You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In actuality, there is no such thing as a "side effect." The notion of side effects applies to unanticipated effects of well-intentioned interventions. In such instances-for example, the overuse of antibiotics leading to antibiotic-resistant pathogens-clinicians' best efforts at finding a solution to a problem could make the problem worse. John Sterman, Professor of Management at the Massachusetts Institute of Technology Sloan School of Management and Director of MIT's System Dynamics group, wrote "…there are no side effects-just effects. Those we expected or that prove beneficial we call the main effects and claim credit. Those that undercut our policies and cause harm we claim to be side effects, hoping to excuse the failure of our intervention. ‘Side effects' are not a feature of reality, but a sign that the boundaries of our mental models are too narrow, our time horizons too short."1Sterman's proposal leads one to acknowledge that resulting effects can be desirable or undesirable, or anticipated or unanticipated, and that it takes both an open mind and the time for sufficient duration of follow-up to see all the effects that one's policy decisions, or clinical decisions, finally manifest.
In 2012, Koka and Zarb presented the concept of the osseosufficiency model.2 In this model, the goal of implant therapy is to strategically align the net positive and negative attributes of clinician, patient, and implant so that "enough" healing for the promotion and perpetuation of osseointegration takes place. The ultimate goal is that the combination of the positive attributes of the clinician, patient, and implant is enough to overcome the combination of the negative attributes of the clinician, patient and, implant; ie, that undesirable effects do not happen. If they do happen, failure in osseointegration will occur. For example, smoking may be a risk factor working against implant survival due to interference with desirable wound healing. However, the higher risk brought on by this patient attribute has been shown by Balshe et al to be mitigated by the use of implants with a "rough" surface.3,4 Today, "rough" surface implants in smokers and nonsmokers have the same survival profile. In this scenario, a "compromised" patient can still achieve and maintain successful long-term osseointegration by use of a modified implant surface. However, there have been unanticipated undesirable effects of rough surfaces.
Continuing on, the noted success of implant therapy has led to many clinicians with less formal surgical and restorative training providing such therapy with the noble intent of serving more patients through this life-changing treatment. Nevertheless, it appears that clinician experience and training level can impact osseointegration outcomes, with less-experienced and less-trained clinicians having less-successful outcomes. Again, one must ask if there have been unanticipated undesirable effects as a result of a well-intentioned change in "policy" from the days when Professor Brånemark insisted that only specialists place and restore dental implants.
Early implant therapy consistent with Brånemark focused on the edentulous patient, and outstanding clinical outcomes were reported in this population.5,6 In the years to follow, excellent prosthetic and surgical outcomes were reported in partially edentulous patients.7,8 Of particular interest are the findings reported by van Steenberghe and colleagues in 1993 where titanium abutments performed better over a 3-year period than natural teeth with regard to traditional periodontal indices.9 The findings indicated that dental implants placed in partially edentulous patients were remarkably resistant to soft-tissue inflammation and bone loss. Indeed, the authors wrote, "The resistance towards marginal bone loss around these implants confirms the previous studies on fully edentulous patients." In essence, the prevailing thinking in the early 1990s was that dental implants were more resistant to peri-implant problems involving soft tissue and hard tissue than natural teeth were to periodontal problems.
Today, prevailing thought has been reversed with the prevalence of peri-implantitis suggested to be as high as 56%.10 In the space of 20 years from the publication of van Steenberghe et al to 2013 in a systematic review published by Wilson,11 the tone of conversation in dentistry regarding peri-implant health and disease has changed dramatically. Wilson's systematic review focused on peri-implantitis and included the following search terms: "peri-implantitis," "mucositis," "partially edentulous," "preventative maintenance," "peri-implantitis and plaque control," "tissue augmentation," "diet maintenance of peri-implantitis," and "oral hygiene instruction for implants." Based on the findings of the included literature, Wilson wrote, "Analysis of the papers revealed that patients with implants are more susceptible to developing peri-implantitis than are patients with natural teeth to developing periodontal disease." The change from 1993 when implants were performing better than natural teeth to 2013 when implants appear to be more susceptible than natural teeth to disease is striking and makes one wonder what has happened to turn a boon of implant therapy into a burden of implant therapy in the course of less than a generation.
In this article, the authors propose that many of the challenges clinicians see today regarding the dramatic rise in peri-implant disease represent unanticipated undesirable effects of well-meaning interventions. Sufficient time has passed for these adverse effects to manifest, and now clinicians are able to better understand how their attempts to solve problems have spawned new challenges. The article also shows how new innovations in engineering and digital technology allow dentistry to address the problems of the past and avoid increasing the risk of peri-implant disease.
Rationale for Implant Abutment-Supported Cement-Retained Restorations
The early years of endosseous implant dentistry ad modum Brånemark were characterized by screw-retained restorations. "Hybrid" prostheses were initially made from cast metal framework/resin denture base material/resin denture teeth for edentulous patients who had experienced significant residual ridge resorption of the mandible and who struggled to wear complete dentures. The expansion of patients deemed suitable for implant therapy led to partially edentulous patients being treated, and the first uses of ceramometal restorations began, again with screw-retained restorations. Although today bone grafting of the labial aspect of edentulous maxillary ridges is considered a routine minor surgical procedure, 20 years ago it was not commonly performed due to concerns about predictability of the response; hence, it was avoided. Consequently, if a patient was to receive an implant in the anterior maxilla, its angulation was often tilted labially such that the screw-access opening emerged on the facial aspect of the restoration with a resultant esthetic compromise.
To counteract this suboptimal outcome, the custom abutment was introduced to "correct" for a labially tilted implant. In essence, the custom abutment was the original "graftless" solution. Abutment-supported cement-retained restorations quickly gained in popularity as a result.
The growth in the use of custom abutments and cement-retained restorations has been sustained over the past two decades. Today, both screw- and cement-retained restorations are widely used. Sufficient time has passed for the consequences, desirable and undesirable, anticipated and unanticipated, to manifest.
Unanticipated, Undesirable Effects of Cement-Retained Restorations
While junctional epithelium similar in structure and hemidesmosomal architecture is found attached to teeth and implants, the osseous and connective tissue relationships between teeth and implants are different. Around teeth, a periodontal ligament, relatively rich in cells, blood supply, and nerves, is a product of evolution designed to nourish and protect teeth. In contrast, an implant is devoid of a periodontal ligament and ostensibly integrates directly with bone. Around teeth, Sharpey's fibers from connective tissue insert directly into cementum cervical to the cementoenamel junction. As a result, and particularly relevant to this article's discussion, when a crown is cemented on a natural tooth the connective attachment to cementum forms a physical barrier to progression of cement toward crestal bone.
Around an implant, the connective tissue is more like scar tissue and does not attach directly into the implant. When a crown is cemented over an implant abutment, cement can "seep" toward the crestal bone being forced between connective tissue and the implant surface. These cement remnants are difficult to see and hard to remove. Consequently, the remnants harbor bacteria and often lead to inflammation of soft tissue, termed peri-implant mucositis. In some patients, the inflammatory response progresses to crestal bone loss and what is commonly referred to today as peri-implantitis. Numerous clinicians have noted this scenario, and, indeed, three recent systematic reviews have highlighted the increased risk of peri-implantitis associated with residual cement. Clearly an association exists between cemented restorations and a higher risk of peri-implant mucositis and peri-implant bone loss.11-13
Rationale for Platform Switching
A major change in implant and abutment design came about with the development of platform switching. First proposed by Lazzara and Porter in 2006, platform switching represents a horizontal offset where the abutment diameter is smaller than the implant diameter at the abutment-implant interface.14 Recent systematic reviews have attempted to determine the validity of the premise that platform switching results in less crestal bone loss than observed in platform-matching scenarios. All reviews acknowledge that the scientific quality of the included articles is routinely poor and that, as a result, the risk of bias is high in how authors of these articles have interpreted their findings. In general, most but not all15 systematic reviews suggest less crestal bone loss associated with platform switching than with platform matching.16,17
The clinical significance of the statistically significant differences (0.3 mm to 0.4 mm) reported, however, is difficult to assess, as clinical patient-centered outcomes between the two philosophies have not been reported. Regardless, platform switching is widely used, and sufficient time has passed since 2006 for the consequences, desirable and undesirable, anticipated and unanticipated, of its use to manifest.
Unanticipated, Undesirable Consequences of Platform Switching
Although the premise of platform switching was developed with the best of intentions, there are unanticipated undesirable effects. The most notable of these occurs when a platform-switched implant is combined with a cement-retained restoration. The curvature of the abutment from the restoration margin toward the platform-switched connection creates an undercut architecture that despite being filled on the macroscopic level by soft tissue, at the microscopic level permits cement remnants to penetrate the space between the abutment and soft tissue. Unfortunately, the undercut compromises attempts by the clinician to retrieve excess cement.
Vindasiute et al demonstrated that undercuts created in the restorative complex with platform switching promote cement retention.18 The undercut increases cement retention as it prevents accessibility to, and removal of, cement remnants using routine dental instruments. The authors further showed that the greater the undercut, the worse the problem with cement remnants becomes.
Ultimately, the putative benefits of platform switching are abrogated by the use of a cement-retained restoration. When one considers the benefits of platform switching in the context of the increased risk of the biological complications associated with inflammation-derived crestal bone loss and/or soft-tissue loss seen with cement-retained restorations, the risks of platform switching with cement-retained restorations are far greater than the benefits. In essence, the risks associated with cement-retained restorations have been magnified by the concurrent use with platform switching. Taken separately, each intervention may make sense; together, however, these risks can be synergistically harmful. If one must use a cement-retained restoration, doing so with a platform-switching-based complex of implant and abutment should be avoided.
Cementless and Graftless Solution
Given the elevated risk associated with the combination of cement-retained restorations and platform switching, it is clear that a screw-retained restoration on a platform-switched implant is preferable. In addition, screw-retained restorations provide greater flexibility with regard to restoration retrieval, which greatly aids management of concerns when removal of the restoration is needed.
In the anterior maxilla, positioning a platform-switched implant in an ideal screw-retained location previously posed a challenge that would require bone grafting to overcome. A recent innovation offers a solution for achieving a graftless and cementless restoration. Specialized engineering capabilities combined with a digital workflow and the many possibilities the latter offers have led to the development of a cementless, graftless, retrievable screw-retained restoration as a viable dental implant treatment option.
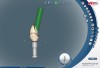
The angulated screw channel (ASC) system allows for the "correction" of implant angulation such that the restoration screw-access channel can be up to 25 degrees different than the long axis of the implant body in a 360-degree radius. This correction is achieved through a novel screw and screwdriver, the design of which allows the screw to swivel on the driver tip and ultimately be tightened and torqued at an angle of up to 25 degrees. The ASC abutment is milled zirconia with a titanium insert containing the connection geometry. The two components index with each other, and upon tightening of the screw are fastened together without cement. If additional firings of the zirconia are required for color matching or contour changes the two components can be easily separated after removal of the screw.
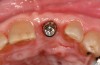
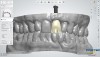
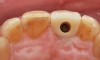
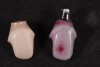
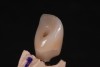
The ASC protocol is illustrated in two separate cases: Figure 1 through Figure 6 demonstrate fabrication of an implant-retained crown, and Figure 7 through Figure 12 show the making of a tooth-supported crown (No. 8) and an implant-supported crown (No. 9) using the ASC system.
The greatest impact of this innovative protocol is that implants can be placed in the anterior maxilla without grafting, thus saving the patient time and money. After osseointegration, a restoration can be affixed to the implant through screw retention with the access opening emerging from the palatal so that the esthetic outcome is uncompromised and retrievability is maintained. The access opening can be filled with restorative materials routinely used for screw-retained restorations. The ASC system eliminates the need to purchase an abutment or use cement to retain the restoration, and there is no risk to using the system with platform switching.
In essence, this protocol solves the problem that initially prompted the use of custom abutments and cement retention in the first place. If engineering and digital workflow capabilities were present 30 years ago, peri-implant tissue disease might likely still be an infrequent occurrence. The two illustrated cases presented (Figure 1 through Figure 6 and Figure 7 through Figure 12) show how a screw-access opening that would have come through the facial/incisal of an anterior restoration can be repositioned using the ASC so that a screw-retained and esthetic restoration can be fabricated without a graft or cement.
Summary
The famous quote, "The best laid plans of mice and men often go awry," has, over time, unfortunately become apt to describe the negative biological consequences of cement-retained restorations. These adverse consequences are magnified when combined with platform switching. When viewed through the lens of osseosufficiency, in which successful therapy is the net outcome of contributions from clinician, patient, and implant,2 the introduction of screw-retained restorations that can be used with an angulated screw channel may lead to fewer iatrogenic, clinician-induced complications and improve patient outcomes.
About the Authors
Alex Matosian, DDS
Private Practice, San Diego, California
Marc Hayashi, DMD
Assistant Clinical Professor,
Restorative Dentistry, UCLA School of Dentistry, Los Angeles, California
Bobby Birdi, DMD, MSc
Faculty, The Pacific Institute for Advanced Dental Education, Vancouver, British Columbia, Canada; Private Practice, Vancouver, British Columbia, Canada
Sreenivas Koka, DDS, MS, PhD, MBA
Restorative Dentistry and Advanced Prosthodontics, UCLA School of Dentistry, Los Angeles, California; Advanced Prosthodontics, Loma Linda University School of Dentistry, Loma Linda, California; Private Practice, San Diego, California
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Sterman JD. Learning from evidence in a complex world. Am J Public Health. 2006;96(3):505-514.
2. Koka S, Zarb G. On osseointegration: the healing adaptation principle in the context of osseosufficiency, osseoseparation, and dental implant failure. Int J Prosthodont. 2012;25(1):48-52.
3. Balshe AA, Eckert SE, Koka S, et al. The effects of smoking on the survival of smooth- and rough-surface dental implants. Int J Oral Maxillofac Implants. 2008;23(6):1117-1122.
4. Balshe AA, Assad DA, Eckert SE, et al. A retrospective study of the survival of smooth- and rough-surface dental implants. Int J Oral Maxillofac Implants. 2009;24(6):1113-1118.
5. Adell R, Lekholm U, Rockler B, Branemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
6. Adell R, Eriksson B, Lekholm U, et al. Long-term follow-up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxillofac Implants. 1990;5(4):347-359.
7. Jemt T, Lekholm U, Adell R. Osseointegrated implants in the treatment of partially edentulous patients: a preliminary study on 876 consecutively placed fixtures. Int J Oral Maxillofac Implants. 1989;4(3):211-217.
8. van Steenberghe D, Lekholm U, Bolender C, et al. Applicability of osseointegrated oral implants in the rehabilitation of partial edentulism: a prospective multicenter study on 558 fixtures. Int J Oral Maxillofac Implants. 1990;5(3):272-281.
9. van Steenberghe D, Kling B, Linden U, et al. Periodontal indices around natural and titanium abutments: a longitudinal multicenter study. J Periodontol. 1993;64(6):538-541.
10. Zitzmann NU, Berglundh T. Definition and prevalence of peri-implant diseases. J Clin Periodontol. 2008;35(8 suppl):286-291.
11. Wilson V. An insight into peri-implantitis: a systematic literature review. Prim Dent J. 2013;2(2):69-73.
12. Staubli N, Walter C, Schmidt JC, et al. Excess cement and the risk of peri-implant disease - a systematic review. Clin Oral Implants Res. 2017;28(10):1278-1290.
13. Quaranta A, Lim ZW, Tang J, Perrotti V, et al. The impact of residual subgingival cement on biological complications around dental implants: a systematic review. Implant Dent. 2017;26(3):465-474.
14. Lazzara R, Porter S. Platform switching: a new concept in implant dentistry for controlling post-restorative crestal bone levels. Int J Perio Rest Dent. 2006;26(1):9-17.
15. Hsu Y, Lin G, Wang HL. Effects of platform-switching on peri-implant soft and hard tissue outcomes: a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2017;32(1):e9-e24.
16. Chrcanovic B, Albrektsson T, Wennerberg A. Platform switch and dental implants: a meta-analysis. J Dent. 2015;43(6):629-646.
17. Herekar M, Sethi M, Mulani S, et al. Influence of platform switching on peri-implant bone loss: a systematic review and meta-analysis. Implant Dent. 2014;23(4):439-450.
18. Vindasiute E, Puisys A, Maslova N, et al. Clinical factors influencing removal of the cement excess in implant-supported restorations. Clin Implant Dent Relat Res. 2015;17(4):771-778.



![Fig 10. Labial view (laboratory [Fig 10] and clinical [Fig 11]) of crown Nos. 8 and 9 (implant-retained crown using angulated screw channel).](/media/thumbnail/17764)
![Fig 10 and Fig 11. Labial view (laboratory [Fig 10] and clinical [Fig 11]) of crown Nos. 8 and 9 (implant-retained crown using angulated screw channel).](/media/thumbnail/17765)