You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Satisfactory long-term survival rates of endosseous implants as treatment options for partially and fully edentulous patients have been well-documented.1,2 However, achieving esthetically pleasing peri-implant tissues long term after implant placement in the anterior area is not always predictable. The most common implant soft-tissue complications encountered in the esthetic zone are interproximal papillae and midfacial implant mucosal recessions.3 Rates of these complications have been reported as high as 7.1% after 5 years in function.1 Kan et al reported that the overall cumulative implant success rate after immediate implant placement and provisionalization was 100% after a mean follow-up of 4 years; however, continuing implant midfacial recession was found over time after 1 year of function, and 11% of these patients expressed dissatisfaction with the esthetic outcomes because of marginal soft-tissue recession and unesthetic final restorations.4 These findings demonstrate that despite high implant survival rates, implant soft-tissue complications in the esthetic zone are not uncommon; patients not only expect implants that are functional but that also have long-term esthetic stability in harmony with the surrounding dentition.
Several factors have been reported as the etiology for implant midfacial mucosal recessions and loss of interproximal papillae, including buccally positioned implants,5 thin gingival biotypes,4 lack of adequate keratinized mucosa,6 implant placement with horizontal bone augmentation, implant placement after horizontal onlay block grafting, inadequate horizontal implant–tooth distance, and increased distance of the tooth bone peak to the contact point.3 Thus, it is prudent for clinicians to address these factors before performing implant therapy to improve predictability of attaining esthetic results and provide a comprehensive treatment plan to meet the patient’s esthetic expectations.
Surgical and restorative interventions, such as bone-grafting procedures,7 connective-tissue grafting,8,9 and implant provisionalization,10,11 have also been reported as treatment options for mucosal recessions around implants. However, a recent systematic review evaluating the effect of several treatment modalities for implant midfacial mucosal recessions failed to find a benefit of using bone-grafting materials to reduce implant recession; nor was there enough evidence to demonstrate the beneficial effect of connective-tissue grafting to improve implant mucosal levels.12 Peri-implant mucosa and gingival tissue around teeth are different in several ways. Compared with gingiva, peri-implant tissue shows absence of root cementum and collagen fiber insertion on implant surfaces. Moreover, the collagen and fibroblast composition of the peri-implant mucosa is different from that of gingival tissue; a study indicated that the tissue turnover of peri-implant mucosa is less rapid than in gingiva.13 Therefore, periodontal procedures, particularly those related to soft-tissue augmentation, may have less-predictable long-term results for treating mucosal recession around implants.14
Hence, it has been suggested that the key determinant to prevent implant esthetic complications is identifying, before implant therapy, all possible etiologies that may cause implant mucosal recession and loss of interproximal papillae, combined with thorough presurgical planning.15 The aim of this article is to review several risk indicators of implant mucosal recession and loss of interproximal papillae, and how to prevent these risks.
Risk Indicators of Implant Mucosal Recession and Interproximal Papillae Loss
Buccally Positioned Implant
A minimum of 2 mm of facial bone thickness has been proposed as the “critical bone thickness” for the prevention of vertical height loss of the facial plate. It has been reported that when the distance of the buccal shoulder position of the implant to facial bone plate is below this critical thickness, an increased amount of facial bone resorption may be observed, which, in turn, may increase the chance of implant mucosal recession and failure (Figure 1). When the facial bone thickness is more than 2 mm from the implant buccal shoulder position, the likelihood of facial bone loss is decreased and the chance for alveolar bone stability is, therefore, increased.16
Chen and coworkers evaluated the soft-tissue and radiographic outcomes of implants placed in extraction sockets using a nonsubmerged protocol. The result showed statistically significantly higher marginal tissue recession at sites when implants were placed 1.1 mm from the inner buccal socket wall compared with implants placed 2.3 mm from the inner buccal socket wall. Six of the eight implant cases that were buccally positioned had unsatisfactory post-restorative esthetic outcomes. The authors concluded that position of the implant shoulder within the socket is a critical factor for ideal esthetic outcomes; thus, a minimum of 2 mm distance from the implant shoulder to the inner buccal shoulder wall was recommended to prevent implant marginal tissue recession.5
Caneva et al also suggested placing implants in a lingual (eg, cingulum) position to achieve optimal esthetic outcomes. The authors assessed the effect of implant positioning on resorptive patterns of the alveolar bone crest and demonstrated the importance of placing implants in a lingual position to minimize buccal bone resorption and thus prevent exposure of the implant. In their study, an average of 0.6 mm more buccal bone resorption was seen on implants that were placed in the center of the socket when healing after 4 months was compared histologically with implants that were positioned toward the lingual bony wall.17 In addition, placing a wider-diameter cylindrical implant in the extraction socket with the aim of filling the void between the implant and the inner socket wall was also shown to present greater buccal alveolar bone resorption (Figure 2).18,19 Based on these findings, it has been suggested that implant placement be performed in the palatal position of the socket to allow the formation of a gap between the implant surface and the inner buccal bone wall surface.19 More recently, in a retrospective cohort study, Cosyn and coworkers evaluated 115 patients who underwent implant placement with function. At 31 months, the buccal shoulder position of the implant was significantly associated with an increased likelihood of midfacial recession.3
Thin Gingival Biotype
While it has been suggested that peri-implant mucosa needs to be only a certain thickness to prevent bone resorption after implant placement, a thin tissue biotype may have an adverse effect on peri-implant soft-tissue stability and esthetic outcomes.20 Kois described thick tissue biotypes as more fibrotic and resistant to recession, whereas a thin tissue biotype is more friable and has less vascularization, or blood supply, and, thus, an increased risk of recession after implant surgery is observed.21 In an animal study, sites with a thin mucosa (≤ 2 mm) displayed consistent bone resorption and angular defects around implants, suggesting that a certain thickness of the peri-implant mucosa was required to favor stability.22 Similarly, Abrahamsson et al, using a dog model, demonstrated that sites with a thin mucosa had an angulated pattern of bone defects, whereas sites with an even pattern of the alveolar crest had an adjacent mucosa that was consistently thick.23
A human prospective clinical trial evaluated whether tissue/mucosa thickness may affect crestal bone stability around implants. This study showed that implants with initially thin tissue (< 2 mm) had bone loss up to 1.45 mm occurring within the first year of function. Contrarily, thick tissues (≥ 2 mm) showed only 0.2 mm of bone loss.24 Moreover, an incomplete filling of the space under the contact point by the interdental papillae was also reported more frequently at implant sites developed with a thin tissue biotype.20
In conclusion, some major differences were noted between implants with thin and thick gingival biotypes regarding marginal bone loss, buccal probing depth, buccal recession, and papilla index. Statistically higher amounts of peri-implant marginal bone loss and buccal recession were noted in a thin gingival biotype than in a thick biotype. Therefore, a thin gingival biotype may be considered a risk factor for implant marginal tissue recessions.14,20
Lack of Adequate Amount of Keratinized Mucosa
In 1972, Lang and Loe reported that at least 2 mm of keratinized gingiva, including 1 mm of attached gingiva, is needed to maintain gingival health and prevent bacterial entry into the gingival crevice.25 Keratinized mucosa around implants acts as a protective tissue seal to cope with bacterial challenge. In an animal experiment, Warrer and coworkers showed that implants placed in the lining (nonkeratinized) mucosa resulted in higher susceptibility for tissue breakdown due to bacterial plaque accumulation, leading to significantly higher attachment loss and higher mucosal recession than implants placed in areas with adequate keratinized mucosa.26 Similarly, Chung et al evaluated 339 endosseous implants in 69 patients that were in function for 3 years and demonstrated that implants with an absence of adequate keratinized mucosa or attached mucosa were associated with higher plaque accumulation and gingival inflammation, regardless of the implant surface configurations.27
Bouri et al, in a cross-sectional study, analyzed 76 patients with 200 implants and found that implants with narrow zones of keratinized tissue (< 2 mm) had significantly more plaque, bleeding on probing, and alveolar bone loss compared with implants with wider zones of keratinized tissue (≥ 2 mm). With a wider zone of keratinized tissue, implants may display an epithelial seal that is more resistant to the forces of mastication and frictional contact that occur during oral hygiene procedures, whereas implants with a lack of keratinized tissue have been shown to be more susceptible to irritation and inflammation.28 Shrott and coworkers also noted that at least 2 mm of keratinized mucosa around implants was beneficial for reducing lingual peri-implant plaque accumulation, bleeding, and buccal soft-tissue recession over a 5-year period.29 In contrast, Wennstrom et al showed that a lack of keratinized mucosa and marginal soft tissue had no significant effect on the health conditions of dental implants. However, the authors also reported that there were more clinically visible signs of inflammation in areas with narrow keratinized tissue (< 2 mm) compared with areas with wider zones of keratinized tissue (≥ 2 mm).30 Furthermore, in a recent systematic review, it was concluded that more plaque accumulation, tissue inflammation, mucosal recession, and attachment loss were found in implants with no keratinized mucosa.6
Implant Placement After Ridge Augmentation Procedures
Implant surgery with ridge recontouring has been suggested as a significant predictor of interproximal recession (ie, loss of interproximal papillae), which has been particularly seen in implants placed after block-grafting procedures. Thus, it has been suspected that multiple surgeries and/or papillae openings increase the risk for incomplete wound closure, resulting in soft-tissue recession. Furthermore, an increase in surgery time during ridge recontouring procedures was found to cause 0.2 mm of additional bone loss at the distal aspect of the adjacent tooth.3
In another report, Tymstra et al evaluated 10 patients who had maxillary anterior implants and had undergone multiple surgeries, including separate bone augmentation procedures with autogenous bone harvested from the chin region before implant placement. The authors reported that the inter-implant papilla was present in only one patient and 30% of the patients lost the papilla between the implant and its neighboring tooth, resulting in six moderate esthetic outcomes and four poor esthetic outcomes based on the clinician’s criteria. The authors concluded that the low esthetic index scores of the sites could be attributed to the patients having been through several traumatic surgeries, such as ridge recontouring by an augmentation procedure before implant placement.31 Thus, it was recommended to limit flap (eg, papilla) opening procedures to optimize soft-tissue esthetics around implants.3
Increased Distance of Tooth Bone Peak to the Contact Point
In 1992 Tarnow and coworkers reported the effect the distance from the contact point to the crest of bone has on the presence or absence of interproximal dental papilla. The data demonstrated that the presence of papilla was decreased when the distance of the bone peak (ie, crest of bone on the adjacent tooth surfaces) to the contact point increased. Incidence of complete interproximal papilla was observed when the distance between contact point and bone crest was ≤ 5 mm.32 Presence of papilla between a tooth and an implant depends on the proximal bone crest level of the adjacent tooth, whereas papilla presence between two adjacent implants is associated with inter-implant distance at the implant shoulder and the distance from the base of the contact point to the bone crest between adjacent implants.
A similar observation was observed by Choquet et al, who reported that the papilla was almost fully present when the distance from the base of the contact point to the bone crest was 3 mm to 4 mm. However, when the distance was 5 mm to 6 mm, some papilla was missing 50% of the time.33 In a prospective study, Andersson et al found a correlation between the marginal bone loss at tooth surfaces facing implants and vertical implant–tooth distance. The results showed that higher mean bone loss at implant-facing surfaces was noted when the vertical distance between the implant–abutment junction and cementoenamel junction (CEJ) of the adjacent tooth was 5.49 mm.34 Another retrospective study, by Cardaropoli et al, evaluating 28 patients with 35 fixed partial prostheses, also showed that implants positioned 6 mm below the CEJ of the adjacent tooth had 0.5-mm mean marginal bone loss at the implant site at the 3-year follow-up period.35
Concurring with these previous studies,33,36 Gastaldo and coworkers evaluated 48 patients who had implant-supported fixed prostheses for a minimum of 18 months and found that the papilla was always present when the distance from the base of the contact point to the bone crest was ≤ 3 mm. However, when the distance increased to ≥ 5 mm, papilla was absent in 60% to 75% of cases.37 Cosyn et al also reported that only 13% of the cases demonstrated a full distal papilla when the distance of the bone peak to the contact point exceeded 5 mm.3
Inadequate Horizontal Implant–Tooth Distance
Regarding placement of dental implants adjacent to natural teeth, careful consideration of available bone coupled with the implant dimension and insertion position is needed. Previous studies38,39 have indicated an increased amount of periodontal bone loss associated with a decrease in horizontal distance to the implant. Esposito et al analyzed the bone modification at teeth facing a single-tooth implant in the maxillary anterior region and reported a strong correlation between bone loss at the tooth site and a decreasing distance between the implant and tooth.38 It was also reported that soft- and hard-tissue alterations occurred predominantly within the first 6 months after one-stage implant placement surgery, and it was found that the presence of a tooth next to the implant positively affects the maintenance of the proximal bone crest level and the topography of the tooth–implant unit soft tissues.40
Vela et al also showed that there was a correlation between bone peak resorption and horizontal implant–tooth distance when platform-switched implants were placed closer than 1 mm to the adjacent tooth.41 Furthermore, Cosyn et al observed that when the implant–tooth distance was < 2.5 mm, there was a significant drop in the incidence of complete distal papilla,3 which is in agreement with previous reports.37,42 The closer the approximation of roots, the more complex the relationship will be between the interproximal tissue, which may be compromised, and the thinner the interproximal bone will be, which can potentially lead to greater risk of lateral resorption of the osseous crest and cause an absence of interdental papilla.21,43
Prevention of Implant Mucosal Recession and Interproximal Papillae Loss
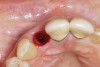
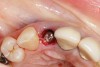
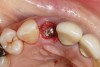
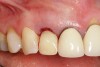
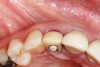
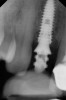
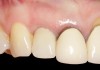
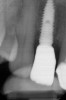
To predict peri-implant esthetic outcomes, Kois described five essential diagnostic keys that need to be assessed before removing a periodontally hopeless tooth (Figure 3 and Figure 4): (1) relative tooth position; (2) form of the periodontium; (3) periodontal biotype; (4) tooth shape; and (5) position of the osseous crest. Failing teeth that have a thick, flat gingival biotype, are square shaped, and have < 3 mm vertical distance from the position of the facial and interproximal crest have the lowest risk of developing recessions after implant placement.23 Therefore, implant surgery may be performed by either an open flap or flapless approach. However, teeth with a thin soft-tissue biotype, a highly scalloped gingival architecture, and a triangular shape that are positioned facially have less-predictable peri-implant esthetic outcomes. When a tooth presents with these unfavorable anatomical features, grafting procedures should be considered both before and after tooth extraction to prevent vertical loss and facial collapse of the gingival architecture.21 Flapless tooth extraction should be attempted in the esthetic zone to maintain blood supply from the periosteum and endosteum and maximize healing potential (Figure 5).44 In addition, several surgical protocols have been proposed to avoid peri-implant mucosal recessions, including 3-dimensional implant positioning,45,46 the use of platform-switching implants,47,48 and soft-tissue augmentation.8,49,50
Three-dimensional Implant Positioning
When placing an implant in the esthetic zone, ideal 3-dimensional positioning, including mesio-distal, apico-coronal, and orofacial dimensions, is essential to achieve favorable esthetic outcomes, regardless of the implant system used (Figure 6).45 With respect to the orofacial dimension, implants should be placed in a more palatal or lingual position to allow the presence of at least 2 mm of buccal bone thickness from the implant buccal shoulder.45,46 When the distance of the buccal bone wall and implant buccal shoulder is < 2 mm, a significantly higher incidence of midfacial recession has been previously reported.3,12 Placement of bone graft (Figure 7) and immediate restoration (Figure 8 and Figure 9) at the time of implant placement has also been suggested to increase peri-implant soft-tissue height and thickness.51 In the apico-coronal dimension, the implant head should be at least 3 mm apical to an imaginary line connecting the CEJ of the adjacent teeth and 1 mm to 2 mm apical to the interproximal and crestal bone to ensure a proper implant emergence profile and facilitate proper implant restoration (Figure 10). Regarding the horizontal implant–tooth distance, implants should be placed no closer than 1.5 mm from the adjacent root surface to minimize resorption of the interproximal alveolar crest, which causes a reduction in the papillary height.46,52
When placing multiple implants in the esthetic zone, Tarnow et al reported a lower height of the bone crest in areas with an inter-implant distance of ≤ 3 mm compared with areas with > 3 mm between the implants and suggested that this difference may be the result of lateral bone loss at the implants.53 Finally, management of subgingival abutment contour and definitive crown restoration shape that is harmonious with the surrounding periodontium is needed to maintain long-term soft-tissue health and stability (Figure 11 and Figure 12).
Use of Platform-switching Implant Designs
The platform-switching implant concept was introduced to reduce or minimize post-restoration crestal bone remodeling that was normally seen around a two-piece implant. The mismatch between the diameter of implant platform and the prosthetic component results in an increased circumferential horizontal tissue from 0.45 mm to 0.95 mm.54 The increased soft-tissue attachment around platform-switched implants thus may potentially reduce the incidence of dehiscence defects and prevent midfacial recessions around implants.47
Canullo et al investigated soft-tissue changes around platform-switching implants placed into extraction sockets with a 2-year follow-up and found 0.18 mm of soft-tissue gain and 0.045 mm of interproximal papillae gain in the platform-switching group; in the platform-matching implant group, interproximal papillae recession of 0.88 mm and buccal mucosal recession of 0.45 mm were noted. The authors described that in the group in which implants were restored with the platform-switching protocol, there was an additional 0.85 mm of horizontal biologic width formation around the implant collar, which may have provided additional peri-implant tissue stability.47 In contrast, Pieri and coworkers failed to show any difference regarding marginal soft-tissue level change and papilla height between platform-switching implants and platform-matching implants. However, the results demonstrated a 0.3 mm greater marginal bone loss at platform-matching implants compared with platform-switching implants after 12 months of loading. This difference was found to be statistically significant. Moreover, the data also showed that 60% of platform-matching implants had a marginal bone resorption > 0.5 mm, whereas only 11% of platform-switching implants had bone resorption > 0.5 mm.55
Soft-tissue Augmentation
Several studies have reported the use of connective-tissue grafting during immediate implant placement to prevent marginal soft-tissue recession.8,49,56,57 Kan and coworkers studied 20 patients, eight with a thick gingival biotype and 12 with a thin gingival biotype, who underwent immediate implant placement with simultaneous connective-tissue grafting, and found comparable mean marginal bone levels in each group. The authors also reported statistically insignificant outcomes regarding facial gingival levels and the presence of papillae in each group, suggesting that connective-tissue grafting in conjunction with immediate implant placement in the esthetic zone may minimize potential future facial gingival recessions. Moreover, it was concluded that a thin gingival biotype can be converted to a thick gingival biotype morphologically and behaviorally with this procedure, which may be beneficial for long-term stability of facial gingival tissues.8
Conclusion
Buccally positioned implants, thin tissue biotype, lack of keratinized tissue around implants, inadequate horizontal implant–tooth distance, increased distance of tooth bone peak to the contact point, and implant placement after surgical recontouring have all been described as risk indicators for peri-implant mucosal recessions. Careful assessment of the position of osseous crest and tissue biotype before tooth extraction and implant placement is critical for predictable esthetic outcomes. Lastly, ideal implant position in all three dimensions is critical to prevent potential recessions around implants. The use of platform-switching implants in conjunction with connective-tissue grafting procedures may be beneficial for the long-term stability of soft tissues around implants.
Acknowledgement
This article was partially supported by the University of Michigan Periodontal Graduate Student Research Fund.
About the Authors
James Mailoa, DDS
Resident
Graduate Periodontics
Department of Periodontics and Oral Medicine
University of Michigan School of Dentistry
Ann Arbor, Michigan
Richard J. Miron, DMD, DDS, MSc, PhD
ITI Scholar
Department of Periodontics and Oral Medicine
University of Michigan School of Dentistry
Ann Arbor, Michigan
Research Fellow, Department of Periodontology
Nova Southeastern University
Fort Lauderdale, Florida
Hom-Lay Wang, DDS, MSD, PhD
Professor and Director of Graduate Periodontics
Department of Periodontics and Oral Medicine
University of Michigan School of Dentistry
Ann Arbor, Michigan
Queries to the authors regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Jung RE, Zembic A, Pjetursson BE, et al. Systematic review of the survival rate and the incidence of biological, technical, and aesthetic complications of single crowns on implants reported in longitudinal studies with a mean follow-up of 5 years. Clin Oral Implants Res. 2012; 23(suppl 6):2-21.
2. Pjetursson BE, Thoma D, Jung R, et al. A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res. 2012;23(suppl 6):22-38.
3. Cosyn J, Sabzevar MM, De Bruyn H. Predictors of inter-proximal and midfacial recession following single implant treatment in the anterior maxilla: a multivariate analysis. J Clin Periodontol. 2012;39(9):895-903.
4. Kan JY, Rungcharassaeng K, Lozada JL, Zimmerman G. Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. Int J Oral Maxillofac Implants. 2011;26(1):179-187.
5. Chen ST, Darby IB, Reynolds EC. A prospective clinical study of non-submerged immediate implants: clinical outcomes and esthetic results. Clin Oral Implants Res. 2007;18(5):552-562.
6. Lin GH, Chan HL, Wang HL. The significance of keratinized mucosa on implant health: a systematic review. J Periodontol. 2013;84(12):1755-1767.
7. Kan JY, Rungcharassaeng K, Sclar A, Lozada JL. Effects of the facial osseous defect morphology on gingival dynamics after immediate tooth replacement and guided bone regeneration: 1-year results. J Oral Maxillofac Surg. 2007;65(7 suppl 1):13-19.
8. Kan JY, Rungcharassaeng K, Morimoto T, Lozada J. Facial gingival tissue stability after connective tissue graft with single immediate tooth replacement in the esthetic zone: consecutive case report. J Oral Maxillofac Surg. 2009;67(11 suppl):40-48.
9. Cosyn J, De Bruyn H, Cleymaet R. Soft tissue preservation and pink aesthetics around single immediate implant restorations: a 1-year prospective study. Clin Implant Dent Relat Res. 2013;15(6):847-857.
10. Barone A, Rispoli L, Vozza I, et al. Immediate restoration of single implants placed immediately after tooth extraction. J Periodontol. 2006;77(11):1914-1920.
11. Block MS, Mercante DE, Lirette D, et al. Prospective evaluation of immediate and delayed provisional single tooth restorations. J Oral Maxillofac Surg. 2009;67(11 suppl):89-107.
12. Lin GH, Chan HL, Wang HL. Effects of currently available surgical and restorative interventions on reducing midfacial mucosal recession of immediately placed single-tooth implants: a systematic review. J Periodontol. 2014;85(1):92-102.
13. Berglundh T, Lindhe J, Ericsson I, et al. The soft tissue barrier at implants and teeth. Clin Oral Implants Res. 1991;2(2):81-90.
14. Levine RA, Huynh-Ba G, Cochran DL. Soft tissue augmentation procedures for mucogingival defects in esthetic sites. Int J Oral Maxillofac Implants. 2014;29(suppl):155-185.
15. Chu SJ, Tarnow DP. Managing esthetic challenges with anterior implants. Part 1: midfacial recession defects from etiology to resolution. Compend Contin Educ Dent. 2013;34 spec no 7:26-31.
16. Spray JR, Black CG, Morris HF, Ochi S. The influence of bone thickness on facial marginal bone response: stage 1 placement through stage 2 uncovering. Ann Periodontol. 2000;5(1):119-128.
17. Caneva M, Salata LA, de Souza SS, et al. Influence of implant positioning in extraction sockets on osseointegration: histomorphometric analyses in dogs. Clin Oral Implants Res. 2010;21(1):43-49.
18. Caneva M, Salata LA, de Souza SS, et al. Hard tissue formation adjacent to implants of various size and configuration immediately placed into extraction sockets: an experimental study in dogs. Clin Oral Implants Res. 2010;21(9):885-890.
19. Sanz M, Cecchinato D, Ferrus J, et al. A prospective, randomized-controlled clinical trial to evaluate bone preservation using implants with different geometry placed into extraction sockets in the maxilla. Clin Oral Implants Res. 2010;21(1):13-21.
20. Annibali S, Bignozzi I, Iacovazzi L, et al. Immediate, early, and late implant placement in first-molar sites: a retrospective case series. Int J Oral Maxillofac Implants. 2011;26(5):1108-1122.
21. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
22. Berglundh T, Lindhe J. Dimension of the periimplant mucosa. Biological width revisited. J Clin Periodontol. 1996;23(10):971-973.
23. Abrahamsson I, Berglundh T, Wennstrom J, Lindhe J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin Oral Implants Res. 1996;7(3):212-219.
24. Linkevicius T, Apse P, Grybauskas S, Puisys A. The influence of soft tissue thickness on crestal bone changes around implants: a 1-year prospective controlled clinical trial. Int J Oral Maxillofac Implants. 2009;24(4):712-719.
25. Lang NP, Loe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43(10):623-627.
26. Warrer K, Buser D, Lang NP, Karring T. Plaque-induced peri-implantitis in the presence or absence of keratinized mucosa. An experimental study in monkeys. Clin Oral Implants Res. 1995;6(3):131-138.
27. Chung DM, Oh TJ, Shotwell JL, et al. Significance of keratinized mucosa in maintenance of dental implants with different surfaces. J Periodontol. 2006;77(8):1410-1420.
28. Bouri A, Jr., Bissada N, Al-Zahrani MS, et al. Width of keratinized gingiva and the health status of the supporting tissues around dental implants. Int J Oral Maxillofac Implants. 2008;23(2):323-326.
29. Schrott AR, Jimenez M, Hwang JW, et al. Five-year evaluation of the influence of keratinized mucosa on peri-implant soft-tissue health and stability around implants supporting full-arch mandibular fixed prostheses. Clin Oral Implants Res. 2009;20(10):1170-1177.
30. Wennstrom JL, Bengazi F, Lekholm U. The influence of the masticatory mucosa on the peri-implant soft tissue condition. Clin Oral Implants Res. 1994;5(1):1-8.
31. Tymstra N, Meijer HJ, Stellingsma K, et al. Treatment outcome and patient satisfaction with two adjacent implant-supported restorations in the esthetic zone. Int J Periodontics Restorative Dent. 2010;30(3):307-316.
32. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
33. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
34. Andersson B, Odman P, Lindvall AM, Lithner B. Single-tooth restorations supported by osseointegrated implants: results and experiences from a prospective study after 2 to 3 years. Int J Oral Maxillofac Implants. 1995;10(6):702-711.
35. Cardaropoli G, Wennstrom JL, Lekholm U. Peri-implant bone alterations in relation to inter-unit distances. A 3-year retrospective study. Clin Oral Implants Res. 2003;14(4):430-436.
36. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
37. Gastaldo JF, Cury PR, Sendyk WR. Effect of the vertical and horizontal distances between adjacent implants and between a tooth and an implant on the incidence of interproximal papilla. J Periodontol. 2004;75(9):1242-1246.
38. Esposito M, Ekestubbe A, Grondahl K. Radiological evaluation of marginal bone loss at tooth surfaces facing single Branemark implants. Clin Oral Implants Res. 1993;4(3):151-157.
39. Andersson B, Odman P, Lindvall AM, Branemark PI. Five-year prospective study of prosthodontic and surgical single-tooth implant treatment in general practices and at a specialist clinic. Int J Prosthodont. 1998;11(4):351-355.
40. Chang M, Wennstrom JL. Peri-implant soft tissue and bone crest alterations at fixed dental prostheses: a 3-year prospective study. Clin Oral Implants Res. 2010;21(5):527-534.
41. Vela X, Mendez V, Rodriguez X, et al. Crestal bone changes on platform-switched implants and adjacent teeth when the tooth-implant distance is less than 1.5 mm. Int J Periodontics Restorative Dent. 2012;32(2):149-155.
42. Romeo E, Lops D, Rossi A, et al. Surgical and prosthetic management of interproximal region with single-implant restorations: 1-year prospective study. J Periodontol. 2008;79(6):1048-1055.
43. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
44. Chu SJ, Salama MA, Salama H, et al. The dual-zone therapeutic concept of managing immediate implant placement and provisional restoration in anterior extraction sockets. Compend Contin Educ Dent. 2012;33(7):524-534.
45. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19(suppl):43-61.
46. Funato A, Salama MA, Ishikawa T, et al. Timing, positioning, and sequential staging in esthetic implant therapy: a four-dimensional perspective. Int J Periodontics Restorative Dent. 2007;27(4):313-323.
47. Canullo L, Iurlaro G, Iannello G. Double-blind randomized controlled trial study on post-extraction immediately restored implants using the switching platform concept: soft tissue response. Preliminary report. Clin Oral Implants Res. 2009;20(4):414-420.
48. Canullo L, Rasperini G. Preservation of peri-implant soft and hard tissues using platform switching of implants placed in immediate extraction sockets: a proof-of-concept study with 12- to 36-month follow-up. Int J Oral Maxillofac Implants. 2007;22(6):995-1000.
49. Covani U, Marconcini S, Galassini G, et al. Connective tissue graft used as a biologic barrier to cover an immediate implant. J Periodontol. 2007;78(8):1644-1649.
50. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
51. Chu SJ, Salama MA, Garber DA, et al. Flapless postextraction socket implant placement, part 2: the effects of bone grafting and provisional restoration on peri-implant soft tissue height and thickness—a retrospective study. Int J Periodontics Restorative Dent. 2015;35(6):803-809.
52. Bashutski JD, Wang HL. Common implant esthetic complications. Implant Dent. 2007;16(4):340-348.
53. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
54. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
55. Pieri F, Aldini NN, Marchetti C, Corinaldesi G. Influence of implant-abutment interface design on bone and soft tissue levels around immediately placed and restored single-tooth implants: a randomized controlled clinical trial. Int J Oral Maxillofac Implants. 2011;26 (1):169-178.
56. Tsuda H, Rungcharassaeng K, Kan JY, et al. Peri-implant tissue response following connective tissue and bone grafting in conjunction with immediate single-tooth replacement in the esthetic zone: a case series. Int J Oral Maxillofac Implants. 2011;26(2):427-436.
57. Chung S, Rungcharassaeng K, Kan JY, et al. Immediate single tooth replacement with subepithelial connective tissue graft using platform switching implants: a case series. J Oral Implantol. 2011;37(5):559-569.