You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Treatment plans involving the transition of a patient from a failed dentition to one supported by implants can take time when the goal is to avoid placing that patient in a removable prosthesis. One option is immediate loading of implants with a full-arch provisional.1,2 However, if the treating surgeon determines that the implants cannot be loaded (which could be for a variety of reasons), methodologies to avoid immediate loading need to be employed. Many restorative dentists and surgeons might then opt for serial extractions so that the patient is never totally without teeth. This protocol—often termed a staged approach, serial extraction protocol, or phased treatment plan—was formulated primarily to provide fixed restorations for patients with hopeless dentitions without the need for removable provisional phases.1,3,4 While it may vary for each patient, this type of treatment generally involves multiple stages of implant placement during which residual but hopeless teeth are kept as temporary abutments to hold fixed provisional restorations. Once the abutment connection is performed on the first set of implants, the residual teeth are extracted and a second stage of implant placement is accomplished. After the second or final set of implants has healed, implant prosthodontic procedures can be performed to complete treatment. Cavallaro and Greenstein divide this protocol into two classifications: Class I, with all the implants placed during the initial surgery; and Class II, with two or more stages of implant placement to generate sufficient implant support.4,5
Whether the staged approach treatment plan has one, two, or multiple implant phases, the main disadvantages often relate to the treatment time and multiple surgical steps involved. The advantages are numerous, including the ability to use a fixed provisional restoration throughout treatment and healing phases, simplified guidance for implant placement, and preserved masticatory function.1,3 Cordaro et al also cite soft-tissue management as an advantage with this staged approach.1 Despite such recent advances in implant dentistry as virtual planning, immediate loading, and improved fixture surfaces, soft-tissue healing is still not routinely predictable.6-9 While loss of up to 1 mm of marginal bone in the first year after abutment connection was once considered acceptable,10,11 it has become evident that over time, this can also mean loss of soft tissue in that same period or in years to come.12,13 Whether tissue loss is immediate or subsequent, the success of treatment is judged not only by function and dental esthetics, but also by soft-tissue esthetics.
Recession defects, whether around a natural tooth or an implant, may be caused by a variety of factors. Surgical trauma, aggressive tooth brushing, periodontitis or peri-implantitis, parafunctional habits, and tooth malposition have been cited as some of the causitive factors.14 With implants specifically, initial longitudinal studies have always measured the recession at the time of abutment placement or periodically at later periods after final case insertion. Adell et al reported 1.7 mm of recession in a 3-year study.15 Aspe et al,16 Bengazi et al,17 and Small and Tarnow18 found similar results in their respective studies that analyzed the issue at times from initial placement to 9 years; all concluded that factors such as keratinized peri-implant tissue tend to help minimize recession. However, after a thorough literature review of many soft-tissue factors, Greenstein and Cavallaro concluded that the literature does not clearly define a patient’s susceptibility to recession related to many of these factors.19
Saadoun and Touati cite biotype at implant sites and position of the implant fixture in relation to the cortical wall as factors in potentially predicting a susceptibility to recession.12,13 Lee et al found that a thin soft-tissue biotype of <2 mm is associated with thinner underlying bone, angular bone defects, and increased susceptibility to the loss of papilla after immediate implant placement.20 In addition, such a biotype is more prone to recession in response to trauma and bacteria than a thick biotype. In response to this concern, Butler and Kinzer recommend planning implant placement at a minimum of 2-mm palatal to the facial contour of the adjacent teeth.21 They agree with Bashutski and Wang, who observed that facially positioned implants are at risk for gingival recession.22 Le and Borzabadi-Farahani concluded that both labial soft-tissue thickness and labial bone thickness are key factors in predicting recession occurrence.23
Tarnow et al have suggested that, if the distance between adjacent implants is <3 mm, the height of the alveolar bone decreases and preserving the gingival papilla becomes difficult.24 In a key study in 2003, Tarnow et al concluded that clinicians should use great caution when placing implants adjacent to each other, so that they are at least 3 mm apart. They further suggest that treatment plans should be modified to either adhere to this rule or utilize pontics and/or natural teeth to better preserve esthetic soft-tissue contours.25
Retained natural-tooth roots were utilized under removable prostheses to preserve alveolar bone many years before implants.26,27 Extraction of teeth triggers the resorption of alveolar bone and surrounding tissues. Schropp et al found that such resorption reduces the width of the alveolar ridge by up to 50% in just 1 year.28 Salama et al demonstrated that submerged roots can maintain surrounding alveolar bone and soft tissues adjacent to implants. They also demonstrated that a submerged root will preserve a much greater amount of surrounding tissue than commonly used socket preservation techniques, which often result in crestal bone resorption, thereby reducing the height of the interdental papilla and edentulous ridge width.29
Abutment connections to implant fixtures can also be a factor in recession susceptibility. Jansen et al30 and Zipprich et al31 found that abutment connection type can be a factor in bone loss and associated soft-tissue recession. Jansen et al tested many different implant abutment systems for microbial leakage and bacterial colonization around the inner surfaces of the implant systems (fixture head, abutment screw, and abutment). They concluded that certain types of implants with flat-to-flat interfaces allow more bacteria to colonize in and around their components.30 Zipprich et al found that elastic deformation of the connection screw in non–self-locking implants—such as externally hexed implants with flat-to-flat abutment interfaces—tilt under extra-axial loading and cause micromovement at prosthetic abutment-to-implant interfaces.31 Brunski stated that “micromotion can be deleterious at the bone–implant interface, especially if the micromotion occurs soon after implantation,” and micromotion of more than 100 µm should be avoided to prevent the wound from undergoing fibrous repair rather than osseous regeneration.32 While techniques like platform switching can reduce such micromovement, self-locking implants such as those that are internally hexed with long internal connections are particularly effective in preventing micromovement that could inflame the soft tissue and cause crestal bone resorption and concomitant recession.30,31
Soft-tissue management in the staged-approach protocol can be unpredictable and present esthetic challenges—mainly gingival recession.13,22,33 This article will show several examples of different staged-approach cases with soft-tissue recession around abutments. These cases are organized by treatment plan modifications, which range from leaving the visible gold collar of the abutments alone to remaking the abutments and castings.
Case Examples
Case 1 – Re-preparing Abutments Intraorally
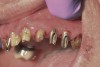
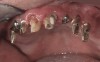
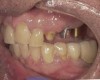
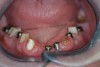
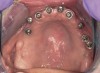
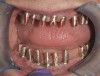
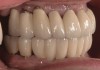
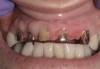
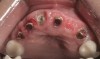
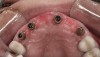
Background: This patient had a failing maxillary dentition and refused to wear a removable prosthesis. A staged approach was employed to retain some of his natural tooth abutments, and recession was noticed at the time of the impression for the second group of implants. Figure 1 shows the patient following insertion of the first set of implant custom abutments; the adjacent natural teeth are still present to support the provisional bridge. Seven months later, as shown in Figure 2, those first-stage custom abutments exhibited evidence of 1 mm to 3 mm of recession.
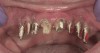
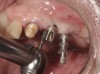
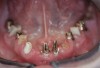
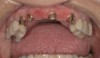
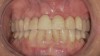
Results: A decision was made to re-prepare all of the abutments intraorally (Figure 3) so that all abutment margins would be at or below the gingival margin. (Of note, teeth Nos. 8 and 9, also shown in Figure 3, were later submerged for the case to be fully implant-supported.) While re-preparation greatly improved the esthetics of the final result, it required retraction cord placement, new impressions, and new castings.
(Note: A separate but similar type of case shown in Figure 4 and Figure 5 further illustrates intraoral abutment re-preparation.)
Case 2 – Re-preparing Abutments Intraorally with Extraoral Impressions
Background: This case had similar recession problems as the previously mentioned cases. Although the abutments were re-prepared intraorally to follow the new tissue margins, the decision was made to impress outside the mouth to avoid manipulation of the patient’s thin biotype tissue. Each custom abutment was removed and healing abutments were immediately inserted to avoid collapse of the tissues.
Results: Each custom abutment was placed on an implant fixture analog. Figure 6 shows the newly prepared abutment on its analog with a large-sized copper band to support impression material (alternatively, a stock quadrant impression tray could be used to provide support for the impression material). Figure 7 shows the custom abutment with cotton and wax placed to prevent impression material from entering the screw-access chamber, and Figure 8 illustrates the impression technique. This avoids the need to place retraction cord in the sulcus around the implant. This technique is also useful for adding to the margins of the provisional.
Case 3 – Remilling of Custom Abutments
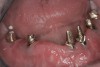
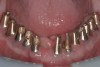
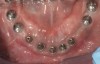
Background: In this case, the patient had a failing mandibular and maxillary dentition due to caries secondary to radiation-induced xerostomia. The patient had had a radical neck dissection to remove a squamous cell carcinoma of the throat 9 years prior to his prosthodontic consultation with the authors. The patient reported a history of radiation therapy following surgery, but did not have a shielding stent. A staged approach was used so as to avoid removable prosthetics on his severely dry soft tissues. He chose to treat his mandibular issues first. Figure 9 shows healing abutments next to the temporarily retained natural teeth, and Figure 10 shows the first-stage custom abutments inserted with relatively good gingival contour and no recession. Recession was clearly seen around all first-stage abutments following adjacent extractions and second-stage implant placement (Figure 11).
Results: The decision was made to remove these abutments and make a fixture-level impression of all the implants so that both new and first-stage abutments could be milled together for parallelism and proper gingival margin location. Because this requires the removal of the first-stage abutments that were retaining the provisional prosthesis, temporary abutments were placed prior to removal of all custom abutments in order to assure proper seating and vertical dimension of the provisional. These temporary abutments then retained the provisional while all custom abutments were fabricated and/or milled in the laboratory. Figure 12 shows the placement of the remilled (first-stage implants) and new (second-stage implants) custom abutments.
Case 4 – Temporary Abutments
Background: This patient had a failing mandibular right posterior dentition due to a vertical root fracture and secondary caries. The authors used screw-retained temporary abutment cylinders as an initial means of retention for the provisional bridge after the first stage of treatment, which included extractions and implant placement.
Results: The temporary cylinders screwed to the implants following placement are shown in Figure 13. They were luted to a prefabricated acrylic shell constructed from the patient’s diagnostic wax-up (Figure 14). Following removal of excess acrylic, the fixed screw-retained provisional prosthesis was inserted (Figure 15).
Case 5 – Conical Abutments Used As Temporary Abutments
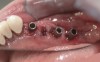
Background: The patient in this case presented with a failing dentition due to generalized severe periodontal disease with secondary endodontic lesions. She adamantly refused to wear removable transitional prostheses. Full maxillary and mandibular extractions were performed in the first phase of treatment. Not all implants could be placed in this initial phase due to the need for healing of certain grafted sites. The implants placed in this first phase were loaded with conical abutments and, in some cases, their angulated counterparts (Figure 16 and Figure 17). These stock titanium abutments were selected to avoid the need, as in Case 3, to change or remill the more costly custom abutments. They also have the advantage of making it unnecessary to use temporary cement near and around surgical sites, as they use occlusal screws only for retention.
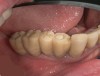
Results: Stock titanium abutments were used until all tissue healing was achieved and the secondary implants had healed. Figure 18 shows the maxillary and mandibular custom abutments inserted. Figure 19 shows a close-up of the patient’s right side quadrants, depicting the final case 15 months after initial treatment began. Recession can be seen around units corresponding to teeth Nos. 5 and 6. In this case, the authors attempted to minimize recession susceptibility by employing stock temporary screw-retained abutments during healing phases throughout the initial stages of the treatment plan. Despite these efforts, recession still occurred in certain areas where the implants were labially placed. Since the photographs shown in this case were taken, an unsuccessful attempt was made by the patient’s surgeon to graft soft tissue around these sites with recession.
Case 6 – Root Submergence
Background: This patient presented with a failing maxillary bridge spanning teeth Nos. 6 through 11. In order to keep the patient in a fixed transitional prosthesis, the first phase of treatment involved placing a provisional restoration on Nos. 6 through 11, with the first set of implants placed at sites Nos. 6 and 11. Once implants Nos. 6 and 11 integrated, custom abutments were placed, and the provisional was relined to add their support. Then implants and their respective subsequent abutments could be placed at positions Nos. 7 and 9 (Figure 20). Tooth No. 8 received elective endodontic treatment in order to be reduced and eventually submerged following insertion of the abutments at Nos. 7 and 9 (Figure 21 and Figure 22).
Results: In Figure 22, it is apparent that there is no recession around abutments Nos. 7 and 9 following root submergence. Of additional note, Figure 23 illustrates excellent bone labial to all the implants, with no recession around abutments Nos. 6 or 11. These first abutments were inserted 8 months prior to the ones at Nos. 7 and 9. The time between Figure 21, when root submergence took place, and Figure 23, when the final bridge was to be inserted, was 7 months. Figure 24 shows placement of the provisional bridge on all abutments.
Discussion
All of the above clinical cases used staged treatment plans that involved careful surgical and prosthetic planning. The one common difficulty throughout each case was managing the soft-tissue architecture. The gingival recession seen in most of these complex cases highlights the importance of careful consideration of various factors that can lead to recession, even in simpler cases. The potential causes of gingival recession, and related considerations when treatment planning implant-supported rehabilitations, are discussed in the following sections.
Implant Position
Quantity of buccal bone—Le and Borzabadi-Farahani concluded that a minimum of 2 mm of facial bone is necessary to prevent future recession.23 Bashutski and Wang noted that the most common esthetic complication is gingival recession, and cited inadequate buccal bone thickness, implants placed too far buccally, and failure to graft “jumping distance” during immediate placement in the etiology of recession.22 Case 5’s final result (Figure 19) shows more than 2 mm of labial recession around the implant-supported abutments at sites Nos. 5 and 6 (this was also the case at sites Nos. 13 and 14). Referring back to Figure 17, it is apparent that sites Nos. 5, 6, 8, and 12 demonstrate very little buccal soft tissue due to the labial placement of the implants. Butler and Kinzer support the premise that there must be adequate bone volume facially, even when the implant is placed ideally, and they found that many complications are related more to the implant position and the associated anatomical findings.21
Buccal-labial position of implants—Saadoun and Touati concluded that the buccal orientation of the implant will impinge upon the buccal cortical wall and induce bone resorption and apical migration of the tissue.13 Chu et al reported that if the implant is not placed more palatally and 3-mm to 4-mm apical to the free gingival margin to assure the proper emergence profile, the esthetic outcome may be compromised.34 Bengazi et al’s 2-year longitudinal study demonstrated that anteriorly positioned implants demonstrated slightly more recession than implants in posterior positions.17 Buccal implant placement can be clearly seen in Case 5 (Figure 17) with healing abutments in place.
Proximity to adjacent implants—Tarnow et al24 and Tarnow et al25 recommend that a minimum of 3 mm of bone exist between two adjacent implants. In sites Nos. 13 and 14 (Case 5) the fixture heads have less than 2 mm between them, and the abutments have less than 1 mm (Figure 17). Because interdental tissues do not have the same level of support between implants as they do with natural teeth, interdental distance becomes more critical in predicting the final soft-tissue position.
Implant tissue depth—While not an issue in any of the cited cases, proper depth during implant placement is also important. Bashutski and Wang suggest that placing an implant too deep may result in bone loss and gingival recession, and they recommend implant placement at 1.5 mm to 3 mm below the cementoenamel junction for optimal esthetics.22
Preoperative tooth position—Rasner notes that patients with periodontal disease requiring tooth replacement often have osseous defects that, if left untreated, can result in esthetic failures. When the gingival margin of the tooth to be extracted is apical to the desired implant position, it may be beneficial to employ orthodontic forced eruption prior to extraction, which allows the tooth or teeth surrounding bone and papilla to be moved coronally.35 Salama and Salama demonstrated that this will enhance both the alveolar bone and soft-tissue profile prior to extraction and implant placement.36 Saadoun and Touati note that after 8 weeks of extrusion, the gingival margin and papilla are located at a level that is compatible with the future implant crown position, followed by 3 months of splinting to gain bone maturation and gingival stability.12 Again, while this is a critical factor, none of the patients in the presented cases required orthodontic therapy to correct preoperative tooth position.
Biotype: Thin Vs. Thick
Cases 3 and 5 presented with a thin-scalloped architecture or biotype. Lee et al20 and Le and Borzabadi-Farahani23 cite this biotype as a major determining factor for increased susceptibility to recession. Kao and Pasquinelli note that for thin biotypes, both acute and chronic inflammation will result in gingival recession. Because patients with a thin biotype respond to periodontal, surgical, or other soft-tissue traumas with recession, additional care and careful treatment planning must be done to minimize the possibility of soft-tissue loss and increase the chance for esthetic success.37
As Saadoun and Touati point out, a thick biotype with a greater amount of attached keratinized gingiva will have more resistance to traumatic or inflammatory recession, while a thin biotype is more susceptible to peri-implant recession induced by the resorption of the thin labial cortical plate.13 Bashutski and Wang recommended that for patients with thin biotypes with less than 1.5-mm facial gingival thickness, implants should be placed more palatally and apically.22 Saadoun and Touti suggest that a connective tissue graft will convert a thin biotype into a thick gingival biotype, which will ultimately enhance gingival stability and improve tissue management throughout the restorative phase.13 Minor grafting to improve the level of attached keratinized tissue was employed in Cases 3 and 6.
Surgery
Number of surgical steps—In many cases, the patient’s treatment plan may consist of both serial extraction and phased implant placement involving as many as four different surgeries, including extractions, implant placement, and uncovering at different stages. The authors believe that reducing the number of surgical interventions may minimize the amount of recession as well as the potential for soft-tissue changes. Cordaro et al also concluded that one of the main drawbacks of a serial extraction/staged approach is extended treatment time and multiple surgical steps.1 In addition, Saadoun and Touati point out that forced eruption may be the best solution for patients with a thin biotype to limit the number of surgical procedures by improving the hard- and soft-tissue profile prior to extraction.12
Surgical preservation protocols—One of the most critical surgical strategies, according to Chu et al, should be atraumatic tooth removal without flap elevation. This is particularly critical in the esthetic zone, where the buccal bone plate and soft tissues are the thinnest. They reason that it is vital to maintain the remaining blood supply from the periosteum and endosteum for maximum healing potential.34
Penarrocha-Oltra et al suggest the use of particulate autogenous bone to fill implant-bone gaps wider than 2 mm and to cover any dehiscences and fenestrations.38 Chu et al recommend using autogenous allograft, xenografts, and synthetic bone materials in the gaps to improve bone contours for better hard- and soft-tissue volume.34 In a recent review of surgical techniques, Orgeas et al concluded that most socket-preservation techniques are effective in preserving horizontal and vertical ridge height. Their meta-analysis concluded barrier membranes alone might improve healing in extraction sites.39
Despite the use of these intricate surgical preservation protocols, soft-tissue preservation did not always occur in the cases above. Cases 1 and 3 employed such techniques; however, recession resulted following post-surgical healing, which may have been due to other contributing factors.
Implant Type
Internally versus externally connected abutments—Recession occurred in Cases 3 and 5, both of which utilized externally hexed implants from two different manufacturers. One factor could have been what Zipprich et al referred to when they discussed both internal and external abutment connections. In their 2007 study, they demonstrated that an external connection can allow for the potential for micromovement, which may lead to crestal bone loss and subsequent soft-tissue recession.31
Implant diameter: standard versus wide or narrow—Saadoun and Touati report that soft-tissue recession around wide-diameter implants measured, on average, 1.58 mm compared to 0.57 mm around standard-diameter implants.12 Small et al suggest that smaller-diameter implants may be more beneficial than wider ones in the esthetic zone, because wider ones may leave thinner labial or buccal bone, which leads to a potential for increased crestal resorption.40 All the cases presented above utilized standard- to small-diameter implants in esthetic zones; therefore, the occurrences of recession was likely due to other factors.
Types of Abutments: Temporary, Stock Titanium, Custom
Cases 1 and 3 demonstrate that placing final abutments adjacent to planned extraction teeth and implant sites during staged approaches often results in gingival recession apical to the shoulder of the final abutments. A better protocol would be to place temporary abutments to secure the provisional, and only once all the teeth have been extracted, all the implants have integrated, and the tissue is stable should impressions be taken for the final abutments. The options prior to final abutments include temporary abutments, as utilized in Case 4; stock titanium abutments would be another option. This would result in a greater degree of gingival predictability because the final abutments and final restoration are fabricated from a post-surgical and, more importantly, a post-healing impression.
All six cases reviewed in this paper used cast custom abutments. While the tissue cuff and contour can be precisely designed per patient, it is not this design that determines recession; rather, the authors believe, it is the timing that determines the soft-tissue outcomes in these staged treatment plans. Some clinicians have converted their techniques to CAD/CAM custom abutments. Several companies suggest that this offers the advantage that two custom abutments can be produced for each implant—one that can be used as a temporary abutment for a temporary phase of treatment, and the other as a final abutment for the final restoration.41,42 While this may offer a benefit, if recession occurs, the implants will still have to be re-impressed or the clinician will have to modify the second abutment with one or more of the techniques discussed above to accommodate the changes in the gingival margins.
Extraction Vs. Root Submergence
Case 6 demonstrates the use of root submergence adjacent to implants. Teeth that have been temporarily retained to secure a provisional during osseointegration can be reduced to a subosseous level and submerged rather than extracted. Salama et al reported that the use of the root submergence technique for pontic site development can result in a minimization of crestal bone resorption and an increased preservation of surrounding soft tissue.29 This ultimately results in a greater degree of gingival stability and predictability.
Immediate Loading Option
Tarnow et al reported that implants stabilized by splinting at initial placement, using the widest anterior-posterior distribution, were able to resist the critical degree of micromovement at the bone–implant interface.43 Lemongello44 and Cooper et al45 suggested that immediate implant placement is recommended for its ability to reduce gingival tissue loss following extraction and maintenance of gingival and alveolar structures. In addition, the advantages of immediate provisionalization include an elimination of additional surgery, immediate nonocclusal loading in some partially edentulous patients, bone preservation, and esthetic benefit. As shown in Case 4, which was an immediately loaded case, no gingival recession was observed.
Regardless of the specific etiology of gingival recession, staged-approach implant treatment plans usually will involve some, if not all, of the factors of potential recession outlined above. The best protocol to avoid recession or to adapt to the changing gingival contours might be to proceed with final custom abutments only when all surgical healing is completed. The ideal practice is to use what the authors call a “staged abutment protocol,” utilizing temporary abutments or stock conical or angled abutments with related temporary cylinders. This staged-abutment protocol would not use a final abutment until all soft-tissue healing has occurred. Then and only then should new fixture-level impressions be done to fabricate these final custom abutments.
Conclusion
The causes of gingival recession are multifactorial. In light of studies that illustrate increased gingival recession when implants are placed buccally or with minimal buccal bone, too close to one another, too deep, are externally connected, employ wide-bodied implants in the esthetic zone, or when the preoperative tooth position is too apical, or a staged approach is required, gingival recession should be anticipated as a possible sequela following extractions and second-stage implant placement. This necessitates reevaluation during the treatment-planning phase to minimize the possibility of gingival recession. Should recession occur, various techniques can be used to modify the final abutments. These range from re-preparing the abutments intraorally and impressing them intraorally or extraorally, or remilling the first set of abutments at the time the second set of implant abutments are being constructed. Unfortunately, in all of the cases presented above, the castings for the final crowns, which were constructed by the laboratory when the abutments were made, had to be discarded and new castings made. While the final result is esthetically acceptable, this can dramatically increase the laboratory costs to the restorative dentist as well as the amount of time required for treatment.
Therefore, it is important to reconsider using temporary abutments rather than final custom abutments while waiting for the second stage of implants to osseointegrate. Temporary abutments would secure the provisional while allowing a fixture-level impression of all the integrated implants to be taken following gingival healing. Thus, when utilizing a staged approach, one must employ staged abutments rather than proceed to the final abutment before all the implants have healed to ensure a greater degree of soft-tissue predictability. Alternatively, immediate loading should be considered to ensure stability of the gingival tissue and minimal future changes following fixture-level impressions. In either case, proper treatment planning and understanding the potential causes of gingival recession are paramount.
Disclosure
The authors had no disclosures to report.
About the Authors
Louis R. Marion, DMD, MS
Clinical Assistant Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Clinical Assistant Professor, Department of Oral and Maxillofacial Surgery and Pediatric Dentistry, Children’s Hospital of Philadelphia, Philadelphia, Pennsylvania; Prosthodontist, Private Practice, Philadelphia, Pennsylvania
Leslie Stone Hirsh, DDS
Clinical Assistant Professor, Department of Preventive and Restorative Sciences, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Prosthodontist, Private Practice, Philadelphia, Pennsylvania
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
References
1. Cordaro L, Ferrucio T, Ercoli C, Gallucci G. Transition from failing dentition to a fixed implant-supported restoration: a staged approach. Int J Periodontics Restorative Dent. 2007;27(5):481-487.
2. Ercoli C, Geminiani A, Heeje L, et al. Restoration of immediately loaded implants in a minimal number of appointments: a restrospective study of clinical effectiveness. Int J Oral Maxillofac Implants. 2012;27(6):1527-1533.
3. Waliszewski M, Janakievski J. Sequencing patients to implant-supported, full-mouth reconstructions: A case report. Pract Proced Aesthet Dent. 2005;17(4):267-272.
4. Cavallaro JS Jr. The classification and clinical application of the serial extraction protocol for full- and partial-arch fixed prostheses. Pract Proced Aesthet Dent. 2008;20(6):377-382.
5. Greenstein G, Cavallaro J Jr. Serial extraction protocol: transitioning a hopeless dentition to a full-arch reconstruction. Compend Contin Educ Dent. 2008;29(9):526-534.
6. Johansson B, Friberg B, Nilson H. Digitally planned, immediately loaded dental implants with prefabricated prostheses in the reconstruction of edentulous maxillae: a 1-year prospective, multicenter study. Clin Implant Dent Relat Res. 2009;11(3):194-200.
7. Katsoulis J, Pazera P, Mericske-Stern R. Prosthetically driven, computer-guided implant planning for the edentulous maxilla: a model study. Clin Implant Dent Relat Res. 2009;11(3):238-245.
8. Junker R, Dimakis A, Thoneick M, Jansen JA. Effects of implant surface coatings and composition on bone integration: a systematic review. Clin Oral Implants Res. 2009;20(4 suppl):185-206.
9. Piattelli A, Pontes AE, Degidi M, Iezzi G. Histologic studies on osseointegration: soft tissues response to implant surfaces and components. A review. Dent Mater. 2011;27(1):53-60.
10. Albrektsson T, Zarb G, Worthington P, Eriksson AR. Long-term efficacy of currently used dental implants: A review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
11. Jemt T, Lekholm U, Grondahl K. A 3-year followup of early single implant restorations: Ad modum Brånemark. Int J Periodontics Restorative Dent. 1990;10(5):340-349.
12. Saadoun AP, Touati B. Soft tissue recession around implants: is it still unavoidable? Part I. Pract Proced Aesthet Dent. 2007;19(1):55-62.
13. Saadoun AP, Touati B. Soft tissue recession around implants: is it still unavoidable? Part II. Pract Proced Aesthet Dent. 2007;19(2):81-87.
14. Rose LF, Mealey B, Genco R, Cohen DW. Periodontics: Medicine, Surgery and Implants. Philadelphia, PA: Mosby; 2004:122-128.
15. Adell R, Lekholm U, Rockler B, et al. Marginal tissue reactions at osseointegrated titanium fixtures (I). A 3-year longitudinal prospective study. Int J Oral Maxillofac Surg. 1986;15(1):39-52.
16. Aspe P, Zarb GA, Schmitt A, Lewis DW. The longitudinal effectiveness of osseointegrated dental implants. The Toronto study: peri-implant mucosal response. Int J Periodontics Restorative Dent. 1991;11(2):94-111.
17. Bengazi F, Wennstrom JL, Lekholm U. Recession of the soft tissue margin at oral implants. A 2-year longitudinal prospective study. Clin Oral Implants Res. 1996;7(4):303-310.
18. Small PN, Tarnow DP. Gingival recession around implants: A 1-year longitudinal prospective study. Int J Oral Maxillofac Implants. 2000;15(4):527-532.
19. Greenstein G, Cavallaro J. The clinical significance of keratinized gingiva around dental implants. Compend Contin Educ Dent. 2011;32(8):24-31.
20. Lee A, Fu JH, Wang HL. Soft tissue biotype affects implant success. Implant Dent. 2011;20(3):e38-e47.
21. Butler B, Kinzer GA. Managing esthetic implant complications. Compend Contin Educ Dent. 2012;33(7):514-522.
22. Bashutski JD, Wang HL. Common implant esthetic complications. Implant Dent. 2007;16(4):340-348.
23. Le BT, Borzabadi-Farahani A. Labial bone thickness in area of anterior maxillary implants associated with crestal labial soft tissue thickness. Implant Dent. 2012;21(5):406-410.
24. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
25. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
26. Dachi, SF, Howell FV. A survey of 3,874 routine full-mouth radiographs. I. A study of retained roots and teeth. Oral Surg Oral Med Oral Pathol. 1961;14:916-924.
27. O’Neal RB, Gound T, Levin MP, del Rio BCE. Submergence of roots for alveolar bone preservation. I. Endodontically treated roots. Oral Surg Oral Med Oral Pathol. 1978;45(5):803-810.
28. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single tooth extraction: a clinical and radiographic twelve-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
29. Salama M, Ishikawa T, Salama H, et al. Advantages of the root submergence technique for pontic site development in esthetic implant therapy. Int J Periodontics Restorative Dent. 2007;27(6):521-527.
30. Jansen VK, Conrads G, Richter EJ. Microbial leakage and marginal fit of the implant-abutment interface. Int J Oral Maxillofac Implants. 1997;12(4):527-540.
31. Zipprich H, Weigl P, Lange B, Lauer HC. Micromovements at the implant-abutment interface: measurement, causes, and consequences. Implantologie. 2007;15(1):31-46.
32. Brunski J. Biomechanics of dental implants. In: Block MS, Kent JN, eds. Endosseous Implants for Maxillofacial Reconstruction. W.B. Saunders Co.: Philadelphia, PA; 1995:22-39.
33. Partalis C, Kampiosiora P, Papavasilou G, Doukoudakis A. Fabrication of a fixed provisional implant restoration. A report of three cases. Eur J Prothodont Restor Dent. 2010;18(2):55-59.
34. Chu SJ, Salama MA, Salama H, et al. The dual-zone therapeutic concept of managing immediate implant placement and provisional restoration in anterior extraction sockets. Compend Contin Educ Dent. 2012;33(7):2-11.
35. Rasner, SL. Orthodontic extrusion: an adjunct to implant treatment. Dent Today. 2011;30(3):104-109.
36. Salama H, Salama MA. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent. 1993;13(4):312-333.
37. Kao RT, Pasquinelli K. Thick vs. thin gingival tissue: a key determinant in tissue response to disease and restorative treatment. J Calif Dent Assoc. 2002;30(7);521-526.
38. Penarrocha-Oltra D, Covani U, Aparicio A, et al. Immediate versus conventional loading for the maxilla with implants placed in fresh and healed extraction sites to support a full-arch prosthesis: nonrandomized controlled clinical study. Int J Oral Maxillofac Implants. 2013;28(4):1116-1124.
39. Vittorini Orgeas G, Clementini M, De Risi V, de Sanctis M. Surgical techniques for alveolar socket preservation: a systematic review. Int J Oral Maxillofac Implants. 2013;28(4):1049-1061.
40. Small PN, Tarnow DP, Cho SC. Gingival recession around wide-diameter versus standard-diameter implants: A 3- to 5-year longitudinal prospective study. Pract Proced Aesthet Dent. 2001;13(2):143-146.
41. Howell KJ, McGlumphy EA, Drago C, Knapik G. Comparison of the accuracy of Biomet 3i Encode Robocast technology and conventional implant impression techniques. Int J Oral Maxillofac Implants. 2013;28(1):
228-240.
42. Priest G. Virtual-designed and computer-milled implant abutments. J Oral Maxillofac Surg. 2005;63(9 suppl 2):22-32.
43. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12(3):319-324.
44. Lemongello GJ Jr. Immediate custom implant provisionalization: a prosthetic technique. Pract Proced Aesthet Dent. 2007;19(5):273-279.
45. Cooper LF, Rahman A, Moriarity J, et al. Immediate mandibular rehabilitation with endosseous implants: simultaneous extraction, implant placement, and loading. Int J Oral Maxillofac Implants. 2002;17(4):517-525.