You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Indirect ceramic restorations are frequently used to restore the function and esthetics of vital and non-vital teeth as well as dental implants. With recent advancements in CEREC (chairside economic reconstruction of esthetic ceramic) and its massive adoption, clinicians and dental assistants are now more involved in the manufacturing process of indirect ceramic restorations and need to understand the clinical indications for the various ceramic materials and their respective manufacturing, finishing, and cementation protocols.
This article discusses key points of the implementation and fabrication of chairside zirconia restorations and cementation protocols to elevate the clinical success rates with CEREC.
Ceramic Material Options
When a chairside computer-aided design/computer-aided manu facturing (CAD/CAM) workflow is intended, several options are available for the fabrication of indirect ceramic restorations, including resin matrix ceramics, silicate ceramics, and oxide ceramics. Each of these materials requires that specific parameters be followed with regard to tooth preparations, manufacturing of restorations, and cementation steps to enhance their clini cal longevity.
Resin Matrix Ceramics
Resin matrix ceramics have become quite popular because of the speed and simplicity of their fabrication process. This group of materials has great machinability and dimensional stability, providing excellent marginal adaptation, which is desired for any indirect restoration. Additionally, a simple manual polishing or light-curing stain/glaze protocol can facilitate the delivery of these restorations in one visit.
Most resin-based ceramic blocks are made under a high pressure/high-temperature process, which increases homogeneity but can reduce bond strength if the surface treatment is not followed according to the manufacturer's recommendations. Multi ple types of fillers are added to these resin blocks to improve their physical and esthetic properties, but the absence of a glassy matrix makes them non-etchable. Air-particle abrasion with 50-µm aluminum oxide particles is required to augment the surface roughness and area, which is desirable to achieve maximum mechanical retention and interlocking. The application of a silane coupling agent will promote chemical bonding, and when these two types of retention methods are present, the bond strength values increase significantly.1 (Please see Spitznagel et al1 for a detailed explanation of the effect of silane and air abrasion technique.)
Another type of resin matrix ceramic material is the hybrid ceramic or polymer-infiltrated ceramic network, having a porous ceramic structure (86%) infiltrated with a polymer (14%). This percentage of added polymer provides better milling properties compared with traditional ceramics and a modulus of elasticity in between human dentin and enamel. Hybrid ceramics are etchable and require 5% hydrofluoric acid etching for 60 seconds to achieve ideal surface roughness for optimized micromechanical retention.2 A silane application will promote chemical bonding, adding to their overall bond strength.
In general, resin matrix ceramics have a lower modulus of elasticity compared with traditional ceramics, making them an ideal option for intracoronal restorations, such as inlays.3
Silicate Ceramics
Silicate ceramics have been used since the beginning of the chairside CAD/CAM era as feldspathic ceramic blocks and have been continuously reformulated from leucite-reinforced ceramics to lithium disilicates and zirconia-reinforced silicate ceramics to improve their physical properties. All silicate ceramics are etchable materials, with etching times varying depending on their composition.
Feldspathic ceramics come in polychromatic blocks, making them a desirable option for laminate veneers or monolithic anterior crowns when the abutment tooth has a natural color. These ceramics require etching with of 5% hydrofluoric acid for 60 seconds to achieve ideal surface roughness and micromechanical retention. A silane coupling agent must always be used before the adhesive cementation process. For thin anterior feldspathic ceramic restorations, a light-curing resin cement system is indicated to facilitate the procedure, as its working time is longer compared with dual-curing resin cement systems.4
Leucite-reinforced ceramics also have a multichromatic distribution within the block, making them ideal for high-esthetic anterior restorations. These materials require etching with hydrofluoric acid for 60 seconds, followed by a silane coupling agent. Resin bonding is necessary for both feldspathic ceramics and leucite-reinforced ceramics, as it augments their flexural strength and long-term survival rates.
Lithium disilicate ceramics have become very popular for various indications, specifically monolithic crowns, onlays, and screw-retained implant crowns. Their high flexural strength makes them the strongest glass-ceramic material.5This material needs to be crystallized in a ceramic furnace after milling to obtain its final color and physical properties. A combination firing applying stain/glaze during the crystallization firing is recommended, as lithium disilicate is monochromatic. Lithium disilicate restorations achieve a strong bond to resin cements after 4% to 5% hydrofluoric acid etching for 20 seconds, followed by silanization of the etched surface.
Novel zirconia-reinforced lithium-silicate ceramics have been introduced in a fully crystallized version, which saves the time otherwise spent with the crystallization process (approximately 25 minutes) of traditional lithium disilicate. Finishing by manual polishing only or with a stain/glazing technique can be done with this newer ceramic material type, although published clinical success data are still limited.6 The internal surfaces of the restorations should be etched with hydrofluoric acid for 20 seconds, followed by silane application. Traditional cementation techniques are also possible with zirconia-reinforced lithium-silicate ceramics, but the overall strength is still higher when an adhesive cementation process is used.
Oxide Ceramics
Oxide ceramics, such as zirconium dioxide (zirconia), are characterized by excellent mechanical and biological properties, which are significantly superior to those of silica-based ceramics.7 Its inherent strength allows for less invasive crown prepar ations, thinner restorations, and conventional cementation. The latest zirconia generations offer significantly greater light transmission than previous generations. Pre-shaded multi-layer high-translucent zirconia materials offer a range of esthetic treatment options and can be used for tooth and implant-supported crowns, fixed dental prostheses, resin-bonded fixed prostheses, and bonded laminate veneers. The higher translucency is achieved by slight changes of the yttrium oxide content, resulting in a larger number of cubic-phase particles. More cubic zirconia offers significantly higher light transmission but lower flex ural strength values than conventional zirconia, between 550 MPa and 1,000 MPa.8
High-translucent zirconia blocks for CEREC have recently entered the marketplace. The restorations are milled from pre sintered blocks with slightly enlarged dimensions, compensating for the 20% to 25% material shrinkage that occurs during the final sintering step after milling. This causes less over-milling in the intaglio surface and allows for an exceptional marginal adaptation. With a special chairside furnace and a speed sintering program, the sintering of a single crown can be accomplished within 20 minutes.2
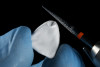
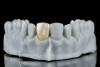
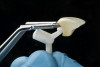
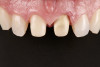
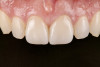
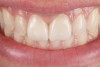
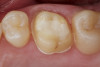
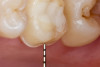
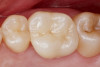
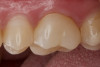
Figure 1 through Figure 14 illustrate steps involved in the fabrication of zirconia restorations using CEREC. Figure 15 through Figure 21 show preparations and postoperative results in two case examples of patients who received zirconia indirect restorations.
Given the broad popularity of zirconia restorations, clinical application and cementation protocols are widely debated. In general, these restorations are typically considered cementable because of their high inherent flexural strength, which exceeds natural chewing forces. Therefore, zirconia-based crowns and bridges with adequate retention and ceramic material thickness can be cemented conventionally. However, translucent zirconia restorations that are less strong, thin, lack retention, or rely on resin bonding, such as resin-bonded fixed prostheses or bonded laminate veneers, require resin bonding with composite resin luting agents.
To achieve high and long-term durable resin bond strengths to zirconia in a practical manner, the APC concept, a three-step approach, is recommended: (1) air-particle abrade the bonding surface with aluminum oxide (A); (2) apply special zirconia primer (P); (3) use dual-cure or self-cure composite resin cement (C).8
After try-in and ultrasonic cleaning with alcohol, zirconia should be air-particle abraded with alumina or silica-coated alumina particles. Small particles (30-50 microns) at a low pressure (<200 kPa [2 bar]) are sufficient. The subsequent step includes application of a special ceramic, which contains special adhesive phosphate monomers. The monomer MDP (10-methacryloyloxydecyl dihydrogen phosphate) has been shown to be particularly effective to bond to metal oxides. Dual-cure or self-cure composite resins should be used to ensure adequate polymerization. The APC concept is also indicated when adhesive cementation to prefabricated titanium abutments (ti-bases) is needed. If custom titanium abutments with retention and resistance form are preferred, conventional cementation of monolithic zirconia restorations with resin modified glass-ionomer or self-adhesive resin cements is suggested.
Conclusion
Understanding ceramic material properties, clinical indications, manufacturing steps, and specific surface treatment protocols will lead practitioners to higher clinical success rates with indirect zirconia restorations. Current adhesive protocols and the ongoing development of ceramic materials for fabrication of indirect restorations provide a promising future for minimally invasive restorative dentistry.
Acknowledgments
Special thanks to Markus B. Blatz, DMD, PhD, and Francisco Rojas, DDS, for their contributions to this project, and to the Kuraray Noritake team for the support provided.
References
1. Spitznagel FA, Horvath SD, Guess PC, Blatz MB. Resin bond to indirect composite and new ceramic/polymer materials: a review of the literature. J Esthet Restor Dent.2014;26(6):382-393.
2. Conejo J, Ozer F, Mante F, et al. Effect of surface treatment and cleaning on the bond strength to polymer-infiltrated ceramic network CAD-CAM material. J Prosthet Dent. 2021;126(5):698-702.
3. de Castro EF, Azevedo VLB, Nima G, et al. Adhesion, mechanical properties, and microstructure of resin-matrix CAD-CAM ceramics. J Adhes Dent. 2020;22(4):421-431.
4. Otto T, Mormann WH. Clinical performance of chairside CAD/CAM feldspathic ceramic posterior shoulder crowns and endocrowns up to 12 years. Int J Comput Dent. 2015;18(2):147-161.
5. Blatz MB, Conejo J. The current state of chairside digital dentistry and materials. Dent Clin North Am. 2019;63(2):175-197.
6. Demirel M, Diken Türksayar AA, Donmez MB. Translucency, color stability, and biaxial flexural strength of advanced lithium disilicate ceramic after coffee thermocycling. J Esthet Restor Dent. 2022. doi: 10.1111/jerd.12960.
7. Blatz MB, Vonderheide M, Conejo J. The effect of resin bonding on long-term success of high-strength ceramics. J Dent Res. 2018;97(2):132-139.
8. Blatz MB, Conejo J. Cementation and bonding of zirconia restorations. Compend Contin Educ Dent. 2018;39(suppl 4):9-13.