You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
In restorative dentistry today, clinicians have a wide variety of cementation options from which to choose. Because a universal cement has not yet been developed that can be used in all clinical situations, proper cement selection is essential for successful restorative treatments and long-term bonding results. Cementation of a dental restoration is a multifactorial challenge, and appropriate selection of cement requires a careful evaluation of the restoration type and preparation, the retention and resistance form of the restoration, the tooth structure being bonded to the restoration (eg, dentin, enamel, or both), and the isolation challenges that the individual case presents. The clinician also needs to have a solid understanding of the cement's composition, bonding mechanisms, and potential interactions with the other restorative materials that are being used. With materials rapidly evolving, the choice of dental cements has become increasingly complex, making it absolutely necessary that practitioners keep up to date on the latest developments in cementation. This article will review the criteria for cement selection for restorations and examine the advantages and disadvantages of the various cement materials. The protocols to be followed for the various bonding agents will also be described.
CEMENTATION MATERIALS
The major categories of cements currently available are glass ionomer and resin-modified glass ionomer (RMGI) cements, resin cements, and bioactive cements. Glass ionomer cements, which can be classified as restorative or luting cements, have been in use since the early 1970s,1 while RMGI cements were developed in the 1990s; both cements remain popular and are a good choice for certain clinical situations. Bioactive cements, a relatively new entry to the marketplace, can be challenging to use, but are useful in some scenarios and as a category will continue to evolve over time. The use of bioactive cements is increasing because of the ability of these materials to foster an ionic exchange that leads to the formation of an apatite layer.2 Resin cements, both dual-cured and light-cured, have numerous clinical indications and are highly popular. Self-etch self-adhesive resins are a new and growing category, developed to facilitate the luting process and rapid bonding.
Adjunctive materials needed for the cementation process include metal primers, cleaning agents, and soft-tissue control armamentaria.
ESTHETICS
Esthetics is one of the primary considerations in cement selection, as the shade of the luting agent may alter the final coloration of the restoration. Gold and porcelain-fused-to-metal (PFM) restorations will not be affected by the shade of the cement.
Because of their opacity, zirconia materials are less likely to
undergo shade alteration that can be caused by the cementation material,3-6whereas the shading of restorations made of lithium disilicate and feldspathic porcelain, which are more translucent materials, can be affected by the shade of the cement.7 Self-etch and bioactive cements are often opaque in color and may alter the shade of a ceramic restoration.
RETENTION AND RESISTANCE FORM
The retention and resistance form of a restoration is one of the most important factors in cementation selection. Depending on the retention and resistance form, which is primarily based on the length and angulation of the axial walls and axial surface area,8 the clinician may have several cement options or, conversely, only a few choices. For example, if a crown preparation has long walls and angulation that is less tapered (Figure 1), there often is much resistance when seating the crown. With this ideal retention and resistance form, there are often many cements that can be used. However, when there is compromised retention and resistance form-for example, with a short preparation with tapered walls-judicious cement selection and choice of technique are critical for the long-term stability of the restoration.
CEMENTATION SELECTION AND PROTOCOLS BASED ON RESTORATIVE MATERIAL
Gold and PFM
For gold or PFM restorations with good retention and resistance form, essentially any cement can be used. With poor or compromised retention and resistance form, however, a dual-cure resin cement should be chosen, because it has the highest strength of bond to tooth structure and will increase the retention to prevent the restoration from becoming dislodged over time. For slightly better (but not excellent) retention and resistance form, a self-etch resin can be a good option.
For gold or PFM restorations with good retention and resistance
form, glass ionomer and RMGI cements are particularly useful
for patients with recurrent decay or at high risk for caries,
because of their fluoride-releasing properties,9 which help protect the tooth from decay at the margin, and they provide ease of cleanup and removal. These cements are also a good choice for cases in which there are subgingival margins and tissue is irri-
tated,10 where the clinician may be faced with challenges controlling the bleeding and fluid release in the sulcus; because these cements allow for quick seating of the restoration, bleeding needs to be controlled for only a few seconds.
As already mentioned, cement shade cannot affect the coloration of gold or PFM restorations.
A crucial step in the cementation process for gold and PFM restorations is cleaning and priming of the internal aspect of the restoration, which help ensure reliable bonding. During try-in, the restoration will become contaminated; therefore, before seating a gold or PFM restoration, the clinician should use a cleaning agent designed for nonabrasive cleansing of the bonding surfaces. Air abrasion can be used in addition to the cleaning agent for additional cleansing. This step should be followed by the use of a metal priming agent, which will significantly increase the bond strength of the cement to the restoration. Metal priming adds very little time to the procedure (about 60 seconds), and because it so greatly enhances the bonding, clinicians should always include it in the cementation process.
Zirconia
Although PFM has traditionally been considered the "gold standard" for dental prostheses, this material has several limitations, including inferior esthetics compared with materials such as zirconia.11,12 Zirconia, which is becoming the most popular restorative material for the placement of crowns and bridges, can essentially be thought of as a white metal that "follows many of the same rules" as gold and PFM. Because zirconia is highly opaque, cement shade is less likely to affect the shade of this material.3-6
As is true with gold and PFM, if retention and resistance form are good, any cement can be used with zirconia. In the author's opinion, in cases with good retention and resistance form, and in which the tissue is well-controlled and the preparation can be well-isolated, self-etch resin cements are a good choice for zirconia restorations. These cements are quick and easy to use and allow simple cleanup, preclude irritating the tissue with phosphoric etching over time, and offer excellent bond strength. If the retention and resistance form is compromised, dual-cure or self-etch resin cements are indicated, with self-etch being the second-choice option. In cases where the clinician is having difficulty controlling hemorrhage around the preparation, a self-etch cement is the better choice because there is less time available to keep the prep area well-isolated. If dual-cure cements are used, maintaining good isolation over a greater period will be necessary.
Another consideration is whether the patient is caries prone. If the retention and resistance form is good but the patient has caries or is at high risk for caries, glass ionomer or RMGI cements are the better choice, owing to their fluoride-releasing properties.9 For cases in which dental sensitivity is an issue, bioactive cements have the potential to calm an irritated nerve or pulp.
As in the case of gold or PFM restorations, after try-in, a nonabrasive cleaning agent should be used to decontaminate the zirconia restoration,13 followed by priming with a metal priming agent. Air abrasion can be utilized for additional cleansing.
Lithium Disilicate and Feldspathic Porcelain
Lithium disilicate is a very strong material with high fracture toughness (Figure 2).14 Because of its translucency, which makes it an appropriate material for tooth-colored restorations, use of lithium disilicate requires judicious evaluation of cement shade, as this can affect the final coloration of the restoration.7
Resin cements are the most common cement of choice when lithium disilicate is used, and they are the first choice of the author when using this restorative material. When retention and resistance form is good, dual-cure cements are the best choice, in the author's opinion, with self-etch resin cements a close second; for restorations with compromised retention and resistance form, dual-
cure resins are the cement of choice. Proper placement proto-
col is required to maximize bond strength.
Veneers
Veneers (Figure 3) are typically made of feldspathic porcelain or lithium disilicate, with the latter generally preferred over the former in recent years. Cementation is the same for both materials. Because veneers do not have the retention and resistance form, as adherence is occurring between two essentially flat surfaces, bond strength among the cement, restoration, and tooth is absolutely critical, as is using a technique that will avoid contamination, which will affect the bond strength and long-term adhesion. Also, because they are thin restorations, veneers are typically highly translucent, so it must be kept in mind that cement shade will affect their esthetics.
Proper treatment of veneers after try-in and before cementation also is critical for attaining optimum bond strength. After try-in, some contamination has certainly taken place, and try-in paste that was used to evaluate the shade of the cement must also be cleaned up. In the past, veneers were cleaned at this stage with phosphoric acid etch, which for this purpose was used not to etch the porcelain but to take advantage of its detergent properties for decontamination. Another traditional method for decontaminating the veneers has been to clean them with isopropyl alcohol and place them in an ultrasonic cleaner for 90 seconds.15
Although these traditional methods are effective for decontamination, today better options are available for cleaning the inside of the veneers-namely, universal cleaning agents that can be used more quickly and easily, and which are designed for the nonabrasive cleaning of the bonding surfaces of zirconia, ceramic, lithium disilicate, and metal restorations to remove phosphate contamination after try-in (Figure 4). After the contamination has been removed, the internal aspect of the veneers can be resalinated and then air-dried. Metal primers are contraindicated with feldspathic porcelain and lithium disilicate.16,17 (It should be noted that, because recent improvements in the translucency and esthetics of zirconia crowns have made it increasingly difficult for the clinician to distinguish it visually from lithium disilicate, extra care should be taken to avoid mistaking lithium disilicate for zirconia, so that the metal primers contraindicated for lithium disilicate are not used in error.)
Either a dual-cure or light-cure resin cement should be used with lithium disilicate veneers, owing to their high bond strength. The author prefers the use of a light-cure resin cement due to the increased working time and because it eliminates any concerns of potential shade shift. A translucent light-cure resin cement is best for tooth shade esthetics, because it absorbs more light and thus allows the underlying tooth structure to more greatly influence the shade of the restoration.18,19 The author finds that a light-cure cement also is preferable when cementing multiple veneers at the same time because it provides for more working time than dual-cure resin cement, although other clinicians may be more comfortable using dual-cure cements. Self-etch, self-
adhesive resin cements are contraindicated for veneers, because
they do not provide sufficient bond strength for these restorations.20,21
As we have already emphasized, bond strength is critical for veneers. A total etch technique to prepare the tooth and veneer for bonding should therefore be employed, because most of the tooth preparation will be enamel and the bond strength of resin to etched enamel is the highest available.22 The teeth should be etched for 20 to 30 seconds. After the etch is rinsed off and lightly dried, apply a universal bonding agent (likewise for 30 seconds), then air-thin and light-cure the bonding agent (Figure 5).
The cementation protocol for veneers made of feldspathic porcelain is similar to that of veneers made of lithium disilicate.
Crowns
The cementation process for placing lithium disilicate crowns is, for the most part, similar to that for veneers. To remove decontaminants after try-in, the internal aspects of the preparation must be cleaned with either isopropyl alcohol and an ultrasonic cleaner, with phosphoric acid, or, preferably, with a universal cleaning agent. The internal aspect of the tooth should then be resalinated, because the salination process has the potential to enhance the bond strength of the cement to the crown.
Because lithium disilicate is an extremely strong material, there is a wide variety of cements that work well with lithium disilicate crowns. Dual-cure resin cements are used most commonly,23,24 and in cases with poor retention and resistance form, a dual-
cure resin cement is the optimal choice, because this cement type will provide the highest bond strength for both cement to the tooth and cement to the restoration.
In cases of ideal retention and resistance form, the author recommends dual-cure resin as the first-choice cement, although self-etch resin cement is another excellent option. If the patient is at high risk for caries, an RMGI cement can be considered for its benefits of fluoride release.9
Indirect Composite Blocks
As in-office milling becomes more popular, so do indirect composites, which can be milled in-office for crown-and-bridge restorations. A dual-cure resin cement is indicated with indirect composites, but a self-etch resin cement would also be suitable. At this time, glass ionomer and bioactive cements should likely be avoided, in the author's estimation, because not enough is known at present about how they interact with indirect composites.
With indirect composite blocks, microabrasion should be performed after the try-in. After cleaning out the inside of the restoration, the clinician should apply the adhesive and light cure, or use silane or a priming agent that enhances adhesion between the indirect restorative material and the resin cement.
The use of metal primers is another important consideration in the cementation of restorations made of these materials.
Soft Tissue Control
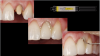
During the cementation of crowns, soft tissue control is important because the restorative field must be free of fluid for optimal bond strength to be achieved. If the patient has not taken good care of the temporary (eg, by not flossing or brushing sufficiently), the surrounding tissue will be irritated and likely to bleed, particularly in cases where subgingival margins are present. To maintain soft tissue control, a 25% aluminum chloride hemostatic agent should be used, which is kind to the tissue. This will stop minor bleeding in the esthetic zone, and because this agent is a transparent gel, it leaves no residue that will stain over time, and it rinses off with ease. Furthermore, it does not interfere with bond strength. Retraction paste (Figure 6) also works very well for soft tissue control. In the past, some cartridges would dry out and not extrude correctly, but modern retraction paste has better-designed unit-dose cartridges that have solved these problems. The color of the paste is vibrant so that the clinician can easily see whether all the paste has been removed. While some clinicians prefer using a retraction cord to control tissue before cementation, it is generally contraindicated because it is likely to further irritate the tissue. If bleeding will not stop despite the use of these methods, the clinician may use a diode laser to cauterize the tissue. Whatever method the clinician uses, controlling the hemorrhage when bonding is crucial, because to obtain the best bond strength for the cement there must be no blood contamination on the prepared tooth.
Finishing the Restoration
Tooth preparation is the last step before cementing temporary crowns and the first step when cleaning off temporary cement before trying in the final crown. The author recommends the use of a flour of pumice paste; instead of water, use a desensitizer containing 2-hydroxyethyl methacrylate (HEMA) and chlorhexidine; place a drop into the pumice and, using a prophy cup, clean the preparation to decontaminate it as much as possible. This also will increase bond strength and may help desensitize the tooth.25
For cemented implant crowns, the author believes that bioactive cements are the best choice, with glass ionomer cements being a good alternative, as they allow ease of cleanup. Resin cements should be avoided. To cement implant crowns or a bridge (Figure 7), the clinician should take an impression of the implant crown and create a chairside dye. The implant crown is then loaded with the cement, after which the dye is inserted into the crown. When the dye is removed, only a thin film of cement will remain on the inside of the crown, and the crown can then be seated. This will significantly reduce the amount of excess cement that seeps out at the margin and allow for quicker and easier cleanup. Excess cement around an implant is contraindicated, so the amount of cement extruded at the margin should be minimized.
Cements of the Future
Bioactives are an increasingly important category of cements because their growing use points to the direction in which restorative dentistry is evolving. Some cements not marketed as such may in fact be bioactive cements if they contain calcium ions. Self-etch, self-adhesive cements are another growing category, although their bond strength is not as high as that of dual- or light-cure resin cements. Self-etch, self-adhesive cements are good, but they cannot do everything-yet. The technology with these and other agents continues to progress.
Already available, a dual-cured, calcium- and fluoride-releasing, self-adhesive resin cement is indicated for luting crowns, bridges, inlays, onlays, and prefabricated metal/non-metal/fiber posts. Such a cement offers continuous calcium and fluoride release26 and transitions from acidic to alkaline pH in minutes.27In addition, it offers high physical strength, delivering a strong bond to zirconia and most substrates, with no priming or etching required (Figure 8).
Conclusion
Currently no single universal cement is available, but it is believed that in the near future one will be developed that will be self-etching in nature. In the meantime, judicious cement selection is a multifactorial challenge, requiring that the clinician evaluate each restoration type and material, preparation retention and resistance form, and isolation challenge on an individual case basis. For many restorations, the clinician has numerous viable cement options from which to choose, and therefore a solid understanding of the multiple factors involved in the cementation process is invaluable. Careful consideration of these factors-always in the context of the individual clinical situation-will guide the clinician in identifying at least one, if not two or more, good cement options, even in situations where there is no one "best" choice. For the most part, a great deal of subjectivity is involved in the selection of cement materials and the appropriate cementation protocol, such that good clinical judgment is ultimately the key to ensuring long-term treatment success and longevity of bonding in restorative dentistry.
About the Author
Gary Radz, DDS
Clinical Associate Professor, Restorative Dentistry
University of Colorado School of Dental Medicine
Aurora, Colorado
President, Snow Mountain Seminars
Board of Directors, Smile Source
Private Practice, Denver, Colorado
References
1. Wilson AD, Kent BE. A new translucent cement for dentistry: the glass ionomer cement. Br Dent J. 1972;132(4):133-135.
2. Corral Nuñez C, Covarrubias C, Fernandez E, Oliveira OB Jr. Enhanced bioactive properties of Biodentine™ modified with bioactive glass nanoparticles [published correction appears in J Appl Oral Sci. 2017;25(3):354]. J Appl Oral Sci. 2017;25(2):177-185.
3. Ayash G, Osman E, Segaan L, Rayyan M, Joukhadar C. Influence of resin cement shade on the color and translucency of zirconia crowns. J Clin Exp Dent. 2020;12(3)e257-e263.
4. Alraheam IA, Donovan TE, Rodgers B, Boushell L, Sulaiman TA. Effect of masticatory simulation on the translucency of different types of dental zirconia. J Prosthet Dent. 2019;122(4):404-409.
5. Ayash G, Osman E, Segaan L, Rayyan M, Joukhadar C. Influence of resin cement shade on the color and translucency of zirconia crowns. J Clin Exp Dent. 2020;12(3):e257-e263.
6. Bayindir F, Koseoglu M. The effect of restoration thickness and resin cement shade on the color and translucency of a high-translucency monolithic zirconia. J Prosthet Dent. 2020;123(1):
149-154.
7. Sakrana AA, Laith A, Elsherbini A, Elerian FA, Özcan M, Al-Zordk W. Influence of resin cement on color stability when luting lithium disilicate and zirconia restorations. Int J Esthet Dent. 2023;18(2):114-126.
8. Sharma A, Rahul GR, Poduval ST, Shetty K. Short clinical crowns (SCC) - treatment considerations and techniques. J Clin Exp Dent. 2012;4(4):e230-e236.
9. Sikka N, Brizuela M. Glass ionomer cement. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2023. Updated March 19, 2023. Accessed June 8, 2023.
10. Yoneda S, Morigami M, Sugizaki J, Yamada T. Short-term clinical evaluation of a resin-modified glass-ionomer luting cement. Quintessence Int.2005;36(1):49-53.
11. AlMashaan A, Aldakheel A. Survival of complete coverage tooth-retained fixed lithium disilicate prostheses: a systematic review. Medicina (Kaunas). 2022;59(1):95.
12. Ghodsi S, Arzani S, Shekarian M, Aghamohseni M. Cement selection criteria for full coverage restorations: a comprehensive review of literature. J Clin Exp Dent. 2021;13(11):e1154-e1161.
13. Sahin SC, Celik E. The effect of different cleaning agents and resin cement materials on the bond strength of contaminated zirconia. Microsc Res Tech. 2022;85(3):840-847.
14. Abdulrahman S, Von See Mahm C, Talabani R, Abdulateef D. Evaluation of the clinical success of four different types of lithium disilicate ceramic restorations: a retrospective study. BMC Oral Health. 2021;21(1):625.
15. Harouny R, Hardan L, Harouny E, et al. Adhesion of resin to lithium disilicate with different surface treatments before and after salivary contamination - an in-vitro study. Bioengineering (Basel). 2022;9(7):286.
16. Tian F, London J, Villalobos V. Effectiveness of different cleaning measures on the bonding of resin cement to saliva-contaminated or blood-contaminated zirconia. J Dent. 2022;210:104084.
17. Feiz A, Rastghalam N, Swift EJ Jr. Effect of different cleansing methods on the artificially aged bond strength of resin to contaminated zirconia: a systematic review. J Prosthodont. 2022;31(9):e125-e137.
18. Comba A, Paolone G, Baldi A, et al. Effects of substrate and cement shade on the translucency and color of CAD/CAM lithium-disilicate and zirconia ceramic materials. Polymers (Basel). 2022;14(9):1778.
19. Pechteewang S, Salimee P. Microhardness of resin cements after light activation through various translucencies of monolithic zirconia. J Adv Prosthodont. 2021;13(4):246-257.
20. Rodrigues RF, Ramos CM, Francisconi PAS, Borges AFS. The shear bond strength of self-adhesive resin cements to dentin and enamel: an in vitro study. J Prosthet Dent. 2015;113(3):220-227.
21. Duarte S Jr, Botta AC, Meire M, Sadan A. Microtensile bond strengths and scanning electron microscopic evaluation of self-adhesive and self-etch resin cements to intact and etched enamel. J Prosthet Dent.2008;100(3):203-210.
22. de Oliveira da Rosa WL, Piva E, da Silva AF. Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent. 2015;43(7):765-776.
23. Johnson GH, Lepe X, Patterson A, Schäfer O. Simplified cementation of lithium disilicate crowns: retention with various adhesive resin cement combinations. J Prosthet Dent. 2018;119(5):826-832.
24. Lepe X, Streiff KR, Johnson GH. Long-term retention of zirconia crowns cemented with current automixed cements. J Prosthet Dent. 2021;125(5):788-794.
25. Gawel R. Desensitizer's antimicrobial action increases bond strength. Dentistry Today.Available at https://www.dentistrytoday.com/products/desensitizer-s-antimicrobial-action-increases-bond-strength. Published February 26, 2019. Accessed June 12, 2023.
26. Gleave CM, Chen L, Suh BI. Calcium & fluoride recharge of resin cements. Dent Mater.2016;32(1):e26.
27. Chen I, Gleave C, Suh B. New self-adhesive resin cement with alkaline pH. Presented at the IADR/AADR/CADR General Session; March 22, 2017; San Francisco, CA. Abstract 286.