You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
There is disagreement in the dental literature concerning the ability of dental implants to preserve peri-implant bone height. It is also unclear whether bone loss adjacent to dental implants continues throughout life. Previously, it was concluded there was inadequate proof to substantiate that implants maintain bone1; however, premises upon which this statement was based are suspect. Therefore, this article assesses relevant information to determine if there is sufficient evidence to confirm that implants assist in sustaining bone height. In addition, data are appraised to ascertain if osseous resorption persists after osseointegration occurs. To answer these questions, clinical investigations are evaluated with respect to vertical bone loss associated with the following scenarios: aging, after extraction(s), subsequent to immediate and delayed implant placement, following implant insertion into partially and fully edentate healed ridges, and under implant-retained/supported overdentures.
Physiologic Bone Reduction
No longitudinal studies were found that assessed the rate of bone loss in edentate sites when a prosthesis was not worn. In this regard, osseous resorption associated with denture wearing does not reflect physiologic bone reduction due to aging or disuse atrophy.2 Under a removable prosthesis, bone loss is usually caused by compressive forces, thereby inducing pressure necrosis.2 However, some individuals who do not wear prostheses manifest severely atrophied ridges. This could be attributed to disuse atrophy, prior history of periodontitis, damage during tooth extraction, systemic issues, etc.
Information related to long-term reduction of bone height was reported in dentate individuals. Streckfus et al3 suggested there was a relationship between bone resorption and aging. They reported that individuals with good versus poor oral hygiene respectively lost 0.38 mm and 0.89 mm of bone per decade adjacent to teeth. However, these data are based upon cross-sectional studies that compared amounts of osseous resorption among individuals in different age brackets; this information was not derived from longitudinal investigations. The finding of a small rate of bone loss over time is in agreement with others who assessed healthy cohorts of individuals and found 0.5 mm to 0.7 mm reduced osseous levels per decade adjacent to teeth.4,5 Pertinently, Huttner et al6 concluded that aging does not induce a significant amount of bone reduction in healthy patients, rather bone formation decreased as individuals aged. It was proposed that this may be due to biochemical alterations of cells, which contribute to disequilibrium between osteoblastic and osteoclastic activities during bone remodeling.
Bone Loss After Dental Extractions
After a tooth is extracted, bone resorption occurs in the vertical and horizontal planes.7,8 In humans, the mean vertical bone loss after flap elevation and an extraction is approximately 1 mm to 1.5 mm,9-11 but it can range from 0 mm to 4 mm. Horizontal bone reduction is approximately 3 mm to 4.5 mm and may be up to 6 mm.9-11 Multiple extractions of adjacent teeth result in more bone resorption than a single extraction.12,13
Subsequent to tooth removal, the buccal plate usually manifests the greatest amount of bone loss, because it is the thinnest supporting wall of the alveolus.7,8 Spray et al14 noted that osteotomies in healed ridges with ≥ 2-mm thick buccal plate do not normally resorb vertically, whereas osteotomy walls < 2-mm wide demonstrate bone loss. (These data may also be true for extraction socket walls, but this has not been investigated.) In the anterior maxilla, the breadth of the buccal plate varies, but it is typically < 2 mm (mean width: buccal 1.59 mm).15 Others reported that the buccal plate is usually less than 1-mm thick.16,17
Long-term assessments of bone loss among denture wearers were recorded.18,19 Tallgren et al18 found that about 2.5 mm to 3 mm of bone height was resorbed in the anterior maxilla and about 9 mm to 10 mm was resorbed in the mandible during a 25-year monitoring period. Similarly, Atwood and Coy19 noted 3-mm bone reduction in the maxilla and 14.5-mm in the mandible over 19 years. In both studies, after extractions, there initially was a large amount of bone loss after which the resorptive rate decreased. These investigations demonstrated great variation among individuals with respect to the amount and rate of bone resorption per year, and it was suggested that bone reduction was continuous after extractions.18,19 With respect to the above studies, the annual rate for bone loss was calculated: 0.05 mm – maxilla, 0.2 mm – mandible18; 0.1 mm – maxilla, 0.4 mm – mandible.19 However, it was not clear if bone resorption was constant, episodic, or combinations of both patterns.
Measurement Error
Historically, Albrektsson et al20 established that 1.5 mm of bone loss during the first year after implant insertion was commonplace. Afterward, osseous reduction of < 0.2 mm per year was considered a successful outcome. However, the question arises as to whether clinicians can monitor 0.2 mm osseous changes per year.21-26 This is a dilemma, because bone-level assessments using x-ray paralleling technique have a precision of around 0.5 mm.21 Therefore, there may be an inherent amount of measurement error associated with assessing small changes in vertical bone height.
Factors That Can Influence Bone Loss After Implant Placement
The following surgical protocols can affect bone resorption: submerging versus not submerging implants under soft tissue27; one- versus two-piece implants28; supracrestal, crestal, and subcrestal placement of implants29; and flapless versus flap implant insertion.30 Previously, animal studies confirmed that bone is lost during the first year after uncovering submerged crestally placed implants, and this is due to biologic width formation.31,32 In humans, two-piece implants, which were initially submerged and uncovered to place abutments, were estimated to lose 1 mm to 1.5 mm of bone by the end of the first year.20,33-35 Crestal or subcrestal implant placement resulted in development of a subcrestal biologic width. In contrast, one-piece implants, whose platforms were placed supracrestally, lost 0.75 mm to 1 mm of bone during the first year.36-38 The decreased amount of osseous reduction was attributed to supracrestal biologic width formation. In general, the magnitude of bone resorption around implants varied within and among studies due to inability to control confounding variables (eg, width of the alveolar ridge, personal hygiene).
Immediate Placement of Implants: Vertical Bone Resorption
Implants immediately placed into extraction sockets have a high survival rate, similar to implants inserted into healed ridges.39-41 However, the issue as to whether immediate implants help maintain bone is controversial. To clarify the ability of implants to preserve bone, three questions are posed: 1) Is there bone loss after immediate implant placement? 2) Post immediate implant insertion, is there less osseous resorption than after an extraction when no implant is placed? and 3) Does immediate implant placement retain more bone than delayed implant insertion?
Numerous investigations confirmed that immediate implantation is associated with vertical and horizontal bone loss. This has been documented in dogs8,42 and humans.13,39,40,43 Answering the second question is more difficult. Several canine studies directly compared bone loss at sites after extractions with and without immediate implant placement.8,44 Araújo et al8 reported that the amount of bone reduction was similar in both situations, whereas Vignoletti et al44 noted that the amount of osseous resorption was greater when implants were inserted. A possible explanation for this discrepancy was provided by Ferrus et al.45 They reported that buccal plate thickness and size of the horizontal gap influenced hard-tissue alterations after immediate placement. Some authors suggested that avoidance of flap elevation reduced bone loss after tooth removal and immediate placement.30 In contrast, Caneva et al46 determined that even with a flapless approach, the amount of vertical bone resorption was similar with and without flap elevation. Conceptually, a flapless approach would benefit bone maintenance, because there would be less disturbance of the bone’s vascularity.30
In humans, the quantity of bone loss after immediate implant placement during the first year47-50 appears to be less than reported when teeth are extracted and no implants are placed.9-11 However, this statement is based on studies that did not directly compare patients that received both therapies. For example, it was previously noted that 1 mm to 1.5 mm vertical bone height is routinely lost after an extraction,9-11 whereas vertical bone loss reported the first year after immediate implant placement was 0.6 mm with TiOblast™ fixtures (DENTSPLY Implants, www.dentsplyimplants.com),47 0.4 mm for Astra Tech (DENTSPLY Implants),48 0.37 for NanoTite™ Prevail®49 (Biomet 3i, www.biomet3i.com), and 1.1 mm of bone reduction occurred after nonocclusal and early loading with Osteotite® implants (Biomet 3i).50
Regarding the third question, additional support for the concept that implants preserve bone can be derived by comparing the amounts of osseous resorption after immediate and delayed implant placement. The data indicate that there were no differences in the amount of bone loss after immediate and delayed placement.40,51,52 However, these studies made direct comparisons with respect to the degree of bone resorption several months after immediate and delayed placement. The baseline for assessing the initial bone height was determined on the day of implant placement. Investigators did not factor in that with delayed placement, bone loss occurred after extractions and prior to delayed insertion of implants. Thus, it can be concluded that delayed placement resulted in an increased amount of bone loss versus immediate insertion, and implant placement contributed to bone preservation. These remarks are made in light of the fact that it is difficult to compare various implant systems, and operator experience can affect results.53
Bone Resorption Associated with Implants Placed into Healed Ridges
Partially Edentulous Patients
Clinical trials addressing short- and long-term peri-implant bone loss in partially and fully edentate healed ridges indicated that bone resorption can be divided into two phases: initial osseous reduction during healing and then a very slow rate of bone loss after implant insertion. In partially edentate ridges, bone resorption ranged from 0.33 mm to 1.5 mm the first year after implantation and subsequently 0 mm to 0.1 mm per year.36,54-57
Fully Edentulous Patients
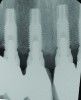
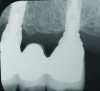
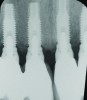
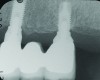
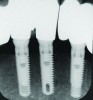
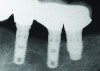
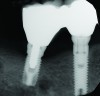
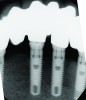
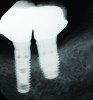
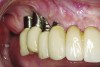
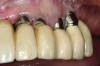
During the first year after implantation, patients with completely restored edentulous ridges demonstrated a mean total bone loss ranging from 0.90 mm to 1.64 mm.58-60 After the first year, the mean annual rate of bone resorption ranged from 0 mm to 0.15 mm58-65 (Figure 1 through Figure 14).
With respect to annual bone loss, O’Neil and Yeung1 compared the above rates of bone resorption (0 mm to 0.15 mm per annum) around implants to a rate of bone loss under dentures selected from an article by Tallgren et al18 (0.05 mm in the maxilla and 0.2 mm in the mandible per annum in years 10 to 25 of the study). They concluded the amount of annual bone loss under dentures and adjacent to implants was similar; therefore, there was insufficient evidence to substantiate the claim that implants affect postextraction bone levels. However, the annual rate of bone resorption under the dentures they used underestimated the annual rate of bone reduction. This statement is based on the following two facts: the mean they used was computed for years 10 to 25 of the monitoring period and did not take into consideration that a large amount of bone resorbed during years 1 to 1018; and this annual rate of bone loss is 50% of the pace reported by Atwood and Coy (0.1 mm in the maxilla [range 0 mm to 0.7 mm], and 0.4 mm in the mandible [range 0 mm to 2.0 mm]).19
Accordingly, if an increased rate of bone loss was selected to represent the pace of osseous resorption under dentures, a comparison between the rates of bone loss under dentures and around implants would indicate that implants preserve bone. Furthermore, the preponderance of data document that usually the amount of bone reduction per year around implants, in the absence of peri-implantitis, is so small that it has a negligible effect on the survival of implants, and it would take years to manifest noticeable bone loss and recession. For example, in areas under implant-supported prostheses (Figure 15), the ridge does not routinely manifest bone resorption and recession.66,67 However, there are patients who demonstrate different degrees of bone loss, and the reason for this is unknown.
Bone Gain Associated with Implant Placement
Anterior, implant-supported fixed mandibular prostheses may facilitate maintenance and possibly bone gain under posterior aspects of rehabilitations.25,26,68,69 This result is attributed to bending moments that create tensional forces and increase osteoblastic activity.26 In addition, the finding of more bone after healing around individual implants supports the concept that implants preserve bone.35,51,70-72 This bone increase is believed to be due to stimulation by the loaded implants on bone remodeling.73 However, detection of bone gain after implantation needs to be interpreted carefully for several reasons. Angulation errors associated with radiographs can result in the appearance of more bone. In addition, the conclusion that there is osseous gain after healing may be erroneous if the bone crest was leveled prior to placing an implant. In these situations, radiographic bone increase could be due to reformation of the crestal cortical bone that was removed.
Implants Under Overdentures: Vertical Bone Reduction
Several systematic reviews addressed marginal bone loss that can occur adjacent to implants supporting overdentures.74-76 Two assessments concluded there was insufficient data regarding bone loss in the maxilla to delineate the magnitude of bone resorption that occurred initially and annually after implant insertion.75,76 Similarly, with respect to the mandible, Ma et al74 noted that studies often failed to provide precise information as to the time of initial radiographic assessment; therefore, it was impossible to determine if the amount of total bone loss included initial healing or occurred after prosthesis insertion. Furthermore, variations in radiographic techniques made it difficult to compare results of investigations. Nevertheless, Cehreli et al75 concluded that in the mandible (eight studies), there was no difference with respect to the bone loss around implants regarding implant systems and attachment designs. The mean total vertical bone loss around implants after > 5 years for different attachment designs was as follows: bar – 0.87 mm; ball – 0.70 mm; and magnet – 0.44 mm.
Numerous authors recorded varied mean total vertical bone loss around mandibular implants supporting overdentures over different periods of time: 2.5 years – 0.93 mm77; 5 years – 0.5 mm78; 12 years – 1.7 mm79; and 16 years – 0.54 mm.80
Average annual bone loss adjacent to implants supporting mandibular overdentures after initial healing was small: after 2.5 years – 0.1 mm77; and > 16 years – 0.043 mm.80 It appears that the amount and annual bone resorption under mandibular overdentures is similar to what is detected around single and multiple implants supporting fixed prostheses in partially36,54-57 and fully edentate patients.58-65
When loss of bone height was directly compared between groups of patients wearing dentures and overdentures, there was more resorption under dentures.81,82 Crum and Rooney81 found that mandibular dentures over a 5-year period resulted in 5.2 mm of bone loss, whereas under overdentures resorption was 0.6 mm. Similarly, but to a lesser extent, Jacobs et al82 demonstrated that over a 12-year observation period, there was greater annual vertical bone loss under a denture than an implant-supported overdenture (0.10 mm versus 0.03 mm per year). There is additional evidence that implants preserve bone from another perspective. Implant-supported overdentures maintain alveolar bone density under prostheses due to load-related positive bone remodeling.67,83 However, these data were specific for osseous density and could not be interpreted to indicate that they preserved bone height.
Comparison of Bone Loss Around Implant-Supported Fixed Prostheses and Overdentures
No long-term study directly compared the amount of marginal bone loss around implant-supported fixed prostheses and overdentures. In this regard, Attard et al84,85 conducted two lengthy investigations; one assessed groups of patients with fixed prostheses, and the other assessed individuals with overdentures. They monitored patients with a total of 33 fixed prostheses for 18 to 23 years. Mean vertical bone reduction the first year was 0.89 mm and, subsequently, the average annual bone loss was 0.05 mm.84 Similarly, among 30 overdenture wearers that were monitored 10 to 19 years, mean osseous reduction the first year was 1.01 mm and then 0.05 mm per year.85 Peri-implant bone resorption varied considerably among patients; some implants lost up to 6 mm of adjacent bone. Based on these two long-term evaluations, it seems that the amount of bone reduction that occurs around implants supporting fixed prostheses or overdentures is similar the first year and during the following years.
Role of Implant Surfaces in Maintaining Bone
Aloy-Prosper et al86 appraised the literature with respect to marginal bone loss adjacent to different implant neck surfaces (implants were present at least 1 year). When textured (without microthreads) and smooth surfaced implants were compared (six studies), four investigations noted no differences in the amount of bone resorption, and two studies reported greater bone loss associated with polished surfaced necks. When textured (with microthreads) versus smooth surfaced implants were evaluated (four studies), all four clinical trials indicated that there was less bone resorption on textured surfaced implants. Thus, six of 10 studies found that textured surfaced implants preserved bone better than smooth surfaced implants, but four of the six investigations had microthreads.
Another recent study indicated that implants with microthreads manifested less bone loss than implants without microthreads after 1 year (0.42 mm with microtexturing and 1.12 mm without microtexturing).87 It appears that when surfaces are compared regarding bone preservation, microthreads may be a critical determinant with respect to retaining additional bone. The microthreads may be providing increased surface area, which facilitates formation of the biologic width on the implant, thereby reducing the amount of bone loss that occurs when re-establishing the biologic width.
Methods to Preserve Bone
Prasad et al88 addressed several techniques that can help maintain osseous support around implants: platform switching and placing an implant with a supracrestal platform. In this regard, a systematic review by Atieh et al89 reported that platform switching resulted in less bone loss around implants than implants restored without platform switching (means 0.055 mm to 0.99 mm versus 0.19 mm to 1.67 mm). It was also underscored that a reduction of bone resorption was attained by placing the implant platform supracrestally to facilitate development of a supracrestal biologic width.27-29
Qualifying Remarks
This assessment presumed patients were healthy. However, there are situations that can contribute to bone loss and individuals may experience a greater amount of osseous resorption than reported in this evaluation: systemic conditions (eg, diabetes, osteoporosis); smoking; medications (eg, bisphosphonates)90,91; subgingival cement retention92 and peri-implantitis; and in some patients, time appears to be a factor (Figure 16 and Figure 17).93 Furthermore, there are patients that lose more bone around implants than expected in the absence of recognized risk factors. It could be speculated that occlusal forces contributed to this, but that is also controversial.94
Summary and Conclusions
The purpose of this assessment was to determine whether dental implants affect bone height. It was clearly documented that the pattern of bone loss after implant placement was biphasic. During the first year after an extraction, there is a relatively large amount of osseous reduction adjacent to implants, and then usually there is a small amount of annual osseous resorption (mean 0.05 mm) that continues throughout a patient’s life. However, there is great variation among individuals, and some patients may manifest large amounts of bone loss and recession.
Regarding the central topic of this paper, there are numerous lines of evidence supporting the concept that dental implants typically help preserve the peri-implant vertical bone height:
• Immediate placement of implants does not prevent osseous resorption, but appears to reduce the amount of bone loss that occurs after tooth extractions.
• Immediate implant insertion seems to help retain more bone than delayed implant placement.
• Single and multiple implants supporting fixed prostheses placed in fully and partially edentulous mouths manifest a very small annual rate of peri-implant bone loss.
• In some patients, osseous levels around implants can increase after implant placement.
• There is less alveolar bone ridge resorption under implant-retained/supported overdentures than under dentures.
• Implants supporting overdentures demonstrate very little bone loss per annum.
In conclusion, the evidence suggests that an implant-supported prosthesis usually retains bone. This is a crucial piece of information when clinicians formulate and present various treatment plans to their patients, especially when they must decide between an implant-supported prosthesis and a removable partial or complete denture.
ABOUT THE AUTHORS
Gary Greenstein, DDS, MS
Clinical Professor, Department of Periodontology, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Periodontics, Freehold, New Jersey
John Cavallaro, DDS
Director, Implant Fellowship Program, Associate Clinical Professor, Prosthodontics, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Prosthodontics, Brooklyn, New York
REFERENCES
1. O’Neill JE, Yeung SC. Do dental implants preserve and maintain alveolar bone? J Investig Clin Dent. 2011;2(4):229-235.
2. Carlsson GE. Responses of jawbone to pressure. Gerodontology. 2004;21(2):65-70.
3. Streckfus CF, Parsell DE, Streckfus JE, et al. Relationship between oral alveolar bone loss and aging among African-American and Caucasian individuals. Gerontology. 1999;45(2):110-114.
4. Rohner F, Cimasoni G, Vuagnat P. Longitudinal radiographical study on the rate of alveolar bone loss in patients of a dental school. J Clin Periodontol. 1983;10(6):643-651.
5. Selikowitz HS, Sheiham A, Albert D, Williams GM. Retrospective longitudinal study of the rate of alveolar bone loss in humans using bite-wing radiographs. J Clin Periodontol. 1981;8(5):431-438.
6. Huttner EA, Machado DC, de Oliveira RB, et al. Effects of human aging on periodontal tissues. Spec Care Dentist. 2009;29(4):149-155.
7. Cardaropoli G, Araújo M, Lindhe J. Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol. 2003;30(9):809-818.
8. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol.2005;32(2):212-218.
9. Lekovic V, Camargo PM, Klokkevold PR, et al. Preservation of alveolar bone in extraction sockets using bioabsorbable membranes. J Periodontol. 1998;69(9):1044-1049.
10. Lekovic V, Kenney EB, Weinlaender M, et al. A bone regenerative approach to alveolar ridge maintenance following tooth extraction. Report of 10 cases. J Periodontol. 1997;68(6):563-570.
11. Camargo PM, Lekovic V, Weinlaender M, et al. M. Influence of bioactive glass on changes in alveolar process dimensions after exodontia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90(5):581-586.
12. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
13. Botticelli D, Persson LG, Lindhe J, Berglundh T. Bone tissue formation adjacent to implants placed in fresh extraction sockets: an experimental study in dogs. Clin Oral Implants Res. 2006;17(4):351-358.
14. Spray JR, Black CG, Morris HF, Ochi S. The influence of bone thickness on facial marginal bone response: stage 1 placement through stage 2 uncovering. Ann Periodontol. 2000;5(1):119-128.
15. Katranji A, Misch K, Wang HL. Cortical bone thickness in dentate and edentulous human cadavers. J Periodontol. 2007;78(5):874-878.
16. Januário AL, Duarte WR, Barriviera M, et al. Dimension of the facial bone wall in the anterior maxilla: a cone-beam computed tomography study. Clin Oral Implants Res. 2011;22(10):1168-1171.
17. Han JY, Jung GU. Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans. J Periodontal Implant Sci. 2011;41(2):60-66.
18. Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27(2):120-132.
19. Atwood DA, Coy WA. Clinical, cephalometric, and densitometric study of reduction of residual ridges. J Prosthet Dent. 1971;26(3):280-295.
20. Albrektsson T, Isidor F. Consensus report of session IV. In: Lang NP, Karring T, eds. Proceedings of the 1st European Workshop on Periodontology. London, England: Quintessence Publishing; 1994:365-369.
21. Schulze RK, d’Hoedt B. Mathematical analysis of projection errors in “paralleling technique” with respect to implant geometry. Clin Oral Impl Res. 2001;12(4):364-371.
22. Sewerin IP. Estimation of angulation of Brånemark titanium fixtures from radiographic thread images. Clin Oral Implants Res. 1991;2(1):20-23.
23. Benn DK. Estimating the validity of radiographic measurements of marginal bone height changes around osseointegrated implants. Implant Dent. 1992;1(1):79-83.
24. Williamson GF. Better techniques, better radiographs. J Prac Hyg. 2003;12:10-15.
25. Davis WH, Lam PS, Marshall MW, et al. Using restorations borne totally by anterior implants to preserve the edentulous mandible. J Am Dent Assoc. 1999;130(8):1183-1189.
26. Reddy MS, Geurs NC, Wang IC, et al. Mandibular growth following implant restoration: does Wolff’s law apply to residual ridge resorption? Int J Periodontics Restorative Dent. 2002;22(4):315-321.
27. Hermann JS, Buser D, Schenk RK, Cochran DL. Crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged and submerged implants in the canine mandible. J Periodontol. 2000;71(9):1412-1424.
28. Hermann JS, Buser D, Schenk RK, et al. Biologic Width around one- and two-piece titanium implants. Clin Oral Implants Res. 2001;12(6):559-571.
29. Linkevicius T, Apse P. Biologic width around implants. An evidence-based review. Stomatologija. 2008;10(1):27-35.
30. Job S, Bhat V, Naidu EM. In vivo evaluation of crestal bone heights following implant placement with ‘flapless’ and ‘with-flap’ techniques in sites of immediately loaded implants. Indian J Dent Res. 2008;19(4):320-325.
31. Hermann JS, Cochran DL, Nummikoski PV, Buser D. Crestal bone changes around titanium implants. A radiographic evaluation of unloaded nonsubmerged and submerged implants in the canine mandible. J Periodontol. 1997;68(11):1117-1130.
32. Hermann JS, Schoolfield JD, Nummikoski PV, et al. Crestal bone changes around titanium implants: a methodologic study comparing linear radiographic with histometric measurements. Int J Oral Maxillofac Implants. 2001;16(4):475-485.
33. Hartman GA, Cochran DL. Initial implant position determines the magnitude of crestal bone remodeling. J Periodontol. 2004;75(4):572-577.
34. Bryant SR, Zarb GA. Crestal bone loss proximal to oral implants in older and younger adults. J Prosthet Dent. 2003;89(6):589-597.
35. Smith DE, Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent. 1989;62(5):567-572.
36. Weber HP, Crohin CC, Fiorellini JP. A 5-year prospective clinical and radiographic study of non-submerged dental implants. Clin Oral Implant Res. 2000;11(2):144-153.
37. Weber HP, Buser D, Fiorellini JP, Williams RC. Radiographic evaluation of crestal bone levels adjacent to nonsubmerged titanium implants. Clin Oral Implants Res. 1992;3(4):181-188.
38. Brägger U, Häfeli U, Huber B, et al. Evaluation of postsurgical crestal bone levels adjacent to non-submerged dental implants. Clin Oral Implants Res. 1998;9(4):218-224.
39. Gapski R, Wang HL, Mascarenhas P, Lang NP. Critical review of immediate implant loading. Clin Oral Implants Res. 2003;14(5):515-527.
40. Crespi R, Capparé P, Gherlone E, Romanos GE. Immediate versus delayed loading of dental implants placed in fresh extraction sockets in the maxillary esthetic zone: a clinical comparative study. Int J Oral Maxillofac Implants. 2008;23(4):753-758.
41. Esposito M, Grusovin MG, Coulthard P, Worthington HV. Different loading strategies of dental implants: a Cochrane systematic review of randomized controlled clinical trials. Eur J Oral Implantol. 2008;1(4):259-276.
42. Vignoletti F, de Sanctis M, Berglundh T, et al. Early healing of implants placed into fresh extraction sockets: an experimental study in the beagle dog. II: ridge alterations. J Clin Periodontol. 2009;36(8):688-697.
43. Schwartz-Arad D, Yaniv Y, Levin L, Kaffe I. A radiographic evaluation of cervical bone loss associated with immediate and delayed implants placed for fixed restorations in edentulous jaws. J Periodontol. 2004;75(5):652-657.
44. Vignoletti F, Discepoli N, Müller A, et al. Bone modelling at fresh extraction sockets: immediate implant placement versus spontaneous healing: an experimental study in the beagle dog. J Clin Periodontol. 2012;39(1):91-97.
45. Ferrus J, Cecchinato D, Pjetursson EB, et al. Factors influencing ridge alterations following immediate implant placement into extraction sockets. Clin Oral Implants Res. 2010;21(1):22-29.
46. Caneva M, Botticelli D, Salata LA, et al. Flap vs. “flapless” surgical approach at immediate implants: a histomorphometric study in dogs. Clin Oral Implants Res. 2010;21(12):1314-1319.
47. Collaert B, De Bruyn H. Immediate functional loading of TiOblast dental implants in full-arch edentulous maxillae: a 3-year prospective study. Clin Oral Implants Res. 2008;19(12):1254-1260.
48. Norton MR. A short-term clinical evaluation of immediately restored maxillary TiOblast single-tooth implants. Int J Oral Maxillofac Implants. 2004;19(2):274-281.
49. Ostman PO, Wennerberg A, Albrektsson T. Immediate occlusal loading of NanoTite PREVAIL implants: a prospective 1-year clinical and radiographic study. Clin Implant Dent Relat Res. 2010;12(1):39-47.
50. Galli F, Capelli M, Zuffetti F, et al. Immediate non-occlusal vs. early loading of dental implants in partially edentulous patients: a multicentre randomized clinical trial. Peri-implant bone and soft-tissue levels. Clin Oral Implants Res. 2008;19(6):546-552.
51. Liñares A, Mardas N, Dard M, Donos N. Effect of immediate or delayed loading following immediate placement of implants with a modified surface. Clin Oral Implants Res. 2011;22(1):38-46.
52. Younis L, Taher A, Abu-Hassan MI, Tin O. Evaluation of bone healing following immediate and delayed dental implant placement. J Contemp Dent Pract. 2009;10(4):35-42.
53. Lambert PM, Morris HF, Ochi S. Positive effect of surgical experience with implants on second-stage implant survival. J Oral Maxillofac Surg. 1997;55(12 suppl 5):12-18.
54. Cavallaro JS Jr. Implant survival and radiographic analysis of proximal bone levels surrounding a contemporary dental implant. Implant Dent. 2011;20(2):146-156.
55. Pylant T, Triplett RG, Key MC, Brunsvold MA. A retrospective evaluation of endosseous titanium implants in the partially edentulous patient. Int J Oral Maxillofac Implants. 1992;7(2):195-202.
56. Henry PJ, Tolman DE, Bolender C. The applicability of osseointegrated implants in the treatment of partially edentulous patients: three-year results of a prospective multicenter study. Quintessence Int. 1993;24(2):123-129.
57. Wyatt C, Zarb GA. Bone level changes proximal to oral implants supporting fixed partial prostheses. Clin Oral Implants Res. 2002;13(2):162-168.
58. Adell R, Lekholm U, Rockler B, et al. Marginal tissue reactions at osseointegrated titanium fixtures (I). A 3-year longitudinal prospective study. Int J Oral Maxillofac Surg. 1986;15(1):39-52.
59. Cox JF. Zarb GA. The longitudinal clinical efficacy of osseointegrated dental implants: a 3-year report. Intl J Oral Maxillofac Implants. 1987;2(2):91-100.
60. Ahlqvist J, Borg K, Gunne J, et al. Osseointegrated implants in edentulous jaws: a 2-year longitudinal study. Intl J Oral Maxillofac Implants. 1990;5(2):155-163.
61. Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
62. Lekholm U, Adell R, Lindhe J, et al. Marginal tissue reactions at osseointegrated titanium fixtures. (II) A cross-sectional retrospective study. Int J Oral Maxillofac Surg. 1986;15(1):53-61.
63. Lindquist LW, Rockler B, Carlsson GE. Bone resorption around fixtures in edentulous patients treated with mandibular fixed tissue-integrated prostheses. J Prosthet Dent. 1988;59(1):59-63.
64. Chaytor DV, Zarb GA, Schmitt A, Lewis DW. The longitudinal effectiveness of osseointegrated dental implants. The Toronto Study: bone level changes. Int J Periodontics Restorative Dent. 1991;11(2):112-125.
65. Wennström JL, Ekestubbe A, Gröndahl K, et al. Oral rehabilitation with implant-supported fixed partial dentures in periodontitis-susceptible subjects. A 5-year prospective study. J Clin Periodontol. 2004;31(9):713-724.
66. Jacobs R, Schotte A, van Steenberghe D, et al. Posterior jaw bone resorption in osseointegrated implant-supported overdentures. Clin Oral Implants Res. 1992;3(2):63-70.
67. von Wowern N, Harder F, Hjørting-Hansen E, Gotfredsen K. ITI implants with overdentures: a prevention of bone loss in edentulous mandibles? Int J Oral Maxillofac Implants. 1990;5(2):135-139.
68. Wright PS, Glantz PO, Randow K, Watson RM. The effects of fixed and removable implant-stabilised prostheses on posterior mandibular residual ridge resorption. Clin Oral Implants Res. 2002;13(2):169-174.
69. Nakai H, Niimi A, Ueda M. Osseous proliferation of the mandible after placement of endosseous implants. Int J Oral Maxillofac Implants. 2000;15(3):419-424.
70. Blanes RJ, Bernard JP, Blanes ZM, Belser UC. A 10-year prospective study of ITI dental implants placed in the posterior region. I: Clinical and radiographic results. Clin Oral Implants Res. 2007;18(6):699-706.
71. Quirynen M, Naert I, van Steenberghe D. Fixture design and overload influence marginal bone loss and fixture success in the Brånemark system. Clin Oral Implants Res. 1992;3(3):104-111.
72. Buser D, Mericske-Stern R, Dula K, Lang NP. Clinical experience with one-stage, non-submerged dental implants. Adv Dent Res. 1999;13:153-161.
73. Brunski JB. In vivo bone response to biomechanical loading at the bone/dental-implant interface. Adv Dent Res. 1999;13:99-119.
74. Ma S, Payne AG. Marginal bone loss with mandibular two-implant overdentures using different loading protocols: a systematic literature review. Int J Prosthodont. 2010;23(2):117-126.
75. Cehreli MC, Karasoy D, Kökat AM, et al. A systematic review of marginal bone loss around implants retaining or supporting overdentures. Int J Oral Maxillofac Implants. 2010;25(2):266-277.
76. Slot W, Raghoebar GM, Vissink A, et al. A systematic review of implant-supported maxillary overdentures after a mean observation period of at least 1 year. J Clin Periodontol. 2010;37(1):98-110.
77. Quirynen M, Naert I, van Steenberghe D, et al. Periodontal aspects of osseointegrated fixtures supporting an overdenture. A 4-year retrospective study. J Clin Periodontol. 1991;18(10):719-728.
78. Jemt T, Chai J, Harnett J, et al. A 5-year prospective multicenter follow-up report on overdentures supported by osseointegrated implants. Int J Oral Maxillofac Implants. 1996;11(3):291-298.
79. van Steenberghe D, Quirynen M, Naert I, et al. Marginal bone loss around implants retaining hinging mandibular overdentures, at 4-, 8- and 12-years follow-up. J Clin Periodontol. 2001;28(7):628-633.
80. Ueda T, Kremer U, Katsoulis J, et al. Long-term results of mandibular implants supporting an overdenture: implant survival, failures, and crestal bone level changes. Int J Oral Maxillofac Implants. 2011;26(2):365-372.
81. Crum RJ, Rooney GE Jr. Alveolar bone loss in overdentures: a 5-year study. J Prosthet Dent. 1978;40(6):610-613.
82. Jacobs R, van Steenberghe D, Nys M, Naert I. Maxillary bone resorption in patients with mandibular implant-supported overdentures or fixed prostheses. J Prosthet Dent. 1993;70(2):135-140.
83. von Wowern N, Gotfredsen K. Implant-supported overdentures, a prevention of bone loss in edentulous mandibles? A 5-year follow-up study. Clin Oral Implants Res. 2001;12(1):19-25.
84. Attard NJ, Zarb GA. Long-term treatment outcomes in edentulous patients with implant overdentures: the Toronto study. Int J Prosthodont. 2004;17(4):425-433.
85. Attard NJ, Zarb GA. Long-term treatment outcomes in edentulous patients with implant-fixed prostheses: the Toronto study. Int J Prosthodont. 2004;17(4):417-424.
86. Aloy-Prósper A, Maestre-Ferrín L, Peñarrocha-Oltra D, Peñarrocha-Diago M. Marginal bone loss in relation to the implant neck surface: an update. Med Oral Patol Oral Cir Bucal. 2011;16(3):e365-e368.
87. Botos S, Yousef H, Zweig B, et al. The effects of laser microtexturing of the dental implant collar on crestal bone levels and peri-implant health. Int J Oral Maxillofac Implants. 2011;26(3):492-498.
88. Prasad DK, Shetty M, Bansal N, Hegde C. Crestal bone preservation: a review of different approaches for successful implant therapy. Indian J Dent Res. 2011;22(2):317-323.
89. Atieh MA, Ibrahim HM, Atieh AH. Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. J Periodontol. 2010;81(10):1350-1366.
90. Moy PK, Medina D, Shetty V, Aghaloo TL. Dental implant failure rates and associated risk factors. Int J Oral Maxillofac Implants. 2005;20(4):569-577.
91. Martin W, Lewis E, Nicol A. Local risk factors for implant therapy. Int J Oral Maxillofac Implants. 2009;24(suppl):28-38.
92. Shapoff CA, Lahey BJ. Crestal bone loss and the consequences of retained excess cement around dental implants. Compend Contin Educ Dent. 2012;33(2):94-101.
93. Safii SH, Palmer RM, Wilson RF. Risk of implant failure and marginal bone loss in subjects with a history of periodontitis: a systematic review and meta-analysis. Clin Implant Dent Relat Res. 2010;12(3):165-174.
94. Isidor F. Influence of forces on peri-implant bone. Clin Oral Implants Res. 2006;17(suppl 2):8-18.