You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Materials and techniques used for the fabrication of provisional (temporary) restorations for fixed prosthodontics have been evolving. For single crowns, clinicians have many choices when deciding what type of provisional crown they want to fabricate. The earliest provisional restorations for single crowns, made from both metal and plastics, were prefabricated and preformed by the manufacturer. They came in a variety of sizes and shapes, which could be selected based on the given clinical situation.1 As part of this evolution, directly manipulated acrylic resins and, later, composite resins were developed for routine use for both single-unit and multiple-unit restorations.2
Provisional restorations are a critical component of fixed prosthodontic treatment, biologically and biomechanically.3 These restorations are also referred to as temporary or interim, or treatment restorations. Because these restorations are fabricated to mimic the definitive restoration that will eventually be placed, they are also diagnostic in nature with regards to shape, size, contour, and esthetic appearance. Definitive crown and fixed partial denture (FPD) restorations are usually a multiple-dental-visit procedure which requires that the interim restoration mimic the planned final restoration independent of the restorative material(s) used for that restoration. A primary goal during delivery and cementation of the definitive restoration is minimal adjustment during insertion. By fabricating a durable, smooth, well-adapted, and well-fitting provisional restoration, chairtime during final restoration insertion can be optimized.
The Purpose of Provisional Restorations
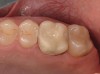
Provisional crown and FPD restorations play several key roles during the treatment process for the health of the tooth, periodontium, and pulp. They protect the underlying tooth preparation and pulp while the definitive restoration is being fabricated by the laboratory. This pulpal protection promotes pulpal healing after the trauma of tooth preparation. Also, a well-adapted and contoured provisional crown assures the return to health of any traumatized soft tissues during crown preparation and impression making by allowing patients to maintain their oral health in the area of the restoration (Figure 1).4 To allow for the maintenance of periodontal health for both natural teeth and implants, materials used for provisional restorations need to be smooth and not plaque-retentive.5-7
Temporary restorations are trial restorations to help determine the desired shape, size, contours, lengths, occlusion, esthetics, and speech during the fabrication of the definitive restoration.2,8 They are also diagnostic in that they provide critical information for the evaluation of adequate axial and occlusal clearance and reduction of the tooth preparation for the final restoration.4 The clinician can make an impression of the provisional to provide guidance in the fabrication of the definitive restoration. Provisional restorations also can provide important diagnostic information on occlusal relationships and tooth positions and changes desired. These provisional materials must be durable for the time required until final restoration fabrication. Also, once cemented for vital teeth, these restorations must provide thermal protection and seal the preparation, protecting the dentin from bacterial invasion and dentinal sensitivity.
Once in place, provisional restorations must be easy to remove without damaging the existing tooth preparation. Provisional restorations help maintain positional stability of the tooth preparations occlusally and proximally.3,9-11 Poorly adjusted provisional restorations can lead to tooth movement and shifting that can have a negative impact on the placement of the final restoration. Preparation/tooth movement will very likely necessitate additional chairtime to make any necessary adjustment of proximal contacts as well as occlusal adjustment during try-in before cementation of the definitive restoration returned by the dental laboratory. For FPDs, tooth movement can lead to changes in the path of insertion between abutments.
For clinicians, the fabrication of temporary restorations for a single crown requires proficiency with a variety of materials and techniques that can be used to make well-adapted and functional provisionals. There are many choices, including preformed/prefabricated metal crowns, polycarbonate crowns, celluloid crowns, composite resin crowns, acrylic resin for custom provisionals, bis-acryl or bis-GMA automix composite resin materials, and composite resin for custom fabrication.3,4,10-13 For multi-unit FPDs, the clinician has the choice of acrylic resins, bis-acryl, bis-GMA, or rubberized-urethane automix composite materials, or laboratory-fabricated resin shells.
Preformed Single-Unit Crowns
Preformed stock crowns refer to interim restorations that are commercially available through a variety of manufacturers as kits. These kits typically contain either anterior-premolar shells, posterior crown shells, or both. The sizes and shapes have been determined by the manufacturers to fulfill many clinical situations relating to different tooth dimensions, including facial-lingual and mesial-distal, and occlusal (or incisal) heights.
To fit these crowns, measurements should be made of the mesial-distal relationship within the arch of the tooth preparation, and the correct size then selected. These stock crowns usually fit poorly at the gingival margins and require adjustments for length and then relining with polymeric resins. After the resin has polymerized, the crowns can be shaped and contoured with disks or burs.
These preformed crowns can be made from aluminum, stainless steel, nickel-chromium, polycarbonate, polymethylmethacrylate (PMMA), and composite resins. Preformed crowns are generally used for single-tooth restorations and, at times, in an emergency situation when there is no time for planning for use of a custom-fabricated, resin-based restoration.1,10,11
Polymeric Resins
The most commonly used provisional restorative materials are polymeric resins. Polymeric resins can be divided into two subclasses: acrylic resin and composite resin. Provisional restorations can be fabricated with either of these two subclasses of resin during prosthodontic treatment using similar techniques.2
Acrylic Resin Provisional Materials
Acrylic resin is a very well-accepted restorative material for provisional restorations. While there are other acrylics, the two most commonly used are self-curing (autopolymerizing or cold cure) polymethylmethacrylate (PMMA) and polyethylmethacrylate (PEMA).10-12 Although these materials are tooth-colored and relatively inexpensive, they are difficult to manipulate and have poor physical properties.1,14
With acrylic resin, the fabrication of the provisional restoration usually requires mixing a powder and liquid together to form a paste, which is placed in either a premade shell, a template, or carrier that is placed over the tooth preparation. For these materials, it can be difficult to time the setting and working stages of the polymerization reaction of acrylics because of the inaccurate method of dispensing and mixing the polymer powder and liquid monomer. Acrylic resins have an unpleasant odor while setting.1,14-16 When the acrylic resin reaches a rubbery consistency, the carrier is removed with the acrylic resin from the tooth preparation so that the resin can achieve complete polymerization and hardening. Some clinicians re-seat the restoration on the preparation while the acrylic resin is setting by taking the temporary on and off the preparation to control the fitting of the restoration.
Other difficulties with acrylic resins include relatively high volumetric polymerization shrinkage and the generation of heat during polymerization. Care must be taken to avoid pulpal and gingival damage by removing the acrylic resin before excessive heat of polymerization occurs.11,12,17 Although hot water will accelerate the set of the resin, the hot water and heat of polymerization of the resin will cause the resin to shrink and distort at a greater rate.15 Room temperature water will equalize the heat of polymerization of the acrylic resin and minimize shrinkage.9,11,15 Also, acrylic resins on rare occasions can cause allergic hypersensitivity.18-20 These resins have a high coefficient of thermal expansion, low strength, and poor abrasion resistance to wear.14,15 For the short time period that these resins will be used, they are dimensionally stable and stain resistant.8,21,22 If used for extended periods of time, these resins will show significant wear in occlusal function, are susceptible to breakage, have poor fit, and can discolor over time.23,24
Many clinicians prefer acrylic resins for more complex cases, especially multi-unit, multi-pontic clinical situations in which long-term durability is required, as they have the ability to reline marginal areas and repair fractures.1,25,26 For long-span FPDs fabricated with acrylic resins, an increase in flexural strength and resistance to breakage can be attained through the use of fiber reinforcement embedded in the provisional material.27,28
Composite Resin Provisional Materials
In recent years, composite resin provisional materials have been introduced. These materials were developed to overcome some of the deficiencies of acrylic resin for interim crown restorations. The chemistry of these provisional composite resins is either bis-acryl, bis-GMA, or rubberized-urethane resins. Their setting reactions can be light-cure, self-cure (autocure), or dual-cure.
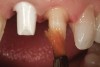
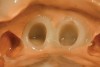
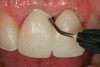
These composite resin provisional materials are easy to use; they dispense with a double-barrel tube configuration where the catalyst and base pastes are mixed in automixing tips. They are used with techniques similar to those used for acrylic resins (Figure 2 through Figure 6). These materials have improved physical properties and provide for a more predictable, easier fabrication of a provisional crown restoration.10,14-16,23,24,28,29 One problem with bis-acrylics is their brittle nature and potential for color changes.12,30,31 Rubberized-urethane resins have been introduced that have demonstrated increased flexural strength when compared to traditional bis-acryl composites.2,32 For FPDs, the flexural strength of composites can be increased significantly through the use of fiber reinforcement materials embedded in the restoration.28,33
Composite provisional materials typically have significantly less shrinkage than acrylic resin due to the presence of radiopaque glass fillers. The addition of fillers to the resin also improves the fit of the provisional restoration to the tooth preparation and improves the wear characteristics of the restoration in occlusal function.24,34
Bis-acryls and rubberized-urethane composites have a paste-paste formulation that undergoes a three-stage polymerization reaction. The first phase begins as a free-flowing paste that adapts to the tooth preparation and then becomes elastic within 60 to 75 seconds. The second phase, which takes place over the next 4 minutes, is a cross-linking polymerization reaction that enables the polymer to reach a high compressive strength. The final phase of polymerization allows the resin to reach its final hardness within 5 minutes after initial mixing so that the restoration can be adjusted and polished before cementation. Use of composite resin provisional materials requires less time than using acrylic resin.2
It has been reported that the composite resins used for provisional restorations have advantages over other resin-based provisional materials.2-4,15,23,24,27-29,35,36 These advantages include the following:
• Because it is a filled composite resin, it is harder, more resistant to dietary solvents, and more resistant to occlusal wear than unfilled acrylic resin
• Quick and easy to use; rapid setting capability enables it to be removed from the mouth after 75 to 90 seconds with less chance of causing thermal damage to the pulp and gingival tissues
• Flexible, making insertion and removal easier
• Minimal polymerization shrinkage and minimal heat of polymerization
• Radiopaque
• Easily repairable with a flowable composite resin37,38
• Excellent color stability and stain resistance
• Little odor when mixed
• Minimal polishing required when used with a resin glaze
Conclusion
Provisional or interim restorations are a key element of fixed prosthodontic treatment, both biologically and biomechanically.3 These restorations provide an important diagnostic function while in place, and they are critical in evaluating the physiologic position of the final restoration. In the esthetic zone, they are important in evaluating the esthetics for the definitive restoration. One can view the provisional restoration as a blueprint for the design of the definitive prosthesis.1
With many choices of materials available to use as interim restorations, it is important for clinicians to make their selection based upon the clinical needs for each situation. As part of these considerations, clinicians must understand and factor in the physical properties, handling characteristics, patient response to the appearance of the interim restoration, durability of the restoration, and the material cost in deciding which material to use. No one material meets all the requirements for provisional restorations. Selection of provisional materials should be made based upon a case-by-case evaluation for any given patient.
References
1. Gegauff AG, Holloway JA. Interim fixed restorations. In: Rosensteil SF, Land MF, Fujimoto J, eds. Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby Elsevier; 2006:466-504.
2. Strassler HE, Lowe RA. Chairside resin-based provisional restorative materials for fixed prosthodontics. Compend Contin Educ Dent. 2011;32(9):10-20.
3. Gratton DG, Aquilino SA. Interim restorations. Dent Clin North Am. 2004;48(2):487-497.
4. Strassler HE, Anolik C, Frey C. High-strength, aesthetic provisional restorations using a bis-acryl composite. Dent Today. 2007;26(11):128-133.
5. Maalhagh-Fard A, Wagner WC, Pink FE, Neme AM. Evaluation of surface finish and polish of eight provisional restorative materials using acrylic bur and abrasive disk with and without pumice. Oper Dent. 2003;28(6):734-739.
6. Buergers R, Rosentritt M, Handel G. Bacterial adhesion of Streptococcus mutans to provisional fixed prosthodontic material. J Prosthet Dent. 2007;98(6):461-469.
7. Davidi MP, Beyth N, Weiss EI, et al. Effect of liquid polish on in vitro biofilm accumulation on provisional restorations? Part 2. Quintessence Int. 2008;39(1):45-49.
8. Vahidi F. The provisional restoration. Dent Clin North Am. 1987;31(3):363-381.
9. Strassler HE. Provisional crown and bridge resin materials: an update. Maryland State Dental Association Journal. 1998;41(1):11-12.
10. Perry RD, Magnuson B. Provisional materials: key components of interim fixed restorations. Compend Contin Educ Dent. 2012;33(1):59-62.
11. Zinner ID, Trachtenberg DI, Miller Rd. Provisional restorations in fixed partial prosthodontics. Dent Clin North Am. 1989;33(3):355-377.
12. Lui JL, Setcos JC, Phillips RW. Temporary restorations: a review. Oper Dent. 1986;11(3):103-110.
13. Jones T, Karim N, Winters E, et al. A new temporary preformed curable crown material: mechanical properties [abstract]. J Dent Res. 2007;87(spec iss A). Abstract 130.
14. Powers JM. Composite restorative materials. In: Powers JM, Sakaguchi RL, eds. Craig’s Restorative Dental Materials. 12th ed. St Louis, MO: Mosby Elsevier; 2006:513-543.
15. Powers JM. Mechanical properties. In: Powers JM, Sakaguchi RL, eds. Craig’s Restorative Dental Materials. 12th ed. St Louis, MO: Mosby Elsevier; 2006:51-96.
16. Driscoll CF, Woolsey G, Ferguson WM. Comparison of exothermic release during polymerization of four materials used to fabricate interim restorations. J Prosthet Dent. 1991;65(4):504-506.
17. Altintas SH, Yondem I, Tak O, Usumez A. Temperature rise during polymerization of three different provisional materials. Clin Oral Investig. 2008;12(3):283-286.
18. Giunta J, Zablotsky N. Allergic stomatitis caused by self-polymerizing resin. Oral Surg Oral Med Oral Pathol. 1976;41(5):631-637.
19. Stugis TE, Fink JN. Hypersensitivity to acrylic resin. J Prosthet Dent. 1969;22(4):425-428.
20. Kanerva L, Estlander T, Jolanki R. Allergy caused by acrylics: past, present and prevention. Curr Probl Dermatol. 1996;25:86-96.
21. Givens EJ Jr, Neiva G, Yaman P, Dennison JB. Marginal adaptation and color stability of four provisional materials. J Prosthodont. 2008;17(2):97-101.
22. Koumjian JH, Firtell DN, Nimmo A. Color stability of provisional materials in vivo. J Prosthet Dent. 1991;65(6):740-742.
23. Sham AS, Chu FC, Chai J, Chow TW. Color stability of provisional prosthodontic materials. J Prosthet Dent. 2004;91(5):447-452.
24. Young HM, Smith CT, Morton d. Comparative in vitro evaluation of two provisional restorative materials. J Prosthet Dent. 2001;85(2):129-132.
25. Lodding DW. Long-term esthetic provisional restorations in dentistry. Curr Opin Cosmet Dent. 1997;4:16-21.
26. Emtiaz S, Tarnow DP. Processed acrylic resin provisional restoration with lingual cast metal framework. J Prosthet Dent. 1998;79(4):484-488.
27. Saygili G, Sahmali SM, Demirel F. The effect of glass fibers and aramid fibers on the fracture resistance of provisional restorative materials. Oper Dent. 2003;28(1):80-85.
28. Hamza TA, Rosenstiel SF, Elhosary MM, Ibraheem RM. The effect of fiber reinforcement on the fracture toughness and flexural strength of provisional restorative resins. J Prosthet Dent. 2004;91(3):258-264.
29. Yap AU, Mah MK, Lye CP, Loh PL. Influence of dietary simulating solvents on the hardness of provisional restorative materials. Dent Mater. 2004;20(4):370-376.
30. Yilmaz A, Baydas S. Fracture resistance of various temporary crown materials. J Contemp Dent Pract. 2007;8(1):44-51.
31. Rutkunas V, Sabaliasuskas V, Mizutani H. Effects of different food colorants and polishing techniques on color stability of provisional prosthetic materials. Dent Mater J. 2010;29(2):167-176.
32. Levine E, Hack G, Prymas S. Using biomaterial investigative skills to assist in the clinical decision making process [abstract]. J Dent Educ. 2011;75(2):190-256. Abstract 117.
33. Karbhari VM, Strassler H. Effect of fiber architecture on flexural characteristics and fracture of fiber-reinforced dental composites. Dent Mater. 2007;23(8):960-968.
34. Powers JM. Resin composite restorative materials. In: Powers JM, Sakaguchi RL, eds. Craig’s Restorative Dental Materials. 12th ed. St Louis, MO: Mosby Elsevier; 2006:189-212.
35. Akova T, Ozkomur A, Uysal H. Effect of food-stimulating liquids on the mechanical properties of provisional restorative materials. Dent Mater. 2006;12(1):1130-1134.
36. Yilmaz A, Baydas S. Fracture resistance of various temporary crown materials. J Contemp Dent Pract. 2007;8(1):44-51.
37. Bohnenkamp DM, Garcia LT. Repair of bis-acryl provisional restorations using flowable composite resin. J Prosthet Dent. 2004;92(5):500-502.
38. Hagge MS, Lindemuth JS, Jones AG. Shear bond strength of bis-acryl composite provisional material repaired with flowable composite. J Esthet Restor Dent. 2002;14(1):47-52.
About the Author
Howard E. Strassler, DMD
Professor, Director of Operative Dentistry
Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland