You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
For centuries, people have employed a variety of teeth whitening methods in the hopes of lightening the shade of their teeth. In 1989, tray bleaching entered the whitening market and spurred a tremendous increase in interest in teeth whitening among the public.1 As beauty standards of modern society favor an esthetically pleasing smile, this elevated desire for whiter teeth endures-and continues to grow. But the threat of tooth discoloration remains, and has many etiologies that can dim even the most luminous of smiles.
TYPES OF TOOTH DISCOLORATION
While teeth have natural variations and gradations in tooth color, there are two classifications of staining for which patients pursue treatment: intrinsic and extrinsic.1-3 Both types of tooth discoloration typically can be treated with whitening modalities, although the optimum whitening treatment to be used varies depending on the type of staining. Because some stains are more responsive to teeth bleaching than others, properly diagnosing the type of staining is key to determining an effective treatment plan.4-6
Intrinsic Stains
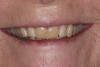
Intrinsic staining is deeper staining embedded within the dentin of the tooth.3,7 Causative factors of intrinsic staining include dental caries, enamel defects such as enamel microcracks, restorations, genetics, aging, trauma, medications, environment, or systemic conditions, as well as excessive fluoride ingestion, severe jaundice in infancy, and porphyria3,7 (Figure 1).
Intrinsic staining is most often the result of aging, as the pulp inside shrinks and dentin thickens, giving the teeth a yellow appearance.3,7 Intrinsic staining is inherently more difficult to treat than extrinsic staining and cannot be removed with prophylactic procedures.7,8
Extrinsic Stains
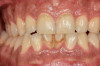
Extrinsic staining is discoloration that occurs on the outside of teeth, either on the surface enamel or in the acquired pellicle to which stain molecules attach (Figure 2).3,4 The result of hygiene, lifestyle, or dietary habits, extrinsic stains can be classified as ether metallic or non-metallic according to their origin, and can differ in appearance, composition, location, and severity.4 For example, brown staining can be caused by drinking coffee or tea as a result of the tannin that these beverages contain, coupled with insufficient teeth brushing.4 Brown staining is thin and translucent and can be found primarily on buccal surfaces of maxillary molars and lingual surfaces of mandibular incisors.5With yellowish-brown staining, chlor-
hexidine is retained in the oral cavity; this staining is located in the cervical and interproximal area of the teeth.4 Black stains are caused by coal tar combustion products due to smoking; by penetration of pits and fissures, enamel, and dentine by tobacco juices; and by iron-containing oral solutions.4
Non-metallic stains are absorbed onto tooth surface deposits, such as plaque or the acquired pellicle.4 Causes of non-metal-
lic staining include beverages, tobacco, mouth rinses, and other medicaments.4 Metallic stains are associated with occupational exposure to metallic salts as well as medicines containing metal salts.8 With metallic staining, metals are penetrated into tooth substances and produce permanent discoloration.4
WHITENING CHEMISTRY
Compounds in teeth stains called chromogens are the darker pigments targeted by the active ingredient of teeth whitening treatments.6 The active ingredient in most whitening products is hydrogen peroxide or hydrogen peroxide-releasing agents (carbamide peroxide).6,8 Carbamide peroxide is less effective than hydrogen peroxide because it breaks down more slowly and has a lower concentration of peroxide.3
During whitening treatment, hydrogen peroxide breaks down into water and peroxide radicals, which are then absorbed by the tooth.3 Unstable electrons inside these radicals seek to bond to unsaturated double bonds, which typically are darker and yellow-pigmented.3Free radicals react with the double carbon bonds and break them into single carbon bonds, which reflect light and make teeth appear whiter.3
TREATMENT CATEGORIES
The American Dental Academy (ADA) recognizes three categories of teeth whitening products: over-the-counter (OTC), at-home, and in-office bleaching or whitening products.9
OTC whitening products include toothpastes, whitening strips, mouth rinses, and gels that are either painted on teeth or administered through the use of trays.4,6 As with all the categories of whiten-
ing products, OTC products contain peroxide-based bleaching compounds, but in lower concentrations than are found in the at-home and in-office options.6 Because they have lower concentrations of peroxide, OTC whitening products typically require long-
er treatment times for results to be seen.6 Additionally, without a proper diagnosis, treatment planning, and supervision by a dentist, outcomes are less predictable and adverse events are less manageable.
The most frequently used teeth whitening methods are the at-home and in-office treatments, both of which are supplied by a dental professional, with at-home treatments being self-admin-
istered by the patient.10,11 At-home kits contain a lower concentration of peroxide (10% to 20% carbamide peroxide) than in-office treatments and are typically administered through custom-fitted trays to be worn either during the day or overnight.3 In-office whitening treatments are the popular option for patients looking to achieve brighter results quickly, owing to the use of higher concentrations of peroxide (30% to 35% hydrogen peroxide).9,12 However, using higher concentrations of peroxide has been associated with increased sensitivity and other adverse effects.7-9
ADVERSE EFFECTS
While considered a safe, effective, and minimally invasive treatment, teeth whitening does come with some risks.8 Temporarily increased dental sensitivity and mild irritation are the most common side effects reported with teeth whitening treatments, and are reported to occur with all categories of whitening products.12-16 The degree to which side effects are experienced by the patient correlates directly with the whitening agent used, its concentration, and the duration of the contact time on the teeth.12
Gingival Irritation
Soft tissue irritation can result from contact with peroxide-based gels, typically occurring within 1 day of treatment and lasting for several days.7,12 Gingival irritation is usually the result of poorly fitting trays or improper gingival isolation methods.17
Tooth Sensitivity
Tooth sensitivity during and after whitening treatment is a common, temporary side effect that normally persists for approximately 4 to 7 days after treatment.7,8 Sensitivity has been attributed to a number of causes, including pulpal inflammation from microscopic surface defects and pores in the tooth enamel that allow the whitening agent to come into contact with the pulp.7,8 Whitening sensitivity can also originate from teeth desiccation, or dehydration, which can result from a few different processes used with most whitening methods.
Nearly all in-office teeth whitening treatments use lip retractors, and many involve the use of ultraviolet or LED lights and a dental dam, which are known to be contributing factors to teeth desiccation.18,19 In 2009, a study completed by Dr Van Haywood determined that the use of a rubber dam for 1 hour or more-the approximate duration of standard in-office teeth whitening treatments-could cause desiccation of the teeth.20 In the same study, Haywood determined that high-powered lights purported to accelerate whitening were not actually helping to whiten teeth but were instead causing the teeth to become dehydrated, which not only results in magnified whitening outcomes that are only temporary, but in intensified tooth sensitivity.20 Furthermore, the use of high-powered lights during these treatments has been shown to cause an increase in pulpal temperatures, potentially damaging teeth and increasing sensitivity and pain for the patient.21,22
MITIGATION OF ADVERSE EFFECTS
While side effects and adverse effects are common with whitening treatments, in-office supervision by a dental professional can reduce the potential risks of these events.16
Effective Gingival Isolation
Instances of burning or irritation to intraoral soft tissues can be reduced with in-office gingival isolation methods that prevent peroxide from contacting soft tissues. Philips® Zoom (Konin-
klijke Philips N.V.) uses Liquidam® (Discus Dental, LLC) light-cure resin to create a gingival barrier for in-office Zoom whitening treatments,23 while many other in-office options such as Opalescence™ Boost™ (Ultradent Products, Inc.)24and Thera-
Smile® Whitening system (Mavrik Dental Systems® Ltd.) employ their own brand of resin products.25 Because TheraSmile Whitening treatment fluids are dynamically delivered, more advanced gingival protection is needed during treatment than with statically applied gels.26Thus the TheraSmile Whitening treatment employs additional gingival protection that replaces the standard dental dam with a proprietary single-use, silicone guard called the MavGuard® that comes pre-cut to fit over the upper and lower gingiva.26 The process is completed with their ArmorLC™ light-cure resin along gingival margins27 (Figure 3).
Sensitivity Prevention
Reducing the likelihood of sensitivity with in-office whitening can be accomplished by using products with lower concentrations of peroxide or that require shorter treatment times, as well as by avoiding products that dehydrate the teeth, such as lip retractors, dental dams, or light accelerators.
Philips Zoom WhiteSpeed uses both lip retractors and a blue LED lamp but includes application of a post-treatment gel that helps protect enamel and reduce sensitivity.28 As with most other treatment options, Philips Zoom QuickPro uses lip retractors, but it offers a shorter treatment time and does not require the use of a lamp, and is therefore less likely to cause sensitivity. The TheraSmile Whitening system, which uses a closed-mouth protocol that does not involve the use of lip retractors, maintains a consistently hydrated treatment environment for teeth, thus helping prevent desiccation-related sensitivity.29
THE ECONOMIC IMPACT OF TEETH WHITENING TREATMENTS
Dental practices that are looking for ways to increase profitability will want to consider incorporating teeth whitening into their treatment offerings. With teeth whitening demand continuously on the rise, market revenue for professional in-office teeth whitening is slated to increase by more than 28% by 2025.30
Patients who are actively taking care of their oral health and visit their dentist regularly are often interested in integrating teeth whitening procedures into their treatment plans. If a dental practice is not offering teeth whitening treatments, its patients may choose to look elsewhere for these services and, potentially, for their other oral care needs. Similarly, whitening treatments that deliver results quickly with little to no sensitivity can be the differentiator that brings patients to the dental practice, whether they have found the practice on their own or by referral. Positive whitening experiences at a dental practice will promote patient retention and word-of-mouth referrals that can keep the practice productive for the long term.
CONCLUSION
Tooth discoloration, which has natural variations in color and gradations, has many causes. Proper diagnosis of the type and etiology of staining by a dental professional can help in determining the best treatment plan to achieve the desired results for the patient. For patients who want to whiten their teeth and mitigate side effects, professional in-office and at-home whitening treatments under a dentist's supervision are the ideal options. Several professional treatments that are currently available offer effective protocols for preventing instances of gingival irritation and tooth sensitivity, when administered as directed. Professionally administered whitening can help ensure a more comfortable patient experience and optimal outcomes.
About the Author
Troy Schmedding, DDS
Private Practice,
Walnut Creek, California
References
1. Heymann HO. Tooth whitening: facts and fallacies. Br Dent J. 2005;198
(8):514.
2. Watts A, Addy M. Tooth discolouration and staining: a review of the literature. Br Dent J. 2001;190(6):309-316.
3. Levine JB. Teeth-whitening technology. Inside Dentistry. 2017;13(3):
42-48.
4. Hosdurga, R. Extrinsic stains and management: a new insight. J Acad Indus Res. 2013;1(8):435-441.
5. Haywood VB, Heymann HO. Nightguard vital bleaching. Quintessence Int.1989;20(3):173-176.
6. Jordan RE, Boksman L. Conservative vital bleaching treatment of discolored dentition. Compend Contin Educ Dent.1984;5(10):803-805, 807.
7. Alqahtani MQ. Tooth-bleaching procedures and their controversial effects: a literature review. Saudi Dent J. 2014;26(2):33-46.
8. Addy M, Roberts WR. The use of polymethylmethacrylate to compare the absorption of staining reactions of some cationic antiseptics. J Periodontal. 1981;52(7):380-385.
9. Department of Scientific Information, Evidence Synthesis & Translation Research, ADA Science & Research Institute, LLC. Whitening. ADA website. www.ada.org/en/member-center/oral-health-topics/whitening. Updated October 30, 2020. Accessed December 13, 2021.
10. Mounika A, Mandava J, Roopesh B, Karri G. Clinical evaluation of color change and tooth sensitivity with in-office and home bleaching treatments. Indian J Dent Res. 2018;29(4):423-427.
11. Moghadam FV, Majidinia S, Chasteen J, Ghavamnasiri M. The degree of color change, rebound effect and sensitivity of bleached teeth associated with at-home and power bleaching techniques: a randomized clinical trial. Eur J Dent.2013;7(4):405-411.
12. Carey CM. Tooth whitening: what we now know. J Evid Based Dent Pract. 2014;14 (Suppl):70-76.
13. de Geus JL, Wambier LM, Kossatz S, Loguercio AD, Reis A. At-home vs in-office bleaching: a systematic review and meta-analysis. Oper Dent. 2016;41(4):341-356.
14. Kielbassa AM, Maier M, Gieren A-K, Eliav E. Tooth sensitivity during and after vital tooth bleaching: a systematic review on an unsolved problem. Quintessence Int. 2015;46(10):881-897.
15. Rodríguez-Martínez J, Valiente M, Sánchez-Martín MJ. Tooth whitening: from the established treatments to novel approaches to prevent side effects. J Esthet Restor Dent. 2019;31(5):431-440.
16. Li Y, Greenwall L. Safety issues of tooth whitening using peroxide-based materials. Br Dent J. 2013;215(1):29-34.
17. Li Y. Safety controversies in tooth bleaching. Dent Clin North Am. 2011;55(2):255-263.
18. Jordan RE, Boksman L. Conservative vital bleaching treatment of discolored dentition. Compend Contin Educ Dent.1984;5(803-805):807.
19. Ontiveros JC. In-office vital bleaching with adjunct light. Dent Clin North Am.2011;55(2):241-253.
20. Haywood VB. In-office bleaching: lights, applications and outcomes.
Curr Pract. 2009;16(4):3-6.
21. Pace Brinker S. Is light-accelerated whitening worth the pain? https://aacd.com/is-light-acceleratedwhitening-worth-the-pain. Published
August 15, 2017. Accessed December 13, 2021.
22. Buchalla W, Attin T. External bleaching therapy with activation by heat, light or laser--a systematic review. Dent Mater. 2007;23(5):586-596.
23. Philips Zoom WhiteSpeed Light-Accelerated Tooth Whitening Procedure Kit [Instructions for Use]. Ontario, CA: Discus Dental, LLC. Retrieved from www.documents.philips.com/assets/20211007/71d0ef4abb834e5daeacadba0110ec28.pdf
24. Opalescence™ Boost™. Procedures. www.ultradent.com/products/categories/whitening/in-office/opalescence-boost. Accessed December 13, 2021.
25. TheraSmile® whitening machine by Mavrik Dental Systems®. (n.d.). https://mavrikdental.com. Accessed December 13, 2021.
26. MavGuard® advanced gingival isolation by Mavrik. (n.d.). https://mavrikdental.com/products/mavguard. Accessed December 13, 2021.
27. ArmorLC® light-curing resin barrier by Mavrik. (n.d.). https://mavrikdental.com/products/armor-lc. Accessed December 13, 2021.
28. In-office whitening. Philips Zoom. (n.d.). www.usa.philips.com/c-m-pe/teeth-whitening/zoom-in-office. Accessed December 13, 2021.
29. TheraSmile oral care automation. (n.d.). https://mavrikdental.com/products/therasmile-system. Accessed December 13, 2021.
30. The global teeth whitening market to reach revenues of over $6.6 billion by 2025 - Market research by Arizton [press release]. Markets Insider website. Retrieved from https://markets.businessinsider.com/news/stocks/the-global-teeth-whitening-market-to-reach-revenues-of-over-6-6-billion-by2025-market-research-by-arizton-1028704469. Published November 20, 2019. Accessed December 13, 2021.
31. Manuel ST, Abhishek P, Kundabala, S. Etiology of tooth discoloration - a review. Nigerian Dent J.2010;18(2): 56-63.