You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
As oral physicians, dentists should always strive to provide the best clinical treatment for their patients. To be a good clinician, a dentist must be a good diagnostician. However, beginning as early as dental school training, the tendency among clinicians is to make pretreatment endodontic (pulpal status) and periradicular (status of gingival and tooth-supporting tissues) diagnoses only when patients present in pain. Even in these clinical scenarios, dentists might not perform all of the necessary clinical objective tests to determine the correct pretreatment endodontic and periodontal diagnosis. The clinical importance of making a pretreatment pulpal and periapical diagnosis when performing non-emergency-type dental treatment typically is not emphasized in dental school curricula. A practical example of this is when a clinician performs restorative treatment, especially in cases of caries removal.
This article, therefore, is intended to provide an overview of current clinical endodontic and periodontal diagnostic terminologies and demonstrate their clinical applications in restorative dental treatment.
Diagnosis
The pretreatment pulpal and periradicular diagnosis of a tooth begins with a review of the patient's medical and dental history. This also should include a recording of the patient's blood pressure, pulse, and, if indicated, temperature. If a patient presents in pain, the pain etiology must be identified before any emergency dental treatment is performed. The first step in determining the pain etiology is listening to the patient's perception of the problem (subjective), which is followed by clinical testing (objective) by the dentist to reproduce the patient's subjective pain symptoms.
If a patient presents with an asymptomatic dental condition, as is often the case in restorative dentistry, the same objective testing (as described below) needs to be completed to properly make a pretreatment pulpal and periradicular diagnosis. With regard to clinically performing objective testing, there may be uncertainty among clinicians as to which test should be performed in order to arrive at a proper pretreatment pulpal and periradicular diagnosis. The following five objective clinical tests should be conducted to determine the pulpal and periradicular diagnosis. The authors recommend performing all five tests in every case, though in no particular order.
Five Objective Clinical Tests
Pulp Sensibility: Cold, Electric Pulp Test, and/or Hot
Pulp sensibility tests (thermal and electric) have been used to indirectly determine the state of pulpal health by assessing the condition of the dental pulp nerves. Pulp vitality testing, on the other hand, is the direct assessment of pulp blood flow1 and may be performed using laser doppler flowmetry (LDF) or pulse oximetry (PO). Clinicians often use pulp sensibility tests rather than pulp vitality tests because of the limitations of LDF and PO in dental applications, as these instruments can be complicated to use and require strict adherence to the respective application techniques in order to achieve proper vitality readings.1
It should be noted that heat and cold tests do not jeopardize the health of pulp.2 Also, teeth with porcelain or metal crowns do conduct temperature and, therefore, can be tested for pulpal sensibility with cold or heat.3 Clinicians may often be unsure of what the numerical readings on an electric pulp tester (EPT) represent. Although the use of an EPT can establish pulp sensibility, the numerical readout should not be used to determine the overall health of the pulp.4 For example, if tooth No. 8 has an EPT reading of "12" and tooth No. 9 has an EPT reading of "24," it does not mean that tooth No. 8 should be considered twice as vital as tooth No. 9. The EPT is used to determine whether or not the pulp is vital. When using an EPT, the clinician should be aware that teeth with metal restorations may give false-positive or false-negative responses.4
Weisleder et al reported that cold test and EPT used in conjunction resulted in a more accurate method for proper pulpal diagnostic testing.5 In another study, Jespersen et al reported that pulp testing with cold spray (Endo Ice®, Coltene, coltene.com) and EPT are accurate and reliable methods of determining pulpal sensibility.6
Percussion Tests to Determine Status of Periodontal Ligament
Percussion testing, performed by tapping the buccal tooth surface with a hard instrument-such as the opposite end of a dental mirror-to test the clinical status of the periodontal ligament (PDL),may often be mistakenly used to directly correlate a pulp's sensibility.7 Although a tooth's sensitivity to percussion testing might be due to a pulpitis or pulpal necrosis, it is only an indirect association. This particular test only helps determine the status of the PDL. A bite test also may need to be performed if a patient complains about pain upon mastication.
Palpation of Buccal and Lingual/Palatal Gingival Tissue
Palpation examination is used to test for sensitivity of the gingival tissue of the tooth in question and for infection and/or inflammation of the cortical and medullary bone. It should be noted that even if there is no radiographic evidence of an apical infection, clinically an infection may be present. In a study, Bender et al reported that extensive disease of the bone is not uncommon even when no evidence of it exists on a radiograph.8
Periodontal Examination: Probings and Tooth Mobility
Periodontal disease can develop anywhere around a tooth; therefore, the entire circumference of the tooth or teeth must be probed. When evaluating tooth mobility, clinicians must be aware that the mobility of the tooth can be either endodontic or periodontal in nature. In the case of periodontal disease, a tooth becomes mobile and loose as the attachment apparatus and surrounding bone are destroyed. Generalized mobility involving multiple teeth usually suggests the problem is periodontal in origin. In acute endodontic infection, the tooth mobility is generally associated with an isolated tooth.9
Current Radiographic Examination
Radiographic examination may include periapical x-rays, bitewings, and/or cone-beam computed tomography (CBCT). Uraba et al reported that CBCT imaging is effective at detecting approximately 20% more periapical lesions compared to periapical radiographs, particularly in maxillary anterior and posterior teeth.10
When a patient presents for restorative treatment and reports that the tooth is asymptomatic, the dentist might be inclined to assume that the pulp and periradicular diagnosis is within normal limits. Hence, the dentist may bypass the aforementioned objective clinical tests though may still take a radiograph. However, using only a dental radiograph to determine the etiology of tooth pain or pretreatment pulpal and periradicular status may lead to a pulpal and periradicular misdiagnosis. Therefore, the authors suggest that the five objective tests be performed to obtain an accurate pretreatment pulpal and periradicular diagnosis.
Pulpal Diagnosis
The pulpal nerve fibers A-delta (which respond to cold and EPT) and C-fibers (which respond to hot and provide the nerve response when a patient reports spontaneous tooth pain) are nociceptors, which are sensory receptors that respond to stimuli by sending nerve signals to the brain. This stimulus can cause the perception of pain in an individual.11 By objectively testing the pulpal nerve fibers, a dentist can best determine the pulpal status.
Current pulpal diagnosis terminologies are identified and discussed in the following paragraphs.12
Normal pulp is the term used when pulp responds within normal limits to cold. Clinically, in this scenario a patient will respond to cold stimulus, and after the stimulus is removed the cold sensation will dissipate immediately. It should be noted that the time it takes for a patient to respond to cold has no correlation to the diagnosis and, therefore, does not need to be recorded.
Reversible pulpitis is pain from an inflamed pulp that can be treated without the removal of the pulp tissue. This is not a disease, but a symptom. A classic clinical symptom of reversible pulpitis is sharp, quick pain that subsides as soon as stimulus is removed. Physiologically, it is the A-delta fibers that are firing, not the C-fibers of the pulp.13 A-delta fibers are the myelinated, low-threshold, sharp/pricking pain nerve fibers that reside principally in the pulp-dentin junction. They are stimulated by cold and EPT and cannot survive in a hypoxic (low oxygen) environment. Reversible pulpitis does not involve unprovoked (spontaneous) response.
Symptomatic irreversible pulpitis is an inflamed pulp that cannot be treated except by the removal of the pulp tissue. Classic clinical symptoms of this condition are the lingering of cold/hot stimulus for more than 5 seconds and/or spontaneous tooth pain as reported by the patient. Physiologically, the A-delta fibers and/or the C-fibers fire neural impulses. C-fibers are the unmyelinated, high-threshold, aching pain nerve fibers. They are distributed throughout the pulp, are stimulated by heat, and can survive in a hypoxic environment.
Asymptomatic irreversible pulpitis is a vital pulp that is incapable of healing and for which endodontic treatment is indicated. Although a histological diagnosis is needed to determine the inflammatory extent of the pulp, two clinical examples of this diagnosis are a pulp polyp and internal resorption.
Pulpal necrosis may result from an untreated irreversible pulpitis or occur immediately after a traumatic injury that disrupts the vascular system of the pulp. A necrotic pulp does not respond to cold tests, EPT, or heat tests.
Previously treated is a term used to describe a tooth that has already been endodontically treated.
Previously initiated therapy describes a tooth that had endodontic treatment started, but the treatment was not completed with obturation.
Periradicular Diagnosis
When clinicians engage in restorative treatment, just as they often do not obtain a pulpal diagnosis, it is commonly known that they similarly usually neglect to procure a periradicular diagnosis. Making a periodontal diagnosis is especially helpful when a patient presents in pain. A study by McCarthy et al demonstrated that patients presenting with periradicular pain are better able to localize the painful tooth (89%) versus patients who present with tooth pain without periradicular pain (30%).14 By objectively testing the periradicular tissue, a dentist can optimally determine the gingiva and periradicular status.
Current periradicular diagnosis terminologies are identified and discussed in the following paragraphs.12
Normal periodontal tissue is tissue that is not sensitive to percussion or palpation testing. Also, radiographically, the lamina dura surrounding the root is intact.
Symptomatic apical periodontitis is a term describing a tooth that has painful response to biting and/or percussion. This condition may or may not be accompanied by periradicular changes radiographically.
Asymptomatic apical periodontitis describes a tooth that has no pain to percussion or palpation. Radiography reveals apical radiolucency.
Chronic apical abscess is a condition in which clinically a sinus tract is present on the gingival tissue. A radiograph typically reveals a radiolucency. It is important that the draining sinus tract be traced with a gutta-percha cone and then confirmed radiographically.
Acute apical abscess is an inflammatory reaction to pulpal infection and necrosis characterized by rapid onset, spontaneous pain, extreme tenderness of the tooth to pressure, pus formation, and swelling of associated tissues. There may be no radiographic signs of destruction. The patient often experiences malaise, fever, and lymphadenopathy.
Condensing osteitis is a diffuse radiopaque lesion in the periapical region. This opacity represents a localized osseous reaction to a low-grade inflammatory stimulus.
Restorative Treatment: Caries Removal
Among the clinical goals of any restorative treatment should be the maintenance of dental pulp vitality. Healthy pulp tissue is necessary for tooth nutrition, innervation, and immunocompetency.15 Maintaining the vitality of the dental pulp increases a tooth's mechanical resistance and long-term survival.16
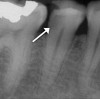
Obtaining a pretreatment pulpal and periradicular diagnosis before performing restorative treatment helps the clinician better understand how to treat the dental pulp, especially if it is exposed during caries excavation (Figure 1). A recent study by Ricucci et al found that a clinical pulpal diagnosis of a normal pulp or reversible pulpitis had a 96.6% histological match to the actual pulp tissue in a tooth.17 Therefore, for patients who present with or without pain from a carious pulp exposure and a pulp diagnosis of a normal pulp or reversible pulpitis, the tooth can be successfully treated with a mineral trioxide aggregate (MTA) pulp capping or pulpotomy if the pulp is exposed during treatment.18 In a randomized clinical trial, Hilton et al reported that MTA performed significantly better than calcium hydroxide as a direct pulp-capping agent.19
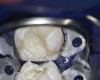
MTA is a bioceramic material. Bioceramics or calcium-silicate-based materials are biocompatible, nontoxic, and nonshrinking and are usually stable within a biological environment (Figure 2). Bioceramic materials also are able to form calcium hydroxide and hydroxyapatite.20 There are many commercially available bioceramics on the market for pulp capping, root repair, and root canal obturation. Examples include EndoSequence® (Brasseler USA, brasselerusa.com), ProRoot® MTA (Dentsply Sirona, dentsplysirona.com), and Biodentine® (Septodont, septodontusa.com).
After executing a bioceramic pulp cap, the dentist should place a light-cured glass-ionomer material (Figure 3) over the pulp cap.21 After this step, a permanent restoration such as a composite or amalgam material should be placed. This may seem counterintuitive to the training many dentists may have received in dental school that would call for a temporary filling to be placed. However, using a permanent restoration instead of a temporary filling is beneficial, because if the tooth remains asymptomatic post-treatment the clinician avoids the chance of causing further inflammation of the pulpal and periradicular tissue by not having to subsequently replace the temporary filling with a permanent one.13 It is, of course, possible that the patient may develop a symptomatic irreversible pulpitis after the pulp-capping procedure and, hence, require a pulpectomy, in which case having a permanent restoration in place will allow for a good access seal.
In a study, Linu et al reported that all pulp-capping failure occurred in the first 2 weeks after treatment.21 They also noted that the teeth that remained asymptomatic at the 2-week failure point remained asymptomatic, vital, and functional over the follow-up period of 12 to 18 months. Early clinical failures (within 2 weeks) are multifactorial but certainly may be related to an improper pretreatment pulpal diagnosis.15
If prior to restorative treatment the pretreatment pulpal diagnosis is necrotic or a symptomatic/asymptomatic irreversible pulpitis, a pulpectomy is indicated, followed by the placement of a permanent restoration. In teeth with signs and symptoms suggestive of a pretreatment pulpal diagnosis of symptomatic irreversible pulpitis, the pulp has a less than 15.6% chance of reverting to a normal pulp with a pulp-cap or pulpotomy treatment alone.17
Summary
Obtaining a pretreatment pulpal and periradicular diagnosis before performing restorative treatment, especially when removing caries, will help the clinician generate the correct treatment plan with regard to the dental pulp. The clinical data used to formulate these diagnostics are derived from the information attained from the patient's medical and dental history (including taking the patient's blood pressure, pulse, and, if indicated, temperature) and the five clinical objective tests: pulp sensibility, percussion (which may include bite testing), palpation, periodontal probing/tooth mobility, and current radiography. When a dentist evaluates the data from the medical and dental history along with these five objective clinical tests in conjunction with the tooth to be treated, a proper pretreatment pulpal and periradicular diagnosis can be made. This diagnosis will then provide the dentist with the optimum guidance to proceed with performing restorative treatment.
About the Authors
James Bahcall, DMD, MS
Clinical Associate Professor, Department of Endodontics, University of Illinois-Chicago College of Dentistry, Chicago, Illinois
Seema Ashrafi, DDS, MS
Clinical Associate Professor, Department of Periodontics, University of Illinois-Chicago College of Dentistry, Chicago, Illinois
Qian Xie, DDS, PhD
Assistant Professor, Department of Endodontics, University of Illinois-Chicago College of Dentistry, Chicago, Illinois
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Alghaithy RA, Qualtrough AJ. Pulp sensibility and vitality tests for diagnosing pulpal health in permanent teeth: a critical review. Int Endod J. 2017;50(2):135-142.
2. Rickoff B, Trowbridge H, Baker J, et al. Effects of thermal vitality tests on human dental pulp. J Endod. 1988;14(10):482-485.
3. Miller SO, Johnson JD, Allemang JD, Strother JM. Cold testing through full-coverage restorations. J Endod. 2004;30(10):695-700.
4. Lado EA, Richmond AF, Marks RG. Reliability and validity of a digital pulp tester as a test standard for measuring sensory perception. J Endod. 1988;14(7):352-356.
5. Weisleder R, Yamauchi S, Caplan DJ, et al. The validity of pulp testing: a clinical study. J Am Dent Assoc. 2009;140(8):1013-1017.
6. Jespersen JJ, Hellstein J, Williamson A, et al. Evaluation of dental pulp sensibility tests in a clinical setting. J Endod.2014;40(3):351-354.
7. Bahcall JK. Update on endodontic diagnosis. Inside Dentistry. 2015;
11(10):52-55.
8. Bender IB, Seltzer S. Roentgenographic and direct observation of experimental lesions in bone: I. 1961. J Endod. 2003;29(11):702-706.
9. Rose L, Mealey B, Genco R, Cohen W. Periodontics Medicine, Surgery, and Implants. St. Louis, MO: Elsevier Mosby: 2004:772-788.
10. Uraba S, Ebihara A, Komatsu K, et al. Ability of cone-beam computed tomography to detect periapical lesions that were not detected by periapical radiography: a retrospective assessment according to tooth group. J Endod. 2016;42(8):1186-1190.
11. Mattscheck D, Law AS, Nixdorf DR. Diagnosis of nonodontogenic toothache. In: Hargreaves KM, Cohen S, Berman LH (web editor), eds. Cohen's Pathways of the Pulp. 10th ed. St. Louis, MO: Mosby Elsevier; 2011.
12. Glickman GN. AAE Consensus Conference on Diagnostic Terminology: background and perspectives. J Endod.2009;35(12):1619-1620.
13. Kim S. Neurovascular interactions in the dental pulp in health and inflammation. J Endod. 1990;16(2):48-53.
14. McCarthy PJ, McClanahan S, Hodges J, Bowles WR. Frequency of localization of the painful tooth by patients presenting for an endodontic emergency. J Endod. 2010;36(5):801-805.
15. Zanini M, Meyer E, Simon S. Pulp inflammation diagnosis from clinical to inflammatory mediators: a systematic review. J Endod.2017;43(7):1033-1051.
16. Reeh ES, Messer HH, Douglas WH. Reduction in tooth stiffness as a result of endodontic and restorative procedures. J Endod. 1989;15(11):512-516.
17. Ricucci D, Loghin S, Siqueira JF Jr. Correlation between clinical and histologic pulp diagnoses. J Endod. 2014;40(12):1932-1939.
18. Taha NA, Ahmad MB, Ghanim A. Assessment of mineral trioxide aggregate pulpotomy in mature permanent teeth with carious exposures. Int Endod J. 2017;50(2):117-125.
19. Hilton TJ, Ferracane JL, Mancl L; Northwest Practice-based Research Collaborative in Evidence-based Dentistry (NWP). Comparison of CaOH with MTA for direct pulp capping: a PBRN randomized clinical trial. J Dent Res. 2013;92(7 suppl):16S-22S.
20. Wang Z. Bioceramic materials in endodontics. Endodontic Topics. 2015;32(1):3-30.
21. Linu S, Lekshmi MS, Varunkumar VS, Sam Joseph VG. Treatment outcome following direct pulp capping using bioceramic materials in mature permanent teeth with carious exposure: a pilot retrospective study. J Endod. 2017;43(10):1635-1639.