You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Tooth wear is commonly found in every dentition and may have physiologic or pathologic causes.1-3 Pathological tooth wear is becoming more evident today, with an aging population who is retaining their natural teeth for significantly longer.2,4
When tooth wear occurs as a natural physiological process, the average wear rates on occlusal contact areas were estimated to be 29 µm per year for molars and 15 µm per year for premolars.5 Tooth wear is considered excessive or pathologic when the normal rate of wear is accelerated by endogenous or exogenous factors2 and the degree of wear exceeds the level expected at any particular age.1,6 Tooth wear caused by parafunction is estimated to progress 3 times faster than physiological wear.2 Tooth surface loss (TSL) has been classified as the following types: (1) erosion: loss of tooth surface by chemical processes not involving bacterial action; (2) attrition: tooth structure loss by wear of tooth or restoration surface caused by tooth-to-tooth contact during functional or parafunctional activity of the teeth; and (3) abrasion: loss of tooth surface caused by the frictional action of a foreign substance on the teeth (other than tooth-to-tooth contact), such as that caused by toothbrushing. Another classification divides tooth wear into two categories: mechanical wear caused by attrition or abrasion, and chemical wear caused by erosion.1,2,7
A differential diagnosis is not always possible because in many situations there is an occurring combination of these processes1,2 although one is likely to predominate.8 Patients often seek help for problems of pain, altered function, and compromised appearance.8 Etiologic factors include bruxism, harmful oral habits, diet with excessive intake of citrus fruits or beverages with a low pH, eating disorders, gastroesophageal reflux disease, environmental and salivary factors as in xerostomic patients, and congenital anomalies such as amelogenesis imperfecta and dentinogenesis imperfecta.1-3
Several changes take place in the relationship of the teeth as they wear: Flat occlusal contacts create lack of stability, reduced clinical crown height, and the exposure of large areas of dentin that may limit the use of conservative adhesive techniques.9 This creates many difficulties for the restorative dentist, who may have to compromise the form of the restorations, their occlusal relationships, and the stability of the occlusion. Adequate retention and resistance forms for fixed prostheses are also difficult.6,9,10
In situations where tooth tissue loss has occurred and the occlusal vertical dimension (OVD) is still acceptable without the need be increased (compensated tooth surface loss [TSL] by continuous tooth eruption and alveolar bone growth2), treatment options may include periodontal surgery to gain clinical crown length, orthodontic movement with limited intrusion, surgical repositioning of a segment of teeth with its supporting alveolar bone, and placement of crowns and fixed partial dentures (FPDs).1,2
In situations where tooth wear exceeds compensatory mechanisms (non-compensated TSL11), loss of OVD will occur.2 With non-compensated TSL, the collapse of the anterior lower facial height needs an increase in the vertical dimension to restore the subjects to their presumed original OVD before TSL took place.11 This will create the interocclusal space required to accommodate the restorative material. Because the tooth structure is already worn, avoiding further tooth reduction to create space is highly desirable.12
The space required can be obtained by an overall increase in OVD. This allows the opportunity to restore the teeth and to re-establish esthetic and occlusal stability.8,12 Determining the OVD can be achieved through several methods such as phonetics, interocclusal distance, swallowing, and esthetics.1,2 A correct determination of the OVD and an appropriate jaw relationship form the basis of treatment whether this employs fixed or removable prostheses.11
Long-term observations have confirmed that, for the majority of patients, moderate alterations to the OVD may be well-tolerated.1 It is commonly believed that changes of OVD should be conservative and that a carefully monitored trial period with an interim prosthesis is desirable.1 Transitional removable partial dentures (RPDs) at the desired OVD, acrylic splints, or provisional restorations are several techniques that can be used.13 Because treatments may be costly and time-consuming, it is preferable to use a prosthesis that does not permanently change the dentition during the assessment period.1,10 The obtained position can be used for the definitive rehabilitation, and the final treatment option is dependent on the condition of the patient's remaining teeth.
In situations where loss of OVD has occurred because of non-compensated TSL,11 the overlay removable partial denture (ORPD) may be a definitive treatment option.2 This treatment consists of a prosthesis that covers and is partially supported by natural teeth, tooth roots, or dental implants and is an effective method of treating a patient with severely worn dentition.14,15 This treatment option has been suggested to be reversible and cost-effective for patients with congenital or acquired anomalies, with the final outcome pleasing to the patient.2,14 The following case report describes the use of maxillary ORPDs consisting of a chrome-cobalt (Cr-Co) framework with anterior acrylic resin veneers, posterior cast overlays, and acrylic resin denture bases in the treatment of a patient with severe tooth wear caused by attrition and erosion.
Case Report
A 51-year-old man was referred for prosthodontic and occlusal rehabilitation to the postgraduate clinic of the Faculty of Dental Medicine at the University of Coimbra, Portugal. His chief complaint was chewing difficulty and poor esthetics ("small teeth"). His medical and dental histories were recorded, and a complete series of radiographs were made. There was no medical or dental history that contraindicated dental treatment.
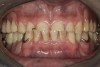
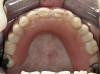
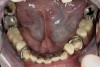
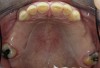
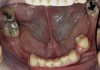
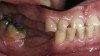
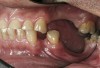
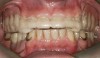
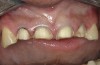
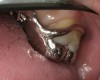
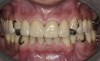
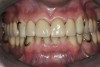
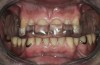
Initial examination revealed a partial edentulous patient with extensive wear of the maxillary anterior teeth and moderate wear in the mandibular teeth (Figure 1, Figure 2, Figure 3 , Figure 4, Figure 5, Figure 6 and Figure 7). The patient's maxillary and mandibular RPDs also showed excessive wear and multiple signs of fractures (Figure 2 and Figure 3). The patient had been wearing a mandibular nightguard for 8 years.
An extensive evaluation was performed that included intraoral and extraoral examinations of the teeth and supporting structures and an examination of the existing prostheses.10 Palpation of the temporomandibular joints and muscles of mastication revealed no evidence of joint sounds and/or tenderness. The mandibular range of motion was within normal limits.
A history of bruxing and consumption of acidic and carbonated drinks were reported. The clinical examination revealed severe tooth wear extending to the cervical level of the palatal surfaces of the maxillary teeth in some areas. Therefore, TSL was diagnosed as being caused by a combination of attrition and erosion.
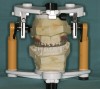
Clinical determination of the OVD was achieved using several methods such as facial measurements and esthetics.10 This distance varies between persons in a range of 2 mm to 4 mm. Phonetics were used to also determine the optimal position of the maxillary central incisor edges, with the incisors lightly touching the junction of the wet and dry border of the lower lip during pronunciation of fricative sounds. Patient preferences and facial appearance were also evaluated. After careful assessment, an interocclusal space of 7 mm was determined. The increase needed in the actual OVD was 4 mm, thereby leaving 3 mm of interocclusal space. Investigation of the patient's maxillo–mandibular relationship revealed an edge-to-edge tooth relationship in intercuspation position (ICP). A functional convenience position had been assumed. Preliminary impressions were made. The diagnostic casts were mounted on a semi-adjustable articulator using an interocclusal relation record with a bite registration material at the presumed final OVD and an average mounting technique.
During the following visit, several treatment options ranging from composite resin restorations to endodontic therapy to fixed restorations were discussed with the patient. After considering the options as well as the life expectancy of FPDs, the amount of time necessary, and patient's financial constraints, the patient elected to have ORPDs.
The design of the final maxillary overlay Cr-Co framework included metal occlusal surfaces on the anterior teeth and left second maxillary molar, a telescopic crown on the right maxillary third molar, circumferential clasps on the canines and left second molar, and a palatal strap as a major connector. Metal occlusal surfaces on the incisive teeth were provided with retention beads for an acrylic resin veneer material in the facial aspect of the incisors, and the tip of the canines were restored with composite resin to avoid further tooth surface preparation and to maintain maximum proprioception.
The prosthetic treatment began with diagnostic wax patterns of the maxillary teeth to restore the OVD and the plane of occlusion (Figure 8, Figure 9 and Figure 10). The proportions of the maxillary anterior teeth were corrected based on anatomic landmarks and averaged values. In addition, the diagnostic wax patterns corrected the maxillary–mandibular relation from edge-to-edge to Class I relationship in order to achieve a stable rehabilitation position.
The diagnostic cast of the wax patterns was duplicated using irreversible hydrocolloid and then poured in dental stone, and 1-mm thick thermal-vacuumed forming material was formed over the cast.
The upper acrylic partial denture of the patient was then modified using the vacuum-formed template as follows: The occlusal surfaces of the patient's teeth were lubricated with Vaseline. Retentive grooves were created on the interim prosthesis, which was then filled with autopolymerizing acrylic resin and inserted into the mouth. After polymerization, the template and prosthesis were removed, the excess bulk of the acrylic was trimmed, and the prosthesis was polished. After insertion, the occlusion was adjusted for canine guidance. This allowed for assessment of the patient's tolerance and acceptance of the restored OVD, testing of the occlusion, and evaluation of phonetics and esthetics before making the definitive prosthesis.
The interim prosthesis was designed to offer bilateral and simultaneous contact of all posterior teeth and a slight contact of the anterior teeth in centric occlusion, incisal guidance in protrusive movement, and canine guidance in laterotrusive movements. The interim prosthesis was delivered to the patient and was worn for approximately 7 weeks, during which occlusal adjustments were made and occlusion was modified on the basis of phonetic and esthetic principles, as well as patient comfort and ease of function. The patient was also evaluated for excessive signs of wear on the prosthesis, symptoms of temporomandibular dysfunction, and muscle tenderness. The prosthesis was well-tolerated and maintained by the patient with no adverse effect on phonetics, and no repairs were necessary.
After 2 weeks using the interim prosthesis, a periodontal examination revealed the presence of gingival marginal inflammation on the palatal aspect of the anterior teeth. Small composite resin restorations were then made to create a supragingival margin and the necessary relief on the interim prosthesis. After 1 week, the examination revealed only a smaller gingival marginal inflammation, with no patient discomfort.
The absence of pain in the masticatory muscles and the improvement in mastication, speech, and facial esthetics confirmed the patient's tolerance to the new mandibular interim prosthesis. The interocclusal space was determined to be 4 mm at the end of the assessment period. On the basis of these observations it was decided to undertake the definitive oral rehabilitation at the newly established OVD using the interim prosthesis as a guide.
Facial reduction of enamel surface on the maxillary incisive was required to accommodate the acrylic resin veneers, which would be bonded to the ORPD framework. Dentin exposure areas of the teeth were treated with dentin bonding agents and fluoride applications (Figure 11).
The interim prosthesis was relined with autopolymerizing acrylic resin. During a subsequent appointment, the process was repeated for the maxillary right third molar, which was prepared for a telescopic crown. On each of these appointments, the relining of the interim prosthesis maintained the established OVD. Rest preparations were not needed because the entire occlusal surface of the teeth served as rest seats under the cast framework. Only sharp edges of the abutment teeth were rounded and polished. After preparations were completed, final silicone impressions were made using standard trays customized with putty silicone and a wash impression with a low-viscosity silicone. They were poured in type IV dental stone to obtain a final cast. The mandibular impression picked up the existing RPD for correction of a clasp fracture and to replace the acrylic teeth that showed excessive wear and an inadequate curve of Spee.
Using an earbow record and the patient interim prosthesis as a centric occlusion record at the newly established OVD, the final casts were mounted on a semi-adjustable articulator. Condylar and side-shift angles were determined with the use of protrusive and lateral bite records. A customized anterior incisal guidance table was also established using autopolymerizing acrylic resin.
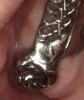
The casts were surveyed to determine the most suitable path of insertion for the definitive prosthesis. The posterior occlusal surfaces were waxed, and wax patterns were used for clasps and denture base connectors. Retentions were placed on the surfaces of the anterior portion of the framework to support acrylic veneers. The wax patterns were casted in a chrome-cobalt alloy (Figure 12).
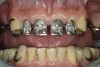
The framework was evaluated intraorally for fit, occlusion, retention, and stability (Figure 13, Figure 14 and Figure 15). With the framework in position, a new maxillo–mandibular relationship record was made with a silicone-based interocclusal record material, and the definitive casts were remounted on the articulator. The framework was returned to the laboratory, and acrylic resin veneers were applied in the esthetic zone and posterior artificial acrylic resin teeth were placed on the framework. The artificial teeth were arranged and tried in to verify esthetics and jaw relation records and to obtain the patient's approval before final processing. The junction between the maxillary natural teeth and the overlay prosthesis was not noticeable during normal speech and function.
The prosthesis was then processed with heat-polymerized acrylic resin. After deflasking procedures, the occlusion was adjusted and the prosthesis was finished and polished. At the next visit, the ORPDs were inserted with minor occlusal adjustments, and the canines were then restored with bonded composite resin (Figure 16 and Figure 17). Postoperative instructions on how to properly insert and clean the prosthesis were provided. These included oral hygiene, the application of sodium fluoride neutral mineral gel, and dietary counseling for caries and erosion prevention. The patient also was instructed to remove the dentures at night and to clean the ORPDs with a non-abrasive paste and soft-bristled brush. At night the patient was instructed to wear a maxillary nightguard (Figure 18). Four post-insertion visits (2 days, 1 week, 2 weeks, 4 weeks) were needed for minor prosthesis adjustments, and the patient was then placed on a 6-month continuous care schedule. During a 48-month follow-up period the only major problem was the fracture of the tip of the right canine, which was easily repaired with resin composite. Small marginal gingival inflammation on the maxillary incisors was also noticed and easily managed. No further wear was noticed on the mandibular teeth.
Discussion
The treatment used in this case is a relatively non-invasive, conservative, and cost-effective solution that allowed an esthetic and functional rehabilitation.1,16 This technique can be useful as an interim measure and allows for the possibility of more involved and complex procedures in the form of conventional crowns to be considered at a later time.12
Several disadvantages are associated with ORPDs such as complaints related to compromised esthetics when the dentures are removed,2 and oral comfort.16 Overlay treatment may be related to caries and progression of periodontal disease adjacent to the abutments even if preventive measures are introduced;16 however, these problems are mainly a result of poor oral hygiene.2 Veneer material fracture, debonding, discoloration, wear, and patient dissatisfaction with a removable prosthesis are also possible complications of ORPD therapy.2,14 To improve denture retention and patient comfort, the abutments may be provided with attachments or conical crowns if the patient is able to maintain satisfactory oral hygiene.16
Other risks of treatment with RPDs are mechanical failures such as fractures of major or minor connectors, as well as occlusal rests, deformation or fracture of retentive clasps, and inflammation of the underlying mucosa from traumatic irritation. Furthermore, the resorption of the residual ridge below the distal extension and wear of the denture teeth may result in a destabilization of the occlusion.16 Such risks could be minimized, to some extent, by a careful design of the framework with adequate dimensions and by using distal abutment or implants and instituting regular recalls to anticipate changes or problems.17
Caries secondary to the prosthesis insertion and periodontal problems are the main cause of loss of abutments.16 The wearing of a close-fitting denture can affect the progression of periodontal disease, accentuating the accumulation/formation of plaque and bacterial colonization (and increasing its pathogenicity).16 Overdenture abutment caries is rarely the reason for tooth extraction considering that it normally could be treated with conventional conservative techniques. The placement of copings with subgingivally located margins is also an additional caries preventive measure.18 In this specific case those copings were not used because of financial limitations, but the authors recognize their advantage in controlling caries and abutment wear.16 The preparation's margins were located just gingivally, and the palatal margin of the anterior tooth was restored with direct acid-etch retained composite resin to minimize gingival inflammation.12,16 When the loss of abutments is inevitable, the consequences are usually readily overcome by re-adaptation of the denture or replacement of the natural tooth by an implant.16
Periodontal health and a reduced risk of caries can be maintained by rigorous oral hygiene measures, daily application of a fluoride or chlorhexidine gel, and by removing the dentures overnight.17 Several authors have stressed that good patient cooperation and regular recalls are of major importance in reducing potential problems compared with the minor impact of the concept and design of the dentures.19 In a study performed by Ettinger et al20 the rate of subsequent periapical pathosis in overdenture abutments due to pulp necrosis or endodontic-associated problems was only 3.8%. The clinician should be aware of potential pulp micro-exposures when using vital teeth as abutments and should use a restorative material to seal the exposed tubules.20 In this clinical case, dentin exposure was managed with a thorough maintenance program that included patient and/or professional application fluoride mouth rinses and varnishes and the use of dentin bonding agents. An average interval between radiographs is typically 6 to 24 months, but they can be taken at any interval when they will aid either in monitoring or early diagnosis of periapical pathosis.
As in this case, when a patient exhibits parafunctional activity, it becomes increasingly important that there are enough opposing posterior teeth to provide stable ICP contacts so that the forces produced during parafunction are distributed over a wide area and in the teeth-long axis direction.6 An adequate anterior guidance will reduce the potentially harmful lateral forces produced by bruxing on interferences between posterior teeth. Canine guidance in lateral excursion and incisal guidance in protrusion discludes the posterior teeth as soon as the mandible moves from ICP and reduces the number of tooth contacts occurring outside ICP.21 There is some evidence that this alters the proprioceptive feedback to the central nervous system, which in turn reduces the level of activity in the masticatory muscles.22 Besides, in terms of laboratory and clinical prosthetic convenience, it is much easier to produce restorations in the presence of an adequately steep, immediate disclusion provided by a small number of teeth near the front of the mouth. When the lower dentition produces a satisfactory occlusal plane and stable ICP contacts there is no need for lower rehabilitation to complement the upper denture unless there are specific esthetic reasons.11
The etiology of parafunction is largely stress-related. It is likely that patients will continue to brux and clench after restoration of the worn teeth. Patients who are prone to nocturnal bruxism should wear occlusal guards at night. This may reduce their parafunctional activity and will prevent damage to teeth and new restorations. It is important to motivate patients to wear their nightguards by stressing the long-term consequences of failing to do so. This should be made clear to the patient before treatment begins.3,6
To prevent framework failures and distribute the occlusal forces, the dentures should be designed with rigid major and minor connectors, reciprocating clasp arms, and occlusal rests.
The choice of denture base material will depend on various factors including the opposing materials and whether coverage is mainly on hard or soft tissue. A well-supported and resistant denture is of primary importance. The definitive upper denture will benefit from a metal construction if the splint has shown signs of excessive wear resulting in breakage.11 The final prosthesis can be veneered over almost its entire occlusal surface with Cr-Co, which will strengthen the appliance and increase its longevity. Long-term wear resistance is essential because of the tremendous occlusal stresses that take place during normal mastication. However, when using Cr-Co, attention must be paid to the probability that the opposing arch may suffer accelerated wear.11 In this case, metal occlusal surfaces on the incisive teeth were provided with retention beads for a veneering material on the facial aspect. Although the esthetic zone in the ORPD can be fabricated either with composite or porcelain veneers, in this patient acrylic veneers were applied to the framework. There are several clinical cases described where acrylic or porcelain veneers were used.2,14,15
Porcelain veneers are more color-stable than acrylic;23,24 however, their low deformation at the yield point indicates that porcelain may be more suitable for rigid areas of a removable partial denture.25 Porcelain veneers are more expensive and more difficult to produce and repair than acrylic. Acrylic resin teeth veneers for RPDs have reasonably good esthetics, can be easily repaired, and are compatible with most dental alloys. In addition to relatively pleasing esthetics, an acrylic prosthesis is inexpensive, not time-consuming, and simple to produce. The retention of the resin to the metal is mainly mechanical. Acrylic resin teeth veneers are more sensitive to microleakage and are less color-stable than porcelain veneers.23,24 They also are less wear-resistant26 and eventually require repair or replacement. But with its high compressive load and yield strength, acrylic resin presents the physical properties that makes it the material of choice for veneering the more flexible areas of overlay dentures that may flex in function, as in the anterior area of a bruxing patient.25,26
In analyzing the literature, it can be concluded that the dental profession has seemingly not reached a consensus on the action needed in cases of tooth surface loss, but it agrees that a preventive regimen, as well as an early diagnosis of tooth surface loss, is preferable to restoration.
Removable prostheses may be the treatment of choice for some individuals, particularly when the time and cost of fixed restorations are considered. This clinical report demonstrated that the use of ORPDs can be a viable, relatively inexpensive, conservative, and non-invasive treatment choice for a patient with a severely worn dentition who expressed concerns over treatment longevity, invasiveness, cost, and long-term maintenance.
Every tooth replacement should be preceded by a careful evaluation of the existing dental and functional situation of the individual patient and the risks, benefits, and costs of any relevant prosthetic treatment. The conversion of existing prostheses into onlay provisional dentures has been presented. With this method of assessing a patient's tolerance to restoration of the occlusal vertical dimension, esthetics and function can be established and acceptability can be evaluated before permanent changes are made to the natural dentition. Any treatment option contemplated should be coupled with an overall preventive approach and a rigorous maintenance program. In well-controlled cases, biological failures through caries, periodontal disease, and endodontic problems will be rare and generally can be easily managed.
References
1. Sato S, Hotta TH, Pedrazzi V. Removable occlusal overlay splint in the management of tooth wear: a clinical report. J Prosthet Dent. 2000;83(4):392-395.
2. Ganddini MR, Al-Mardini M, Graser GN, Almog D. Maxillary and mandibular overlay removable partial dentures for the restoration of worn teeth. J Prosthet Dent. 2004;91(3):210-214.
3. Davies SJ, Gray RJ, Qualtrough AJ. Management of tooth surface loss. Br Dent J. 2002;192(1):11-6,19-23.
4. Shaw L, Smith AJ. Dental erosion—the problem and some practical solutions. Br Dent J. 1999;186(3):115-118.
5. Lambrechts P, Braem M, Vuylsteke-Wauters M, Vanherle G. Quantitative in vivo wear of human enamel. J Dent Res. 1989;68(12):1752-1754.
6. Capp NJ. Occlusion and splint therapy. Br Dent J. 1999;186(5):217-222.
7. Yip HK, Smales RJ, Kaidonis JA. Management of tooth tissue loss from erosion. Quintessence Int. 2002;33(7):516-520.
8. Ibbetson R. Tooth surface loss. 9. Treatment planning. Br Dent J. 1999;186(11):552-558.
9. Setchell DJ. Conventional crown and bridgework. Br Dent J. 1999;187(2):68-74.
10. Jahangiri L, Jang S. Onlay partial denture technique for assessment of adequate occlusal vertical dimension: a clinical report. J Prosthet Dent. 2002;87(1):1-4.
11. Faigenblum M. Removable prostheses. Br Dent J. 1999;186(6):273-276.
12. King PA. Adhesive techniques. Br Dent J. 1999;186(7):321-326.
13. Cura C, Saracoglu A, Ozturk B. Prosthetic rehabilitation of extremely worn dentitions: case reports. Quintessence Int. 2002;33(3):225-230.
14. Del Castillo R, Lamar F Jr, Ercoli C. Maxillary and mandibular overlay removable partial dentures for the treatment of posterior open-occlusal relationship: a clinical report. J Prosthet Dent. 2002;87(6):587-592.
15. Pavarina AC, Machado AL, Vergani CE, Giampaolo ET. Overlay removable partial dentures for a patient with ectodermal dysplasia: a clinical report. J Prosthet Dent. 2001;86(6):574-577.
16. Budtz-Jorgensen E. Restoration of the partially edentulous mouth—a comparison of overdentures, removable partial dentures, fixed partial dentures and implant treatment. J Dent. 1996;24(4):237-244.
17. Bergman B, Hugoson A, Olsson CO. Caries, periodontal and prosthetic findings in patients with removable partial dentures: a ten-year longitudinal study. J Prosthet Dent. 1982;48(5):506-514.
18. Molin M, Bergman B, Ericson A. A clinical evaluation of conical crown retained dentures. J Prosthet Dent. 1993;70(3):251-256.
19. Keltjens HM, Schaeken MJ, van der Hoeven JS, Hendriks JC. Effects of chlorhexidine gel on periodontal health of abutment teeth in patients with overdentures. Clin Oral Implants Res. 1991;2(2):71-74.
20. Ettinger RL, Krell K. Endodontic problems in an overdenture population. J Prosthet Dent. 1988;59(4):459-462.
21. McIntyre F. Restoring esthetics and anterior guidance in worn anterior teeth. A conservative multidisciplinary approach. J Am Dent Assoc. 2000;131(9):1279-1283.
22. Wiskott HW, Belser UC. A rationale for a simplified occlusal design in restorative dentistry: historical review and clinical guidelines. J Prosthet Dent. 1995;73(2):169-183.
23. Marei MK, el-Shimy A. Restoration of inadequate occlusal face height by using resin bonded to etched metal removable prosthesis. J Prosthet Dent. 1994;71(6):640-645.
24. Lakatos S, Rominu M, Negrutiu M, Florita Z. The microleakage between alloy and polymeric materials in veneer crowns. Quintessence Int. 2003;34(4):295-300.
25. Rominu M, Lakatos S, Florita Z, Negrutiu M. Investigation of microleakage at the interface between a Co-Cr based alloy and four polymeric veneering materials. J Prosthet Dent. 2002;87(6):620-624.
26. Kountouras CG, Howlett JA, Pearson GJ. Flexural and thermal cycling of resins for veneering removable overlay dentures. J Dent. 1999;27(5):367-372.
About the Authors
Júlio Fonseca, DMD
Assistant Professor
Department of Occlusion, Faculty of Dental Medicine
University of Coimbra
Coimbra, Portugal
Pedro Nicolau, DMD, PhD
Professor
Department of Prosthodontics, Faculty of Dental Medicine
University of Coimbra
Coimbra, Portugal
Tony Daher, DDS, MSEd
Associate Professor
Department of Restorative Dentistry, School of Dentistry
Loma Linda University
Loma Linda, California