You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Considerable research and product development in implant dentistry is focused on preventing crestal bone loss.1-3 Although a small amount of crestal bone remodeling around implants has been considered normal in the past,4 more significant amounts of bone loss can lead to a variety of negative consequences.5 The greater the degree of bone loss, the more severe the consequences can become.6 While most of the causes of bone loss around implants are biologic in nature,7 there are also iatrogenic causes. One of these causes is retained excess cement, which has been the subject of several articles in the dental literature.6,8,9
In the past, crestal bone loss of 1.5 mm to 2 mm has been considered "normal" during the first year after restorative loading. This bone loss often corresponded to the first thread below the implant collar. Annual bone loss < 0.1 mm in subsequent years was also considered acceptable.4,10,11 This bone loss is often attributed to the establishment of a "biologic width" around dental implants.3 Bone loss beyond these levels is considered pathologic.4
Numerous theories may account for bone loss noted after dental implant placement. Gingival inflammation around an implant can result in bone loss, referred to as peri-implantitis.12 Excessive occlusal forces on an implant restoration can result in advanced bone loss and even implant failure.13 Endodontic infections on adjacent teeth can spread and destroy bone around dental implants.14
Crestal bone levels around dental implants are important to their long-term success. The more bone loss around an implant, the less bone-to-implant contact (BIC) there is to support a restoration. In addition, bone loss can result in deeper probing depths around an implant, making oral hygiene difficult.15,16 Soft-tissue esthetics around the restoration, much like around natural teeth, depend on the height of the crestal bone.17 Therefore, while a small amount of crestal bone loss may occur around a dental implant restoration during the first year, every effort should be made to keep it to a minimum.18
Recent modifications to implant and abutment design have been shown to minimize crestal bone loss. Platform switching and abutment connection design have been reported to reduce crestal bone loss.19,20 More significantly, implants designed with microchannels (8 μm to 12 μm) on the implant platform and certain abutments have shown a fibrous connection to the nano-featured collar.21,22 This technology results in reduced sulcular depth23 and blocked epithelial downgrowth along the abutment or implant surface21,22 as well as reduced crestal bone loss.23-25
Despite these recent technological advances in implant design, retained cement around dental implant restorations can still cause significant crestal bone loss,8 gingival inflammation, and suppuration, and, in the process, create problems for the patient, restorative dentist, and implant surgeon.26 Wilson noted an 81% correlation to the presence of excess cement and continued sulcular bleeding or suppuration.8 The clinical significance of cement peri-implantitis is crestal bone loss, loss of gingival support, and potential acute abscess, which may put the survival of the implant and restoration at risk. As cement-retained restorations have become the method of choice for securing implant crowns, the incidence of this type of peri-implant bone loss has increased.
Implant restorations are either screw-retained or cemented, and each technique has its advantages and disadvantages. Studies of screw-retained restorations demonstrate a more precise fit to the abutment margin.27,28 Disadvantages of this connection type include screw loosening,29 less-than-optimal esthetics, and a lack of passivity of fit.30 Cement-retained crowns addressed these drawbacks29 and have now become the connection of choice especially in the esthetic zone. The advantages of cement-retained crowns include better esthetics, more natural contours of anterior restorations, and intact porcelain on the occlusal surfaces. Cement-retained restorations are not without drawbacks of their own. Removing the restoration intact once cemented is more difficult compared to screw-retained restorations.29 In addition, the larger marginal gap discrepancy between a cemented restoration and abutment can make it easier for bacteria to colonize in that area.31 The more destructive drawback is the potential for retained cement around the restorative margin.26 This article discusses the predisposing factors that lead to retained cement and clinical strategies to minimize or prevent cement peri-implantitis.
Predisposing Factors Leading to Cement Retention
Connection
The connection of soft tissue to a dental implant is different than to a natural tooth. Natural teeth have an epithelial hemidesmosomal adhesion and true connective tissue attachment through Sharpey's fibers inserted into the cementum. Connection of soft tissue to most dental implants is through an epithelial hemidesmosomal adhesion with collagen fibers arranged in a circular parallel pattern around the implant collar. This same unattached circular arrangement of connective tissue is also found on zirconia abutments.32 This attachment mechanism may be less resistant than the attachment of a natural tooth. In contrast, the aforementioned implants featuring microchannels (8 μm to 12 μm) have been reported to have a functional perpendicular connective tissue attachment to the microengineered 8-μm to 12-μm grooves placed on the implant collar and specific abutments.21,22 While this tissue attachment may be similar to a natural tooth, it may not be more protective against the pathologic changes associated with excess cement retention.
Placement
Exposed restorative margins on dental implant crowns are often much more problematic than those on natural teeth. Implant abutments, especially in the maxillary anterior, are often custom made and cannot just be reprepared and impressed for a new crown. Because material and laboratory costs are often greater for implant restorations than those on natural teeth, the financial hardship of a failed restoration is often greater with implants. These factors, as well as factors related to implant design, may result in the restorative margin being placed more subgingival, especially in the maxillary anterior.33 Implants in the esthetic zone, where bone and soft tissue often can be thin, are susceptible to collar exposure from gingival recession. In addition, inadequate bone dimension can lead to less-than-optimal positioning of the implant. To guard against collar exposure from bone loss, the surgeon may place the implant too far apically, resulting in a deep subgingival tissue cuff.
Abutment Selection
If a stock abutment with a fixed restorative margin 2 mm to 3 mm above the implant collar is used, or if a one-piece implant with a built-in restorative margin is used, the potential for excess cement removal is made more difficult in this deep tissue cuff.29,33 A recent article by Callan and Cobb9 showed that retained cement around implant crowns drastically increases the bacterial load and inflammatory response in the area. Several articles have reported cases of retained cement leading to gingival inflammation, suppuration, and crestal bone destruction.6,8,26 One article reported actual implant failure associated with retained cement.6 Even in cases with less severe consequences than implant failure, additional costly regenerative procedures may be necessary to repair the damage.
Radiographs
It may be commonplace to take a check radiograph at the time of abutment connection to assess proper placement; however, a final radiograph after cementation may not be taken. Radiographs may not even show the presence of retained cement.
Cementation Issues
The amount and type of restorative cement will influence the potential for excess cement retention as will the cementation technique used by different clinicians.
Maintenance
Periodic maintenance of the dental implant restoration is as important as maintenance of a natural tooth. Once restored, dental implant restorations resemble adjacent restored natural teeth but require different parameters of re-evaluation.
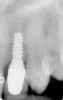
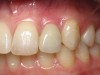
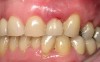
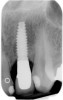
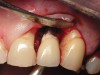
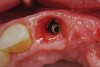
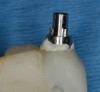
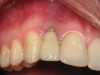
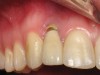
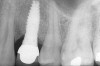
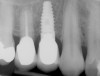
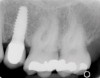
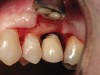
Figure 1 through Figure 13 depict examples of implant restorations in which retained cement caused periodontal inflammation and crestal bone loss requiring surgical intervention for debridement and repair of the damage.
Discussion
Avoiding deep subgingival restorative margins may be the best way to prevent retained cement that results in a destructive inflammatory process. Recognizing the predisposing factors that can lead to excessive retained cement is the best method of prevention. Radiographs taken after the crown is cemented may identify retained cement before destructive pathologic processes occur. Another method of prevention can be accomplished by the implant surgeon through precise site preparation and implant positioning. It is recommended that a clinical protocol should include a reduced amount of cement, cement with thinner film thickness, and cementation technique utilizing an abutment analog. Another recommendation would be to incorporate petroleum jelly in the cement to facilitate easier removal of cemented crowns and cement clean-up. Finally, the use of custom abutments that allow for shallow marginal placement with a more physiologic contour will assist the restorative dentist in cement removal.
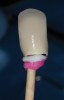
There have been a few articles in the literature that describe techniques for limiting excess cement. One common theme in these technique articles is to limit the amount of cement in the restoration by a trial run with a "practice abutment" (Figure 14 through Figure 16).33,34 Another technique described by Wolfart and coworkers35 limited the quantity of cement by only filling the occlusal half of the crown with cement before delivery. The potential concern with these techniques is delivering an inadequate amount of cement for retention. A recent study by Santosa and colleagues36 showed that while this was a concern with temporary cement, it was less of a concern when a permanent resin-modified glass-ionomer (RMGI) cement was used.
Other articles have described a technique in which a venting hole is fabricated on either the occlusal or lingual aspect of the permanent restoration.37 The disadvantage of this technique is the additional laboratory work involved and the necessity of filling the access hole after permanent cementation.
The limitations of these articles are that, with the exception of the in vitro study by Santosa and colleagues,36 they are technique articles without any clinical evaluation of their effectiveness. Thus, while using a venting or practice abutment cementation technique makes sense intuitively, it is difficult for a clinician to make an evidence-based decision on how to properly cement implant restorations.
Research on the type of cement that should be used for implant restorations has focused more on retentive strength, and whether that is desirable or not. Some studies have advocated a less-retentive cement to allow retrievability of the restoration. Very few studies have looked at which cements might be more likely to result in retained cement after delivery of the restoration. Agar and coworkers38 found that resin cements were more difficult to remove in a simulated subgingival environment. A recent survey of cementation protocols for implant restorations in US dental schools found that RMGI luting agents were the most commonly used.39 However, the authors suggested that the choice seemed to be based more on convenience and familiarity with that particular cement rather than a literature-based decision.
Various articles have discussed the film thickness of various luting agents.40,41 The thicker the luting agent, the greater the risk of poor marginal adaptation of the crown margin to the abutment. Wadhwani and colleagues42 investigated the radiographic density of eight different cements used for implant prostheses. They concluded that some of the cements commonly used for the cementation of implant-supported prostheses have poor radiodensity and may not be detectable after radiographic examination.
Once the restoration has been cemented, the clinician will try to detect and remove any excess cement. Most clinicians will attempt to do this clinically by exploring subgingivally with an instrument. Agar and coworkers38 discussed avoiding metal scalers and explorers because of the potential for scratching of the abutment or implant surface. They advocated the use of plastic instruments.
Maintenance of the dental implant restoration should be accomplished on a periodic basis. Office protocol should include visual inspection of soft tissues for color changes around the implant restorations, checking for bleeding on probing, and yearly or biyearly radiographic evaluation as well as monitoring of occlusal forces. Comparison of serial yearly radiographs may demonstrate crestal bone level changes, which can be a result of bacterial infection, retained cement, or occlusal overload. Follow-up of the final restoration at a 1- to 2-month time period would also allow for the evaluation of possible retained cement by monitoring the gingival response to the restoration or detection on a radiograph. Color changes of marginal gingiva, bleeding upon light probing with plastic probes, or evidence of suppuration may alert the clinician to the possibility of retained excess cement. Wilson demonstrated that suppuration or continued bleeding on probing around the gingival margins of implant restorations had an 81% correlation to the presence of excess cement.8 The shared maintenance responsibility between the restorative dentist and the implant surgeon must include clinical gingival inspection, radiographic comparison, monitoring occlusal forces to prevent occlusal overload issues, and considering pathologic changes from retained excess cement.
Conclusion
The destructive nature of retained excess cement has been reported in the literature and, unfortunately, is a frequent problem that requires recognition and management. Predisposing factors that can lead to retained excess cement have been reviewed and office protocol strategies have been discussed. Early recognition is advantageous to prevent destructive changes to the peri-implant soft and hard tissues. Ideally, establishing an office protocol of abutment design, cementation technique, and reassessment procedures would be beneficial in preventing or minimizing the problem. Evidence of retained cement issues on dental implants have been demonstrated in the case reports.
References
1. Weiner S, Simon J, Ehrenberg DS, et al. The effects of laser microtextured collars upon crestal bone levels of dental implants. Implant Dent. 2008;17(2):217-228.
2. Prosper L, Redaelli S, Pasi M, et al. A randomized prospective multicenter trial evaluating the platform-switching technique for the prevention of post restoration crestal bone loss. Int J Oral Maxillofac Implants. 2009;24(2):299-308.
3. Hermann JS, Schoolfield JD, Schenk RK, et al. Influence of the size of the microgap on crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged implants in the canine mandible. J Periodontol. 2001;72(10):1372-1383.
4. Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
5. Tabanella G, Nowzari H, Slots J. Clinical and microbiological determinants of ailing dental implants. Clin Implant Dent Relat Res. 2009;11(1):24-36.
6. Gapski R, Neugeboren N, Pomeranz AZ, Reissner MW. Endosseous implant failure influenced by crown cementation: a clinical case report. Int J Oral Maxillofac Implants. 2008;23(5):943-946.
7. Oh TJ, Yoon J, Misch CE, Wang HL. The causes of early implant bone loss: myth or science? J Periodontol. 2002;73(3):322-333.
8. Wilson TG. The positive relationship between excess cement and peri-implant disease: A prospective clinical endoscopic study. J Periodontol. 2009;80(9):1388-1392.
9. Callan DP, Cobb CM. Excess cement and peri-implant disease. Journal of Implant and Advanced Clinical Dentistry. 2009;1(6):61-68.
10. Smith DE , Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent. 1989;62(5):567-572.
11. Roos J, Sennerby L, Lekholm U, et al. A qualitative and quantitative method for evaluating implant success: a 5-year retrospective analysis of the Brånemark implant. Int J Oral Maxillofac Implants. 1997;12(4):504-514.
12. Fransson C, Wennström J, Tomasi C, Berglundh T. Extent of peri-implantitis-associated bone loss. J Clin Periodontol. 2009;36(4): 357-363.
13. Misch CE, Suzuki JB, Misch-Dietsh FM, Bidez MW. A positive correlation between occlusal trauma and peri-implant bone loss: literature support. Implant Dent. 2005;14(2):108-116.
14. Sussman HI. Endodontic pathology leading to implant failure—a case report. J Oral Implantol. 1997;23(3):112-116.
15. Quirynen M, Papaioannou W, van Steenberghe D. Intraoral transmission and the colonization of oral hard surfaces. J Periodontol. 1996;67(10):986-993.
16. Tanner A, Maiden MF, Lee K, et al. Dental implant infections. Clin Infect Dis. 1997;25(suppl 2):S213-S217.
17. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
18. Laurell L, Lundgren D. Marginal bone level changes at dental implants after 5 years in function: a meta-analysis. Clin Implant Dent Relat Res. 2009;13(1):19-28.
19. Herman JS, Buser D, Schenk RK, et al. Biologic Width around one- and two-piece titanium implants. Clin Oral Implants Res. 2001;12(6):559-571.
20. Cappiello M, Luongo R, Di lorio D, et al. Evaluation of peri-implant bone loss around platform-switched implants. Int J Periodontics Restorative Dent. 2008;28(4):347-355.
21. Nevins M, Nevins ML, Camelo M, et al. Human histologic evidence of a connective tissue attachment to a dental implant. Int J Periodontics Restorative Dent. 2008;28(2):111-121.
22. Nevins M, Kim DM, Jun SH, et al. Histologic evidence of a connective tissue attachment to laser microgrooved abutments: a canine study. Int J Periodontics Restorative Dent. 2010;30(3):245-255.
23. Pecora GE, Ceccarelli R, Bonelli M, et al. Clinical evaluation of laser-microtexturing for soft tissue and bone attachment to dental implants. Implant Dent. 2009:18(1):57-66.
24. Weiner S, Simon J, Ehrenberg DS, et al. The effects of laser microtextured collars upon crestal bone levels of dental implants. Implant Dent. 2008;17(2):217-228.
25. Shapoff CA, Lahey B, Wasserlauf PA, Kim DM. Radiographic analysis of crestal bone levels around Laser-Lok collar dental implants. Int J Periodontics Restorative Dent. 2010;30(2):129-137.
26. Pauletto N, Lahiffe BJ, Walton JN. Complications associated with excess cement around crowns on osseointegrated implants: A clinical report. Int J Oral Maxillofac Implants. 1999;14(6):865-868.
27. Keith SE, Miller BH, Woody RD, Higginbottom FL. Marginal discrepancy of screw-retained and cemented metal-ceramic crowns on implant abutments. Int J Oral Maxillofac Implants. 1999;14(3):369-378.
28. Guichet DL, Caputo AA, Choi H, Sorensen JA. Passivity of fit and marginal opening in screw- or cement-retained implant fixed partial denture designs. Int J Oral Maxillofac Implants. 2000;15(2):239-246.
29. Michalakis KX, Hirayama H, Garefis PD. Cement-retained versus screw-retained implant restorations: a critical review. Int J Oral Maxillofac Implants. 2003;18(5):719-728.
30. Lee A, Okayasu K, Wang HL. Screw- versus cement-retained implant restorations: current concepts. Implant Dent. 2010;19(1):8-15.
31. Quirynen M, van Steenberghe D. Bacterial colonization of the internal part of two-stage implants. An in vivo study. Clin Oral Implants Res. 1993;4(3):158-161.
32. Tetè S, Mastrangelo F, Bianchi A, et al. Collagen fiber orientation around machined titanium and zirconia dental implant necks: an animal study. Int J Oral Maxillofac Implants. 2009;24(1):52-58.
33. Dumbrigue HB, Abanomi AA, Cheng LL. Techniques to minimize excess luting agent in cement-retained implant restorations. J Prosthet Dent. 2002;87(1):112-114.
34. Wadhwani C, Piñeyro A. Technique for controlling the cement for an implant crown. J Prosthet Dent. 2009;102(1):57-58.
35. Wolfart M, Wolfart S, Kern M. Retention forces and seating discrepancies of implant-retained castings after cementation. Int J Oral Maxillofac Implants. 2006;21(4):519-525.
36. Santosa RE, Martin W, Morton D. Effects of a cementing technique in addition to luting agent on the uniaxial retention force of a single tooth implant supported restoration: an in vitro study. Int J Oral Maxillofac Implants. 2010;25(6):1145-1152.
37. Schwedhelm ER, Lepe X, Aw TC. A crown venting technique for the cementation of implant-supported crowns. J Prosthet Dent. 2003;89(1):89-90.
38. Agar JR, Cameron SM, Hughbanks JC, Parker MH. Cement removal from restorations luted to titanium abutments with simulated subgingival margins. J Prosthet Dent. 1997;78(1):43-47.
39. Tarica DY, Alvarado VM, Truong ST. Survey of United States dental schools on cementation protocols for implant crown restorations. J Prosthet Dent. 2010;103(2):68-79.
40. Li J, Naito Y, Chen JR, et al. New glass polyalkenoate temporary cement for cement-retained implant restoration: evaluation of elevation and retentive strength. Dent Mater J. 2010;29(5):589-595.
41. Kerby RE, McGlumphy EA, Holloway JA. Some physical properties of implant abutment luting cements. Int J Prosthodont. 1992;5(4):321-325.
42. Wadhwani C, Hess T, Faber T, et al. A descriptive study of the radiographic density of implant restorative cements. J Prosthet Dent. 2010;103(5):295-302.
About the Authors
Cary A. Shapoff, DDS
Private Practice Limited to Periodontics—Dental Implant Surgery
Fairfield, Connecticut
Brent J. Lahey, DMD, MS
Private Practice Limited to Periodontics—Dental Implant Surgery
West Hartford, Connecticut