You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
The physiologic loss of hard and soft tissues after tooth extraction from caries, trauma, or advanced periodontitis often leads to osseous deformities of the alveolar ridge. These deformities can present difficulty in achieving proper pontic design. In an inappropriately contoured ridge, removable dentures may exhibit compromised retention, and ideal endosseous implant placement might not be possible. Many of these problems could be eliminated if the alveolus had been preserved after tooth extraction.
Although the prevention of postextraction alveolar bone loss was first described by Greenstein and colleagues1 and Ashman and Bruins2 in 1985, the term socket preservation was first coined by Cohen in 1988 to describe a procedure designed for prosthetic socket maintenance, ridge preservation, and augmentation.3 He defined socket preservation as a surgical procedure in which graft material or a scaffold is placed in a fresh extraction socket to preserve the alveolar ridge for a future prosthesis.2,3 In 2007, the Expert Committee on Socket Preservation unanimously decided to use the term socket preservation specifically for the treatment of fresh extraction sockets with intact buccal bone walls.4 In contrast, ridge preservation was deemed an appropriate term for situations involving deficient buccal bone walls. The rationale behind this terminology is that the presence of the buccal bone wall is believed to have a relevant influence on bone healing, and these terms reflect the differences between the situations.4
Socket-Alveolus Healing
Healing of the extraction socket is a highly dynamic process, beginning with a cascade of inflammatory reactions activated immediately after tooth extraction. It occurs in five different stages (Table 1) starting with the formation of a blood clot and ending with fully mature hard- and soft-tissue structures.5
Animal studies have analyzed the dimensional ridge changes after tooth extraction.6 The remodeling process has been described in two phases. During the first phase, the bundle bone is remodeled and replaced by newly formed woven bone, causing a reduction in the vertical ridge. In the second phase, the buccal surface of the alveolar ridge is remodeled, causing a horizontal volume reduction as well as additional vertical volume reduction.
Rationale Behind Socket Preservation
A striking feature of the healing extraction socket is the chronic progressive catabolic remodeling of the residual alveolar process that results in atrophy of the alveolar process described as reduction of residual ridges.7 As a part of the extraction socket healing process and because of a lack of tooth support, bone resorbs to a flat contour, resulting in the thinning of bony structures.5 The rate of postextraction bone loss is rapid in the first 6 months, followed by gradual modeling and remodeling of the remaining bone with approximately 40% of the alveolar height and 60% of alveolar width lost in the first 6 months.8 Studies have shown that most bone loss occurs at the labial/buccal side of the alveolar process compared with the lingual/palatal side.6 The margins of the facial alveoli are thin, mostly cortical (although in rare cases they contain cancellous bone), knife-edged, and frail. The significance of implementing a less traumatic extraction (eg, using periotomes) can be emphasized when looking at the healing of damaged extraction sockets. Damaged bony walls as well as both systemic and local factors may alter the healing process and may result in the formation of fibrous tissue rather than a complete bony fill.5 The remodeled alveolar process can affect the success of prosthetic therapy with a conventional or implant-retained prosthesis, thereby underlining the importance of socket preservation.8
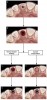
The most important esthetic goals of socket preservation are the maintenance or enhancement of the facial and interproximal gingival contours and the height of the interproximal papilla.9 The soft-tissue color, consistency, and contour are some of the important parameters that affect the esthetic outcomes of this procedure. The severity of the healing pattern poses two problems for clinicians: it creates an esthetic problem when fabricating an implant-supported restoration or a conventional prosthesis and it may make the placement of an implant challenging, if not unfeasible. However, it is possible to minimize such problems by simply carrying out ridge or socket preservation procedures in extraction sockets using grafted materials with or without barrier membranes.8 Most general dentists perform routine tooth extractions; therefore, they should consider incorporating a simple, fast, and relatively inexpensive procedure of socket preservation into their practices. In short, socket preservation: minimizes residual ridge resorption; preserves crestal ridge volume after extraction; allows ideal implant placement in relation to bone and gingival tissues; reduces or eliminates ridge augmentation procedures during implant placement; and prevents loss of both hard and soft tissues, thus providing optimum esthetic outcomes. Figure 1 depicts a schematic diagram of the procedure and importance of socket preservation.
Mechanism of Socket Preservation
The exact mechanism of alveolar ridge resorption and preservation has been said to involve a complex cascade of events.
Biomechanical Stimulation
Many authors have suggested that the random orientation of the graft placed in extraction sites provides physiologic and bioelectric stimulation of the adjacent bone via attachment and load transmission from the overlying prosthesis during normal jaw function.10 Therefore, indirect physiologic forces on the bone–graft interface may contribute to bone preservation.
Wound Isolation and the Scaffolding Effect
Wound isolation by the principles of guided tissue regeneration with membranes prevents invagination of the oral epithelium into the socket, favoring bone-regenerating cells to complete the bone fill.11 The presence of an osteoconductive bioactive framework or scaffold allows osteoblasts to migrate and form bone more efficiently within the extraction space, which facilitates bone healing.12
Modification of Cellular Activity
The physiochemical and structural characteristics of implanted bioactive material evokes a cellular response from the adjacent tissues by providing a biomimetic environment for initiating bone repair.13
Techniques Used for Socket Preservation
Various prophylactic measures that minimize injury to the alveolar process and surrounding soft tissues during tooth extraction have been attempted to minimize bone resorption. Postextraction therapeutic measures include physiologic preservation of the alveolar process by retention of the natural roots, application of prefabricated root form implants, and modified versions of guided tissue regeneration and guided bone-regeneration techniques.14
Currently, the most commonly used methods are placement of the graft/membrane alone, placing a graft and covering it with a membrane or collagen wound dressing, or placing a sponge in the socket with or without any coverage.15 All these procedures can be followed by flap advancement to achieve complete or partial primary closure (Table 2).8,13,16-39
Materials Used for Socket Preservation
An ideal graft material for the alveolar socket should prevent the volume reduction that often occurs after tooth extraction and remain in situ as a scaffold until sufficient healing (bone formation) has occurred.23 Bone-replacement materials must allow the initiation of osteogenesis and serve as a supportive frame for ingrown bone. Various graft materials, including autogenous, allogenous, xenogeneic, and alloplastic bone grafts as osseoinductive and/or osteoconductive materials, have been used in attempts to preserve the alveolar ridge. When the socket walls are intact, osteoconductive graft materials can be used and barrier membranes may not be necessary. On the contrary, when socket walls are missing, regenerative techniques using osseoinductive graft materials and/or the use of barrier membranes are used.
Studies have been conducted using various bone grafts and bone-substitute materials, including demineralized freeze-dried bone allograft (DFDBA),15 autologous bone,15 bioactive glass,19,21 hydroxyapatite,18 calcium sulphate,20,29 solvent-preserved cancellous allograft,17,28 and coral granules.22,34 It is also possible to cover the socket to prevent ingress of soft tissues, thereby promoting maximal bone healing. Generally there are two types of membranes used: resorbable and nonresorbable. In the studies, the most commonly placed membranes were expanded polytetrafluoroethylene (e-PFTE) membranes15,23,25 or collagen membranes.13,29,30 In addition, polylactic/polyglycolic (PL/PG) membranes, titanium,27 or acellular dermal matrix26 have also been evaluated in various studies.
Sponges made of PL/PG31,32,34 or collagen have also been placed in extraction sockets to preserve the ridge. The collagen sponges can also act as a carrier for either recombinant human bone morphogenetic protein-2 (rhBMP-2)33 or synthetic cell-binding peptide P-15.13 The authors suggested that the sponge served as a support to prevent the collapse of the surrounding soft tissue into the socket during the healing process.
The use of grafting materials in fresh extraction sockets has been questioned because they seem to interfere with the normal healing process in the sockets in which oral implants have to be inserted.15,16 A substantial number of the studies reported remnants of graft material particles in sockets 6 to 9 months after insertion.16,17,19,37 The long-term effect of residual grafting material on implant survival and success was not reported.
The diverse soft- and hard-tissue regenerative procedures may be technically demanding and unpredictable in the hands of most clinicians. Other evaluated alternatives are minimally invasive socket preservation procedures immediately following tooth extraction known as socket-seal surgery.35 In socket-seal surgery, a soft-tissue graft is harvested from the palate to be placed atop the bone graft in the socket. Also, the rotated pedicle palatal connective tissue flap technique has been used for soft-tissue closure of the grafted extraction sockets in the posterior maxilla without excess tension, producing optimal outcomes.36 In summary, there is strong evidence that ridge preservation significantly maintains more ridge width and height. Most grafting materials are effective and there are only slight differences between them.
Conclusion
Given the current advances in stem-cell technology, in the future it might be possible to place tooth buds in sockets to regrow teeth or place a cellular scaffold in the socket to maintain the bone. Cultivated scaffolds from bone-marrow mesenchymal stem cells have been placed into fresh extraction sockets with results that “show promise.”40
Clinically, it is evident that the healing of postextraction sockets may result in the considerable loss of alveolar ridge height and width. The deficient alveolar ridge may jeopardize its suitability for a future prosthesis, both esthetically and functionally. Hence, the new concept of socket preservation should be given thoughtful consideration to enhance the predictability and success of future prostheses. Dentists often encounter clinical situations in which teeth have to be extracted in areas of esthetic concern. As a result, the alveolar bone gets resorbed, the soft tissues shrink, and the final non-anatomical prosthesis appears to be false. Such negative results usually can be avoided by using socket preservation techniques.
References
1. Greenstein G, Jaffin RA, Hilsen KL, Berman CL. Repair of anterior gingival deformity with durapatite: report of case. J Periodontol. 1985;56(4):200-203.
2. Ashman A, Bruins P. Prevention of alveolar bone loss postextraction with HTR grafting material. Oral Surg Oral Med Oral Pathol. 1985;60(2):146-53.
3. Cohen ES. Socket preservation. In: Cohen ES, Atlas of Cosmetic and Reconstructive Periodontal Surgery. 1st ed. Philadelphia, PA; Lippincott Williams and Wilkins; 1988:347-363.
4. Ackerman KL. Extraction site management using a natural bone mineral containing collagen: Rationale and retrospective case study. Int J Periodontics Restorative Dent. 2009;29(5):489-497.
5. Al-Harbi SA. Minimizing trauma during tooth removal: A systematic sectioning approach. Eur J Esthet Dent. 2010;5(3):274-287.
6. Araujo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32(2):212-218.
7. Atwood DA. Some clinical factors related to rate of resorption of residual ridges. J Prosthet Dent. 2001;86(2):119-125.
8. Lekovic V, Camargo PM, Klokkevold PR, et al. Preservation of alveolar bone in extraction sockets using bioresorbable membranes. J Periodontol. 1998;69(9):1044-1049.
9. Darby I, Chen S, De Poi R. Ridge preservation: what is it and when should it be considered. Aust Dent J. 2008;53(1):11-21.
10. Ortman LF, Casey DM, Deers M. Bioelectric stimulation and residual ridge resorption. J Prosthet Dent. 1992;67(1):67-71.
11. Lekovic V, Kenney EB, Weinlaender M, et al. A bone regenerative approach to alveolar ridge maintenance following tooth extraction. Report of 10 cases. J Periodontol. 1997;68(6):563-570.
12. Bartee BK. Extraction site reconstruction for alveolar ridge preservation. Part 1: rationale and materials selection. J Oral Implantol. 2001;27(4):187-193.
13. Neiva RF, Tsao YP, Eber R, et al. Effects of putty-form hydroxyapatite matrix combined with the synthetic cell binding peptide P-15 on alveolar ridge preservation. J Periodontol. 2008;79(2):291-299.
14. Nair PN, Odont HC, Schug J. Observations on healing of human tooth extraction sockets implanted with bioabsorbable polylactic-polyglycolic acids (PLGA) copolymer root replicas: A clinical, radiographic, and histologic follow-up report of 8 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;97(5):559-569.
15. Darby I, Chen ST, Buser D. Ridge preservation techniques for implant therapy. J Oral Maxillofac Implants. 2009;24(Suppl):260-271.
16. Becker W, Becker BE, Caffesse R. A comparison of demineralized freeze-dried bone and autologous bone to induce bone formation in human extraction sockets. J Periodontol. 1994;65(12):1128-1133.
17. Artzi Z, Tal H, Dayan D. Porous bovine bone mineral in healing of human extraction sockets. Part 1: histomorphometric evaluations at 9 months. J Periodontol. 2000;71(6):1015-1023.
18. Nemcovsky CE, Serfaty V. Alveolar ridge preservation following extraction of maxillary teeth. Report on 23 consecutive cases. J Periodontol. 1996;67(4):390-395.
19. Froum S, Cho SC, Rosenberg E, et al. Histological comparison of healing extraction sockets implanted with bioactive glass or demineralised freeze-dried bone allograft: a pilot study. J Periodontol. 2002;73(1):94-102.
20. Guarnieri R, Pecora G, Fini M, et al. Medical grade calcium sulfate hemihydrate in healing of human extraction sockets: clinical and histological observations at 3 months. J Periodontol. 2004;75(6):902-908.
21. Camargo PM, Lekovic V, Weinlaender M. Influence of bioactive glass changes in alveolar process dimensions after exodontia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90(5):581-586.
22. Sàndor GK, Kainulainen VT, Queiroz JO, et al. Preservation of ridge dimensions following grafting with coral granules of 48 post-traumatic and post-extraction dento-alveolar defects. Dent Traumatol. 2003;19(4):221-227.
23. Lekovic V, Kenney EB, Weinlaender M, et al. A bone regenerative approach to alveolar ridge maintenance following tooth extraction. Report of 10 cases. J Periodontol. 1997;68(6):563-570.
24. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: A clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.
25. Fugazzotto PA. GBR using bovine bone matrix and resorbable and nonresorbable membranes. Part 1: histologic results. Int J Periodontics Restorative Dent. 2003;23(4):361-369.
26. Fowler EB, Breault LG, Rebitski G. Ridge preservation utilizing an acellular dermal allograft and demineralised freeze-dried bone allograft: Part 1. A report of 2 cases. J Periodontol. 2000;71(8):1353-1359.
27. Pinho MN, Roriz VL, Novaes AB Jr, et al. Titanium membranes in prevention of alveolar collapse after tooth extraction. Implant Dent. 2006;15(1):53-61.
28. Wang HL, Tsao YP. Histologic evaluation of socket augmentation with mineralized human allograft. Int J Periodontics Restorative Dent. 2008;28(3):231-237.
29. Kesmas S, Swasdison S, Yodsanga S, et al. Esthetic alveolar ridge preservation with calcium phosphate and collagen membrane: Preliminary report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;110(5):e24-e36.
30. Vasilic N, Henderson R, Jorgenson T, et al. The use of bovine porous bone mineral in combination with collagen membrane or autologous fibrinogen/fibronectin system for ridge preservation following tooth extraction. J Okla Dent Assoc. 2003;93(4):33-38.
31. Serino G, Biancu S, Iezzi G, Piattelli A. Ridge preservation following tooth extraction using a polylactide and polyglycolide sponge as space filler: A clinical and histological study in humans. Clin Oral Implants Res. 2003;14(5):651-658.
32. Serino G, Rao W, Iezzi G, Piattelli A. Polylactide and polyglycolide sponge used in human extraction sockets: Bone formation following 3 months after its application. Clin Oral Implants Res. 2008;19(1):26-31.
33. Fiorellini J, Howell T, Cochran D, et al. Randomized study evaluating recombinant human bone morphogenetic protein-2 for extraction socket augmentation. J Periodontol. 2005;76(4):605-613.
34. Molly L, Vandromme H, Quirynen M, et al. Bone formation following implantation of bone biomaterials into extraction sites. J Periodontol. 2008;79(6):1108-1115.
35. Landsberg CJ. Implementing socket seal surgery as a socket preservation technique for pontic site development: Surgical steps revisited. A report of two cases. J Periodontol. 2008;79(5):945-954.
36. Chaar ES. Soft tissue closure of grafted extraction sockets in the posterior maxilla: The rotated pedicle palatal connective tissue flap technique. Implant Dent. 2010;19(5):370-377.
37. Kfir E, Kfir V, Kaluski E. Immediate bone augmentation after infected tooth extraction using titanium membranes. J Oral Implantol. 2007;33(3):133-138.
38. Caiazzo A, Brugnami F, Mehra P. Buccal plate augmentation: a new alternative to socket preservation. J Oral Maxillofacial Surg. 2010;68(10):2503-2506.
39. Hurzeler MB, Zuhr O, Schupbach P, et al. The socket shield technique: a proof-of-principle report. J Clin Periodontol. 2010;37(9):855-862.
40. Marei MK, Nouh SR, Saad MM, Ismail NS. Preservation and regeneration of alveolar bone by tissue-engineered implants. Tissue Eng. 2005;11(5-6):751-767.
Related Content:
Learn more about bone grafting/tissue regeneration materials at: dentalaegis.com/go/cced123
For more information, read Alveolar Ridge Augmentation at: dentalaegis.com/go/cced122
About the Authors
Garima Agarwal, MDS
Postgraduate Student
Department of Periodontics
Bapuji Dental College and Hospital
Davangere
Karnataka State, India
Raison Thomas, MDS
Reader
Department of Periodontics
Bapuji Dental College and Hospital
Davangere
Karnataka State, India
Dhoom S. Mehta, MDS
Professor and Head
Department of Periodontics
Bapuji Dental College and Hospital
Davangere
Karnataka State, India