteotomy (Figure 11). As per protocol, appropriate osteotomy diameter was created with the successive use of OD burs followed by the application of a bone grafting putty (NovaBone®, NovaBone Products, LLC, novabone.com) via the crestal osteotomy. The bone putty was introduced to the site (Figure 12), and OD burs were used to propel the graft apically beneath the sinus membrane (Figure 13). Implant placement was performed and the flaps were sutured closed with 3.0 PTFE sutures (Figure 14). The additional bone graft at the apical portion of the implant site after implant placement was demonstrated through a series of intraoperative x-rays (Figure 15).
Case 3: Use of Osseodensification During a Socket-Shield Technique in Esthetic Zone
In a third case, OD burs were utilized as part of a socket-shield procedure (also known as root-membrane technique) for extraction and immediate implant placement in the esthetic zone. Briefly, use of this technique leaves a portion of the buccal root surface intact prior to implant placement in order to support maintenance of buccal tissues in the esthetic zone.7-10
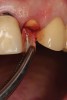
A 65-year-old male patient presented to the office with a fractured maxillary left lateral incisor (Figure 16). Radiographic analysis revealed minimal buccal bone. Having deemed the tooth nonrestorable, the clinician presented several options to the patient, which they carefully reviewed together. A socket-shield approach was selected with the goal of maintaining existing gingival zenith long-term.
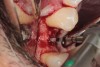
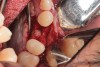
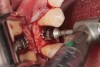
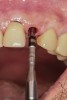
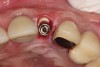
Appropriate rotary burs were used to section the tooth in half in the mesial-distal direction, followed by careful removal of the palatal root half (Figure 17). Next, the remaining labial root was contoured to a thickness of approximately 1.5 mm followed by removal of the apical third (Figure 18). OD burs were then utilized to densify the bone in the osteotomy via lateral bone displacement (Figure 19). A bone grafting putty (Novabone) was placed into the osteotomy and the implant was then inserted with a primary implant stability reading of 60 Ncm (Figure 20). Typically, mineralized allograft is the preferred choice for grafting between the implant body and facial root.
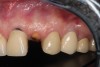
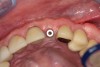
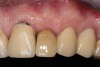
After 2 weeks, excellent soft-tissue healing and maintenance of the labial gingival tissue was evident. The same was true after 3 months (Figure 21). The gingival zenith continued to be maintained after 1.5 years (Figure 22). Importantly, the facial wall bone thickness of the implant also was maintained at the 1.5-year follow-up (Figure 23), suggesting favorable maintenance of this case.
Discussion
The initial biomechanical stability of dental implants usually depends on a number of factors. Implant macro and micro design and quality and quantity of surrounding bone have been important parameters during initial implant stability.3 The aforementioned first article on this concept discussed the biological background relating to the use of OD.1 The present article focuses primarily on its clinical uses and indications.
The use of OD burs promotes the accumulation of autogenous bone along the internal component of implant osteotomy sites.11 As a result, bone volume within the osteotomy site as well as bone-to-implant contact and primary implant stability may be increased. By preserving bone volume within the defect, an acceleration of implant stability and osseointegration has been reported both in preclinical and clinical models.11-18
Nevertheless, some disadvantages of this technique must be noted. For example, during bone compaction and implant loading under high torque, bone is subject to a micro-damage threshold. It has previously been shown by Frost et al that if the bone's micro-damage threshold is exceeded, the bone remodeling cycle may require an additional 3 months or more to repair these damaged areas.19 This is particularly important in relation to OD since over-compression may also unintentionally cause bone necrosis.20
Therefore, case selection for using OD burs in counterclockwise mode is important as the procedure is not recommended in dense bone (D1, D2). Furthermore, it is most important to not undersize the implant osteotomy with the use of OD as this could result in bone necrosis and implant failure. In this case series, the procedures were performed in the maxilla where lower bone density is observed as compared to the mandible. Moreover, in the case involving the socket shield (case 3) no crestal bone compression was observed at all.
Incorrect use of this technology may lead to implant failure that would otherwise not have occurred with the use of standard conventional burs. Clinicians are cautioned that there is an upper limit to how much bone can be compressed/densified. Future research aimed at better understanding this upper limit is needed. It is noteworthy and imperative that the treating clinician be appropriately trained with this technology prior to clinical use. The following clinical guidelines may enhance a practitioner's understanding of the technique:
- This technique has been shown to have clinical safety characteristics similar to conventional drilling when proper rotary speed, penetration speed, and irrigation are used.12
- The bone mineral density of the osseous densification sites is increased by both compaction and autografting of bone along the periphery and at the apex of the osteotomies.11
- The percentage of bone at the implant surface increases similarly in osseous densification sites as compared with sites achieved with standard drilling or extraction drilling.11
- Trabecular bone compaction produced during the osseous densification technique creates a smaller osteotomy site than conventional drilling due to spring-back recovery of viscoelastic deformation when the OD bur is removed from the osteotomy.11
- By using the osseous densification technique to preserve bone volume, faster primary stability can be achieved, which supports immediate loading.17
- Caution should be taken when using OD burs in dense bone such as cortical bone. Here the burs are used in clockwise (cutting) mode. Over-compression has been shown to lead to bone necrosis and as a result, implant failure may occur.20
Conclusion
Osseodensification represents a novel implant osteotomy technique that has been shown to preserve bone volume through the compaction of cancellous bone due to the inherent bone properties of viscoelasticity and plastic deformation. The use of OD burs offers the ability to obtain primary stability in cases where it previously may not have been obtainable. This method has been shown to be effective for a variety of clinical indications when utilized in low-density bone. In the present article, three clinical cases/indications were described, including the use of OD during a lateral sinus augmentation procedure, a crestal approach in combination with bone graft, and in conjunction with a socket-shield technique. Because the use of OD burs in implant dentistry is in its early development, it is advised that proper clinical training be obtained prior to implementation of this technology into practice.
About the Authors
Michael A. Pikos, DDS
Oral Maxillofacial Surgeon, CEO, Pikos Institute, Tampa, Florida
Richard J. Miron, Dr. med. dent., DDS, PhD
Adjunct Professor, Periodontology, Nova Southeastern University,
Fort Lauderdale, Florida
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Pikos MA, Miron RJ. Osseodensification: an overview of scientific rationale and biological background. Compend Contin Educ Dent. 2019;40(4):217-222.
2. Insua A, Monje A, Wang HL, Miron RJ. Basis of bone metabolism around dental implants during osseointegration and peri-implant bone loss. J Biomed Mater Res A. 2017;105(7):2075-2089.
3. Meyer U, Vollmer D, Runte C, et al. Bone loading pattern around implants in average and atrophic edentulous maxillae: a finite-element analysis. J Craniomaxillofac Surg. 2001;29(2):100-105.
4. Bertollo N, Walsh WR. Drilling of bone: practicality, limitations and complications associated with surgical drill-bits. In: Klika V, ed. Biomechanics in Applications. London, UK: InTech; 2011.
5. Cha JY, Pereira MD, Smith AA, et al. Multiscale analyses of the bone-implant interface. J Dent Res. 2015;94(3):482-490.
6. Misch CE, Judy KW. Classification of partially edentulous arches for implant dentistry. Int J Oral Implantol. 1987;4(2):7-13.
7. Du Toit J, Gluckman H. The modified socket-shield technique. J Craniofac Surg. 2018;29(7):2005-2006.
8. Gluckman H, Nagy K, Du Toit J. Prosthetic management of implants placed with the socket-shield technique. J Prosthet Dent. 2018. doi: 10.1016/j.prosdent.2018.06.009.
9. Gluckman H, Salama M, Du Toit J. A retrospective evaluation of 128 socket-shield cases in the esthetic zone and posterior sites: partial extraction therapy with up to 4 years follow-up. Clin Implant Dent Relat Res. 2018;20(2):122-129.
10. Siormpas KD, Mitsias ME, Kotsakis GA, et al. The root membrane technique: a retrospective clinical study with up to 10 years of follow-up. Implant Dent. 2018;27(5):564-574.
11. Trisi P, Berardini M, Falco A, Podaliri Vulpiani M. New osseodensification implant site preparation method to increase bone density in low-density bone: in vivo evaluation in sheep. Implant Dent. 2016;25(1):24-31.
12. Lahens B, Lopez CD, Neiva RF, et al. The effect of osseodensification drilling for endosteal implants with different surface treatments: a study in sheep. J Biomed Mater Res B Appl Biomater. 2019;107(3):615-623.
13. Lahens B, Neiva R, Tovar N, et al. Biomechanical and histologic basis of osseodensification drilling for endosteal implant placement in low density bone. An experimental study in sheep. J Mech Behav Biomed Mater. 2016;63:56-65.
14. Oliveira PG, Bergamo ET, Neiva R, et al. Osseodensification outperforms conventional implant subtractive instrumentation: a study in sheep. Mater Sci Eng C Mater Biol Appl. 2018;90:300-307.
15. Tian JH, Neiva R, Coelho PG, et al. Alveolar ridge expansion: comparison of osseodensification and conventional osteotome techniques. J Craniofac Surg. 2018. doi: 10.1097/SCS.0000000000004956.
16. Witek L, Neiva R, Alifarag A, et al. Absence of healing impairment in osteotomies prepared via osseodensification drilling. Int J Periodontics Restorative Dent. 2019;39(1):65-71.
17. Huwais S, Mazor Z, Ioannou AL, et al. A multicenter retrospective clinical study with up-to-5-year follow-up utilizing a method that enhances bone density and allows for transcrestal sinus augmentation through compaction grafting. Int J Oral Maxillofac Implants. 2018;33(6):1305-1311.
18. Huwais S, Meyer EG. A novel osseous densification approach in implant osteotomy preparation to increase biomechanical primary stability, bone mineral density, and bone-to-implant contact. Int J Oral Maxillofac Implants. 2017;32(1):27-36.
19. Frost HM. A brief review for orthopedic surgeons: fatigue damage (microdamage) in bone (its determinants and clinical implications). J Orthop Sci. 1998;3(5):272-281.
20. Wang L, Wu Y, Perez KC, et al. Effects of condensation on peri-implant bone density and remodeling. J Dent Res. 2017;96(4):413-420.