You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Several techniques have been used to modify the width of a deficient alveolar ridge. These techniques range from guided bone regeneration (GBR), to block bone grafting, to distraction osteogenesis, to ridge splitting. Expansion of the deficient alveolar ridge by ridge-splitting was described early by Scipioni et al1 and has been performed with various expansion methods.2-18 The indication for treatment using a ridge expansion procedure includes an edentulous span with minimal loss of vertical bone height accompanied by an inadequate alveolar thickness (2 mm to 4 mm) in the buccopalatal dimension. The technique described by Scipioni et all has traditionally involved a partial-thickness flap, crestal and vertical intraosseous incisions into the ridge, and buccal displacement of the buccal cortical plate and, very rarely, the lingual/palatal plate. The implant is placed and covered until osseointegration has occurred.1
It is the authors' list belief that the original technique has limitations in ensuring the long-term predictability of implant placement. These limitations include: limited visibility of both buccal and palatal alveolar bone plates; an increased risk of buccal plate fracture at the time of ridge expansion due to the presence of vertical bone incisions; and the preclusion of performing a GBR procedure in conjunction with implant placement to prevent loss of and maintain buccal hard-tissue volume during the healing phase. A modified expansion technique has been developed to maximize the predictability of bone augmentation with simultaneous implant placement. As with any surgical procedure, case selection is crucial. Criteria for case selection for this procedure include:
- an edentulous span in the anterior maxilla
- at least 2 mm to 4 mm of alveolar ridge width so there is adequate trabecular bone between the buccal and palatal cortical plates to allow for ridge expansion
- the presence of adequate vertical height for implant placement
- adequate keratinized tissue and vestibular depth to allow for passive soft-tissue coverage of the implant site
Description of Technique
Three major differences between the original technique developed by Scipioni et al1 and the modified technique presented in this article are listed in Table 1. One component of the modified splitting technique is elevation of a full-thickness flap. Examination of the residual buccal plate of bone throughout the procedure will help the clinician identify the magnitude of the buccal concavity, any fractures that may occur during expansion, or implant exposure that may occur during implant placement. A full-thickness flap also enables the surgeon to identify the contour of the palatal plate to ensure proper implant positioning. Changes in the alveolar ridge as a result of healing following tooth extraction can lead to the presence of a buccal concavity or an undercut that is not easily detectable with a partial-thickness view. Full visibility with a full-thickness flap allows the surgeon to visualize the hard-tissue topography so that the osteotomy position and angulation can be modified to avoid perforating through any undercut. Furthermore, full-thickness flap reflection provides access to the deficient ridge for additional bone regeneration procedures at the time of implant placement.
There are times when following displacement of the buccal cortical plate and implant placement that a bony dehiscence or fenestration may be present. The presence of such a defect, however, might not be visualized when using a partial-thickness flap. In order to ensure that adequate bone volume is present around the buccal implant surface, a GBR procedure is indicated. A partial-thickness flap precludes the possibility of performing GBR due to the presence of residual periosteum covering the bony surface. A full-thickness flap enables the surgeon to place bone graft material and a resorbable membrane in conjunction with implant placement. This allows for more predictable healing and osseointegration of the implant when bony deficiencies are present.
A second modification of the original splitting technique is the elimination of vertical intraosseous-releasing incisions. A major problem often encountered with vertical intraosseous incisions is the complete fracture of the buccal plate instead of a greenstick fracture as intended. The vertical bone-releasing incisions weaken the buccal plate and may increase the risk of perforation of the apical part of the vestibular cortex during implant placement.9 The elimination of bone incisions also provides better implant stability, which is achieved by the expanded yet intact buccal plate in the maxillary edentulous ridge. If a fracture of the alveolar plate is present, the buccal plate will be more likely to remain intact with the elimination of the bone incisions. Additionally, any fracture that is present can be easily detected, and a GBR with the use of a barrier membrane can be performed to prevent the ingrowth of soft tissue into these sites.
The final modification to the surgical protocol is the addition of bone augmentation.Concerns over buccal bone resorption surrounding implants are especially relevant in cases of ridge expansion, where a very thin alveolar ridge is present in the first place. When an already thin buccal plate composed of mostly cortical bone is displaced buccally, it may not heal favorably compared to the buccal plate with both cortical and cancellous bone. Additional bone grafting at the site can compensate for the amount of resorption that may occur following implantation. The grafts can be protected with a resorbable barrier membrane, autogenous connective tissue graft, or an acellular dermal matrix, depending on the presence of a dehiscence or fenestration after implant placement into the expanded ridge. If a dehiscence or fenestration is present, the use of a barrier membrane is recommended to prohibit soft-tissue growth from reaching the implant surface and augmented site.
Case Report of Modified Surgical Technique
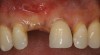
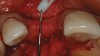
A 45-year-old woman presented with a narrow edentulous ridge in the maxilla (Figure 1). Following adequate anesthesia, a horizontal incision palatal to the crest and two vertical incisions were placed to outline the surgical field. A periodontal probe was used to measure the width of the alveolar crest at the most coronal dimension after a full-thickness flap was elevated (Figure 2). From the author’s experience, it was not necessary to maintain palatal bone-periosteum.
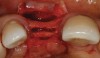
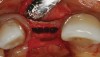
A long diamond bur was used to make a cut, which was 6-mm to 8-mm deep in the center of the alveolar ridge (Figure 3). The cut was made at least 1 mm away from the adjacent teeth in order to prevent any damage to them. A 4-mm wide bone-spreading chisel was used to mobilize and displace the buccal plate facially (Figure 4) so that a small, tapered osteotome for expansion could be used for implant site preparations. A 2-mm round bur was used to mark the implant location, and a 2-mm twist drill was used to guide the expansion with osteotomes.
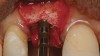
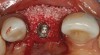
Tapered osteotomes were used to expand the ridge completely to the working length, which was at least 10 mm (Figure 5). It should be noted that if too much resistance is encountered, a drill smaller in diameter than a previously used osteotome can be used along the palatal wall. An implant was then placed into the osteotomy created by tapered osteotomes (Figure 6). Minor cracks were found in the middle of the expanded buccal plate during and after implant placement. Particulate bone allograft (freeze-dried bone allograft) was used to fill the gap between buccal and palatal alveolar plates, and another bone graft (bovine bone mineral) was packed outside the expanded buccal plate. A resorbable membrane was placed over the buccal plate and bone grafts (Figure 7 and Figure 8).
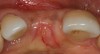
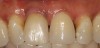
Following bone grafting and adaptation of the barrier membrane, the overlying flap was coronally positioned to achieve primary closure of the split alveolar ridge. After 4 months of healing, the site presented with ideal hard- and soft-tissue profiles (Figure 9). The implant was uncovered and a taller healing abutment was placed. A single crown was delivered (Figure 10), and the patient was restored to form and function.
This modified ridge-splitting technique enabled the placement of an implant with proper positioning and allowed for maintenance of hard- and soft-tissue volume. The patient was very satisfied with the final esthetic results of the procedure.
Conclusions
A case study was presented to describe modifications to the original maxillary ridge expansion technique. Based on their experience, the authorlist believe that this modified maxillary ridge expansion technique offers the following advantages over the original technique:
- Better access and flap mobility: Clinicians are able to examine both buccal and palatal bone contours for more accurate implant placement and identification of any buccal plate fractures or dehiscences.
- Lower risk of complete bone fracture: By eliminating vertical intraosseous incisions, there is a decreased likelihood of complete fracture of the buccal plate.
- Improved implant stability: Because the osteotomy for implant placement is prepared by expansion with the use of an osteotome, the buccal plate remains intact, which allows for increased primary implant stability.
- Better maintenance of soft- and hard-tissue volume: Simultaneous bone grafting and membrane placement can compensate for any buccal bone resorption during the healing process and allow for the maintenance of ideal hard- and soft-tissue profiles.
References
1. Scipioni A, Bruschi GB, Calesini G. The edentulous ridge expansion technique: a five-year study. Int J Periodontics Restorative Dent. 1994;14(5):451-459.
2. Basa S, Varol A, Turker N. Alternative bone expansion technique for immediate placement of implants in the edentulous posterior mandibular ridge: a clinical report. Int J Oral Maxillofac Implants. 2004;19(4):554-558.
3. Bravi F, Bruschi GB, Ferrini F. A 10-year multicenter retrospective clinical study of 1715 implants placed with the edentulous ridge expansion technique. Int J Periodontics Restorative Dent. 2007;27(6):557-565.
4. Calesini G, Micarelli C, Coppe S, Scipioni A. Edentulous site enhancement: a regenerative approach to the management of edentulous areas. Part 2: Peri-implant tissues. Int J Periodontics Restorative Dent. 2009;29(1):49-57.
5. Coatoam GW, Mariotti A. The segmental ridge-split procedure. J Periodontol. 2003;74(5):757-770.
6. Duncan JM, Westwood M. Ridge widening for the thin maxilla: A clinical report. Int J Oral Maxillofac Implants. 1997;12(2):224-227.
7. Elian N, Jalbout Z, Ehrlich B, et al. A two-stage full-arch ridge expansion technique: review of the literature and clinical guidelines. Implant Dent. 2008;17(1):16-23.
8. Engelke WD, Diederichs CG, Jacobs HG, Deckwer I. Alveolar reconstruction with splitting osteotomy and microfixation of implants. Int J Oral Maxillofac Implants. 1997;12(3):310-318.
9. Ferrigno N, Laureti M. Surgical advantages with ITI TE implants placement in conjunction with split crest technique. 18-month results of an ongoing prospective study. Clin Oral Implants Res. 2005;16(2):147-155.
10. Jensen OT, Cullum DR, Baer D. Marginal bone stability using 3 different flap approaches for alveolar split expansion for dental implants—a 1-year clinical study. J Oral Maxillofac Surg. 2009;67(9):1921-1930.
11. Koo S, Dibart S, Weber HP. Ridge-splitting technique with simultaneous implant placement. Compend Contin Educ Dent. 2008;29(2):106-110.
12. Lai YL, Chou IC, Liaw YC, et al. Triple immediate therapy (ridge expansion, soft tissue augmentation, and provisional restoration) of maxillary anterior single implant. J Periodontol. 2007;78(7):1348-1353.
13. Lee EA, Anitua E. Atraumatic ridge expansion and implant site preparation with motorized bone expanders. Pract Proced Aesthet Dent. 2006;18(1):17-22.
14. Park JB. Ridge expansion with acellular dermal matrix and deproteinized bovine bone: a case report. Implant Dent. 2007;16(3):246-251.
15. Piccinini M. Mandibular bone expansion technique in conjunction with root form implants: a case report. J Oral Maxillofac Surg. 2009;67(9):1931-1936.
16. Sethi A, Kaus T. Maxillary ridge expansion with simultaneous implant placement: 5-year results of an ongoing clinical study. Int J Oral Maxillofac Implants. 2000;15(4):491-499.
17. Summers RB. The osteotome technique: Part 2—The ridge expansion osteotomy (REO) procedure. Compend Contin Educ Dent. 1994;15(4):422-426.
18. Vercellotti T. Piezoelectric surgery in implantology: a case report—a new piezoelectric ridge expansion technique. Int J Periodontics Restorative Dent. 2000;20(4):358-365.
About the Authors
Taeheon Kang, DDS, MS
Assistant Professor
Department of Periodontology
Nova Southeastern University
Davie, Florida
Matthew J. Fien, DDS
Periodontist
Private Practice
Pembroke Pines, Florida
Daniel Gober, DDS
Department of Periodontology
Nova Southeastern University
Davie, Florida
Christopher J. Drennen, DMD
Periodontist
Private Practice
Davie, Florida