You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
When patients present with erosive tooth wear, which may be caused by such common conditions as gastroesophageal reflux disease, the erosion process must be properly identified and diagnosed before proceeding with a smile design change. Erosive wear is defined by hard tissue loss of teeth absent of bacterial acid.1 Time, frequency, duration, and temperature of the acid determine the extent of damage seen on hard tissue.2 Barbour and Rees also noted that the titratability of the acid, overall pH, and total ion concentrations will also have influence over the severity of erosive wear seen in patients.3 While there are many sources of the acid that results in damage to hard tissues, for the purpose of this discussion the author includes gastric acids from voluntary and involuntary causation, namely gastroesophageal reflux (GERD) and bulimia nervosa. In the present case, dentoalveolar extrusion of the patient's maxillary anterior teeth was diagnosed as a secondary condition to tooth erosion resulting from a long-standing reflux. A three-phase treatment plan included improved management of the patient's reflux symptoms by working with her primary care physician, orthodontics, and full-coverage restorations. A key component of the zirconia-based treatment was the use of an intraoral scanner for digital impressions, which allowed for clear marginal visualization, time efficiency, and a simplified impression process.
Current literature suggests a prevalence of 8% to 33% for GERD worldwide across all ages and genders.4 With this level of prevalence in today's patient population, dentists will likely encounter many patients with GERD over their professional career. The impact of acidic substances such as stomach acid (pH 2.5) on tooth enamel (pH 5.5) is a demineralization of enamel, resulting in dissolution of hydroxyapatite over time. When activities such as chewing, brushing, and swallowing are added, the destruction of enamel and later dentin can be quite extensive. 1 In some cases, the patient will be aware of their condition and whether treatment has been indicated by their primary care physician, while others will present with clinical signs and symptoms of GERD with no formal diagnosis by a medical provider. Common symptoms of GERD can often include pain in the chest, burning sensations in the throat, regurgitation, and chronic cough.5 Understanding a patient's medical record, including past and present conditions, is imperative to a comprehensive oral diagnosis.
When patients present in a dental setting without prior knowledge of any gastroesophageal reflux, a dentist plays an integral part in working with the patient and physician to move forward with diagnosis and treatment. Dentists can provide referrals to primary care physicians or specialists which include examination findings and intraoral photography to express the concerns observed. A referral might also include a request for a comprehensive in lab sleep test as GERD and sleep related breathing disorders are highly correlated disease processes.6 A dentist should be prepared to encounter potential challenges when communicating with physicians regarding an oro-systemic connection but must persist for the benefit of the patient.7 A patient should consider both oral and systemic treatment of erosion in order to achieve ideal outcomes dentally. Even the best dentist will have premature failure of restorative work when completed in compromised environments such as high acidity. A patient should understand this risk prior to moving forward with dental treatment to prevent unmet expectations of future dental restorative success.
A patient at the author's practice had been concerned for years with how much shorter her teeth appeared than when she was younger. The woman had presented at age 57 with a history of acid reflux and bulimia, although the latter had been under control for some time. The patient was currently under the care of a physician for the management of gastroesophageal reflux but still reported occasional symptoms despite treatment. She wanted a "quick fix" to her chief complaint of shorter anterior teeth. She thought her length could be restored by simply adding bonding to the edges of her teeth, and believed that the reflux had affected only the incisal edges. This type of thinking is not surprising, as patients often do not notice the subtle changes that occur over time, like dentoalveolar extrusion, buccal collapse, and premature contacts. Patients often can only appreciate that something looks different and is unattractive to them, and in their mind the solution should be relatively quick and easy. To the patient, the changes seem to happen relatively quickly, while clinicians know these types of structural changes occur often over years to decades. With the advent of social media, direct-to-consumer treatment options, and instant makeovers on television, patients often do not understand the complexity or length of time involved in complex treatment plans. Additionally, clinicians often gloss over the "gory" side of dentistry to provide comfort to patients and to ensure they seek treatment. Dentists' successful ability to undersell their services means many patients will not fully comprehend the journey required for full rehabilitation. This author's patient was no exception to that challenge.
Gastric reflux, whether voluntary or involuntary, can be very destructive to tooth structure. During an intraoral examination, several factors can suggest to the clinician an active or past presence of GERD. Much like most extrinsic cases of erosion (from GERD or bulimia), the wear presents as smooth lingual surfaces of the maxillary anterior teeth and flattened occlusal surfaces of mandibular posterior molars.8 This erosive wear evolves over time and destroys the enamel except along the gingival margin, giving the teeth a darker hue.9 As the lingual surfaces of the maxillary teeth begin to erode, the teeth often respond by undergoing dentoalveolar extrusion.10 This process needs to be identified and diagnosed appropriately when proceeding with a smile design change to achieve an ideal cosmetic result. In this patient's case, dentoalveolar extrusion of the maxillary anterior teeth was diagnosed as a secondary condition resulting from the long-standing reflux condition.
Three-Phase Treatment Plan
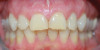
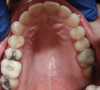
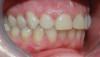
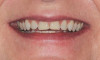
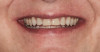
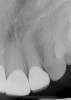
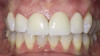
After several years and many consultations, the patient finally agreed to move forward with the recommended treatment. The patient's pretreatment condition is depicted in Figure 1 through Figure 3. Upon evaluation, several conditions were documented. The observation of a more coronally positioned gingival margin on the maxillary anterior teeth was noted. The differential diagnosis of dentoalvealor extrusion versus altered passive eruption was considered. The process of altered passive eruption was ruled out after appropriate bone sounding and palpation of the cemento-enamel junction (CEJ) apical to tooth Nos. 7 through 10. The gingival margin and bone heights were determined to be localized in a normal position within the gingival sulcus. This confirmed the diagnosis of dentoalveloar extrusion.10 As the linguals of the upper teeth were destroyed with acidic exposure, the teeth continued to erupt into function. Observations also included buccal collapse of the arches, malalignment of teeth, incisal wear, and dentoalveolar extrusion of the lower anterior teeth. A thorough smile design work-up was completed using numerous intraoral and extraoral radiographs and photographs. The lower incisal edges, particularly of tooth Nos. 24 and 25 showed signs of extrusion and wear but since the incisal edges closely followed the curvature of the lower lip line and the patient was only interested in maxillary treatment, their intrusion was limited to leveling and aligning the incisal edges. The preferred treatment option in this type of case is to consider orthodontic intrusion of maxillary teeth to relevel the gingival margins and subsequently increase occlusal clearance between arches for restorations. At that point, a treatment plan was developed that would address incisal edge position, which had shortened over time, and the appearance of gingiva versus tooth structure during a full smile.11 In addition, the photographs were used to evaluate the curvature of her smile, the midline of the teeth to the face, and the overall esthetics of the smile.
The treatment plan was then constructed to be in three phases. The first phase was to improve management of the patient's reflux symptoms working through her primary care physician. The second and third phases would be dentally driven changes through orthodontics and full-coverage restorations, respectively.
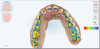
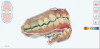
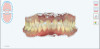
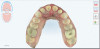
Working with a local orthodontist, the author's team proceeded with clear aligner therapy to level and align the occlusion and intrude the maxillary anterior teeth back to their original gingival position. The patient was presented with both clear aligner therapy and conventional orthodontics. She was only willing to pursue treatment using clear aligners. Unfortunately, aligner therapy proved to be highly challenging because the patient maintained poor compliance. After 18 months of orthodontics, there was minimal improvement in tooth position (Figure 4 and Figure 5). It was evident that during treatment the patient rarely wore her aligners for as much as 12 hours a day. Compliance played a part in the clinician's decision paradigm and risk management of the patient moving forward.
The patient was interested in changing her overall tooth shade before new restorations were fabricated. In the author's practice, if a patient desires a shade change, a bleaching protocol typically is completed prior to their preparation visit. In this case, after completing 2 weeks of an at-home bleaching regimen, the patient was ready to proceed with anterior restorations. Shade matching can be completed at the preparation visit, as shade regression from at-home bleaching is not shown to be statistically significant when done within 6 months of completion.12 Full-coverage porcelain restorations were chosen over veneers because priority was placed on protecting the lingual surfaces of the teeth from further erosion.13 While the patient's reflux condition was being supervised by a medical physician, there was residual concern that more damage would occur since the reflux continued to be moderately present.
Zirconia Restorations
Preparation of the teeth was completed to allow for monolithic zirconia-oxide restorations. Full-coverage restorations were selected for this case for several reasons: the teeth had existing interproximal restorations with recurrent decay, prior facial bonding, and erosion of most of the enamel on the lingual surfaces. Full-coverage restorations would be able to meet the esthetic needs to the patient while protecting the teeth from continued erosive challenges in the future. The lingual preparations were as minimal as possible due to previous erosive reduction. Preparation of the full-coverage restorations on the lingual was only performed to accommodate zirconia restorations, as further preparation would have likely resulted in pulpal involvement of the teeth.
Because the patient was not as compliant as needed during the orthodontic phase of treatment, the amount of clinical overjet that was desired was not achieved (Figure 6 and Figure 7). As a compromise to meet this challenge, the author had to limit the choice of materials for the final restorations due to reduced interarch spacing at the end of orthodontics. A monolithic zirconia base was selected because of several physical characteristics that made it a well-suited material for this case. First, its high flexural strength at lower thickness compared to other ceramic options would allow the restoration to be able to withstand the limited overjet created from the orthodontic treatment without catastrophic failure.15 Monolithic zirconia oxide also is a superior material for minimizing wear on opposing teeth, which was desirable in this case, as other biochemical issues were already creating a caustic environment for the patient's enamel integrity.16 Moreover, monolithic zirconia-oxide restorations require less preparation of the teeth, which allows the clinician to maintain a greater amount of pulpal integrity of the teeth. On the other hand, the laboratory opted to add a layer of pressed porcelain on the zirconia-oxide cores to improve the overall esthetics of the case. Layered zirconia restorations are more susceptible to fracture and chipping over time.15
Tissue retraction was managed with two cords (size 1), which were placed as atraumtically as possible. The decision was then made to impress the case using an intraoral scanner. Digital impressions were chosen because they offer clear marginal visualization, time efficiency, and patient comfort.14
Scans of the preparations, opposing arch, and buccal bite were completed. The STL file of the impressions was immediately sent to the laboratory along with a prescription for the restorations. Additionally, the clinical photographs were sent to the laboratory via email to aid in the customization of the final product.
Based on the clinical photographs emailed to the laboratory, the master ceramist determined that a pressed porcelain veneer on the zirconia core would provide the customization of shade required to match the patient's existing dentition. The final restorations were made of zirconium dioxide with a feldspar veneering ceramic, shade 1M1, as the pressed layer on porcelain on the facials. The restorations had pressed porcelain only from above the incisal edge to the gingival margin. Monolithic zirconia oxide was used for the lingual and incisal edges of the restorations in an effort to prevent chipping.
Delivery and Final Outcome
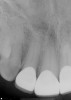
The restorations were delivered a few weeks later. Prior to cementation, marginal integrity of the restorations was reviewed. The author's protocol for approval of restorations for final delivery includes tactile and radiographic evaluation of the margins (Figure 8 and Figure 9). Once the restorations were approved for marginal integrity, occlusion, contacts, and esthetics, the process of isolation and cementation began. In this case, it was decided to cement the restorations with resin-modified glass-ionomer cement (RMGIC). The long-term stability of using RMGIC to cement zirconia-oxide restorations, especially for preparations of teeth demonstrating an adequate resistance and retention form, has been shown to be effective in preventing premature loss of restoration and microleakage.17
The final outcome of the case met the patient's primary concerns, achieving the lengthening and lightening of the anterior teeth that she desired (Figure 10). As a clinician, the author noted several areas in the patient's overall smile where a more ideal result could have been achieved. However, because of the patient's continued challenges with GERD, she reported having difficulty with compliance related to clear aligner therapy and whitening protocols. Nonetheless, the patient was pleased with her new smile and the clinician was satisfied with the clinical results of the final restorations.
Digital Impressions
Digital impressions are an effective alternative to conventional impression techniques and may be considered as the first option for impression-taking because of predictable, efficient, and simplified processes for both patients and clinicians.18 Using an intraoral scanner, such as the iTero Element 2 used in this case, affords the clinician many efficiencies that cannot be achieved with traditional polyvinyl siloxane (PVS) impression materials. Preparations can be reviewed and verified, including marginal clarity and restorative clearance, while the patient is still in the office. With a digital platform such as MyiTero (Align Technology, Inc.) or other comparable software, clinicians can quickly assess the quality of their preparations, marginal design, marginal visualization, and clearance between arches, as shown in Figure 11 and Figure 12, which are additional digital images of the preparations in this case. If any areas require modification, the clinician can complete those steps and rescan the areas as needed without having to reappoint the patient. Digital impressions also provide a permanent record storage of the case which can be revisited at any time.
When using PVS impression techniques, clinicians are limited in their ability to assess an ideal impression, marginal integrity, and interarch clearance. Clinicians often will temporize the patient and hope the information captured in PVS, as well as the quality of their preparations, meets the clinical standards to fabricate an ideal restoration. With digital impressions, clinicians can avoid unwanted phone calls from the lab requesting more clearance or a better impression of the margin. Digital impressions allow clinicians to be confident that their crown deliveries will be completed with high success rates. By developing a proper smile design treatment plan and executing each phase of treatment completely, practitioners can achieve a high-quality result despite a patient's overall lack of compliance with treatment.
Conclusion
The advent of digital impression techniques as also brought along the ability to track oral changes over time. Scanning of full dental arches allows clinicians to take images of a patient periodically and overlay the scans to note changes. This aids clinicians in noting changes related to recession, abfraction, abrasion, occlusion, and erosion, and help patients appreciate a condition which is often asymptomatic and changing subtly over time. Clinicians are then able to intervene more quickly with the consent and willingness of a patient who has become a more educated consumer of his/her healthcare.
ACKNOWLEDGMENT
The author would like to acknowledge Precision Esthetics Dental Laboratory (precisionesthetics.com), West Palm Beach, Florida, for the laboratory work in this case, and Fritz Orthodontics, Holly Springs, North Carolina, for the orthodontic photographs and work.
About the Author
Jennifer Bell, DDS
Private Practice, Holly Springs, North Carolina; Fellow, Academy of General Dentistry
References
1. MRamachandran A, Raja Khan SI, Vaitheeswaran N. Incidence and Pattern of Dental Erosion in Gastroesophageal Reflux Disease Patients. J Pharm Bioallied Sci. 2017;9(Suppl 1):S138-S141.
2. West NX, Hughes JA, Addy M. Erosion of dentine and enamel in vitro by dietary acids: the effect of temperature, acid character, concentration and exposure time. J Oral Rehabil. 2000;27(10):875-880.
3. Barbour ME, Rees GD. The role of erosion, abrasion and attrition in tooth wear. J Clin Dent. 2006;17(4):88-93.
4. Gyawali CP, Kahrilas PJ, Savarino E, et al. Modern diagnosis of GERD: the Lyon Consensus. Gut. 2018;67(7):1351-1362.
5. Dundar A, Sengun A. Dental approach to erosive tooth wear in gastroesophageal reflux disease. Afr Health Sci. 2014;14(2):481-486. doi:10.4314/ahs.v14i2.28
6. Emilsson ÖI, Bengtsson A, Franklin KA, et al. Nocturnal gastro-oesophageal reflux, asthma and symptoms of OSA: a longitudinal, general population study. Eur Respir J. 2013;41(6):1347-1354. doi:10.1183/09031936.00052512
7. Sippli K, Rieger MA, Huettig F. GPs' and dentists' experiences and expectations of interprofessional collaboration: findings from a qualitative study in Germany. BMC Health Serv Res. 2017;17(1):179. Published 2017 Mar 7. doi:10.1186/s12913-017-2116-4
8. Donovan T. Dental erosion. J Esthet Restor Dent. 2009;21(6):359-364.
9. Lussi A, Jaeggi T. Erosion-diagnosis and risk factors. Clin Oral Investig. 2008;12(suppl 1):S5-S13.
10. Dolt AH 3rd, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28(6):363-372.
11. Tak On T, Kois JC. Digital smile design meets the dento-facial analyzer: optimizing esthetics while preserving tooth structure. Compend Contin Educ Dent. 2016;37(1):46-50.
12. Velayati Moghadam F, Majidinia S, Chasteen J, Ghavamnasiri M. The degree of color change, rebound effect and sensitivity of bleached teeth associated with at-home and power bleaching techniques: a randomized clinical trial. Eur J Dent. 2013;7(4):405-411.
13. Lambrechts P, Van Meerbeek B, Perdigão J, et al. Restorative therapy for erosive lesions. Eur J Oral Sci. 1996;104(2[Pt 2]):229-240.
14. Mangano F, Gandolfi A, Luongo G, Logozzo S. Intraoral scanners in dentistry: a review of the current literature. BMC Oral Health. 20172;17(1):149.
15. Sun T, Zhou S, Lai R, et al. Load-bearing capacity and the recommended thickness of dental monolithic zirconia single crowns. J Mech Behav Biomed Mater. 2014;35:93-101.
16. Albashaireh ZSM, Ghazal M, Kern M. Two-body wear of different ceramic materials opposed to zirconia ceramic. J Prosthet Dent. 2010;104(2):105-113.
17. Dogan S, Raigrodski AJ. Cementation of zirconia-based toothborne restorations: a clinical review. Compend Contin Educ Dent. 2019;40(8):536-540.
18. Rutkūnas V, Gečiauskaite A, Jegelevičius D, Vaitiekūnas M. Accuracy of digital implant impressions with intraoral scanners. A systematic review. Eur J Oral Implantol. 2017;10(suppl 1):101-120.