You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
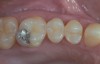
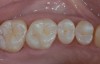
Strong and durable adhesion to tooth substrate is critical for clinical long-term success of resin-bonded direct and indirect restorations. Resin-composite restorative materials are applied directly in the oral cavity (Figure 1 and Figure 2) but undergo a certain degree of shrinkage on polymerization, resulting in the possible formation of a gap at the resin/tooth interface. Bonding agents, paired with the application of resin composites, attempt to seal the interface between the cavity and the restorative material, thus reducing the risk of interfacial gap formation, marginal leakage, postoperative sensitivity, and recurrent caries.
Adhesion to tooth substrate is based on an exchange process in which inorganic tooth material is replaced by synthetic resin. This process involves two phases: one phase consists of removal of calcium phosphates, by which microporosities are exposed in both enamel and dentin surfaces; the other, the so-called hybridization phase, involves infiltration and subsequent in situ polymerization of resin within these microporosities. The result is a micromechanical interlocking of the resin with the tooth structure.1
Buonocore2 was the first to demonstrate that etching of enamel with phosphoric acid enlarges the microscopic surface area for better resin penetration and increases resin-enamel bond strength. Resin treatment of acid-etched enamel created a new structure that was neither enamel nor resin but a hybridization of the two.3 This was the first description of the “hybrid layer,” although the term had not yet been introduced. While adhesion to enamel was effectively achieved with this hybrid interlocking, adhesion to dentin was not reliable.
Enamel is almost homogenous in structure, consisting of 95% mineral by weight. In contrast, dentin is heterogeneous, containing vital tissue with 70% mineralized structure by weight. Dentin has a relatively high organic content with a tubular structure that contains odontoblastic processes and continuous moist conditions due to the presence of dentinal fluid, intratubular pressure, and high permeability.4 Nakabayashi et al5 were first to demonstrate hybrid layer formation in dentin and showed that resins could infiltrate into acid-etched dentin to form a new structure composed of a resin matrix reinforced by collagen fibers of the organic structure.
Dentin bonding strategies can be classified according to their historical progression (1st to 7th generations) and adhesive strategies employed. This article gives an overview of current self-etch and etch-and-rinse dentin bonding systems.
Historical Development of Dentin Bonding Agents
The first generation of adhesives bonded to dentin by interaction of bifunctional resin molecules with calcium ions of hydroxyapatite. Buonocore et al6 confirmed in 1956 that a glycerophosphoric-acid-dimethacrylate-containing resin would bond to acid-etched dentin. Nine years later, Bowen7 introduced a different adhesive solution using N-phenylglycine and glycidyl methacrylate (NPG-GMA). The bond strengths with these early systems were only 1 to 3 MPa.
In the late 1970s, 2nd-generation systems were introduced. The majority of these incorporated halophosphorous esters of unfilled resins such as bisphenol-A glycidyl methacrylate (Bis-GMA) and hydroxyethyl methacrylate (HEMA). The mechanism by which these bonded to dentin was an ionic bond to calcium, facilitated by chlorophosphate groups. The bonds to dentin were weak and prone to hydrolysis, but presented a significant improvement over 1st-generation systems. The smear layer was incorporated into the bonding process for both of the first two generations. Bond strengths seldom exceeded 5 to 6 MPa.8
Third-generation dentin bonding agents involved acid-etching of dentin, application of a hydrophilic resin phosphate primer, and an unfilled adhesive resin. Etching of the dentin partially removed and/or modified the smear layer, opened dentinal tubules, and increased their permeability. The primer contained hydrophilic resin monomers, including hydroxyethyl trimellitate anhydride (4-META) and biphenyl dimethacrylate (BPDM). It infiltrated and modified the smear layer and thereby promoted adhesion to dentin. Following primer application, an unfilled resin was placed on dentin and enamel. However, bonding to smear-layer-covered dentin was not very successful before 1990, because the resins were not able to penetrate through the smear layer and the smear layer was very weak.9 Scotchbond™ 2 (3M ESPE, www.3MESPE.com) was the first product to receive acceptance by the American Dental Association. Other popular 3rd-generation systems were Clearfil™ New Bond (Kuraray Dental, www.kuraraydental.com), Coltène® A.R.T. Bond (Coltène Whaledent, www.coltene.com), C&B-MetaBond® (Parkell, Inc., www.parkell.com), Gluma® (Heraeus Kulzer, www.heraeus-dental-us.com), and Tenure® (DenMat, www.denmat.com).
Complete removal of the smear layer was achieved with 4th-generation bonding systems through application of a total-etch technique.10 Today, these systems are generally offered with 30% to 40% phosphoric acid gels and are referred to as three-step etch-and-rinse adhesives. With the introduction of the multi-step application procedure, the term “bonding agent” was then replaced by the term “adhesive system.” Representative adhesives in this group are All-Bond 2® (BISCO, Inc. www.bisco.com), Scotchbond™ Multi-Purpose (3M ESPE), and PermaQuik® (Ultradent Products, Inc., www.ultradent.com).
Because of the complexity and number of steps involved with the application of 4th-generation bonding systems, researchers and manufacturers have aimed to simplify the clinical procedure by reducing the number of bonding steps and, thus, working time. Fifth-generation adhesives are usually called “one-bottle systems.” They comprise a separate etch-and-rinse phase followed by the application of a combined primer-adhesive-resin solution. Despite being dubbed one-bottle systems, they require two steps: acid-etching and adhesive application.1 Commercial products include OptiBond® Solo (several versions) (Kerr Corporation, www.kerrdental.com), Prime & Bond® (several versions) (DENTSPLY Caulk, www.dentsply.com), Adper™ Single Bond (3M ESPE), and Excite® (Ivoclar Vivadent Inc., www.ivoclarvivadent.com).
Sixth-generation adhesives are usually referred to as self-etch adhesives. These non-rinsing adhesives do not require a separate acid-etch step, as they condition and prime enamel and dentin simultaneously by infiltrating and partially dissolving the smear layer and hydroxyapatite to generate a hybrid zone that incorporates minerals and the smear layer.11 The first self-etch adhesives were composed of two solutions: an acidic primer and a bonding resin. Later, one-step/two-component self-etch adhesives appeared on the dental market. Representative 6th-generation two-step self-etch adhesives include AdheSE® (Ivoclar Vivadent Inc.), Clearfil™ SE Bond (Kuraray Dental), OptiBond® Solo Plus Self-Etch (Kerr Corporation), and Prelude™ Dentin Adhesive (Danville Materials, www.danvillematerials.com). Two-component self-etch adhesives are Adper™ Prompt™ L-Pop™ (3M ESPE) and Xeno® III (DENTSPLY Caulk).
Seventh-generation adhesives combine conditioning, priming, and application of adhesive resin in one bottle. They are, therefore, named “single-component one-step self-etch adhesives” or “all-in-one adhesives.” Representative products include Clearfil™ S3 Bond (Kuraray Dental), G-Bond™ (GC America Inc., www.gcamerica.com), iBond® (Heraeus Kulzer), and Xeno® IV (DENTSPLY Caulk).
Adhesive Strategies
Adhesives are the compounds containing both hydrophilic monomers that allow bonding to tooth structure and hydrophobic monomers that contribute to coupling with restorative materials. All adhesives involve three major steps that are responsible for a durable adhesive/dentin-bonding interface: 1) etching; 2) priming; and 3) bonding. Etching involves an acidic solution that demineralizes the enamel/dentin surface, thus creating a surface that is more receptive for bonding. The primer is composed of a mixture of hydrophilic monomers and solvents, aiming to improve the wettability of the tooth structure and to permit substitution of the water retained within the substrate with the resin monomers by expanding collagen fibers of dentinal tissue. The bonding agent contains the hydrophobic part of the system that allows coupling with the resin-based composite restorative material.
Bonding strategies can, therefore, be classified according to the number and combination of treatment steps:
1. Etch-and-rinse three-step adhesive systems—These systems are characterized by the subsequent application of etching, primer, and bonding agent in separate solutions. Dentin and enamel are treated with an acid gel to remove the smear layer and demineralize the most superficial hydroxyapatite crystals. This results in exposed dentin collagen fibrils, which are nearly completely uncovered from hydroxyapatite and form a micro-retentive network. Establishment of a thick hybrid layer occurs due to micromechanical entanglement of resin monomers with etched dentin.12
2. Etch-and-rinse two-step adhesive systems—These systems are characterized by a combined primer and bonding agent in one bottle. Prior etching of the enamel and dentin surfaces is necessary for optimal bonding.
Etch-and-rinse adhesives that utilize three steps seem more durable than two-step etch-and-rinse adhesives.13 In dentin, water is required to prevent collapse of the collagen fibers for proper formation of the hybrid layer. Two clinical techniques have been suggested to achieve adequate hybridization: the dry-bonding and the wet-bonding techniques, which differ in respect to the solvent used in the primer/adhesive. With etch-and-rinse adhesive systems, hydrophilic primer monomers are dissolved in volatile solvents, such as acetone and ethanol, and primer solvents are then evaporated by gentle air-drying, leaving the active primer monomers behind.
When applying the dry-bonding technique, the substrate field is air-dried. The collagen network on the demineralized dentin surface collapses as the interfibrillar spaces between the exposed collagen fibrils are being lost. Adhesive systems containing water-based primers re-hydrate and, therefore, re-expand the air-dried and collapsed dentin collagen network.3
Alternatively, the acid-etched dentin surface can be kept moist with the wet-bonding technique, introduced by Kanca and Gwinnett in 1992.14,15 This technique-sensitive approach is recommended for etch-and-rinse systems that contain an acetone-based adhesive. It increases resin/dentin-bond strengths and enables good dentin sealing with less postoperative sensitivity. However, the optimal amount of surface wetness necessary to maintain the integrity of collagen without compromising bond strength is difficult to determine.
Three-Step Vs. Two-Step Etch-and-Rinse Adhesives
Bond strength results obtained with one-bottle two-step adhesives appear to be less consistent than those recorded for three-step adhesives. Also, three-step etch-and-rinse adhesives have demonstrated superior bonding performance compared to two-step adhesives.16
One-bottle two-step etch-and-rinse adhesives seem more technique-sensitive and provide weaker resin-collagen interaction.3
1. Self-etch two-step adhesive systems—These systems require application of self-etching primer to the enamel and dentin, followed by a separate hydrophobic bonding agent. The self-etch effect is derived from monomers to which carboxylic or phosphate acid groups are added.
2. Self-etch one-step adhesive systems—Combining etchant, primer, and adhesive into one bottle, these systems do not require mixing; they are also called “all-in-one adhesives.”
In general, self-etch adhesives have the advantage of demineralizing and infiltrating the tooth surface simultaneously to the same depth, ensuring complete penetration of the adhesives. Self-etch adhesives can be mild or strong, depending on their pH. Strong self-etch adhesives with a pH < 1 are able to completely dissolve the smear layer, similar to etch-and-rinse systems, and almost completely demineralize the dentin surface. In contrast, mild adhesives (pH around 2) usually contain weaker acids like maleic, citric, oxalic, and nitric acids in lower concentrations and, therefore, partially demineralize the dentin matrix, leaving residual hydroxyapatite crystals on the collagen fibrils to provide additional chemical bonding.17 Laboratory and clinical data with strong self-etch adhesives have shown that despite their reasonable bonding potential to enamel, they are not reliable on dentinal surfaces with regard to bond durability and restoration longevity.18,19
Two-Step Vs. One-Step Self-Etch Adhesives
One-step self-etch adhesives reportedly produce lower bond strengths to dentin than two-step self-etch and etch-and-rinse adhesives.20,21 However, it has been confirmed that application of the all-in-one adhesive in multiple layers may result in higher bond strength.22 One-step self-etch adhesives are extremely hydrophilic as they contain high concentrations of both ionic and hydrophilic monomers. A large amount of water is added to these one-step adhesive solutions. It is, therefore, difficult to evaporate water from these one-step self-etch adhesives. Even if evaporation is successful, water will rapidly diffuse back from the bonded dentin into the adhesive resin, creating permeable membranes and water movement across the adhesive layer (Figure 3 and Figure 4), contributing to the degradation of the resin/dentin bond.23 Moreover, one-step self-etch adhesives are technique-sensitive and have a reduced shelf life.11
Self-Etch Vs. Etch-and-Rinse Adhesives
Clinically, self-etch systems do not require a separate etching step. They not only eliminate some application steps, but also reduce technique sensitivity (ie, no wet bonding, just simple drying) associated with etch-and-rinse adhesives. Etch-and-rinse adhesives are considered to be technique-sensitive for adequate dentin bonding, because overdried dentin causes demineralized collagen fibers to collapse and reduce monomer diffusion among the collagen fibers. In addition, the presence of excessive humidity may result in incomplete monomer polymerization and water absorption in the hybrid layer.3,24
Self-etch adhesives are also associated with absence or lower incidence of postoperative sensitivity. Most self-etch adhesive systems are water-based and, therefore, simplify dentin moisture control. One has to keep in mind that air drying is an important step and that the duration of air blowing and the pressure of air stream are different for each product. Deviations from suggested protocols may affect the bonding capacity of the systems. Sano et al25 confirmed that, to obtain optimal bonding performance with a dentin adhesive system, the operator should be aware of the technique sensitivity of the system. Clinical experience also seems important as operator experience influences bond strength values of dentin bonding systems.26 Omission of the etch-and-rinse step with self-etch adhesive reduces the risk of errors during application and manipulation of the material in clinically inexperienced operators.
Multi-step self-etch and etch-and-rinse adhesives have shown almost the same performance on different tooth substrates, such as intact, sclerotic, and caries-affected dentin.27-29 Conversely, a self-etch adhesive performed better on amelogenesis-imperfecta-affected enamel surfaces than an etch-and-rinse adhesive bonding agent. Interestingly, the most simplified (one-step self-etch and two-step etch-and-rinse) adhesives have shown the least clinical durability, while other multi-step adhesives revealed reliable performances. Insufficient resin impregnation of dentin, high permeability of the bonded interface, lack of polymerization, phase separation, and activation of endogenous colleganolytic enzymes are some of the factors that reduce the longevity of the bonded interface. The etch-and-rinse technique is considered to be sensitive because of reduced resin-monomer diffusion within the etched dentin, which results in incompletely infiltrated zones along the bottom of the hybrid layer that contain denuded collagen fibrils.30
For enamel, an etch-and-rinse approach using phosphoric acid remains the preferred option. Scanning electron microscopic studies indicate that the enamel etching pattern caused by self-etch adhesive is not as deep and appears less retentive than the one achieved with phosphoric acid. The degree of enamel etching with self-etch adhesives depends on the pH of the adhesive system. Bonding of self-etch systems to enamel still remains critical, and, typically, separate phosphoric acid-etching of unground enamel surfaces is recommended.24
Clinical Recommendations
Self-etch adhesives have brought resin bonding to dentin to new levels and are superior to previous concepts and approaches, both in performance and simplicity of application. To enamel, however, etch-and-rinse adhesives involving phosphoric acid-etching are still widely preferred, as the stronger etchant creates a more pronounced etching pattern and a more retentive surface with improved wettability. The scientific evidence available today reveals great variations and makes determination of the “better” approach difficult. Therefore, the selection of a bonding agent is often a matter of personal preference. Clinical recommendations and guidelines, however, can be based on the individual situation and desired treatment. As a general rule, the greater the amount of remaining enamel, the more likely the use of an etch-and-rinse adhesive should be. This is especially true for indirect restorations, such as bonded laminate veneers, where the ideal preparation is preferably confined to enamel. Self-etch adhesives are typically light-cure materials and perform better when light-cured before composite/restoration application.31 Many of them also have an increased film thickness, which may make final cementation of well-fitting indirect restorations difficult.
For direct composite resin restorations, especially when the cavity comprises large areas of dentin, self-etch adhesives seem to be the bonding agents of choice. Large enamel surfaces approximate to the supporting dentin may benefit from “selective enamel etching,” where phosphoric acid is applied to the enamel surfaces only. Care should be taken not to apply phosphoric acid to the exposed dentin when self-etch adhesives are used. If that happens accidentally, the acid should be rinsed off with water within 10 seconds.
Dentin and enamel bonding agents have evolved dramatically over the past decades, providing excellent and durable resin bonds while supporting the quest for less invasive and more predictable conservative tooth restorations. However, these materials undergo constant improvements, and it will be interesting to follow future developments and research in this area.
Conclusions
While current trends favor fewer and simpler clinical application steps, one-step dentin bonding systems reveal lower and less predictable bond strengths than multi-step etch-and-rinse and self-etch systems. The varying evidence available today suggests that the choice between etch-and-rinse and self-etch systems is often a matter of personal preference. In general, however, phosphoric acid creates a more pronounced and retentive etching pattern in enamel. Therefore, etch-and-rinse bonding systems are often preferred for indirect restorations and when large areas of enamel are still present. Self-etch adhesives, on the other hand, provide superior and more predictable bond strength to dentin and are consequently recommended for direct composite resin restorations, especially when predominantly supported by dentin.
References
1. Summit JB, Robbins JW, Hilton TJ, Schwarz RS. Fundamentals of Operative Dentistry. 3rd ed. Hanover Park, IL: Quintessence Publishing; 2006:183-242.
2. Buonocore MG. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
3. Pashley DH, Tay FR, Breschi L, et al. State of the art etch-and-rinse adhesives. Dent Mater. 2011;27(1):1-16.
4. Lopes GC, Baratieri LN, de Andrada MA, Vieira LC. Dental adhesion: present state of the art and future perspectives. Quintessence Int. 2002;33(3):213-224.
5. Nakabayashi N, Kojima K, Masuhara E. The promotion of adhesion by the infiltration of monomers into tooth substrates. J Biomed Mater Res. 1982;16(3):265-273.
6. Brudevold F, Buonocore M, Wileman W. A report on a resin composition capable of bonding to human dentin surfaces. J Dent Res. 1956;35(6):846-851.
7. Bowen RL. Adhesive bonding of various materials to hard tooth tissues. II. Bonding to dentin promoted by a surface-active comonomer. J Dent Res. 1965;44(5):895-902.
8. Dentin bonding systems: an update. Council on Dental Materials, Instruments, and Equipment. J Amer Dent Assoc. 1987;114(1):91-95.
9. Tao L, Pashley DH, Boyd L. Effect of different types of smear layers on dentin and enamel bond strengths. Dent Mater. 1988;4(4):208-216.
10. Kanca J III. A method for bonding to tooth structure using phosphoric acid as a dentin-enamel conditioner. Quintessence Int. 1991;22(4):285-290.
11. Van Meerbeek B, Yoshihara K, Yoshida Y, et al. State of the art of self-etch adhesives. Dent Mater. 2011;27(1):17-28.
12. Perdigão J. New developments in dental adhesion. Dent Clin North Am. 2007;51(2):333-357.
13. De Munck J, Van Landuyt K, Peumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84(2):118-132.
14. Kanca J III. Resin bonding to wet substrate. I. Bonding to dentin. Quintessence Int. 1992;23(1):39-41.
15. Gwinnett AJ. Moist versus dry dentin: its effect of shear bond strength. Am J Dent. 1992;5(3):127-129.
16. Inoue S, Vargas MA, Abe Y, et al. Microtensile bond strength of eleven contemporary adhesives to dentin. J Adhes Dent. 2001;3(3):237-245.
17. Yoshida Y, Van Meerbeek B, Nakayama Y, et al. Evidence of chemical bonding at biomaterial-hard tissue interfaces. J Dent Res. 2000;79(2):709-714.
18. Shirai K, De Munck J, Yoshida Y, et al. Effect of cavity configuration and aging on the bonding effectiveness of six adhesives to dentin. Dent Mater. 2005;21(2):110-124.
19. De Munck J, Shirai K, Yoshida Y, et al. Effect of water storage on the bonding effectiveness of 6 adhesives to Class I cavity dentin. Oper Dent. 2006;31(4):456-465.
20. Bouillaguet S, Gysi P, Wataha JC, et al. Bond strength of composite to dentin using conventional, one-step, and self-etching adhesive systems. J Dent. 2001;29(1):55-61.
21. Ulker M, Ozcan M, Sengun A, et al. Effect of artificial aging regimens on the performance of self-etching adhesives. J Biomed Mater Res B Appl Biomater. 2010;93(1):175-184.
22. Ito S, Tay FR, Hashimoto M, et al. Effects of multiple coatings of two all-in-one adhesives on dentin bonding. J Adhes Dent. 2005;7(2):133-141.
23. Van Landuyt KL, De Munck J, Snauwaert J, et al. Monomer-solvent phase separation in one-step self-etch adhesives. J Dent Res. 2005;84(2):183-188.
24. Manuja N, Nagpal R, Pandit IK. Dental adhesion: mechanism, techniques, and durability. J Clin Pediatr Dent. 2012;36(3):223-234.
25. Sano H, Kanemura N, Burrow MF, et al. Effect of operator variability on dentin adhesion: student vs. dentists. Dent Mater J. 1998;17(1):51-58.
26. Unlu N, Gunal S, Ulker M, et al. Influence of operator experience on in vitro bond strength of dentin adhesives. J Adhes Dent. 2012;14(3):223-227.
27. Say EC, Nakajima M, Senawongse P, et al. Bonding to sound vs caries-affected dentin using photo-and dual-cure adhesives. Oper Dent. 2005;30(1):90-98.
28. Koyuturk AE, Sengun A, Ozer F, et al. Shear bond strengths of self-etching adhesives to caries-affected dentin on the gingival wall. Dent Mater J. 2006;25(1):59-65.
29. Karakaya S, Unlu N, Say EC, et al. Bond strengths of three different adhesive systems to sclerotic dentin. Dent Mater J. 2008;27(3):471-479.
30. Breschi L, Mazzoni A, Ruggeri A, et al. Dental adhesion review: Aging and stability of the bonded interface. Dent Mater. 2008;24(1):90-101.
31. Chapman JL, Burgess JO, Holst S, et al. Precuring of self-etching bonding agents and its effect on bond strength of resin composite to dentin and enamel. Quintessence Int. 2007;38(8):637-41.
About the Authors
Fusun Ozer, DMD, PhD
Clinical Associate
Department of Preventive and Restorative Sciences
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Markus B. Blatz, DMD, PhD
Professor of Restorative Dentistry
Chairman, Department of Preventive and Restorative Sciences
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania