You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Scientific literature on sleep disorders suggests that patients may be diagnosed when they are young, as early as adolescence.1 However, dental professionals are not always in agreement regarding the tools to implement for diagnosis, such as cone-beam computed tomography (CBCT). Opinions are divided regarding the reliability of detecting sleep disorders by using CBCT to conduct upper-airway analysis, diagnosis, and treatment planning. Accepting the use of CBCT depends on the knowledge of the individual clinician. CBCT scans provide accurate static images of airways; however, clinicians should also include dynamic assessments. The static CBCT images focus on the well-defined bony and soft-tissue relationships; they also quantify tongue position, mandibular configuration, hyoid-to-mandible relationship, and airway obstruction/narrowing. Upper-airway analysis with CBCT images may also reveal missing adult dentition, airway morphology, smaller pharyngeal volume with smaller cross-sectional area, tongue position relative to the palate, shorter mandibular length, and flatter mandibles. Hence, CBCT, a radiographic imaging method that allows 3-dimensional (3D) imaging of hard-tissue structures, has been introduced as an effective diagnosis method to evaluate upper airways.2-5
Missing Teeth and Sleep Apnea
Missing teeth in early childhood can result in abnormal facial morphology with a narrow upper airway.6 Dental agenesis, which is the manifestation of missing permanent teeth, is the most prevalent craniofacial anomaly in humans.7 The potential association between dental agenesis or early dental extractions and the presence of OSA has been investigated.6 OSA causes breathing to repeatedly stop and start during sleep; this type of apnea occurs when the throat muscles intermittently relax and block the airway. A noticeable sign of OSA is snoring. OSA is characterized by upper airway collapsibility, repetitive pharyngeal collapse during sleep. Therefore, one variable used in describing the mechanics of the upper airway is to measure its propensity for collapse.8
A study was conducted of 31 children with dental agenesis and 11 children with early dental extractions who had at least two permanent teeth missing.6 All children with missing teeth had identifiable clinical signs of OSA. There was a significant difference in mean apnea-hypopnea indices (AHI) in the agenesis, dental extraction, and tonsillo-adenoid studied groups, with mean abnormal AHI lowest in the pediatric dental agenesis group. In the children with missing teeth, aging was associated with the presence of a higher AHI. When a child has dental agenesis or early extractions, over time a breathing pattern develops due to alveolar bone growth in the absence of teeth. Alveolar bone growth is dependent on the presence of the teeth that it supports. Children with permanent teeth missing due to congenital agenesis or permanent teeth extraction have smaller oral cavities. Patients with smaller oral cavities are predisposed to collapse of the upper airway during sleep and present with OSA symptoms as they mature.9 Parents of these children often do not recognize these symptoms due to the low-grade initial symptomatology. Daytime mouth breathing and sleep-disordered breathing, if left untreated for a prolonged period, suggest that worsening symptoms will occur over time.6
Sleep disturbances in general and OSA in particular are related to other health conditions, such as cardiovascular disease, type 1 and type 2 diabetes, hyperinsulinemia, dementia, hypertension, migraines, and weight gain, the latter due to increases in cortisol and insulin hormone levels and decreases in human growth hormone (reducing lean muscle mass and forcing fat to be stored as energy, resulting in weight gain).10 To identify potential OSA patients during adolescence, CBCT examinations can help evaluate airway volume, soft-palate area, and soft-tissue thicknesses that can be measured before and after rapid maxillary expansion. Rapid maxillary expansion causes significant increases in nasal cavity volume, nasopharynx volume, anterior and posterior (A-P) facial heights, and palatal and mandibular planes.11
CBCT Images and Diagnostic Information
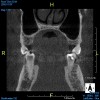
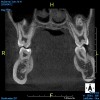
The morphology of the airway can be evaluated with CBCT images. Understanding the length and width of the upper airway is important to assess the pathology and the physiology of OSA and deliver the appropriate treatment therapies that best fit the patient's needs and predict effectiveness of the treatment. Wider and shorter upper airways display less airway resistance than narrow and long upper airways, which have an increase in airway resistance. Increase in airway resistance evokes inflammation of the airway, creating more inflammation and, therefore, increasing the severity of OSA. Figure 1 and Figure 2 display different morphologies in airways, as shown through CBCT imaging.9
Using CBCT with a patient in a sitting position has been a topic of discussion because changes in posture can create an obstructed airway that differs from the position of the airway when the patient is in a sleeping position. Because a CBCT image is static, when obtaining the image, the teeth should remain in occlusion to prevent posterior movement of the mandible and surrounding soft tissues (tongue, nasopharynx, oropharynx, and hypopharynx). Figure 3 shows a narrow upper airway of a patient in a sitting position demonstrating an airway obstruction. When the patient is in a sleeping position, the obstruction is more pronounced (Figure 4).
Additional information gathered from the CBCT images shows the distinct airway divisions, tongue size/position, and relative hyoid position, all critical in developing a diagnosis and a decision to refer to a physician to begin the process of either clinical or home sleep studies. The sleep study provides the physician with information regarding sleep disturbances and how these disturbances may potentially lead to overall diminishing health, fatigue, and metabolic disturbances. After a diagnosis has been confirmed, the physician is able to discuss therapies that best suit the needs and compliance considerations of the patient. If the physician determines that the patient will not benefit from continuous positive airway pressure (CPAP) or bilevel positive airway pressure (BiPAP) due to lack of compliance or claustrophobia, then the patient has an option to be referred to a dentist who is well versed and trained in providing OSA oral appliance therapy (OAT).12
Finally, the patient is evaluated face to face in the dental practice for medical history review, dynamic evaluations within the temporomandibular joint (TMJ) assemblies, thorough periodontal review, caries risk assessment, and overall satisfactory condition that allows for a stable sleep oral appliance. Scheduled follow-ups should be discussed after the seating of the OAT in the following intervals for the first year: 1 week, 3 weeks, 6 weeks, 3 months, 6 months, and 1 year.13 The patient should return to the referring physician for evaluation of sleep pattern and well checks.
Familial Case of Dental Agenesis
Four brothers with dental agenesis are currently being evaluated and treated by the author with CBCT imaging and digital treatment planning to regain their dentition. Developing arch form and palatal positioning by using CBCT imaging and digital software is critical. Much is learned from evaluating CBCT images and the advancement of virtual implant therapies. Combined with durable medical equipment and orthopedic/mandibular repositioning appliances, normal daytime breathing and normal sleep breathing patterns can be achieved through surgical dental implant services, orthodontic services, and long-term dental restorations that reposition the mandible and create a comfortable tongue position within the oral cavity. In the author's experience, CBCT in these situations provides a considerable amount of diagnostic information, improves quality of life, and improves the opportunity to enjoy a healthier lifestyle without the previously mentioned diseases of civilization.
Figure 5 through Figure 12 exemplify what currently may present in private dental practices with these types of patients. Four brothers aged 14 years to 27 years all suffered from obstructed airways; high incidence of caries of dentin, enamel, and cementum; moderate periodontal disease; collapsed vertical; undiagnosed OSA; and the potential for increase in comorbidities such as diabetes, cardiovascular disease, dementia, cancer, high blood pressure, and others. Symptomology was presented throughout the young lives of the brothers in this family. The parents were unaware that the dental agenesis and premature permanent tooth extraction could have led their sons into severe health issues as they matured.
Swift intervention took place with caries control, periodontal care, orthodontic evaluation for arch form development to aid in the development of facial bones and creating an improved upper airway with nasal patency. These interventions were followed up with definitive implant therapies and rapidly advancing restorative technology and materials. Thus, not only were these young men's smiles restored, they also were provided with the opportunity to regain their dignity when they become confident with their new smiles.
Conclusion
CBCT imaging is a tool that is recommended for use in investigating the dimensions of upper airways and contributing to the diagnosis of possible upper-airway obstructions.2-5 The 3D scan measurements of CBCT can be helpful in evaluating upper-airway patency in patients suspected to be suffering with sleep disorders. The upper airway is the final common pathway for abnormalities in respiratory control and neuromuscular function leading to sleep apnea. Patients with OSA have a smaller upper airway compared with other individuals, with the exception of airway length.4 The lack of a significant difference in the average A-P distance indicates that patient position during imaging (vertical versus horizontal) can affect this measurement. However, if there is a visible decrease in upper airway with the patient in a sitting position during imaging, then one can be certain there is a high potential for this patient to show signs of OSA while in a sleeping position.14 CBCT imaging is rapidly evolving to the point where it is difficult to keep up with the technological advancements. CBCT imaging provides the clinician with many measurements and quantifying information regarding congenital dental agenesis, premature dental extraction, tongue position, mandible position, and relative hyoid position, ultimately providing the information required for diagnosis.
About the Author
Thomas M. Bilski, DDS
Co-Director, Midwest Implant Institute
Columbus, Ohio
Private Practice
Independence, Ohio
References
1. Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9):1217-1239.
2. Kumar M, Shanavas M, Sidappa A, Kiran M. Cone beam computed tomography - know its secrets. J Int Oral Health. 2015;7(2):64-68.
3. Aboudara C, Nielsen I, Huang JC, et al. Comparison of airway space with conventional lateral headfilms and 3-dimensional reconstruction from cone-beam computed tomography. Am J Orthod Dentofacial Orthop. 2009;135(4):468-479.
4. Hatcher DC. Cone beam computed tomography: craniofacial and airway analysis. Dent Clin North Am. 2012;56(2):343-357.
5. Lenza MG, Lenza MM, Dalstra M, et al. An analysis of different approaches to the assessment of upper airway morphology: a CBCT study. Orthod Craniofac Res. 2010;13(2):96-105.
6. Guilleminault C, Abad VC, Chiu HY, et al. Missing teeth and pediatric obstructive sleep apnea. Sleep Breath. 2016;20(2):561-568.
7. Shimizu T, Maeda T. Prevalence and genetic basis of tooth agenesis. Jpn Dent Sci Rev. 2009:52-58.
8. Malhotra A, Pillar G, Fogel R, et al. Upper-airway collapsibility: measurements and sleep effects. Chest. 2001;120(1):156-161.
9. Rivlin J, Hoffstein V, Kalbfleisch J, et al. Upper airway morphology in patients with idiopathic obstructive sleep apnea. Am Rev Respir Dis. 1984;129(3):355-360.
10. Mesarwi O, Polak J, Jun J, Polotsky VY. Sleep disorders and the development of insulin resistance and obesity. Endocrinol Metab Clin North Am. 2013;42(3):617-634.
11. Smith T, Ghoneima A, Stewart K. Three-dimensional computed tomography analysis of airway volume changes after rapid maxillary expansion. Am J Orthod Dentofacial Orthop. 2012;141(5):618-626.
12. Mohsenin N, Mostofi MT, Mohsenin V. The role of oral appliances in treating obstructive sleep apnea. J Am Dent Assoc. 2003;134(4):442-449.
13. Silverman L, Razavi M. Seven appointment protocol for OSA treatment. Sleep 101 dental sleep medical model. June 24-25, 2013.
14. Baik UB, Suzuki M, Ikeda K, et al. Relationship between cephalometric characteristics and obstructive sites in obstructive sleep apnea syndrome. Angle Orthod. 2002;72(2):124-134.