You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
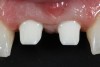
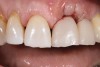
Following the successful integration of implants in the esthetic zone and creation of satisfactory hard- and soft-tissue volume, the restoring clinician is responsible for managing and shaping the definitive soft-tissue architecture. In the esthetic zone, this is a process generally achieved through the use of an implant-retained provisional restoration. The restoring clinician and technician should be intimately familiar with esthetic principles of tooth size, shape, and position. However, the subgingival area of the provisional restoration is also vitally critical. This area, known as the “emergence profile” (Figure 1), plays a significant role in the creation and maintenance of a satisfactory gingival architecture and will ultimately determine the final architecture of the peri-implant soft tissue.
Creation of the correct emergence profile can enhance the esthetic and biologic outcome, while a poorly designed emergence will compromise it. Knowledge of the peri-implant biology and principles of emergence profile design will enable the restoring clinician to accurately manipulate the position of the free gingival margin and adjacent papilla. Success cannot be achieved through manipulation of the emergence profile alone; however, sufficient tissue volumes are a prerequisite.
The focus in this situation is on maximizing the biologic and esthetic outcome of the soft tissue starting at any point following the completion of surgery. That is, it is important to determine what can be done prosthetically to achieve the optimum result of a given implant situation. The techniques and concepts discussed in this article will not guarantee an exceptional outcome in every situation, but they can aid clinicians in maximizing the results of any given situation. While a poor surgical foundation will preclude an exceptional outcome, an excellent surgical foundation will not necessarily guarantee an exceptional outcome. However, shaping of the soft tissue through the creation of proper emergence profiles on the abutment can enhance the outcome for any given starting point.
Peri-Implant Hard and Soft Tissue: Biologic And Esthetic Considerations
The soft tissue around an implant differs markedly from that which is around a natural tooth. It is less vascular, more fragile, and greater in volume.1 This greater volume allows, for better or worse, an enhanced ability to change the position of the tissue based upon the prosthetic contours. In a healthy periodontium, the transverse fibers insert into the cementum on the tooth root with Sharpey’s fibers along the zone of the biologic width known as the connective tissue attachment.2 This connection provides a relatively strong and stable foundation for the soft tissue around the natural tooth. Around an implant, there is no evidence of such a connection. The peri-implant attachment is from hemidesmosomes and basal lamina, but it is a much more fragile connection.3 The transverse fibers that insert into the cementum of a natural tooth instead appear to reorient into a circumferential orientation around the implant.4 Upon maturation, these circumferential fibers can develop into a protective “o-ring” at the point of minimal diameter. In a traditional implant design, this is often at the position of the first thread. On a “platform-switch” designed implant this position is located much more coronally and may contribute to the observation that a platform-switch design better preserves the volume of the peri-implant bone and soft tissue.5 Sufficient development of the peri-implant “o-ring” takes 4 to 6 weeks to develop.6
The “biologic width” around an implant also differs from that of the natural tooth. It is greater in mean dimension (~ 3 mm versus ~ 2 mm)7,8 and has greater mean probing depths.9 The base of the sulcus is also more fragile, and probing must be carried out with less force to avoid disturbing the delicate attachment. To this end, probing should be avoided during the early stages of tissue maturation.
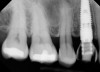
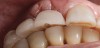
Management of the peri-implant papilla has generally been considered to be a challenge in the esthetic zone. It is worth noting though, that a shortened papilla is not an indication of a biologic problem, merely an esthetic one. The study of average papilla heights and volumes around natural, healthy teeth has been thoroughly explored with fairly clear and consistent outcomes.10 Between adjacent implants of similar design, the papilla height from the crest of bone has been less predictable, ranging from 1 mm to 7 mm with an average of 3.4 mm11 (Figure 2). Use of varying implant designs (platform-switched, conical connections, tissue-level, etc.) would likely increase the data divergence. Factors that are largely outside of the control of the treatment team but will bear heavily on the mature height of the papilla include: patient genetics, tissue biotype (thickness), oral microbiology makeup, and oral hygiene. Factors within the control of the treatment team include: implant diameter, volume of the peri-implant bone, position of the bone on adjacent natural roots, implant connection design, inter-implant distance, and the shape of the emergence profile.
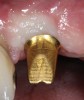
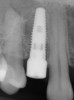
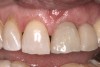
In order to maximize the height of the peri-implant papilla, significant efforts must be made to maximize the blood supply and to preserve the bone on the adjacent roots and between the implant.12 Pressure and blanching of the peri-implant tissues compromises the blood supply of this fragile complex and (eventually) leads to reduction in the height of the papilla (Figure 3). At a given site in a given individual, there is a natural biologic width that the body will strive to maintain between any bone and any non-integrated material. Thus, if a non-integrating abutment is placed within close proximity to the bone on the adjacent natural tooth (Figure 4), inevitably the bone will be remodeled to a more apical position to re-establish the biologic width. This distance obviously varies, but generally 1 mm to 1.5 mm is needed.13
Though it has often been proposed that the interdental papilla is much like a “water balloon” and will respond to pressure by increasing in length, this may not be true for papilla adjacent to an implant. Pressure will initially “squeeze” the papilla into a more coronal position, but this pressure will decrease the blood supply to this fragile tissue, and in many scenarios the increased emergence profile volume will result in an apical remodeling of the adjacent bone and corresponding apical migration of the soft tissue.
Abutment Emergence Profile: How It Changes the Soft-Tissue Position
The emergence profile is the portion of the abutment from the head of the implant to the free gingival margin, and it has significant impact on the shape and position of the soft tissue. Generally, a larger diameter emergence profile will compress the soft tissue and move it apically (Figure 5), while a narrowed emergence profile will allow the soft tissue to drape in a more coronal position (Figure 6). Neither design is indicated for all situations, and the design must be based on the needs of the particular clinical scenario.
Ultimately, the emergence profile design must be tested in-situ, and time must be allotted for the patient’s peri-implant tissues to respond and mature before further alterations are made. The maturation process should be allowed to take place for at least 4 weeks. It should also be noted that strong evidence exists that indicates repeated disconnection of components from the implants results in significant loss of peri-implant bone and soft tissue (~ 0.7 mm and 1.5 mm, respectively).14 This loss is most acutely seen during the initial osseointegration and soft-tissue maturation stage. Thus, repeated removal of the abutment and reshaping of the emergence profile should be kept to an absolute minimum and postponed at least 4 months following implant placement.
Any enlargement of the emergence profile will result in blanching of the soft tissues. This is caused by a transient decrease in blood flow due to pressure from the abutment. There is no definitive way to know exactly how much positional change the blanching will result in, only that it will happen. In the subsequent weeks, the peri-implant tissues will reorganize and adjust to the pressure by settling at a more apical position. The speed and extent to which this happens depends on the amount of increased abutment size, the tissue thickness, oral hygiene, and bone position. Thus, it is advisable that critical changes in soft-tissue contours be performed in a provisional stage, allowing the tissue to mature and adjust for at least 4 weeks and then re-evaluating before making the final impression.
Special attention should be given to the shape and apparent width of the tooth at the cervical area. The mesio-distal width of the abutment at this position should mirror that of the contralateral tooth or teeth. Within the peri-implant zone, the most delicate and challenging aspect is the management of the papilla. This small, pyramid-shaped soft tissue depends on its attachment to adjacent natural tooth roots and underlying bone for its height and blood supply. Adjacent to an implant, at least half of this support no longer exists. Attempts have been made (with occasional success) in compressing the papilla from the sides to increase its height.15 However, this is an unpredictable approach, and greater success may be achieved by allowing space (open gingival embrasure) during the provisional stage for the papilla to mature to its maximum vertical length and then closing any remaining open embrasure with the definitive prostheses by extending the interproximal contact point apically.
Controlling Soft-Tissue Position and Shape with Provisional Restorations
The final architecture of the soft tissue is ultimately a result of the foundation of bone and soft tissue and the shaping and support of these tissues by the prostheses.16 In the esthetic zone, far too much uncertainty is brought about when the clinician moves from healing abutments to definitive prostheses without utilizing an implant-retained provisional restoration.17 This procedure can be used in both immediate and delayed loading approaches. The provisional restoration allows maturation and development of the peri-implant tissues in a form resembling the desired final outcome. The emergence profile can also be modified as needed to reposition the peri-implant soft tissue. Use of the provisional restoration in this manner creates an exceptionally predictable protocol whereby the clinician, patient, and all other involved parties can evaluate the final outcome before the definitive prostheses are even fabricated.
Screw-retained provisional restorations allow the creation of a seamless and cement-free transition from the head of the implant to the free gingival margin. This is critical during use in immediate load cases where wound healing will be occurring in contact with the abutment. The screw-retained approach also allows for easy access and manipulation of the emergence profile should the need arise. Three components are needed to fabricate a screw-retained provisional restoration: titanium abutment, clinical screw, and provisional tooth shell (acrylic, composite, polycarbonate, etc.) (Figure 7).
Abutment selection for the provisional restoration must meet three key criteria: biocompatibility, high strength, and narrow. Though variation exists between systems, a narrow-diameter titanium abutment is generally available and easily meets the above criteria. When implemented in immediate load cases, strength of the abutment is critical to avoid having to manipulate components at the head of the implant during the period of low implant stability. Some provisional abutments are designed with a flared collar at the interface that can be removed (Figure 8 and Figure 9) to enhance the potential soft-tissue volume during healing.18 The length of the abutment will need to be shortened to fit within the tooth shell. Any adjustments to the abutment are to be done outside the mouth to avoid titanium debris in the wound and transfer of heat and vibration to the implant. It is esthetically beneficial to opaque the surface of the abutment with a low-viscosity opaquing resin. This will help to minimize any graying of the provisional.
Once cut to length, the provisional abutment is re-placed onto the implant. The tooth shell is then connected to the abutment with flowable composite or autopolymerizing acrylic resin. A putty matrix can be helpful in accurately placing the shell. Care must be taken to avoid blocking access to the screw chamber. Following light-curing or autopolymerization, the shell and abutment are now connected and removed as a single unit. The emergence zone now needs to be designed and finished.
Utilizing composite or acrylic, the space between the titanium collar and the crown margin is filled in. Generally, it is advisable to create a contour that is relatively narrow. This will allow space for a blood clot to form and potentially create additional volume of soft tissue. Keeping the emergence profile narrow will avoid blanching, compromised blood flow, and the corresponding apical migration of soft tissue. Additionally, the narrow emergence will maintain a maximum distance from the peri-implant bone and help to maintain the critical interproximal bone peaks adjacent to the implants (Figure 10). As mentioned previously, gingival embrasures should be kept open to allow for maximum development of the papilla height (Figure 11 and Figure 12). The provisional restoration should be fully out of occlusion in maximum intercuspal position (MIP) and throughout the excursive range (Figure 13); this will often result in a tooth form that is shorter than the definitive restoration will be.
This narrow emergence profile provisional restoration should remain undisturbed on the implant for at least 4 months following immediate implant placement. Patients are instructed to avoid using or chewing on the provisional restoration. Patient selection is key to success with immediate loading.
Following sufficient time for osseointegration and maturation of the soft tissue, the peri-implant architecture can be evaluated. Because the initial emergence profile was quite narrow, there may be an excess of soft tissue (which is rather desirable around an implant) (Figure 14). The mesio-distal width of the tooth may also be deficient at the gingival aspect. At this time, the restoration is removed and the deficient areas are augmented with composite or acrylic. Open gingival embrasures should also be closed, if desired. When the restoration is reinserted onto the implant the tissue will blanch, indicating that the increased emergence volume is placing pressure and reducing blood flow. The tissue will migrate away from this pressure, but it is unknown how far and how quickly this will occur.
To accurately reposition the tissue, pressure must be applied in the correct amount to move the tissue the desired distance, but no further. To this end, use of a “pseudo cementoenamel junction (CEJ)” design is helpful (Figure 15). When adding composite or acrylic to the emergence area, particularly near the free gingival margin, a bulk of material is added in the amount desired to move the tissue (eg, 1 mm), and apical to this position the emergence remains narrow. This will “push up” on the tissue to the desired position and allow the tissue to settle into the low-pressure area apical to it (Figure 16). Though this technique is effective, manipulation and attachment of components at the head of the implant should be minimized to avoid loss of bone and soft tissue. This is particularly true during the initial 3 to 4 months.
Any modifications to the emergence profile intended to affect the soft tissue should be allowed to remain in place for 4 to 6 weeks (Figure 17). This will give the tissues sufficient time to mature and adjust.
Conclusion
Clinicians cannot fully predict how peri-implant tissues will respond to treatment and modifications, nor can they completely understand what the patient is expecting. Use of a provisional restoration and careful manipulation of the emergence profile provides in-situ testing of the patient’s biology, adaptation, and expectations. Changes to the position of the soft tissue can be tested, proven, and modified as needed and to the extent possible given inherent patient factors. When all of the parties involved are satisfied with the results in the provisional, the final impression is made (preferably with customized copings) and the technician will now have a comprehensive blueprint to follow.
Disclosure
The author had no disclosures to report.
About the Author
Todd R. Schoenbaum, DDS
Associate Clinical Professor
Division of Constitutive and Regenerative Sciences
University of California-Los Angeles School of Dentistry
Director of Continuing Dental Education
University of California-Los Angeles School of Dentistry
Los Angeles, California
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Lindhe J, Berglundh T, Ericsson I, et al. Experimental breakdown of peri‐implant and periodontal tissues. A study in the beagle dog. Clin Oral Implants Res. 1992;3(1):9-16.
2. Page RC, Ammons WF. Collagen turnover in the gingiva and other mature connective tissues of the marmoset Saguinus oedipus. Arch Oral Biol. 1974;19(8):651-658.
3. Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
4. Piattelli A, Scarano A, Piattelli M, et al. Histologic aspects of the bone and soft tissues surrounding three titanium non-submerged plasma-sprayed implants retrieved at autopsy: a case report. J Periodontol. 1997;68(7):694-700.
5. Rodríguez X, Vela X, Calvo-Guirado JL, et al. Effect of platform switching on collagen fiber orientation and bone resorption around dental implants: a preliminary histologic animal study. Int J Oral Maxillofac Implants. 2011;27(5):1116-1122.
6. Rompen E, Raepsaet N, Domken O, et al. Soft tissue stability at the facial aspect of gingivally converging abutments in the esthetic zone: a pilot clinical study. J Prosthet Dent. 2007;97(6 suppl):S119-S125.
7. Berglundh T, Lindhe J, Ericsson I, et al. The soft tissue barrier at implants and teeth. Clin Oral Implants Res. 1991;2(2):81-90.
8. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32(3):261-267.
9. Buser D, Weber HP, Lang NP. Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res. 1990;1(1):33-40.
10. Chu SJ, Tarnow DP, Tan JH, Stappert CF. Papilla proportions in the maxillary anterior dentition. Int J Periodontics Restorative Dent. 2009;29(4):385-393.
11. Tarnow DP, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
12. Lops D, Chiapasco M, Rossi A, et al. Incidence of inter-proximal papilla between a tooth and an adjacent immediate implant placed into a fresh extraction socket: 1-year prospective study. Clin Oral Implants Res. 2008;19(11):1135-1140.
13. Abrahamsson I, Berglundh T, Wennström J, Lindhe J. The peri-implant hard and soft tissues at different implant systems. A comparative study in the dog. Clin Oral Implants Res. 1996;7(3):212-219.
14. Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. J Clin Periodontol. 1997;24(8):568-572.
15. LeSage BP. Improving implant aesthetics: prosthetically generated papilla through tissue modeling with composite. Pract Proced Aesthet Dent. 2006;18(4):257-263.
16. Zetu L, Wang HL. Management of inter-dental/inter-implant papilla. J Clin Periodontol. 2005;32(7):831-839.
17. De Rouck T, Collys K, Wyn I, Cosyn J. Instant provisionalization of immediate single-tooth implants is essential to optimize esthetic treatment outcome. Clin Oral Implants Res. 2009;20(6):566-570.
18. Schoenbaum TR, Chang YY, Klokkevold PR, Snowden JS. Abutment modification for immediate implant provisional restorations. J Esthet Rest Dent. 2013;25(2):103-107.